Abstract
This Perspective article explores the complex role of motivation in mental health treatment, drawing from the author's personal experiences as a patient. Motivation is often viewed as a prerequisite for treatment success, or for accessing care at all. However, this ceonceptualization can overlook the multifaceted challenges patients face which can impact their motivation in the first place—such as prolonged waits for treatment, systemic barriers to care, and the nature of mental illness itself. Misunderstandings about patient motivation can reinforce harmful narratives that stigmatize individuals, ultimately undermining their recovery efforts. The author emphasizes the need for clinicians to adopt a more reflexive approach—examining their own motivations and biases in order to improve features of treatment and foster more empathetic relationships with patients. A shift towards a more nuanced and compassionate understanding of patient motivation will be supported by: (1) recognizing patient strengths through validation; (2) enhancing trust in treatment through consistency; (3) responding to trauma; (4) creating more acceptable and flexible treatment models via co-production; and (5) seeing ambivalence as a therapeutic opportunity. By redefining motivation as a fluid and shared experience, mental healthcare can itself become more motiviating—creating treatment that is more inclusive, equitable, and supportive of recovery.
Introducing Motivation
Motivation is undoubtedly an important ingredient in making positive change happen, and there is evidence to show that increased patient motivation at the outset of treatment can contribute to better outcomes from psychological therapies. 1 Whole modalities such as Motivational Interviewing have been developed to support behavior change 2 and to enhance readiness for engaging in other forms of treatment such as Cognitive Behavioral Therapy. 3
However, my own lived experiences illustrate many of the problems that can arise from how motivation is conceptualized within mental healthcare. Becoming more aware of the potential harms in these conceptualizations—which are often rooted in stigmatizing and unbalanced narratives of motivation—in the first step in helping treatment providers and patients alike to create more nuanced, shared understandings of how treatment can best be provided and received. This in turn will help prevent the marginalization of patients with similar experiences to my own, resulting in more compassionate and equitable care.
Patient Motivation is Often Misunderstood and Overlooked
I have often been told that I am insufficiently motivated in my treatment and recovery. This has evoked a sense of injustice within me, feeling that the motivation, effort, and persistence I have shown to seek help in the first place have been ignored. I reality, there have been times when I have been highly motivated to recover from a severe eating disorder, among other difficulties. I have wanted to channel my optimism and belief in a future unburdened of debilitating mental illness into creating a healthier, more fulfilling life. My excitement and conviction for recovery have bubbled up to the surface, and I have wanted others to come alongside me to help me harness this energy to make meaningful change.
During these periods, I have often sought help from healthcare professionals, knowing that the severe difficulties I have experienced aren’t things I should expect myself to recover from in isolation, or without treatment. However, help has often been slow to come, or denied entirely. Whilst the windows of opportunity when I have been highly motivated haven’t always been frequent or lengthy, no amount of motivation would have persisted over the many months and years I have spent being refused treatment, waiting for assessments, or sitting on waiting lists to see anyone at all. I have sometimes experienced a visceral sense of deflation, where my drive for recovery and a healthier future has come crashing down to earth when I have had nobody alongside me to share it with.
Irrespective of structural barriers to treatment provision which can demotivate patients and clinicians alike (particularly those from marginalized backgrounds), many mental illnesses make it fundamentally challenging for patients to demonstrate motivation in the ways that are often expected of us within clinical settings. We may be reluctant, resistant, and unwilling to participate in treatment, at times. This does not mean that we are inherently demotivated, as though this is a constituent component of our character. Rather, motivation is shaped by a complex array of features. Notably, in the case of eating disorders, poor nutrition can dramatically impair motivation—but this is transient, and returns with nutritional rehabilitation. 4 It has felt unfair to be described as “unmotivated,” “lacking engagement,” or “uncooperative”—as so many of my medical records note—when it would be a challenge for even the most well-regulated and medically stable of people to be enthusiastic and agreeable about the uncomfortable, unfamiliar, and sometimes invasive interventions that treatment can involve.
Acknowledging demotivation as a part of illness itself can feel less blaming, and more compassionate. I have felt more fully understood when clinicians have acknowledged the gap between how motivated and hopeful I might have felt when seeking help initially, and how I may have presented to them after a period in which that help has been very slow to arrive. Appreciating this complexity can make motivation a viable treatment target, too—be that through nutritional rehabilitation in my own case, or via addressing any of the many factors that can impact motivation across biopsychosocial domains. 5
Ultimately, it is important to recognise how being present in a healthcare setting at all may have exhausted a patient's capacity for motivation. It is well known that patients with diverse symptomatologies and/or identities may also face significant barriers to accessing treatment, and they may feel poorly understood when they do. This includes people from racial minorities and those living in poverty, 6 or—in my own case—autistic patients, 7 and males with eating disorders. 8 Recognizing that patients are doing the best they can with the resources they have is a vital step towards creating the therapeutic relationships upon which treatment and recovery are built.
False Narratives can Stigmatize and Marginalize
Throughout my experiences, I have witnessed how the imposition of unhelpful narratives can obscure the motivations of patients, resulting in feelings of injustice and alienation. They can also leave features of treatment provision that impact motivation unchallenged, resulting in missed opportunities to make mental healthcare easier to engage with for all, and more motivating in itself.
It has been suggested to me that not only do I “not want to get better,” but that I actively “want to be unwell.” As one emergency department consultant told me when I sought treatment for life-threatening electrolyte imbalances, “if you really wanted to get better, you wouldn’t keep getting admitted,” asking, “what do you get out of being unwell? Do you like the attention?” This made me feel deeply misunderstood and blamed, causing distress. I have routinely been allowed to discharge myself when in distress, with no psychological support ever being provided across dozens of medical and psychiatric crises.
I’ve been told, “if that is what you want to do, we can’t stop you,” when I have desperately wanted to stay in hosptial and find the treatment acceptable. Just because the treatment has been there doesn’t mean that I have been able to receive it when severely unwell, especially without support or in the presence of stigmatizing narratives. This understanding has never been comprehended. Instead, my difficulties participating in treatment have been explained as me being difficult, instilling a sense of shame which only worsened my symptoms and made me less likely to seek help again in the future.
Even when suicidal, I have asked for help only to be told, “if you really want to kill yourself, there is nothing we can do to stop you.” In those moments, I have needed staff to engage with the part of me that really wants to live, and has been deeply distressed by thoughts and plans around death. The practice of explaining away patients’ difficulties engaging with the limited help they are offered using harmful narratives must be questioned, and the motivations for doing so challenged. For example, portraying illness as volitional and stigmatizing patients as problematic may deflect from acknowledging the existence of insufficiencies in treatment provision itself.
Re-Conceptualizing Motivation
It is important to consider the features of treatment that may expend patients’ motivation to persist with it, and to resist blaming patients when they encounter barriers such as those I have described here. Preventing and remediating the harms of experiences like mine requires a more nuanced understanding of patient motivation, and a greater commitment to reflexivity on the part of service providers. I hope that the following dimensions of care—summarized visually in Figure 1, below—can be used by healthcare professionals to inform a more compassionate and practically effective approach to conceptualizing patient motivation:
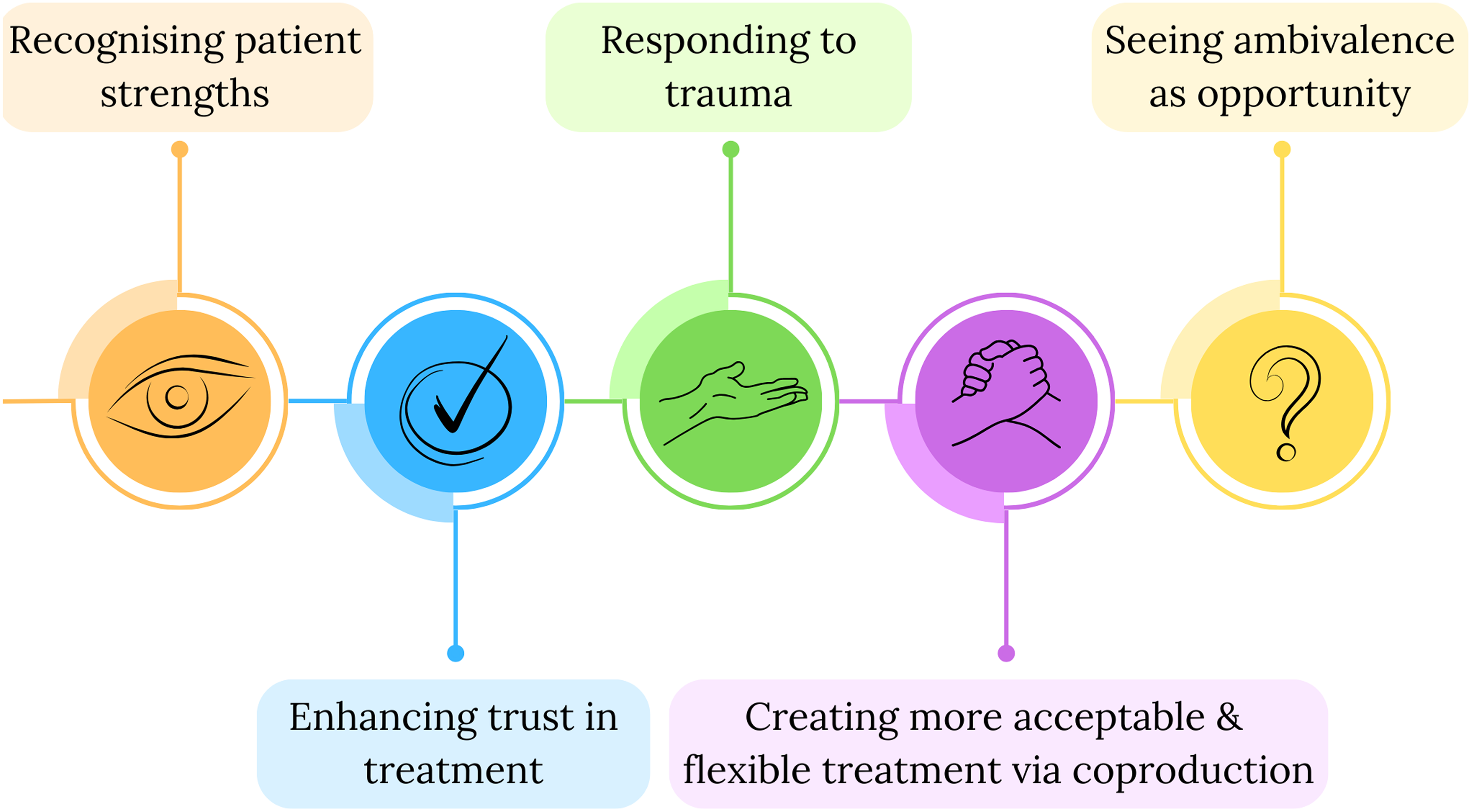
Steps to reconceptualizing motivation for more inclusive mental healthcare.
Changing the Narrative
By recognizing motivation as a fluid concept that is often influenced by a complex interplay of individual experiences, systemic barriers, states of illness, and features of treatment, we can create more inclusive mental healthcare that is less likely to perpetuate stigmas and power imbalances, and more likely to facilitate recovery. Despite some of the challenging examples I have shared in this paper, I know the benefits of a more nuanced approach from my own experience, too. Some of the most pivotal moments in my recovery have been times when I have been met with an understanding and appreciation of the challenges I have had, not only with my health, but with my ability to seek help from professionals and engage with treatment. It has been incredibly reassuring when my ambivalence, distress, and difficulty communicating my needs in effective ways have been seen as natural struggles for someone with my history, rather than something to be blamed for.
For example, having a member of staff say, “I can see that it is very difficult for you to be here”, helped me to stay in hospital to receive life-saving emergency treatment during a period when I usually tried to escape the building because I felt like I was being blamed for my distress. Having another person see my motivational difficulties as valid has helped absolve ingrained feelings of stigma and shame that have held me back in my recovery. Compassionate responses to my distress have been an important part of helping me to reconceptualize my sense of self-worth, where I now feel more deserving of care and better able to seek and engage with it. Similarly, having my efforts to engage with treatment acknowledged—even if they have been imperfect—has helped me build a more trusting relationship with healthcare providers, meaning I can seek help earlier rather than waiting until a crisis in which I would be more likely to refuse essential treatment. Simple statements that affirm my help-seeking have encouraged me to become more skillful in how and when I take responsibility for my health and recovery. These examples demonstrate the therapeutic opportunities provided by working with the concept of motivation, even where patients do not appear motivated and engaged in conventional ways.
In conclusion, there are undoubtedly significant structural barriers to creating more inclusive and less stigmatizing mental healthcare, and these barriers will not change overnight or be removed by the efforts of any one individual. In the here and now, tending to the relational elements which shape patient motivation is a priority, and requires an appreciation of the ways in which narratives of motivation can constrain and blame on the one hand, but may offer opportunities for transformation and therapeutic change on the other. Reflexivity is central to creating a more nuanced understanding of patient motivation, and involves clinicians and treatment providers examining their own motivations and biases, and how these factors can shape their perceptions of patient engagement. This awareness can help in providing more supportive and empathetic relationships that validate the efforts patients have already made in simply seeking help at all. Allowing patients to define their own experience of motivation and creating shared understandings will contribute to a treatment environment in which every patient feels seen, heard, and included.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author received no financial support for the research, authorship, and/or publication of this article.
Ethical Approval
Ethical approval is not required.
