Abstract
The objective for this initiative was to reduce parental anxiety and thus improve their satisfaction related to hospital admission by ensuring that the child’s management plan and basic amenities were communicated to the parents within the first hour of arrival at the Children’s Hospital inpatient unit. The intervention for this project was developed based on the Theory of Change framework. Effectiveness of the intervention was assessed by comparing change in parent-reported anxiety scores and improvement in patient satisfaction scores at 24 hours post-admission as an indicator of experience. The frequency of delivery of each individual message was also tracked and compared at baseline and post-intervention. The results showed a significant reduction in parental anxiety levels within the first 24 hours of admission (3.5 to 3.2, P = .01). The parent satisfaction score was significantly improved from baseline to post-intervention (4.00 vs 4.82 respectively; P < .001). Comparison between the baseline and post-intervention demonstrated a statistically significant (P < .001) increase in frequency of messages delivered. This initiative highlighted that reengineering the current system using existing resources to standardize admission communication along with an adequate monitoring and feedback plan can help reduce parental anxiety, thus improving parent satisfaction with the services.
Introduction
The Institute of Medicine describes 6 key dimensions for an effective health system, which include safety, effectiveness, efficacy, equitable, timely, and patient centered (1). Recently, there has been a considerable shift toward prioritizing patient experience by catering to the emotional needs of the patients through reducing their anxieties, as it is critical to improving clinical outcomes as well as patient satisfaction with health-care services (2). Coulter described patient experience in terms of relational and functional dimensions (3). The relational dimensions pertain to the quality and continuity of care services, while the functional dimensions deal with the physical and environmental needs of the patients and their families (3). A multisite survey by Harris et al reported that ambience of the care facility and housekeeping facilities was among the top 3 determinants of patient satisfaction (4). In a review of patient satisfaction studies, Al-Abri and Al-Balushi reported that clear communication skills and information delivery were rated to be more important than technical skills and competence (5).
With respect to the pediatric population, parent/caregiver experience determines overall satisfaction with care. A large survey of approximately 50 000 parents with an inpatient pediatric admission experience in the United States reported that from the parent’s lens, caring for the sick child encompasses physical treatment and recovery and also includes “family-centered” issues such as the availability of amenities, ensuring a comfortable stay for the child, and flexibility with visitors schedule correlated strongly with patient satisfaction (6). However, literature reporting quality initiatives that focus on parent experience of perceived quality of care in low- and middle-income countries is limited. In August 2017, a baseline survey using questions from Health Consumer Assessment of Healthcare Providers and Systems form was conducted on parents of 221 admitted patients at the Children’s Hospital, The Aga Khan University (AKU), Karachi, Pakistan. Approximately 40% of the parents stated to be “extremely stressed,” as they felt that they had not received adequate explanation regarding their child’s clinical condition from the nurse or doctor. It appeared that although the current messages regarding basic amenities for the parent and child and child management plans are part of standardized hospital protocols, inconsistent communication during admission process, lack of monitoring data for these messages, and incomplete feedback loop to the staff regarding these led to inadequate message delivery and the parent being unhappy with the admission process. Despite demonstrating effectiveness in health-care provider behavior change, audits and feedback loops have been inconsistently adopted and implemented in health-care settings (7). Hysong et al have reported that tailored feedback with an emphasis on the task at hand can prove to improve effectiveness of intervention delivery (8).
In light of this evidence, the purpose of this initiative was to implement a standardized communication and monitoring plan with a feedback loop to achieve the following objective: To reduce parental anxiety related to hospital admission process by informing parents regarding care plan and basic amenities available for the child and the parent at the Children’s Hospital within the first hour of arrival in the inpatient unit
Methods
A quality initiative approved by the University’s Ethical Review Committee (2019-1749-4563) was conducted at Children’s Hospital, AKU. AKU is a 700-bed quaternary care private teaching hospital located in one of the largest and most populated (∼28 million people) cities of Pakistan. It is one of the main health-care facilities providing specialized care in the province of Sind. The pediatric ward at AKU has approximately 120 beds with 8000 admissions per year, majority of which occur through the emergency department. The initiative site for this work was the pediatric ward which has 31 general and 20 semi private beds with a nurse bed ratio of 1:6 and annual admissions of 3000. As the hospital protocols are different for the intensive care areas, these units were not part of this initiative.
Resources
The core team included managerial representatives from each cadre involved in information delivery (ie, service coordinator, business manager, head nurses, residency coordinator, and faculty). This team finalized the messages that would be part of this initiative. Several training sessions (20 sessions with 10-20 participants in each) were conducted for the staff over 2 months (February-March 2018). The participants included 10 unit receptionists, 10 security guards, 130 nurses, and 104 trainee physicians. The 1-hour interactive sessions used various teaching and learning strategies such as role-plays and 30-second videos (developed in-house) to demonstrate the style and content of message delivery. Verbal and structured written feedback obtained from the trainings was used to improvise subsequent sessions that were conducted after a month following which they were conducted on an ad hoc basis.
Intervention
The intervention plan for this project was developed based on the Theory of Change (TOC) framework to create a sense of certainty for the parents by making them aware of the hospital system and by providing them assurance that the hospital system knew about their child (Figure 1). The standard messages to be given in the first hour of admission to the pediatric ward were related to communication by the team physician regarding child’s current condition at the time of first assessment in the ward, and clinical management plan, along with information regarding visitors policy, basic amenities such as prayer area, availability of child and attendant meals, and patient safety and comfort messages (demonstration of use of call bell and side rails) that were delivered by the unit receptionist and nursing staff.

Implementation framework for this initiative.
Evaluation Strategy
To ensure a standardized communication that would be sustained beyond the project, detailed monitoring plan was developed according to the RACI (responsible, accountable, consulted and informed) matrix (Table 1) (9). The tasks were assigned as per the following categories:
RACI Matrix for the Intervention.

Abbreviations: A, approver; C, consulted; I, informed; R, responsible.
a These include unit receptionists, security guards, bedside nurses, and trainee physicians.
Responsible: the person who performs the task
Approver: the person who is accountable for the task
Consulted: the person who provides the information to get the task done
Informed: the person who needs to be informed regarding the progress of the task
Some team members were assigned responsibility of being leads who included service coordinator, chief resident, and head nurses for the ward area, while the managers including the nurse manager and business manager were the ones accountable. Weekly reports were sent to the team leaders and managers of each cadre for targeted intervention on the information that lagged behind by the lead author with recommendations for improvement.
Data Collection
Parents of children admitted to the general pediatric ward were informed regarding the purpose of this initiative, and verbal informed consent was obtained following which a short survey was conducted. A dedicated staff was hired to collect the data on a smart phone-based application that synced to a service management dashboard on the computers of the core team and managers for transparency. For data collection, the survey staff obtained a list for all admissions in the past 24 hours from the ward counter and approached the patient’s family for consent for data collection. Parents were asked to rate their anxiety level on a scale of 1 to 5 (lowest to highest) at admission and 24 hours post-admission along with their satisfaction level (on a similar scale). Interview was conducted 24 hours post-admission. Questions designed to assess patient and family’s receipt of the information provided were asked in the local language, and answer choices included “yes, no, maybe, don’t know, or not applicable” (refer to supplementary information for the survey). Once completed and synced, an overall score (maximum = 73) was generated. If the total score on this survey was 58 to 73 (≥80%), the bed appeared green for a score of 37 to 57 (50%-80%), the bed appeared yellow for the score of less than 37 (50%), and the concerned bed was highlighted in red color on the dashboard for quick feedback to the service coordinator and head nurse for ensuring transparency (Figure 2).

Dashboard developed for data monitoring and visualization.
Quality Checks
As the intervention progressed, random checks using a predesigned checklist were performed by the core team and team leads to assess the communication style of the staff and provide supportive supervision (refer to the supplementary file). Baseline data were collected between April and July 2018, while post-intervention data was collected from February 2019 to May 2019. Effectiveness of the intervention was assessed by change in parent anxiety levels and improvement in satisfaction with admission process using Student t test during the specified period. Frequency of delivery of each individual message at baseline and post-intervention was compared via χ2 test.
Results
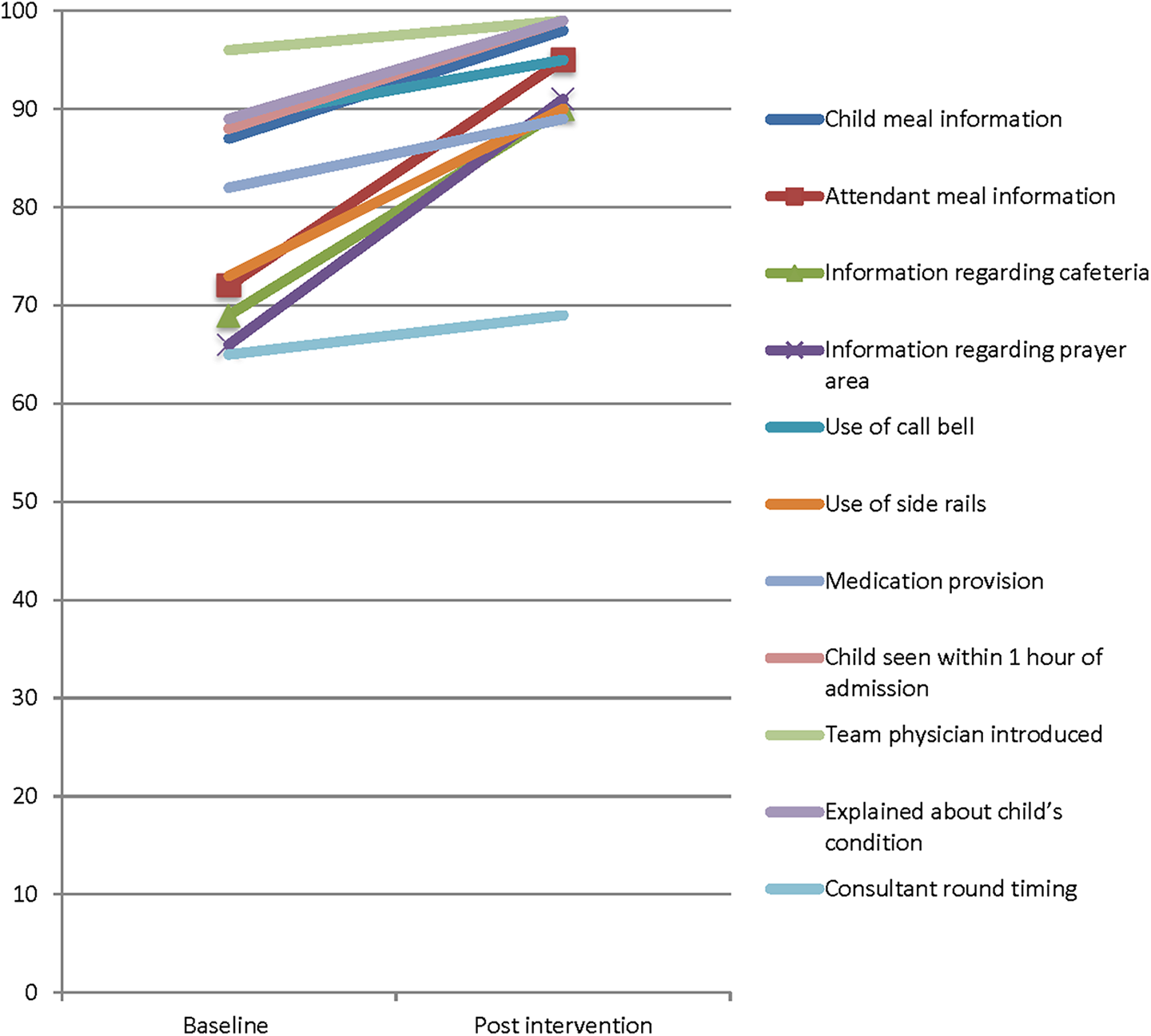
Baseline data for percentage of individuals who received the messages was available for 471 parents, while the post-intervention data on these indicators were available on 380 parents. The trends of these indicators at baseline and post-intervention have been shown in Figure 3. Majority of the patients were between 1 and 5 years of age (n = 565, 31%) followed by infants between 1 month and 1 year of age (n = 400, 21%). All these patients were admitted to the pediatric ward at AKU Hospital. The most common diagnosis for these patients were infectious diseases (ie, upper and lower respiratory tract infections, enteric fever, etc) 66% followed by chronic or complicated GI issues 6%, congenital heart disease 5%, chronic or complicated pulmonary 4%, genetic metabolic 2%, and so on.
Supervisor checklist.
The intervention led to a significant reduction in parent-reported anxiety levels in the first 24 hours of admission (3.5 vs 3.2, P = .01). The parent satisfaction score significantly improved (4.00 vs 4.82, respectively; P < .001) with no statistically significant association between patient age and parental satisfaction. There was no difference in the pre- or post-anxiety scores (P value = .4 and .83, respectively) for parents of children admitted for acute illnesses versus those admitted for chronic/complicated conditions.
When the baseline and post-intervention frequency of messages was compared, all the indicators in the figure except for consultant’s round timings info were statistically significant (P < .001 vs P = .24, respectively).
Discussion
This quality initiative demonstrated that a simple intervention of a detailed monitoring and feedback plan resulted in consistent message delivery by staff within first hour of admission leading to a reduction in parental anxiety levels. Resource utilization would be an important consideration in low-resource health-care settings, where quality projects may be abandoned due to several human and financial constraints exist. An important aspect of this intervention was that this work was supported by the leadership and was aligned with the job description of the various cadres involved, and minimal new staff was hired to execute this work. This initiative reengineered the current system to ensure maximum efficiency of the cadres to communicate these messages according to the standard protocols, thus demonstrating a scalable model for similar settings.
Davies et al have reported that accountability and data transparency with the implementing teams using objective tools can help provide comparative analysis and are useful for quality improvement (10). Creating a standard operating procedure (SOP) has been shown to improve process outcomes in several industries (11). In a hospital setting, SOPs can help describe a certain clinical or management condition comprehensively, thus ensuring consistency in practices and substantial improvement in quality of care (12). Besides SOPs, matrices such as the RACI help identify specific tasks that need to be accomplished and the individual assigned for the task (13). Such tools have proven to be valuable in successful health transformation efforts (13). The current project demonstrated similar results where effective communication, clear SOPs, user-friendly data visualization, and regular feedback to the staff helped improve parent experience with the admission process. Due to the unpredictability around the physician’s round timings that may be encountered, this indicator did not show an upward trend. Despite being proponents of quality of care, physicians have known to report hesitance in participation in quality initiatives as such programs are perceived to have “misplaced priorities” in terms of patient care and add significantly to their clinical and administrative responsibilities (14). Albeit not studied for this particular initiative, the underlying reasons for this trend may be similar.
Similar results have been reported by Miceli and Clark, where effective communication regarding management plans as well as the physical and emotional needs of parents played a significant role in determining patient experience (6). Improving communication skills of front line health-care providers using interactive teaching and learning strategies has demonstrated improvement in parent satisfaction with care (15,16). A qualitative study on nurse–patient communication reported that this relationship was greatly influenced by the culture of the organization (17). With adoption of a patient-centered approach, the nurse–patient relationship can be fostered, which can translate into effective communication and improved patient experience (17). Effective communication between health-care providers and parents can further contribute toward reduction in parental anxiety (18). Using the existing evidence and feedback from our baseline survey, a consistent and standardized communication was ensured as a core component of this intervention.
Parents of children especially neonates, those undergoing surgical procedures, or admitted in intensive care units undergo significant anxiety and stress at the time of admission (19). Care of their child, separation from family, and lack of adequate amenities at the hospital are major factors that contribute to parents stress (19). These factors were kept in mind while designing the intervention to ensure that parents are made comfortable with the inpatient environment and also informed regarding the child’s medical condition. A recent review by Wensley et al described the Comfort ALways Matters framework to describe themes that determine patient and caregiver comfort in hospital settings (20). The central idea of this framework was that when care is revolved around individual’s needs, overall patient experience is seen to improve significantly. Some of the important themes included a physically clean environment with familiarity of the hospital surroundings and being well informed regarding the management plan of their loved one (20).
Our study reported similar findings, where parental satisfaction improved as communications regarding physical and emotional needs of the family were met. This study had several strengths and limitations. Firstly, the initiative was designed based on feedback from the parents. Intervention strategy was a clear SOP demarcating the role of each member which was aligned to their job description to ensure that staff does not feel overwhelmed thus ensuring sustainability of this initiative. The strategy was complemented with having interactive training strategies. The outcomes were tracked using a user-friendly data visualization platform to ensure easy interpretability and also ensuring transparency with the implementing team. The subsequent phase of this initiative aims to work on quality of message delivery by ensuring effective communication skills for all frontline staff involved in patient care at the Pediatrics Unit and also encouraging active use of live dashboards for message delivery for timely intervention by team leaders. This work had a few limitations. Firstly, this intervention was only conducted in the general pediatric wards at AKU, with the potential to scale up across the intensive care areas as well. Due to limited resources, all admissions could not be captured. There was lack of a control group in this study, and hence the attribution of the change in satisfaction and anxiety scores to the intervention may require further research with inclusion of such a group. The research team designed the tools used to evaluate the effectiveness of this initiative as the evaluation needed to be tailored to the intervention being delivered keeping in mind feasibility of the using the tools. Despite their simplicity and brevity, such tools have been shown to provide comprehensive information regarding the service being evaluated (21). The effectiveness of the workshops that were used to train the cadres and the dashboards were not analyzed systematically. A dedicated staff was hired to collect evaluation data and for the development and maintenance of the dashboards, leading to additional cost to the existing system.
Conclusion
This quality initiative has helped to demonstrate that a 2 pronged approach, that is, using simple interventions such as training staff for effective communication skills along with a clearly outlined governance strategy supported by data can help create behavioral change in hospital employees using minimal resources, thus leading to improved patient satisfaction in low-resource settings.
Supplemental Material
Supplemental Material, SUPPLEMENTARY_FILE_Pt_Ex - A Framework for Improving Parent Satisfaction With the Inpatient Pediatric Admission Process: Experience From a Low-Resource Setting
Supplemental Material, SUPPLEMENTARY_FILE_Pt_Ex for A Framework for Improving Parent Satisfaction With the Inpatient Pediatric Admission Process: Experience From a Low-Resource Setting by Zahra Hoodbhoy, Muneera A Rasheed, Farheen Sherali, Sehrish Hussain, Rahmat Hassan, Aneela Hameed, Rashid Ali and Babar Hasan in Journal of Patient Experience
Footnotes
Acknowledgments
The authors would like to thank all the families and staff of the Children’s Hospital, AKUH for their contribution in this initiative.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Supplemental Material
Supplemental material for this article is available online.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
