Abstract
The purpose of this study was to describe the use of opioids and complementary and alternative medicine (CAM) among uninsured free clinic patients. A self-administered paper survey was collected to describe the use of opioids, complementary, and alternative medicine, and other pain relievers from 877 free clinic patients from January to April 2018. The US born English speakers are more likely to use CAM, nonprescription pain relievers, and prescription opioids, and to be more knowledgeable about opioids compared to non-US born English speakers and Spanish speakers. The main source of opioids for free clinic patients is a health care facility other than a free clinic as well as friends. Although nonprescription pain relievers are commonly used among free clinic patients, CAM is less common to use for pain control. More health education programs are needed to increase the knowledge of opioid risks among free clinic patients as well as other underserved population.
Introduction
The number of deaths from opioid overdose has been increasing since the 1990s, with a significant increase since 2013 (1). Approximately 40% of opioid deaths are caused by prescription opioids (2). Opioids are often prescribed for controlling chronic pain (3). Prescription opioid abuse is predominantly found among white patients (4). Due to the complexity of this issue, it is also challenging to discern how the opioid crisis affects insured versus uninsured individuals. Because health care for uninsured individuals is limited to specific settings as emergency departments and free clinics, uninsured patients may have fewer opportunities to be prescribed an opioid. Additionally, uninsured people are less likely to utilize health care services than people with insurance (5).
A previous study on opioid risks among uninsured individuals using a free clinic indicated several gaps in opioid-related research (6). First, opioid abuse among Hispanic free clinic patients needs to be further examined because there is little research regarding this population. Second, since free clinics do not necessarily prescribe opioids, it is important to determine the possible sources of opioid obtainment among free clinic patients. Third, given that prescription opioids are primarily used for pain control, it is important to examine what nonopioid pain relief free clinic patients are using to better understand free clinic patients and pain relief.
In addition to prescription opioids for pain relief, complementary and alternative medicine (CAM) is utilized for pain control (7). Although CAM is not always effective, several studies found that CAM is effective in controlling pain in some cases (8). In fact, pain is the most common reason to use CAM in the United States (8,9). However, little is known about uninsured individuals’ use of nonopioid pain relievers such as Ibuprofen or Tylenol or CAM. The purpose of this study is to describe the use of opioids and CAM among uninsured free clinic patients. In particular, this study focused on differences by ethnicity/nativity/language spoken, information related to obtaining prescription opioids, and the use of CAM and nonopioid pain relievers. This study increases knowledge, which is currently lacking, about prescription opioid use among uninsured individuals. Since opioid misuse is a significant public health issue (1), examining understudied populations can be worthwhile to develop effective prevention strategies. Additionally, it is hypothesized that there may be protective factors among populations not as heavily affected by the opioid crisis, and this study seeks to examine and better understand these factors. This study was conducted in the state of Utah, which has higher opioid-related overdose deaths, as well as opioid prescriptions than the national average (9,10). Utah was ranked 22nd regarding age-adjusted opioid overdose deaths in 2017 (10).
Methods
Setting
This study was approved by the institutional review board of University of Utah. Data were collected at a free clinic in a metropolitan area of Utah. For un- or underinsured individuals or undocumented immigrants, a free clinic is often the only health care facility in which they are able to seek medical care, other than emergency departments (11). The clinic, where this study was conducted, has been providing free primary care services to uninsured individuals in poverty, mostly aged 19 and 64 since 2005. The clinic has 10 paid staff and over 400 volunteers. All physicians, except the medical director, are volunteers. The clinic provides the following services: adult family medicine, pediatric care, assistance obtaining medications, adult and childhood immunizations, on-site laboratory offering a full range of lab tests, X-ray, ultrasound and screening mammograms, women’s health, diabetes specialty clinic, and healthy living classes. Although the free clinic does not prescribe opioids, there is an increasing concern about opioid abuse among its patients because the clinic is in the area where opioid abuse is prevalent. Approximately half of the patients self-identify as Hispanic.
Compared to the results of the national survey on free clinics (12), the characteristics of the patients of this clinic have some similarities in terms of being uninsured, mostly ages 18 and 64 and being in poverty. However, this clinic has a higher percentage of Hispanic patients than the national average (25.1%). In addition, while 41.9% of free clinic patients are homeless in the nation, the clinic where the current study was conducted does not serve homeless patients because there is another free clinic that treats only homeless people in the same city.
Study Participants and Data Collection
Eligible participants were adult patients of the clinic who spoke English or Spanish. Patients who did not speak English or Spanish were not included due to limited translation ability because the patients of the clinic are from more than 50 countries and speak a wide variety of languages. Since this survey was self-administered, patients with limited literacy were not included. An interviewer-administered survey was not performed because of a lack of privacy in the waiting room and resources. The majority of the clinic’s patients speak English and/or Spanish. All survey materials were available in English and Spanish. A translator translated English materials into Spanish. Another translator performed back-translation from Spanish to English to ensure the accuracy of the forward-translation. Three translators were used to review the accuracy of each translation. None of the translators involved were nationally certified. Research assistants approached all potential participants in the waiting room and answered any questions that potential participants had regarding the survey. Patients who expressed interest in participating in the survey received a consent cover letter and the survey instrument. Each participant selected a preferred language. Consent was obtained from each participant. The research assistants verified each participant filled the survey only once. Participants received a small gift (eg, reusable washcloths, US$1 or less value) when they completed the survey.
Measures
The survey questions are presented in Appendix.
Measures related to CAM or opioids
There was one question about oral herbal remedy “Do you currently take or have you ever taken an oral herbal remedy (herbal medicine)?” (13). In addition, for each type of the following types of CAM, participants were asked whether they used the medicine/supplement/therapy in the past 12 months: vitamins/supplements, herbal medicine, dietary/nutritional therapy, massage, meditation/relaxation exercises, chiropractic, acupuncture, yoga, cupping, curanderismo, tai chi, Espiritismo, hypnosis, and Santeria.
Communication regarding CAM use with physicians was measured by a 4-item questionnaire using a 5-point Likert scale (5 = strongly agree, 1 = strongly disagree) (14). An example of the 4 item is “I feel comfortable telling my doctor about complementary and alternative medicine therapies I use or might use.” Twelve items were asked (true/false/I don’t know) to measure levels of the knowledge of opioid overdoses (eg, “Long-acting opioids are used to treat chronic “round the clock” pain” (15).
General health and demographic characteristics
Self-rated general health was asked using a 5-point Likert scale. The following sociodemographic questions were also asked: age, gender, race/ethnicity, educational attainment, employment status, marital status, nativity, years in the US (non-US born only), and being a patient of the free clinic for 2 or more years (or not).
Data Analysis
Data were analyzed using IBM SPSS ver 22. The analyses were primarily based on the comparison of the following 3 groups: US born English speakers, non-US born English speakers, and Spanish speakers because previous studies at the free clinic suggest the 3 groups reported different levels of substance use and opioid risks (6). The 3 groups were compared by Pearson χ2 tests for categorical variables and analysis of variance (ANOVA) tests for continuous variables. These analyses were descriptive and did not test association among variables. All variables are listed on the tables. Only completed surveys were included in the analysis. P value denotes significance from Pearson χ2 tests between categorical variables (for cell size ≥5 only), and ANOVA tests for continuous variables comparing US born English speakers, non-US born English speakers, and Spanish speakers. Logistic regression analysis was conducted to examine the associations between opioid or CAM use (dependent variables) and sociodemographic characteristics (independent variables).
Results
Table 1 summarizes the sociodemographic characteristics of participants (N = 887—US born English speakers n = 199, non-US born English speakers n = 191, and Spanish speakers n = 497). Nearly 70% of the participants were female (67.6%). The most common race/ethnicity among the participants was Hispanic/Latino/Latina (68.1%) followed by non-Hispanic white (n = 170, 19.2%). The percentage of people having had some college or higher educational attainment was much lower among Spanish speakers (33%) than US born (52.3%) and non-US born (51.3%) English speakers. Spanish speakers (49.7%) had a higher percentage of being employed than US born (40.7%) and non-US born (40.3%) English speakers. The US born English speakers (21.6%) had a much lower marriage rate compared to non-US born English speakers (53.9%) and Spanish speakers (50.3%). Approximately one-quarter of the participants were US born (24.6%). Non-US born participants were from 34 countries. The most common country of origin was Mexico (n = 274) followed by Venezuela (n = 64), Peru (n = 38), El Salvador (n = 26), and Tonga (n = 22). The percentage of being a patient of the clinic for 2 years or longer was highest among Spanish speakers (52.3%) followed by non-US born English speakers (n = 86, 45%) and US born English speakers (24.6%). Spanish speakers (mean = 47.60, standard deviation [SD] = 13.86) were older than non-US born English speakers (mean = 45.79, SD = 15.92) and US born English speakers (mean = 41.26, SD = 13.68). A post hoc Tukey test indicated that US born English speakers were significantly younger than non-US born English speakers and Spanish speakers at the .05 level. But there was no significant difference in age between non-US born English speakers and Spanish speakers. The average self-rated health status was 3.18 (SD = 0.96). Age has a few very old participants (older than 70, n = 35) but also has some skewness toward younger participants. Therefore, there are outliers. Years in the United States were skewed toward shorter years. Overall health of the sample was skewed toward poorer health.
Sociodemographic Characteristics of Participants and Descriptive Statistics.a
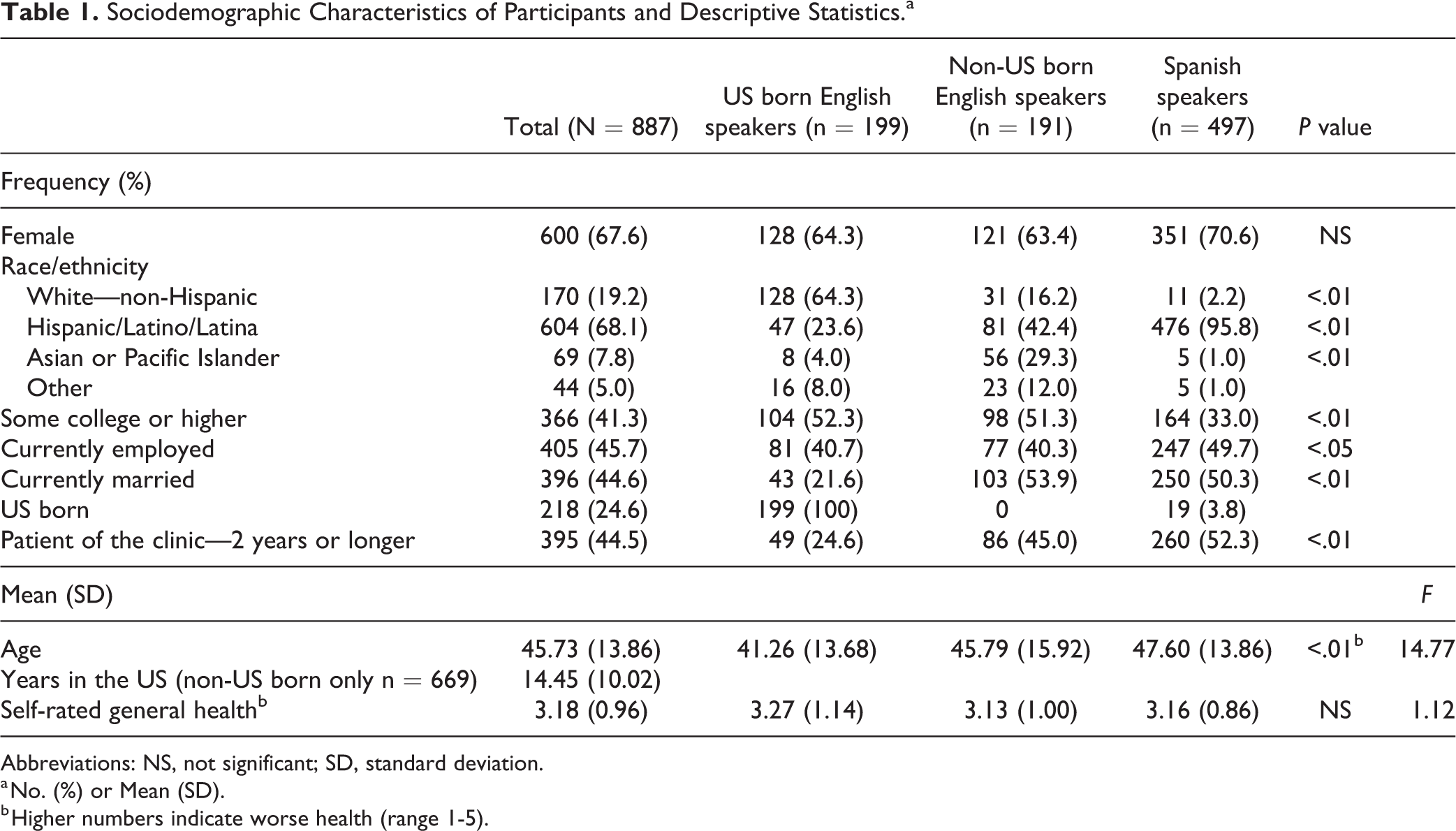
Abbreviations: NS, not significant; SD, standard deviation.
a No. (%) or Mean (SD).
b Higher numbers indicate worse health (range 1-5).
Table 2 presents the use of CAM and pain management among the participants. More than one-third of the participants had used oral herbal remedies (35.5%). The percentage of having used oral herbal remedy was highest among US born English speakers (42.2%) followed by Spanish speakers (36.6%) and non-US born English speakers (25.7%). The most common CAM used in the past 12 months was vitamins/supplements (59.2%) followed by herbal medicine (19.1%). Slightly less than one-quarter of the participants had used CAM to control pain (23.6%). The US born English speakers (29.6%) had a higher percentage of having used CAM to control pain than Spanish speakers (23.7%) and non-US born English speakers (16.8%). Nearly 70% of the participants preferred nonprescription pain relievers (68%).
Use of Alternative Medicine and Pain Management Sociodemographic Characteristics of Participants and Descriptive Statistics.a,b
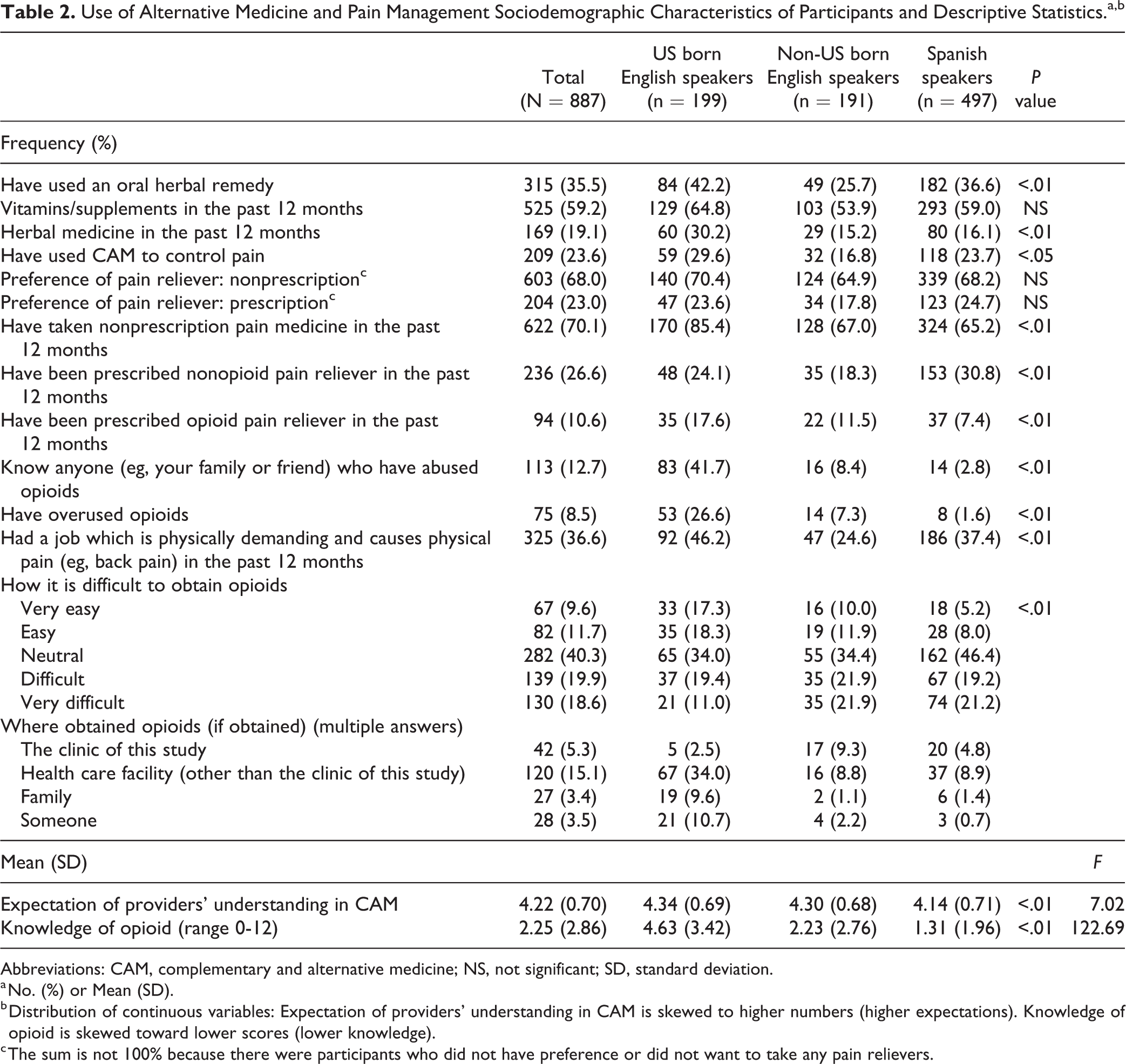
Abbreviations: CAM, complementary and alternative medicine; NS, not significant; SD, standard deviation.
a No. (%) or Mean (SD).
b Distribution of continuous variables: Expectation of providers’ understanding in CAM is skewed to higher numbers (higher expectations). Knowledge of opioid is skewed toward lower scores (lower knowledge).
c The sum is not 100% because there were participants who did not have preference or did not want to take any pain relievers.
In the past 12 months, participants reported the following prevalence for each type of pain reliever: having used a nonprescription pain medicine (70.1%), having been prescribed a nonopioid pain reliever (26.6%), and having been prescribed an opioid pain reliever (10.6%). The US born English speakers reported a higher percentage of knowing anyone who have abused opioids (41.7%) than non-US born English speakers (8.4%) and Spanish speakers (2.8%). Likewise, US born English speakers reported a higher percentage of having over-used opioids (26.6%) than non-US born English speakers (7.3%) and Spanish speakers (1.6%).
Furthermore, the prevalence of manual labor employment was analyzed. The US born English speakers reported a higher percentage of having a job which is physically demanding and causes physical pain in the past 12 months (46.2%) than non-US born English speakers (24.6%) and Spanish speakers (37.4%). Additional analyses were conducted to examine the associations between opioid or CAM use and sociodemographic characteristics using logistic regression. There was no difference in being prescribed opioids in the past 12 months by sociodemographic characteristics. Participants who had some college or higher educational attainment were less likely to have used herbal medicine in the past 12 months (P < .01).
Over one-third of US born English speakers (35.6%) believed it would be easy or very easy to obtain opioids while the percentage was lower among non-US born English speakers (21.9%) and Spanish speakers (13.2%). The most common place where participants had obtained opioids was a health care facility other than the clinic of this study (15.1%). The second most common place was the clinic of this study (5.3%), although this is inaccurate as the clinic does not prescribe opioids. The US born English speakers had higher levels of expectations of providers’ understanding in CAM and of knowledge of opioids compared to non-US born English speakers and Spanish speakers.
Discussion
This study described the use of opioids and CAM among uninsured free clinic patients. There are 3 main findings. First, US born English speakers are more likely to use CAM, nonprescription pain relievers, and prescribed pain relievers including opioids and to be more knowledgeable about opioids compared to non-US born English speakers and Spanish speakers. Second, the primary source of opioids for free clinic patients is a health care facility. Third, CAM is less common to use for pain control in comparison to nonprescription pain relievers.
The results of this study suggest that in comparison to non-US born English speakers and Spanish speakers, US born English speakers have a higher likelihood of utilizing CAM, nonprescription pain relievers, and prescription pain relievers including opioids. Additionally, this group was shown to be more knowledgeable about opioids. Previous studies suggest that immigrants have a lower prevalence of substance use than US born populations (16). Likewise, among free clinic patients, US born English speakers have a higher prevalence of substance use than non-US born English speakers and Spanish speakers (17). It is important to implement opioid abuse prevention programs for free clinic patients, in particular US born English speakers, given that our study does demonstrate opioid misuse among the groups, although at different rates.
National data suggest that the primary sources to obtain prescription opioids among non-Medicaid populations are friends and relatives (4). This study, however, concluded that the main source of obtaining opioids among free clinic patients is a health care facility other than a free clinic. It is important to note that a small number of participants reported that they obtained opioids from the clinic of this study (although the clinic does not prescribe opioids). The reasons of the misunderstanding should be further explored.
In terms of pain control and CAM or other nonopioid use, CAM was not commonly used, while nonprescription pain relief was common among participants. Previous studies suggest that higher levels of educational attainment and income are associated with greater CAM usage (18). Complementary and alternative medicine can be costly in certain areas, such as the cost associated with a massage or going to a chiropractor. All of the participants of the current study lived in poverty. This might have affected less use of CAM. Because the participants in this survey were free clinic patients, there may be a correlation between socioeconomic status and use of CAM. The use of nonprescription pain relievers was more common. Nonprescription pain relievers, such as Tylenol or Ibuprofen, are low cost and easy to obtain. In fact, the clinic of this study offers many over-the-counter pain relievers to the patients, free of charge. This issue of managing pain among free clinics needs to be further examined.
Although this study contributes to increasing the knowledge about opioid use, CAM, and nonopioid pain relievers among free clinic patients, it has limitations. This study is descriptive and does not examine causal relationships among factors. There is a possibility that some of the study participants did not understand the questions or possibly mistook an opioid for another medication, such as Ibuprofen. Further research is necessary to clarify the levels of understanding of types of pain medications among the free clinic population. Additionally, the over-use of opioids is a socially sensitive topic. Thus, some participants might have chosen socially desirable answers. This may be especially applicable for undocumented immigrants. However, this study did not ask immigration status.
Since the participants were not asked their pain levels and diagnoses, some of the participants of this study may not have pain that they are required to control. Additionally, study participants may have diagnoses for which opioids are indicated (severe, cancer-related pain, or end-of-life care, etc). The list of types of CAM was extracted from the Ho et al’s (14) study that was conducted in Southeast Asia (13). The majority of participants of this study were not from Southeast Asia, however. Finally, since a prescriber monitoring program was not possible, as the clinic preferred to be anonymous, it is unknown how the self-report was correlated with the actual report. In particular, it is not clear that the participants could accurately define opioids, other drugs in the survey, and CAM. Because the motive for opioid use was not assessed, it cannot be known why a person may be using an opioid. Finally, since the translators for the current study were not nationally certified, future research projects should use certified translators.
Although it is known that Hispanic individuals have a lower rate of opioid use compared to non-Hispanic whites and non-Hispanic blacks, it is unknown exactly what factors influence this trend and what pain medications Hispanic individuals are utilizing instead of opioids (19). Further research is necessary to examine the racial and socioeconomic factors within the opioid epidemic. Such studies should aim at better helping diverse populations in this subject matter avoid any stereotype or discrimination against particular populations of color. Cultural competence related to CAM may also be important to further explorer. This study builds knowledge and creates a platform for further research on the topic of pain management techniques and opioid use among free clinic patients. For example, future studies may examine the communication between patients and providers regarding opioids, stress relief, and lack of pain management, and the role of use/nonuse of CAM/pharmaceuticals.
Supplemental Material
Supplemental Material, CAM_opioid_appendix - The Use of Complementary and Alternative Medicine Strategies, Opioids, and Nonsteroidal Anti-Inflammatory Drugs (NSAIDS) Among Patients Attending a Free Clinic
Supplemental Material, CAM_opioid_appendix for The Use of Complementary and Alternative Medicine Strategies, Opioids, and Nonsteroidal Anti-Inflammatory Drugs (NSAIDS) Among Patients Attending a Free Clinic by Akiko Kamimura, Sullivan Howard, Shannon Weaver, Samin Panahi and Jeanie Ashby in Journal of Patient Experience
Footnotes
Authors’ Note
Patients who expressed interest in participating in the survey received a consent cover letter and the survey instrument. Each participant selected a preferred language. Consent was obtained from each participant. This study was approved by the University of Utah institutional review board. Data were collected at a free clinic in a metropolitan area of Utah.
Acknowledgments
The authors want to thank the patients who participated in this study and acknowledge the contribution of the staff and volunteers of the Maliheh Free Clinic. In addition, the authors thank Guadalupe Aguilera, Sara Dewitt, Travis Dixson, Tuane Ellis, Maria Reyes, and Shiya Zeng for their help in data collection, data entry, or translation related to this study. This project was supported by the Undergraduate Research Opportunities Program (UROP) at the University of Utah (Sullivan Howard).
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This project was funded by the Sorenson Legacy Foundation (PI: Akiko Kamimura).
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
