Abstract
Objectives
Acquiring communication and interpersonal skills is an important part of providing patient-centered care and improving patient satisfaction. This study explores whether residents' own values about patient communication can be influenced by training.
Methods
As part of service excellence, a three-hour communication skills training in AIDET™ (Acknowledge, Introduce, Duration, Explanation, Thank You) was delivered to first and second Post-Graduate Year (PGY) residents (n = 123). A survey was designed to measure the value of patient communication and administered pre/post communication skills training.
Results
Residents' scores about communication values improved significantly for all areas pre- to post-training for patient communication skills (p<0.04). After training, there was little difference by medical specialty, other than surgical specialties, which showed the greatest increase in valuing requesting permission (p=0.034). Gender was also not associated with differences in values, except men showed a greater increase in valuing sitting down (p=0.021) and introductions (p=0.005) than women who already valued these specific behaviors prior to training.
Conclusions
Residents value communication, and AIDET™ training is a useful tool to increase the values of good communication and interpersonal skills to enhance service excellence.
Introduction
Patient satisfaction is tied to good communication, and now is directly measured by questions on the Hospital Consumer Assessment of Healthcare Providers and Systems (HCAHPS) survey that hospitalized patients complete after discharge. Press Ganey, a national patient satisfaction vendor, includes five additional questions in the doctor communication domain. Studies have investigated how physicians are taught to communicate, but many have not included what behaviors are taught to improve patient communication. 11 Furthermore, these studies contain a mismatch between the assessment instruments or procedures and the actual behaviors measured. Current models, such as The Four Habits Model, are now addressing these behavioral tasks and matching them to evaluations. 12 In this training model, physicians are taught about communication skills in four broad categories: 1) Invest in the beginning, 2) Elicit the patient's perspective, 3) Demonstrate empathy, and 4) Invest in the end. There is now the Four Habits Coding Scheme, which is an instrument derived from this teaching model. 13
The AIDET™ mnemonic was developed originally by the Studer Group as a template for improving physician communication with patients and now is widely applied across hospitals and trainings: Acknowledge (address each person in the room), Introduce (introducing yourself, role, specialty), Duration (setting expectations for the visit/procedure), Explanation (treatment and/or diagnosis), and Tank You (appreciation).14–16 The Doctor Communication, Attention, Respect, Expertise (CARE) Task Force is part of our institution's service excellence efforts and is charged with improving patients' satisfaction with their physicians. In 2012, the task force did a needs assessment of communication skills training using survey data from program directors. Less than 10 percent of program directors acknowledged training house staff in verbal and nonverbal communication skills. This reinforced the strategic plan to train all PGY1s and PGY2s who are often on the front line with patients. Training was developed to address these communication skills for house staff physicians to improve patient satisfaction. Training included didactics, large and small group discussions with faculty facilitators, video of good/bad doctor-patient communication, role play and audience response ratings with discussion. Previous research has shown that communication skills training increases self-efficacy up to three years later and increases performance up to a year later. 12
Increasing residents' values of these communication skills, like self-efficacy, may be another determinant of utilization and retention of these skills with patients.
Methods
In 2013, as part of an institutional effort on value-based purchasing and service excellence, six three-hour communication skills training sessions in AIDET™ were delivered to mixed clinical specialty groups of PGY1s and PGY2s. IRB approved surveys (n=123) were collected before and after training to determine changes in participants' valuation of the specific communication skill. All residents were asked to complete the survey, but some arrived late and missed the pre-training survey.
The survey was developed by pairing AIDET™ behaviors such as introducing oneself when entering the room, as well as other behaviors such as sitting down with a patient with a five-point Likert scale response for how much the resident valued that behavior. (Figure 1.) The survey was developed internally by three of the authors (Kunkel, E., Braverman, A., Katona, A.) for the purpose of this study. It included demographics for PG year, specialty, gender and age. Eighteen items were rated very important, important, moderately important, of little importance, or unimportant. The ratings were converted to a 1 to 5 scale. No items were directly related to the AIDET™ mnemonic taught in the communication skills workshop. Two questions were related to No. 2 of the three-part physician initiative: sitting down to speak with the patient and asking, “What questions do you have for me?” The third part of the physician initiative related to use of AIDET™. Six additional items included both verbal and nonverbal communication skills. All items paralleled the audience response segment of the communication skills workshop. Participants were asked to name which item was most important for patient care and which item was least important for patient care. Heretofore, studies have measured the actual behaviors and not the residents' perception about the value of these behaviors.

Values Questionnaire
Descriptive statistics were calculated for all collected items at both pre- and post-survey time points. Frequencies and percentages were reported for categorical items; means and standard deviations were reported for continuous items.
While the survey was administered in a pre-post format, there were no identifiers that matched the pre- and post-surveys, and there were different numbers of surveys collected pre and post (123 and 128, respectively). This was done to preserve resident confidentiality in the context of evaluating the impact of training. A pseudo ID was created based on sex, PGY, age and specialty. This allowed for unique identification of about 50 respondents and small clusters of the remaining respondents that ranged in size from two to six. This identifier was then used to represent clusters in generalized estimating equation models (GEE) with robust variance estimation. These models were used to estimate differences in scores overall, and differences in score change by sex, PGY and specialty.
HCAHPS and Press Ganey scores preceding and following communication skills training were compared to see if there were positive trends but were not calculated for statistical significance.
Results
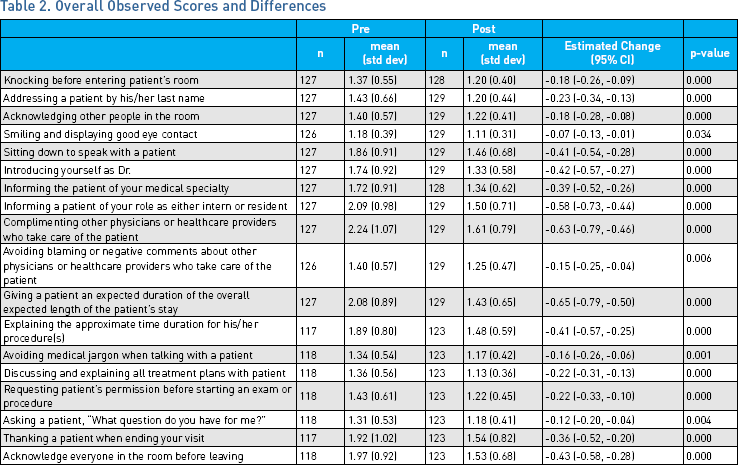
Table 1 presents respondent characteristics at pre and post. Respondents were evenly divided by sex and averaged 28 years of age. Table 2 presents the change in residents' valuation of communication behaviors after skills training. Smaller values reflect a higher valuation of the communication or interpersonal skill being queried, e.g., a drop in score meant the physician endorsed a higher value for that particular skill after training. Scores for all questions declined significantly (p<0.04) for all questions between pre- and post-survey, indicating a higher valuation for all communication skills after training.
Respondent Characteristics

Overall Observed Scores and Differences
In a comparison of male and female residents' valuation of communication behavior before and after training, there were two behaviors that showed significant differential change between males and females: sitting down to speak with a patient (p=0.021) and introducing oneself as Dr. ________ (p=0.005). With regard to sitting, females started with a lower pre score/higher valuation and had a smaller score change (1.62 and −0.25, respectively) than males, who started with a higher pre score/lower valuation and had a larger drop showing more improvement in their valuation score (2.1 and −0.55, respectively). A similar pattern is seen with the introduction question.
There was little difference by years of training with valuation scores; PGY2s had a greater valuation of asking a patient, “What questions do you have for me?” (p=0.01) after training, compared to trainees from other post-graduate years.
Table 3 shows surgical specialties had a significantly larger decrease in scores regarding asking a patient's permission before starting an exam or procedure (–0.44 vs −0.13, respectively, p=0.034), indicating that there was an increased valuation after training compared to nonsurgical specialties.
Observed Scores and Differences by Specialty

Table 4 presents changes in both HCAHPS and Press Ganey scores preceding and following communication skills training and reflects a positive increase in patient satisfaction. The HCAHPS doctor communication domain increased from 79.9 to 80.8. The Press Ganey doctor communication domain increased from 87.8 to 88.6 (from 52nd to 64th national percentile). These domains trended in an upward direction from before to after training.
Integrated HCAHPS/PG Survey (all specialties)

Pre-training;
Training September – October;
Post-Training
Percent of always response/national percentile
HCAHPS (Hospital Consumer Assessment of Healthcare Providers and Systems) PG (Press Ganey)
Discussion
Across specialties, medical residents highly value all aspects of communication and interpersonal skills with patients.9,12 Teaching communication skills, therefore, falls on receptive ears and is congruent with already established values. According to the Kalamazoo report from 2002, residents' values mirror attending physicians' valuation of these skills. 17 Our use of attending physicians at the training may have reinforced the valuation of these skills. The recent focus on physician communication skills appears to resonate with already held values, as training moved all scores to a more positive valuation.
Communication skills are also correlated with patient care and safety. Miscommunication between physicians and patients is the most common cause of medical errors and is responsible for more than 60 percent of sentinel events that lead to increased mortality or injury among hospitalized patients.18–19 Communication skills contribute to patient satisfaction as measured by patients' survey ratings under value-based purchasing and whether patients choose specific health care providers. 12 With revenue dollars now at risk, hospitals are increasingly incentivized to train their physicians to provide excellent communication with patients. Research has shown that patient perceptions and values can be influenced by physician behavior, e.g., a patient significantly overestimates the time a physician spends with her when the physician is seated. 20 Training residents with these communication skills contributes to the likelihood that behavioral changes will be made. If these skills are valued, there is a higher opportunity for the skills to be utilized and/or retained. 21 As seen in the psychological theory, Bandura has shown that behavior will change with self-reinforcement. 22 Another theory takes this further and suggests that the evaluation of consequences also leads to behavior change. 23 Being instructed to change a behavior that is not perceived to be of value is unlikely to be as effective as making a behavior change because the resident intrinsically values that change.
In 1999 and 2002, two conferences brought attention to the high valuation of communication skills and identified the need for better education and evaluation of medical professionals. 17 Five ways were identified to evaluate communication and interpersonal skills. In a study of 33 surgical residents and 16 attending surgeons, participants rated communication as very important in the successful care of patients despite attending surgeons reporting that they did not give feedback on communication skills. 24 Providing specific skills training can, therefore, improve this proficiency and can be effectively measured. Absent from these studies and conferences was an exploration of whether these skills are equally valued by training physicians.
Training physicians involves education about value-based purchasing, which necessitates the understanding of how communication and interpersonal skills are an integral part of patient care. Resident physicians bring their own independent valuation of these skills and, if training increases this valuation, the opportunity for good communication skills and greater patient satisfaction is enhanced. This increased satisfaction improved hospital value-based purchasing scores and often can improve quality, safety and patient satisfaction. 15 When put into practice, patient-centered communication constitutes an important indicator of quality care and contributes to a better patient experience and improved health outcomes.25–27
Physicians come to AIDET™ training with different levels of valuation of these skills despite all indications that these skills are of overall value. For example, initially, women valued a formal introduction prior to training more than men. During the course of their training, female physicians voiced having had the experience of being mistaken for a nurse, some other health professional, or support staff. This may predispose women to valuing a formal introduction and clarification of their role for patients. Most sessions had meaningful dialogue regarding the role of transitioning from a medical student to a PGY1/2 physician, as well as the use of “doctor” versus an introduction using the resident's first name. Feedback from this training led to a rollout of “doctor” identification tags for all physicians.
Female physicians valued sitting down with patients more than their male colleagues before training (as had been seen in previous research). 28 Although physicians appear to value sitting down, studies have shown few actually do sit down and, in one study, less than 10 percent actually sat with patients when being observed. 29 Other research has shown that sitting with a patient can have a significant positive impact on patient satisfaction and provider-patient rapport. 30
AIDET™ training teaches the skills of a formal introduction and reinforces the value of role clarification so that patients understand clearly who their physicians are. Our training also taught the value of sitting down to our residents. Physicians who initially did not value sitting as highly as others were the ones to see the most change in that value after training. The finding that surgical house staff increased their valuation of requesting a patient's permission before starting an exam or procedure may reflect that they are in a procedural specialty. Increased differences between medical and surgical specialties might have been found with more senior house staff who have better consolidated their professional clinical specialty identities.
The communication skills that were reported to be more highly valued after training may have contributed to the increase of inpatient satisfaction scores as measured by HCAHPS and Press Ganey inpatient satisfaction survey. Although there is no way to be certain that the AIDET™ training was directly responsible for the increase in patient satisfaction scores, this training of all house staff was the only hospitalwide intervention that was made with physicians during this time period.
There are several limitations to this study. Although resident surveys were anonymous, there were many attendings who were involved in the training. The desire to please those attendings by demonstrating increased values for the skills taught may have masked actual valuation of those skills. The training emphasized that these skills were valued by the hospital leadership and faculty, and this also may have had a biasing effect rather than a personal intrinsic change in valuation. The study could benefit from follow-up with the residents to see whether the valuation of the communication and interpersonal skills translated to behavioral changes with the implementation of these skills. Follow-up would create an opportunity to see whether the valuation of communication skills was sustained over time. Another limitation of the study was due to the choice of statistical analysis which involved assumptions that could contribute to differences in sensitivity analyses.
The challenge of teaching communication involves both how to train and how to measure these skills. Future research must focus on what specific skills are being taught and measured, and if the resident also values the skill being taught. Focusing on the value of the skill, along with the specific skill, promises to be an important part of changing that behavior and fulfills the ACGME core competency for developing communication and interpersonal skills with patients. Self-evaluation of this kind, done with pre/post surveys and audience response systems also can be used as part of the required 360° resident evaluations.
Conclusions
Residents appear to intrinsically value communication skills, but training in communication and interpersonal skills, such as AIDET™, increases the perceived value of these skills. We believe that increased value contributes to the implementation of these skills. Gender, specialty, and surgical versus nonsurgical specialty do not appear to play a major role in how residents view and value communication skills.
