Abstract
Patient satisfaction is an important aspect of medical care. This study aimed to assess if patient satisfaction improved when patients shared their expectations with the provider in writing before a visit, and providers purposefully addressed those expectations during the visit. We gave 2 types of questionnaires to 343 patients: Version 1 asked for written expectations before the visit and assessed the visit quality after addressing those expectations, while Version 2 only evaluated the visit without soliciting expectations. Patient satisfaction and meeting expectations were measured on a 1–10 Likert-type scale. The grouped that shared written expectations before the visit (n = 169) showed a significantly higher patient satisfaction score (9.88) compared to the group without shared expectations (n = 136, score 9.43, P < .0001). Conveying written expectations to healthcare providers before the visit improved patient satisfaction, potentially enhancing compliance and overall medical outcomes.
Introduction
The success of medical interventions depends largely on how well patients follow recommendations.1–3 This includes taking medications, attending appointments, and making lifestyle changes. These tasks can be challenging, and if patients face difficulties and do not comply with recommendations, the intended interventions may not work.4–7 Patient compliance is influenced by the trust in the relationship between the patient and the healthcare provider. 8 When patients trust their providers and believe in the proposed treatment plans, they are more likely to follow lifestyle suggestions, take prescribed medications, and keep up with medical appointments.9,10 Positive patient-provider experiences play a crucial role in building trust between patients and healthcare providers. 11 Although trust is difficult to measure objectively, patient experience and satisfaction provide effective alternatives to evaluating trust. Therefore, patient satisfaction is not only an important aspect of medical care, it also serves as a measurable factor for evaluating providers, clinics, and even entire hospital systems in their relationship with patients and the community. 12
Our aim in this study was to assess how conveying patient expectations in writing before outpatient clinic visits affects the improvement of patient experience and satisfaction.
Methods
Survey Questionnaire
The Patient Experience Aligned with Conveyed Expectations (PEACE) questionnaire was created at Kapi’olani Medical Center for Women and Children for a quality improvement (QI) project. Our team reviewed prior prominent patient satisfaction surveys, including the Consumer Assessment of Healthcare Providers and Systems (CAHPS) surveys, and created a simple version with a singular aim: evaluate the effect of written expectations on patient satisfaction. Our survey was reviewed by the hospital QI committee, but was not validated in any prior study before. The QI project aimed to assess patient experience and patient satisfaction in outpatient clinics. We developed 2 versions of the questionnaire: Version 1 (V1) contained a separate open-ended question prior to the provider's visit asking: “What do you expect from this visit?,” and 3 further questions following the visit: “How well did we do to meet your expectations?” (Q1), “How satisfied are you with your visit?” (Q2), and “How helpful was it to communicate your expectations to the provider prior to the visit?” (Q3). Version 2 (V2) did not have a chance to convey written expectations before the visit, and had only 3 questions after the visit: “How well did we do to meet your expectations?” (Q1), “How satisfied are you with your visit?” (Q2), and “How helpful would it be to communicate your expectations to the provider prior to the visit?” (Q3). All questions used a 1–10 Likert-type rating scale, with 1 being the poorest, and 10 being the best.
Patients were given V1 or V2 questionnaires randomly. Medical professionals purposefully addressed specific written expectations for patients with the V1 questionnaire. We implemented this project in selected pediatric and adult outpatient clinics to assess whether addressing written expectations improves patient satisfaction. Since the original questionnaire was developed as part of a simple quality improvement project for the outpatient clinics, it was exempt from regulatory review or approval at the time of distributing the questionnaires.
Retrospective Study Participants
The current study was conducted as a retrospective analysis of previously completed V1 and V2 questionnaires from a consecutive sample of 343 patients. We collected 146 surveys from adult clinics and 197 from pediatric clinics (parents filled out the surveys in pediatric clinics), with a total of 178 V1 questionnaires and 165 V2 questionnaires. The outpatient clinics included general pediatric clinic, pediatric cardiology clinic, general adult clinic, and adult congenital cardiology clinic. The clinics were located in urban Honolulu, part of a tertiary care pediatric and adult hospital. Patients of all ages, genders, and ethnicities were included in the study without any exclusion. All questionnaires were de-identified and did not include any personally identifiable information or protected health information. This retrospective study of previously distributed and collected surveys was reviewed by the Hawaii Pacific Health Research Institute and was deemed exempt from further Investigational Review Board review and exempt from retrospective patient consent.
Statistical Analysis
Patient responses were analyzed and presented using descriptive statistics including mean, standard deviation, standard error of measurement, median, interquartile range, and range. Responses were analyzed with Mann-Whitney as well as Kolmogorov-Smirnov tests to compare the mean and distribution. Statistical significance was defined as P < .05. Graphical representation of the results was displayed using violin plots. Statistical analysis was performed using Prism version 8 (GraphPad Software, San Diego, CA).
Results
We analyzed a total of 343 questionnaires, 146 from adult clinics (V1 n = 76, V2 n = 70) and 197 from pediatric clinics (V1 n = 102, V2 n = 95). Out of the original 343 questionnaires, 38 incomplete or erroneous questionnaires were excluded (V1 n = 9, V2 n = 29). The final analysis included responses from 305 questionnaires/patients, 123 from adult clinics (V1 n = 70, V2 n = 53), and 182 from pediatric clinics (V1 n = 99, V2 n = 83). This comprised 169 responses with the V1 questionnaire and 136 responses with the V2 questionnaire (total n = 305).
The distribution of the responses on a 1–10 Likert-type scale is summarized in Table 1. When patients shared expectations in writing and providers addressed them during the visit (V1 n = 169), 90% of patients (n = 152) reported a perfect 10/10 satisfaction score, compared to only 68% of patients (n = 93) without this opportunity (V2 n = 136). Similarly, patient expectations reached a 10/10 score in 89% of patients (n = 151) receiving the V1 questionnaire compared to 65% of patients (n = 88) with the V2 questionnaire (Table 1).
Comparison of Questionnaire Answers Between the 2 Groups (V1 and V2).

Abbreviations: V1, version 1; V2, version 2.
Overall satisfaction was higher when patients communicated expectations in writing before the appointment. The mean satisfaction scores were significantly higher in the V1 group compared to the V2 group (V1 9.88 vs V2 9.43, P < .0001) with a more consistent distribution (coefficient of variations V1 4% vs V2 10.9%, P = .0018) (Figure 1). When comparing surveys from pediatric and adult clinics, there was a significant but less pronounced difference in the mean satisfaction scores in pediatric clinics between the V1 and V2 groups (V1 9.92 vs V2 9.73, P = .039), compared to adults (V1 9.81 vs V2 8.96, P < .0001) (Figure 2). Surveys from pediatric and adult groups showed similar patient satisfaction scores with written expectations before the visit (pediatric V1 9.92 vs adult V1 9.81, P = .63), but adult clinics had lower patient satisfaction scores compared to pediatric clinics without the opportunity of sharing their expectations before the visit (pediatric V2 9.73 vs adult V2 8.96, P < .0001) (Figure 2).

Comparison of responses in meeting expectations and patient satisfaction. Patients, who conveyed their expectations and received directed counseling in response to those expectations (V1) had significantly higher scores in terms of meeting expectations and overall satisfaction compared to the group of patients, who did not have a chance to convey their expectations (V2) before the visit.
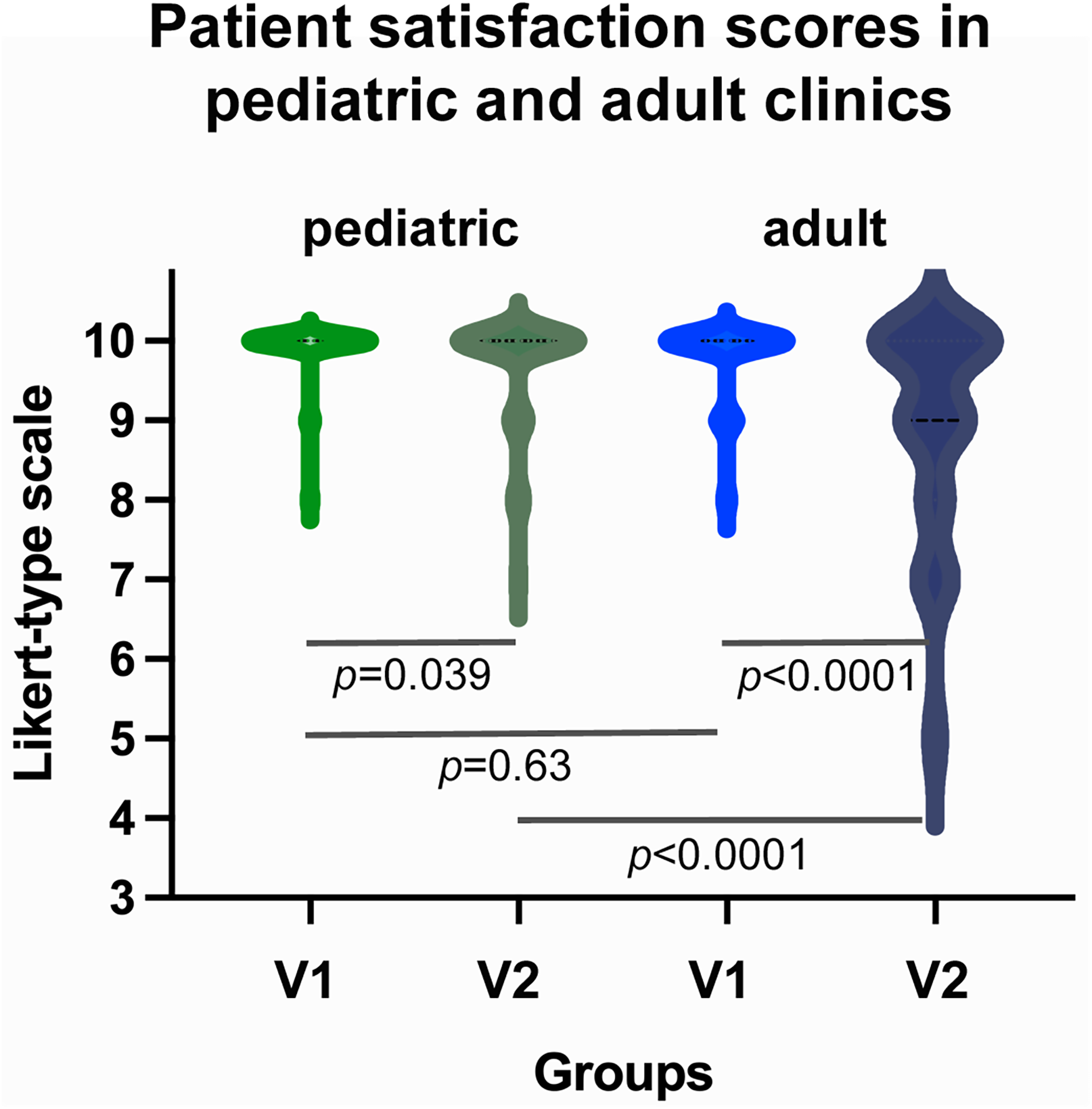
Comparison of patient satisfaction in pediatric and adult clinics. In both pediatric and adult clinics there was a significant improvement in patient satisfaction scores for patients, who shared their expectations in writing before the visit (V1), compared to patients without this opportunity (V2). This improvement in patient satisfaction was more pronounced in adult clinics compared to pediatric clinics.
In addition, the majority of patients in both pediatric and adult clinics (94% total n = 288, 93% in the V1 group n = 158, and 96% in the V2 group, n = 130) believed that communicating expectations to the provider in writing would be very helpful (10/10), whether it was implemented or only suggested for the future (Table 1).
Discussion
This study demonstrates that conveying expectations in writing to healthcare providers before outpatient visits leads to improved patient satisfaction scores.
Patient satisfaction is one of the most important elements of medical management on both individual and system-wide levels. Measurable patient satisfaction serves not only as a representative index of healthcare quality, but it has also become a central focus of the evolving healthcare service industry, influencing how we evaluate medical outcomes in the modern healthcare environment.12–14 The overall patient satisfaction and experience during outpatient visits or inpatient admissions extend beyond factors like staff courtesy, convenient amenities, service completeness, and an aesthetically pleasing environment. 15 A crucial aspect of patient experience and satisfaction is the unique expectation each patient brings to the medical facility. Since each patient may have a slightly different expectation, assuming and providing the same care to every patient is not the most effective or successful approach to enhance patient experience and satisfaction.
In our study, patients reported a more positive experience and higher satisfaction when their written, explicit expectations were met during an appointment. Listening to patients make sense. When patients received the V1 version of the PEACE questionnaire and shared their expectations in writing, the provider was able to align the medical management to those written expectations, which resulted in a higher rate of fulfilled expectations and better patient satisfaction scores (Figure 3). Improved patient satisfaction establishes a positive and trusting relationship between the patients and the medical team, subsequently improving the patients’ compliance with recommended medical regimens and lifestyle modifications (Figure 3). Patient compliance significantly influences the overall outcome of medical interventions, presenting an effective means to reduce costs associated with unnecessary readmissions and repeated treatment efforts.
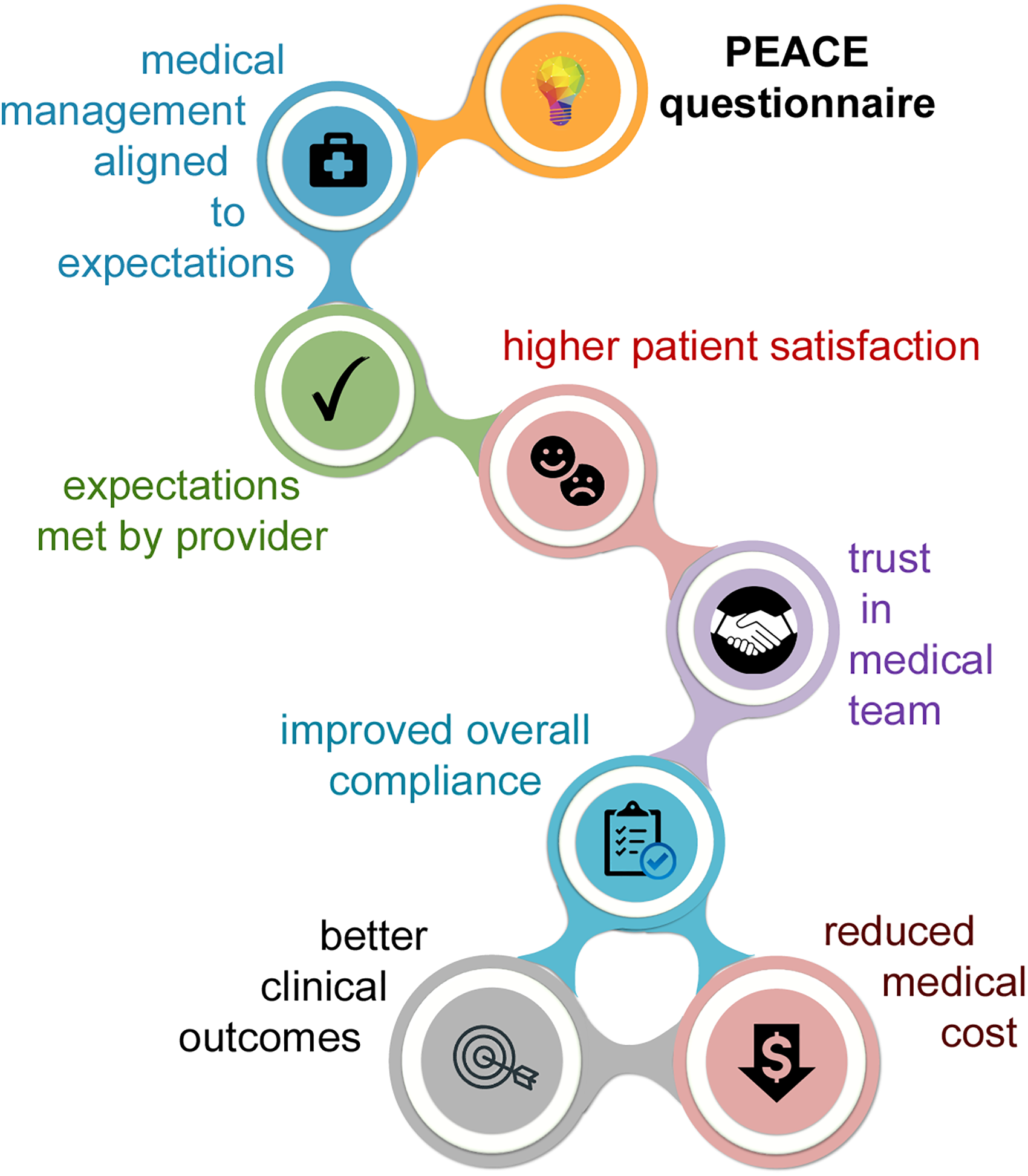
Medical management aligned with patient expectations improves patient satisfaction. The flowchart demonstrates the downstream effect of conveying written expectations to the provider prior to the medical visit. Medical management that is aligned with patient expectations results in higher patient satisfaction, which improves the trust in the provider and the proposed medical care, leading to better compliance with the treatment plan, which in turn may result in more favorable clinical outcomes and reduced medical costs. PEACE, Patient Experience Aligned with Conveyed Expectations questionnaire.
Limitations
Our study was limited by its retrospective nature and by the primary care or specialty clinics in which the surveys were utilized at. The analysis is also limited by the fact that the surveys did not collect sociodemographic data. Nevertheless, even in this pilot study, we were able to show significant improvement in both patient expectations and patient satisfaction using the PEACE questionnaire. In the future, a more extensive study including multiple sociodemographic aspects of patients surveyed in multiple different outpatient clinics and facilities could strengthen our findings.
Conclusion
Conveying patient expectations to the provider in writing before the visit, and aligning the subsequent encounter to these expectations, not only improves patient satisfaction, but it may positively impact the overall trajectory of the medical condition while reducing medical costs.
Supplemental Material
sj-docx-1-jpx-10.1177_23743735241240925 - Supplemental material for Listening to Patients Makes Sense: Soliciting and Purposefully Addressing Written Patient Expectations at a Provider Visit Improve Patient Satisfaction
Supplemental material, sj-docx-1-jpx-10.1177_23743735241240925 for Listening to Patients Makes Sense: Soliciting and Purposefully Addressing Written Patient Expectations at a Provider Visit Improve Patient Satisfaction by Andras Bratincsak, Josephine Quensell and Bryan Mih in Journal of Patient Experience
Supplemental Material
sj-docx-2-jpx-10.1177_23743735241240925 - Supplemental material for Listening to Patients Makes Sense: Soliciting and Purposefully Addressing Written Patient Expectations at a Provider Visit Improve Patient Satisfaction
Supplemental material, sj-docx-2-jpx-10.1177_23743735241240925 for Listening to Patients Makes Sense: Soliciting and Purposefully Addressing Written Patient Expectations at a Provider Visit Improve Patient Satisfaction by Andras Bratincsak, Josephine Quensell and Bryan Mih in Journal of Patient Experience
Footnotes
Declaration of Competing Interest
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Approval
The research study was reviewed by the Hawaii Pacific Health Research Institute and was deemed exempt from Institutional Review Board review and exempt from patient consent.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Patient Consent
Not required.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
