Abstract
Many hospitals face a common challenge: limited space for a high number of patients. This has led to quick patient throughput, which can impact patient perception of discharge readiness. This study examined whether a poster highlighting tasks to complete as part of the discharge process improved caregiver perception of readiness to transition home. Using a sequential, exploratory mixed methods design, focus groups were convened to explore clinical staff perspective on the discharge process on 3 pediatric inpatient units at a large, urban, pediatric academic medical center in the United States. Analysis of this content informed the design of a poster intervention to “nudge” caregivers (eg, parents, legal guardians) toward readiness and self-efficacy that was then tested in a randomized, controlled experiment. The poster focused on practical knowledge for specific areas of transition adjustment, such as medication and care recipient recovery behaviors, barriers, and enablers. Caregivers (n = 135) completed surveys at discharge indicating their perceived readiness to transition home with their child. Analysis of covariance was used to test the effect of the poster condition (poster vs no poster) on caregiver readiness, preparedness, and confidence for discharge while controlling for previous admission history. Significant effects for poster presence were found on caregivers’ perceived readiness for discharge, F 1,125 = 7.75, P = .006, Cohen’s d = 0.44; and caregivers’ perceived preparedness for the transition home, F 1,121 =7.24, P = .008, Cohen’s d = 0.44. Only a marginal effect was found for poster condition on caregivers’ confidence ratings, F 1,125 = 2.93, P = .090, Cohen’s d = 0.29. The results suggest that simple nudges in the patient care environment may yield measurable improvements in caregiver outcomes.
Introduction
Every day 9706 pediatric patients are discharged from hospitals in the United States (1). Hospital discharge procedures vary within and across hospitals and regions (2,3), and only recently has a framework for pediatric discharge been developed (4). In many cases, the discharge process is fraught with inconsistencies, omissions, and duplications of care (5 –8). Even when discharge plans exist, patients, families, and outpatient health-care providers have difficulty understanding and executing them (8 –10). In many cases, patients leave the hospital unprepared for the transition home (11), which can contribute to worsening health and increased likelihood of hospital readmission (7, 9, 12,13).
Various discharge toolkits have been developed to help patients and providers in discharge planning, such as checklists covering essential processes and guides to educate and empower patients (3,14 –17). Such tools target slower, deliberate, logical, “system 2” human reasoning (18 –25). The present study examined whether interventions targeting automatic, fast, “system 1” thinking could also improve the discharge process. Such “nudges” aim to improve automatic decision-making by altering physical, social, and psychological aspects of the decision environment to increase the probability of individuals choosing better options for themselves and society at large (26). This framework has steadily gained popularity in the past decade, as both private industry and governments in several nations have experimented with building nudge research teams to develop and test nudge-based policies (27).
The present study tested whether caregiver (eg, parent or legal guardian) exposure to a “nudge” poster that highlighted discharge process tasks improved perceived readiness for discharge from a large, urban, pediatric academic medical center in the United States. There is currently limited evidence as to whether nudges can improve the hospital discharge process. A secondary aim of this work was to derive preliminary insights and “proof-of-concept” fruitfulness on using nudges to facilitate improved patient outcomes in clinical settings.
A sequential, exploratory mixed-methods design was utilized in 2 connected studies. The first, qualitative study (Study 1) used focus groups with clinical staff to inform potential nudge strategies for a second, randomized controlled trial of the derivative nudge intervention (Study 2). Collectively, these activities met local criteria for quality improvement and as such were not formally supervised by the hospital’s Institutional Review Board per their policies.
Study 1
Methods
Given the limited evidence on the use of nudging to improve hospital discharge, a qualitative focus group study examined clinical staff perspectives on the status quo discharge process in 3 pediatric inpatient units, particularly around strengths and weaknesses of discharge procedures as well as urgency, importance, and ability to act on identified problems.
Participants
A combination of purposeful and convenience sampling was used to recruit 3 focus groups of 33 interdisciplinary clinical staff (1 male, 32 females, n∼11 per focus group) from 3 inpatient units: Stem Cell Transplant, Hematology/Oncology, and Neuroscience (Table 1). Focus group samples were representative of the gender segmentation in pediatric nursing. Purposeful sampling was utilized to recruit secondary clinical staff (social workers, unit leadership) to ensure adequate representation and diversity of opinion. Convenience sampling was used to invite clinical staff (nurses, nurse practitioners [NPs]) who were most directly responsible for discharging the patient. Criteria for participation were employment on participating units with a direct role or vested interest in patient discharge, availability at the given time, and willingness to participate. Participants were nurses (64%), NPs (18%), researchers (10%), a nurse manager, and a social worker. Most (45%) were early career (<5 years), 37% were midcareer (between 5-20 years), and 18% were late career (>20 years).
Unit Characteristics, August 2018.

a Maximum occupancy across all units = 2 patient beds per room.
b Although we did not collect demographic or medical history data for the current sample, clinical staff have confirmed that unit descriptions are broadly representative of the “typical” patients admitted, and no specific steps were taken to over- or under-sample a specific patient subpopulation. Caregivers of patients receiving end-of-life support and caregivers who did not speak or read English were excluded from the study.
Procedures
Focus groups were held by 2 experienced facilitators in August 2018 at the hospital to minimize disruption to clinical operations and maximize attendance. Participants were asked to identify areas of the discharge process that needed improvement versus those that work well. Facilitators utilized a semi-structured protocol and encouraged participants to interact in a more informal, spontaneous manner. Sessions lasted 30 to 45 minutes and all audio was recorded.
Data analysis
Data were analyzed using grounded theory approach (28 –30), an inductive analytic procedure that involves “breaking down, examining, comparing, conceptualizing, and categorizing data” (31). Data were interpreted in terms of first-order explanations from the participants’ own answers and second-order explanations through our eyes as researchers. The coding team worked independently and convened to discuss similarities and dissimilarities with emerging themes after completing independent coding. This process of peer debriefing enhanced the validity of our interpretations (32), resulting in several concrete recommendations that informed the design of Study 2.
Results and discussion
The focus groups produced an array of avenues for intervention, ranging across variables such as cost, organizational complexity, practical ease of implementation, and day-to-day workflow impact (Table 2). Another key conclusion was that not all of these interventions were equally suitable for a low-cost, time-limited study. In particular, any study that would immediately impose notable disruption or workload burden for clinical staff, patients, or caregivers would not be supported.
With this in mind, caregiver perceptions were identified as an outcome variable that are both (a) readily measurable with minimal disruption or burden to the day-to-day care team workflow and (b) highly relevant to understanding the effectiveness of the discharge process and experience. Hence, attention was focused on crafting a minimally disruptive nudge intervention and approach to collect caregiver experience data.
Staff Recommendations on How to Improve the Patient Discharge Process.

Abbreviation: NP, nurse practitioners.
Study 2
Based on focus group feedback, we created The Way Home poster (Figure 1), a nudge focused on enhancing caregiver readiness and self-efficacy (33), while increasing practical knowledge for specific areas of transition adjustment, such as medication issues, use of web-based records and tools, and effective communication skills around care recipient recovery behaviors, barriers, and enablers. Caregiver readiness is a common reason for delayed discharge (34). The poster provided a clear “roadmap” noting key actions caregivers needed to complete before discharge, increasing their capacity to prepare. The nudge poster addressed 3 (caregiver readiness, communication, and portal adoption) of the 11 recommendations that emerged from Study 1. It is considered a “nudge” because it was a subtle addition to the environment. Caregivers could glance at it, scrutinize it, or ignore it altogether.
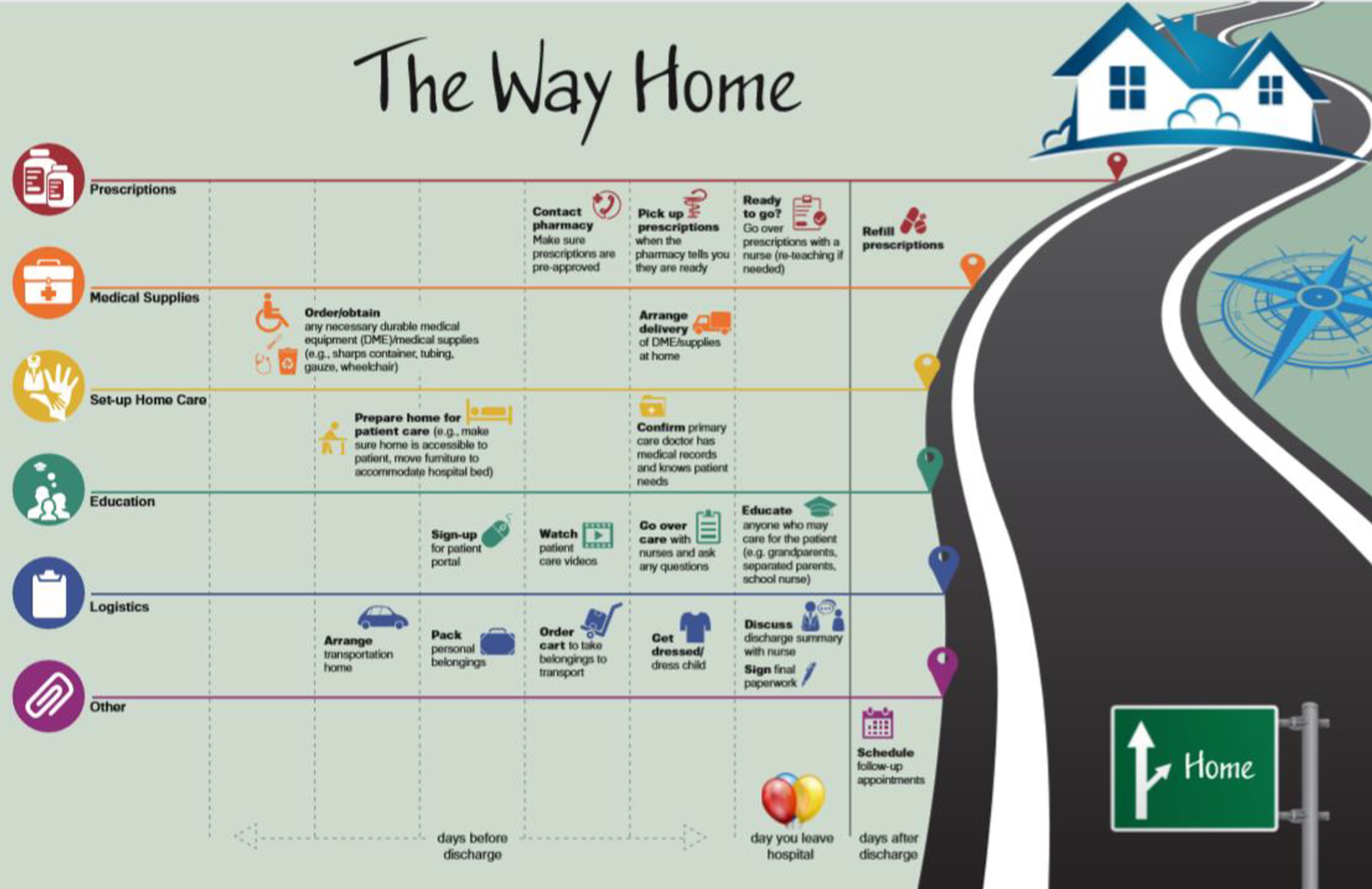
“The Way Home” nudge poster.
Methods
Participants/Setting
Participants were caregivers (n = 135; parents or legal guardians) whose children had been admitted to one of the participating inpatient units (Table 1). Rooms occupied by patients whose admission predated the study start did not have a poster hung until empty, to ensure that exposure to the intervention always started on admission day one. Otherwise, some patients may receive the intervention (nudge poster) only for a brief time before discharge, weakening the intervention “dose.”
Random assignment
Caregivers were randomly assigned to the poster (n = 79) or no-poster control (n = 56) condition. Assignment was randomized by room rather than by patient. For double occupancy rooms assigned to the poster condition, 2 posters were affixed on the walls. Caregivers of patients already admitted to rooms prior to study start were not included.
Materials
Intervention
The intervention consisted of a 11" × 17" laminated “The Way Home” poster (see Figure 1). The poster covered 6 key tasks that caregivers needed to complete before discharge: prescriptions, medical supplies, home-care set-up, education, billing, and departure logistics. It was consistently hung at eye level on the wall most directly facing the patient’s bed.
Outcome questionnaire
Dependent variables were measured with an investigator-constructed, one-page, self-report questionnaire (see Supplement A). The questionnaire consists of 2 open response items and 12 items that use a 5-point Likert-style response scale with the following options: “Strongly Disagree,” “Disagree,” “Neither Agree Nor Disagree,” “Agree,” “Strongly Agree” (note 1). No confidential or sensitive patient information was recorded; responses were matched to control or intervention group by room number.
Key dependent variables were responses to 3 items assessing general perceptions of perceived readiness and self-efficacy for post-discharge adjustment: I feel ready for the transition home. The hospital prepared me for the transition home. I am confident in my ability to care for my child after discharge.
No demographic information was collected because collecting demographic information about children and caregivers within the therapeutic relationship can be sensitive for many reasons.
Procedures
Study 2 was conducted over a 4-month period from April to July 2019. Research assistants, independent of the care teams, hung the nudge poster in patient rooms preassigned to the poster condition as rooms become available to new patients. Clinicians were instructed to ignore the posters entirely, unless the caregiver called attention to it.
At the end of each patient’s hospital stay, a research assistant not involved in the patient’s clinical care administered the outcome questionnaire (Supplement A) to caregivers; one caregiver per discharged patient completed the survey, whether their room contained a poster or not. Completion of the survey was voluntary and took approximately 2 to 5 minutes to complete. Throughout the study implementation period, laminated posters were cleaned per infection control guidelines and replaced as needed.
Hypotheses
We hypothesized that The Way Home poster would increase perceptions of readiness and self-efficacy (33) for effectively navigating the caregiving transition from hospital-based care to home-based care. The poster aimed at striking a balance between (1) providing a substantively informative overview of the different domains of transition adjustment and their relative temporal sequencing, and (2) presenting information in a highly compact and visually intuitive format. For example, although some amount of text is necessary to convey concepts, the use of visual icons and perceptual principles of element grouping, tabular presentation, and left-to-right directional flow often can communicate the salience and logical or temporal relationships among different elements and action steps far more compactly and holistically than discursive narrative. This also has the advantage of minimizing literacy or other cognitive-information-processing barriers to entry. This is in keeping with the key “nudge” (35) strategies of information simplification, use of graphical communication, and increasing the ease or convenience of information-processing and/or actions (36).
All 3 focal survey items were positively worded, such that stronger agreement connoted stronger perceptions of readiness (Items 1 and 2) or self-efficacy (Item 3; Supplement A). Therefore, we hypothesized that intervention (poster-exposure) participants would report significantly higher levels of agreement with each statement than control (no-poster) participants. Further, we speculated that this effect could be moderated by previous hospital stay experiences. We expected the effects of the poster to be most pronounced for those without prior inpatient discharge experience, as measured by self-reported number of prior visits for this condition. This corresponds to a hypothesized effect for each of the 3 (3) items, such that poster exposure increases readiness/self-efficacy (possible main effect), though possibly only or to a greater extent for those without prior discharge experience (possible interaction effect).
Data analysis
The 3 main dependent variables were assessed via analysis of covariance, where item ratings were modeled as a function of treatment condition (between subjects) controlling for number of previous hospital visits. Each dependent variable (DV) was separately analyzed. Cohen’s d effect sizes were computed between pairs of means.
Results and discussion
Caregiver perceived readiness
There was a main effect of condition, F1,125 = 7.75, P = .006, Cohen’s d = 0.44, such that caregivers who had posters in the room had higher readiness than those without posters (Figure 2). There was no interaction between the number of hospital visits and poster, F1,125 = 2.95, P = .088.

Scatter plot and regression lines of Q1 responses for caregivers who received a poster (blue) versus no poster (red).
Caregiver perceived preparedness for transition home
We found a main effect of poster condition on caregivers’ perceived preparedness for the transition home, F1,121 = 7.24, P = .008, Cohen’s d = 0.44; caregivers in the poster condition had higher preparedness ratings than those in the no poster condition. There was no interaction between the number of hospital stays and poster condition on readiness for transition home rating, F1,121 = 1.90, P = .170.
Caregiver perceived confidence to care for child after discharge
There was a marginal effect of poster condition on caregivers’ confidence ratings, F1,125 = 2.93, P = .090, Cohen’s d = 0.29, such that caregivers in the poster condition tended to have higher confidence they could care for the child at home than caregivers in the no poster condition. There was no interaction between the number of hospital stays and poster condition, F1,125 = 1.21, P = .272.
General Discussion
Overview
Our 2 studies addressed a handful of distinct but closely related goals: (1) to understand barriers and opportunities for more efficient and effective patient discharge; (2) to isolate those areas of potential intervention that would be most readily amenable to a minimally disruptive “nudge” experiment; (3) to execute a randomized pilot study to test that nudge intervention and evaluate its results; (4) to report our approach and its results toward the goals of identifying and disseminating best practices for more effective discharge and for the testing these sorts of lightweight interventions more broadly (ie, creative, realistic, data-driven interventions).
Primary Insights and Contributions
Each of the 2 studies—one a qualitative focus-group effort, the other a small-scale randomized experiment—yielded some important results that merit further testing and experimentation. First, the focus group analyses revelated 11 actionable intervention targets, ranging from low-cost and unobtrusive tweaks to more costly organizational changes. These included everything from providing checklists and educational materials to altering the sequencing of physicians’ morning rounds to creating a new formal job position of “discharge physician”—among several other intervention candidates.
Focus group insights directly informed planning for our randomized pilot experiment, both in terms of highlighting the importance of a low-footprint “nudge” intervention strategy and in suggesting the specific nudge intervention avenues that would be most practicable and promising. This led to our second study, in which caregivers/patients were randomly assigned to rooms with or without a poster nudge, illustrating key discharge-related actions, events, and their suggested timelines. Results showed that, compared to control participants, caregivers in the poster intervention condition perceived higher overall discharge readiness, greater preparedness for the transition home, and increased confidence in their post-discharge caregiving ability. Although not definitive, the results indicate that The Way Home poster intervention and other such nudges merit further research and applied use.
Implications
This work has provisional implications for hospital discharge practice and future research. Concerning hospital practice, Study 1 focus group results indicate that diverse intervention strategies may be promising for improving discharge efficiency and quality (eg, patient readiness, success outcomes), including but not limited to lighter-weight nudge interventions. The 11 intervention ideas reflect input from active, experienced hospital staff and run the gamut of simplicity, cost, and organizational disruptiveness. As such, each of these levers may be worthy of further analysis and study.
The study results have encouraging implications, suggesting that a simple, easily mass-produced and implemented poster may yield measurable improvements in discharge outcomes simply by hanging it in patients’ rooms. This provides further evidence in support of the basic behavioral economics insights that inform nudge theory (35), while also underscoring another equally important tenet: The most reliable way to determine which nudge efforts work and how well they work is by conducting as much rigorous, relevant outcome research as possible.
Strengths and Limitations
Key strengths of this study include its applied nature, testing a concrete intervention in a major metropolitan children’s hospital. Focus group insights were derived from a participatory, bottom-up manner, leveraging the perspectives of active and experienced staff who bring a wealth of day-to-day experience and tacit knowledge. Such an approach is critical for both generative (brainstorming) and evaluative (reality-testing) aspects intervention development, as it is informed by concrete domain experience and not merely by general principles or purely “academic” intuitions.
Another strength of our applied, clinical approach is that the type of intervention represented by The Way Home poster is viable in any clinical setting. Many interventions that have strong in-principle or in-laboratory benefits may prove impracticable in clinical settings, though this is not always obvious in advance. Despite a modest sample size, results demonstrate that it is both practicable and low-risk to implement this sort of intervention in a real hospital setting, such that it could be replicated elsewhere to realize the practical benefits suggested by this study and/or to accumulate further data (eg, meta-analytic estimates of intervention effects and factors that may moderate impact). Efforts like this are critically important, but so also are replication efforts.
Finally, another key strength of this project was its methodological features. A mixed methods approach was utilized that included qualitative focus groups to inform a small-scale randomized controlled trial aimed at supporting preliminary causal inferences about the efficacy of The Way Home poster as a nudge intervention for increasing discharge-related readiness and self-efficacy. In doing this, we endeavored to realize the complementary and mutually informing strengths of 2 very different methodological paradigms, first to understand our specific contextual problem set (Study 1) and then to test the efficacy of our intervention with a rigorous experimental design (Study 2). This design yielded actionable insights of both a qualitative and quantitative nature, illustrating how different methods can be applied to address practical problems in a real hospital setting.
The limitations of this study are perhaps obvious, but there is value in stating them directly. First, our focal dependent outcome variables consisted of questionnaire-based caregiver self-reported perceptions. We did not directly measure concrete discharge-related behaviors, mastery of discharge information, or post-discharge outcomes. Despite this real limitation, there is strong, diverse methodological evidence for the general validity of well-designed self-report questionnaires, along with extensive evidence that domain-specific self-efficacy perceptions are closely linked to behavioral outcomes in those same domains. Though we lack concrete behavioral data or long-term outcome data for our particular intervention participants, the broader evidence base from self-efficacy theory demonstrates that personal efficacy perceptions do predict behavior and are not “just talk” (33). A second caveat is that more research—in other settings, with more and different caregivers, and (ideally) performed by other independent research teams—is desirable to determine the robustness of our results.
Supplemental Material
Supplemental Material, Supplement_A - Nudging Discharge Readiness With a Poster: A Sequential, Exploratory Mixed Methods Pilot Study of Patient Caregivers
Supplemental Material, Supplement_A for Nudging Discharge Readiness With a Poster: A Sequential, Exploratory Mixed Methods Pilot Study of Patient Caregivers by Laura L Leets, Jennifer Cahill, Amber M Sprenger, Juli Simon Thomas, Rob Hartman, Mary E Poyner Reed, Haylee Manning, Marge Britt, Chrissy T Vu, Nicholas W Kohn, Sandi Aguirre, Sanith Wijesinghe and Sybil Klaus in Journal of Patient Experience
Footnotes
Authors’ Note
Laura Leets and Jennifer Cahill contributed equally to this article. This research met the Boston Children’s Hospital local Institutional Review Board criteria for minimal-risk activities with human subjects and was deemed “exempt” from federal regulatory requirements (Protocol Number: P00029267). Patient consent was not required.
Acknowledgments
Special thanks are in order for La Toya Hardy, who helped us finalize the design of the Way Home poster.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This research was supported by MITRE’s innovation program (PRS # 20-1970).
Supplemental Material
Supplemental material for this article is available online.
Note
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
