Abstract
Limited data exist describing how hospital discharge readiness checklists might be incorporated into care. To evaluate how assessing patient readiness for discharge effects discharge outcomes. We assessed hospitalized adults’ readiness for discharge daily using a checklist. In the first feedback period, readiness data were given to patients, compared to the second feedback period, where data were given to patients and physicians. In the first feedback period, 163 patients completed 296 checklists, and in the second feedback period, 179 patients completed 371 checklists. In the first feedback period, 889 discharge barriers were identified, and 1154 in the second feedback period (
Introduction
Many adults in the United States experience an adverse outcome posthospitalization (1 –3); in many cases, these events might be preventable with better efforts to prepare the patient for discharge (4). Problems preparing patients for discharge can be exacerbated by efforts to reduce hospital length of stay (3,5) but may also be due to the discordance between health-care providers’ perceptions of readiness for discharge and patients’ own assessments—with physicians tending to overestimate patients’ readiness for discharge (6,7). Even when concordant, patients often report they are ready to go home from hospital, but once at home they will face the reality of a range of postacute care challenges (8,9).
Galvin and colleagues recently defined key attributes of readiness for hospital discharge, noting that physical stability, psychological ability, and adequate support, information, and knowledge were central (5). Discharge readiness checklists have been developed to systematically identify medical, obstetric, and surgical patient-reported barriers to, and preparedness for, discharge (10 –13). Once completed, responses can provide a foundation to discharge planning that can ensure patient needs are ultimately addressed, resulting in an optimized hospital care transition. However, few data exist to describe how, and whether, these tools might be incorporated into care to improve the discharge process. This is surprising, given checklists are commonly used in clinical medicine and surgery to standardize processes and reduce variations in care (14,15). For example, checklists have been shown to improve clinical guideline adherence, communication among care providers as well as reduce adverse patient events (16,17). Therefore, we undertook this study as we hypothesized that the use of a checklist derived from patient-reported barriers to discharge would impact positively on patients’ discharge outcomes. Specifically, the aims of this study are to describe the impact of providing a daily discharge checklist to physicians regarding their patient-reported barriers to hospital discharge on the number of reported discharge barriers and readmissions. We also sought to understand physicians’ perceptions of the usefulness of this checklist.
Method
Study Design, Setting, and Participants
We conducted our study at the Universty of California San Francisco (UCSF) Medical Center —a 600-bed tertiary care academic medical center in San Francisco. We recruited patients in 2 time periods, the first between November 6, 2013, and April 28, 2014, and the second between April 29, 2014, and May 20, 2015.
Patients were eligible to participate if they were admitted to the general medicine service, aged older than 18 years, English-speaking, were cognitively able to provide informed consent, and were not under contact, droplet, airborne, or radiation isolation. Patients were eligible to participate regardless of where they were admitted from or expected to be discharged (eg, home, skilled nursing facility). Patients were excluded if they were in the intensive care unit, were delirious, or otherwise unable to provide informed consent. Trained research assistants who remained consistent throughout the entire study screened consecutively admitted patients charts daily to assess for eligibility and approached eligible patients to consent them into the study on their first or second day of hospitalization. We used an enrolment tracker to document reasons for patients’ exclusion or refusal. The UCSF Committee on Human Research approved our study (IRB15-18439).
Study Activities and Data Collection
Development of readiness for discharge tool
We adapted a Readiness for Hospital Discharge Survey (RHDS) previously used in obstetric, surgical, and medicine patients to assess patients’ readiness for discharge (10). We refined the domains of the RHDS tool to be more relevant to hospitalized medical patients (18). Our refined checklist included 12 items in 4 domains: physical status (ie, pain, mobility), self-care knowledge (ie, medications, problems to watch for, recovery plan), coping ability (ie, emotional support, who to call with problems), and expected support (ie, related to activities and instrumental activities of daily living) (18). Our adapted checklist was then pretested for face validity in a separate group of physicians, nurses, patients, and caregivers (18).
Readiness for discharge assessment protocol
All eligible patients were approached to participate in the study and those who consented were invited to complete our adapted readiness for discharge checklist at admission, which was either on their first or second day of hospitalization. The patient was then revisited daily (Monday through Friday) to obtain readiness data on subsequent days. Each patient was attempted to be assessed at least 3 separate times each day; checklist data were not obtained if the patient was out of room for procedures or tests, if the patient was noted to be confused or newly unable to complete the survey, or if they asked to not be assessed that day. This approach was followed for each patient on each hospital day until discharge.
Intervention design
Our patient-facing intervention involved 2 distinct feedback periods. During the first (patient only) feedback period, we collected readiness for discharge data and shared the results with the patient, though no specific guidance was offered other than to prompt the patient to discuss any concerns identified with their physician. During the second (both patient and physician) feedback period, we again shared information with the patient (along with encouragement to discuss the results with their providers); however, we also reported data back to patient’s primary physician team, including attending physician, by e-mail every day a checklist was completed. Following each patient’s discharge, we abstracted demographic, clinical, and 30-day readmission information from their electronic medical record.
Physician perceptions of usefulness of readiness data
We sent a short electronic survey to each attending physician who received discharge readiness checklist data during the second feedback period. The 5-item survey created specifically for our study asked whether the physician recalled receiving the checklist data or whether they looked at the e-mail and the usefulness of the data for discharge planning.
Study outcomes
Our primary study outcome is the mean number of patient-reported discharge barriers by hospital day in each feedback period. Secondary outcomes include number, and type, of discharge barriers reported on the day of discharge, 30-day hospital readmission, and physician perceptions of the usefulness of readiness checklist data.
Analytic Approach
We compared the demographic and clinical characteristics of patients in each feedback period using
Results
Following exclusions based on eligibility criteria by medical record screening, refusals, and inability to participate, there were 163 patients in the first (patient only) feedback and 179 in the second (patient and physician) feedback period (Figure 1). This translates to an enrolment rate of 12.1% and 6.7%, respectively (
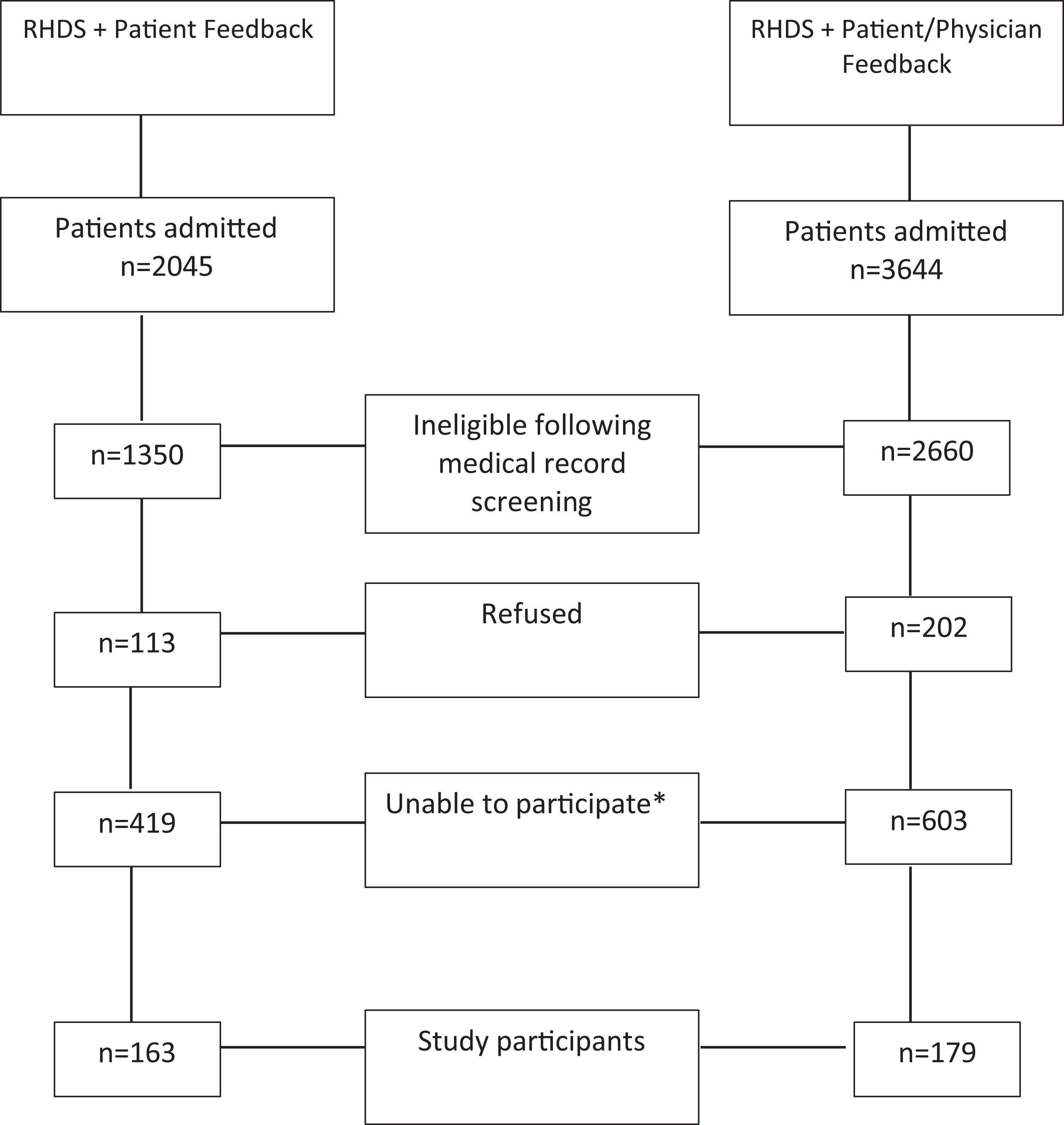
Study inclusion and exclusion flow diagram. *Reasons for inability to participate include impaired vision/physicality/communication, too sick, discharged before recruitment approach, violent, and homelessness.
Demographic and Clinical Characteristics of Participants.a

Abbreviation: SD, standard deviation.
a Data missing values do not equal 100%.
Barriers to Discharge Readiness
Patients completed a total of 667 surveys (296 in the first and 371 in the second feedback periods). On average, patients completed 1.82 surveys (standard deviation [SD] 1.10; range 1-8) in the first feedback period and 1.96 (SD 1.25; range 1-7) in the second feedback period (
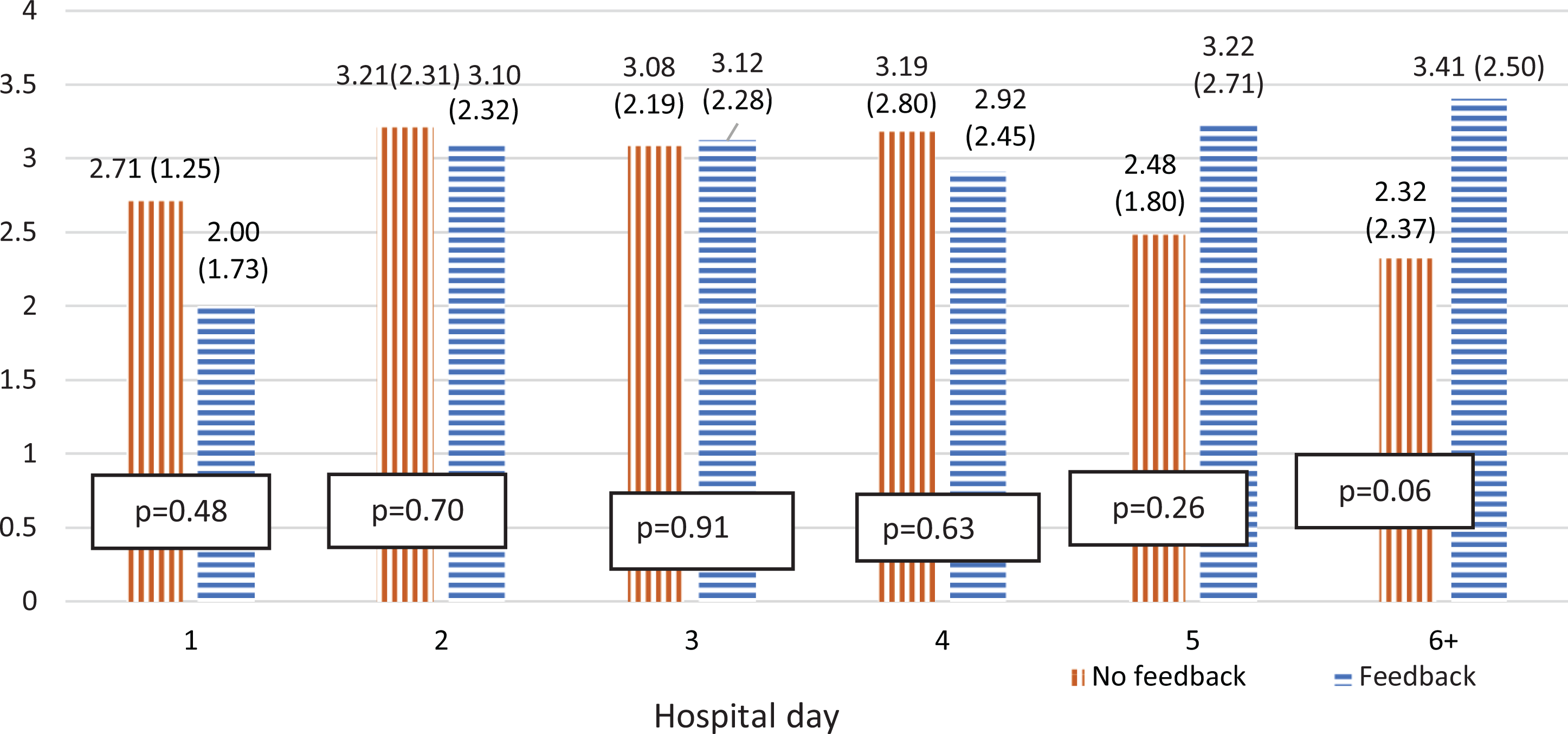
Mean (standard deviation) number of barriers per patient by hospital and group status.
Barriers at Discharge
There were 69 patients in the first and 83 in the second feedback periods who completed an admission and final survey (≤48 hours before discharge). For these subset of patients, those in the first feedback period completed significantly fewer surveys (2.46, SD 0.85) compared to patients in the second feedback period (2.92, SD 1.32;
Comparison of Individual Barriers Reported by Patients on Final Survey ≤48 Hours Before Discharge by Group.

Thirty-Day Hospital Readmission
In the second feedback period, lower 30-day readmissions (23/179, 12.8%) were reported compared to the first feedback period (29/163, 17.8%); however, this difference was not statistically significant (
Physician Perspectives on Receiving Readiness for Discharge Data
Eighty-nine physicians responded to our survey (79% response rate). Seventy-six (85%) recalled receiving the e-mail containing patients’ responses to the discharge readiness checklist, and of these, 66 (87%) stated they read the e-mails either “always” or “most of the time.” Only 23 (30%) of physicians who recalled receiving e-mails containing checklist responses thought that the data were useful for discharge planning and 45 (59%) stated the data “never” or “rarely” highlighted anything that was unexpected or that they were not already aware of.
Discussion
In our study, gathering structured assessments of discharge barriers using a checklist and providing these data to both patients and physicians did not appear to influence the number of challenges to transition home reported by patients. Although some barriers did appear to be reduced somewhat, none did so in a statistically significant manner and many patients were discharged with a number of unmet needs.
The lack of impact of our intervention may be due to a combination of factors. Many may relate to specific aspects of our intervention’s design. For example, eliciting discharge barriers and expecting patients to share concerns with their care team may be unrealistic, given patients may not comfortable asking questions, (19) may prefer to leave clinical care decisions to their doctor (20), or may not even have the opportunity to ask questions during interactions with their physician (21). The passive nature of how we informed physicians of discharge needs, electronically via e-mail, may also not be the most effective method to disseminate this information, especially during busy clinical ward attending times (22).
Feedback from physicians regarding the utility of the discharge readiness information suggested that most felt the data were not useful for discharge planning, with many stating they were already aware of the concerns raised. However, data from patients suggest that, despite physician awareness, patients' actual and perceived barriers remained prevalent up to the time of discharge. One interpretation of this discordance in physician and patient perceptions may represent a limitation in our feedback approach, in that we did not explicitly guide physician to clinical tools (eg, motivational interviewing (23,24)) or resources (eg, suggested referrals to case management) necessary to address patients’ barriers. Each discharge readiness criterion represents potential opportunities for training and engagement around thorny clinical issues (such as management of chronic pain) or challenging social and cognitive issues that might impact physicians’ perceived ability to address problems such as housing instability or lack of social supports. This is particularly true for many of the needs related to independent living, activities of daily living, or social determinants of health. Sullivan states that hospitals have an obligation to address these social determinants of health; however, structural and systemic barriers largely prevent hospitals having the capacity to address such issues (25).
An overview of strategies to improve the postacute care period noted that hospital–community partnerships are emerging as one meaningful way to help address postdischarge needs (26). Despite the presence of social work and case managers at our institution, resolution of these needs largely depends on the availability of outpatient social or community care services. In retrospect, without external resources to address the variety of potential nonclinical drivers or social determinants of health, hospital-based providers are never going to be able to impact on discharge barriers, perhaps explaining another reason for our negative findings.
Across both feedback periods of our study, discharge barriers remain pervasive and persistent with patients reporting unmet needs at discharge. In fact, patients in the second feedback period reported higher levels of unmet discharge needs, although this may be a reflection of this group completing significantly more surveys, which may have raised more awareness of, and comfort to, reporting discharge needs. One positive finding from our study was that patients’ understanding of their recovery plan improved in the second feedback period. It should be noted that this need is one that is entirely modifiable by physicians, suggesting a utility in our intervention, albeit for hospital-relevant needs that hospital-based providers can directly address.
Including other members of the patient’s care team in our intervention may have resulted in different findings. For example, sharing patient self-reported discharge barriers with nursing or social work staff, who are integrally involved in preparing patients for discharge, may have altered the education of patients during the discharge process, prompted question asking or reemphasized elements of self-care. Future studies could determine the impact of our intervention when all members of the patient’s care team involved in discharge planning are included. Similarly, understanding patient and caregiver perspectives of our intervention should also be a priority if we are to truly create patient-centered discharges.
In addition to the limitations outlined, it must be noted that our enrolment rates in both feedback periods were low, resulting in a highly selective study population. The fact that so many eligible patients were unable to participate for reasons, such as impairments, disability, and acute symptoms, suggest those enrolled in the study may not have the greatest needs. Our pre- versus poststudy design is also not optimal for rigorous intervention but highly appropriate for a pilot quality improvement-focused research study. Finally, although our adapted checklist was pretested for face validity (18), it has not undergone complete psychometric testing and validation.
In summary, our study found that patients were discharged from hospital with a variety of discharge needs that were not resolved during hospitalization. Provision of discharge readiness information to physicians was not successful at ameliorating postdischarge needs. Despite our overall negative study, hospital discharge processes and the transition from hospital to home remains a top priority for patients (27). As such, identifying interventions that can positively impact on the clinical and social needs of patients at this time should remain a focus for hospital-based providers and health-care systems.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
