Abstract
Patient satisfaction studies have gained more and more attention, and there are many patient satisfaction studies. These studies assume that patients were selected randomly and independently, but patient satisfaction surveys are described as a multistage or hierarchically structured sample. Thus, there is a need to conduct a hierarchical linear model (HLM) analysis with a large number of hospitals. This study utilized an HLM to investigate both the individual patient-level effect on the overall satisfaction rating and the effect of hospital characteristics on the combining process of patient’s overall satisfaction rating. This study used patient satisfaction data collected from 100 hospitals with the sample size of 85 766. The hospital-level characteristics include total expense per personnel, payroll expense per personnel, number of staffed beds per personnel, and number of admission per personnel. This study found that hospital characteristics influence overall rating of the hospital through the doctor, staff, and room attributes. When considering the complex nature of the overall patient rating process of hospitals, it makes more sense to analyze hospital characteristics that are interacting with attributes rather than treat hospital characteristics as independent of these factors.
Introduction
Patient satisfaction studies have gained more and more attention for several reasons. First, patients are considered as customers in health care (1). With more information available to patients, they have more power to choose their health-care providers. Satisfied patients come back to the same health-care providers and may recommend to their family members and friends. Second, for patients with chronic conditions, adherence to prescribed treatments is very important. Satisfied patients tend to adhere to a treatment (2,3). Third, patient satisfaction itself influences the reimbursement rate to health-care providers (4). This aspect is unique compared to other industries, and it affects the bottom line of health-care providers.
The focus of patient satisfaction studies has moved from identifying patient demographic characteristics that are related to their overall satisfaction (5,6) to identifying health-care attributes such as nursing care, physician care, and room amenities that are related to overall satisfaction (7 –9). These studies found that some attributes are more influential than others on overall satisfaction. In general, nursing care is most influential for a hospital setting, and physician care is most influential for an outpatient setting. The earlier patient satisfaction studies that focus on patient demographic characteristics are useful for case-mix adjustment, and the latter studies that focus on health-care attributes are useful for health-care managers to improve their patient satisfaction scores.
Although many patient satisfaction studies use solid methodologies and sound statistical analyses, most of them assume that patients were selected randomly and independently. When patients are selected from one hospital, this assumption may be acceptable. However, when patients are selected from many hospitals, there is a clustering effect, where patients may have a reason to choose a particular hospital (10 –13). Patients who are admitted to a particular hospital may share some unique experiences compared to patients admitted to another hospital. Individual observations are not completely independent. Thus, patient satisfaction data with multiple hospitals are considered as being organized at more than 1 level. The units of analysis are individual patients (at a lower level) who are nested within hospitals (at a higher level). In other words, there would be an organizational influence on which patients combine their attribute reactions to arrive at their overall satisfaction. In fact, patient satisfaction surveys are described as a multistage or hierarchically structured sample (11,12).
There are a few patient satisfaction studies that pay attention to the hierarchical structure of the patient satisfaction data. These studies point out that there is a need to consider a hierarchical model or multilevel analysis. They obtained hospital characteristics such as size (13), academic affiliation (13), special nursing staff (14), capital investment (15), and information technology (15). These studies agree that there is an organizational effect. One study used ratios such as average spending on employees and average spending per bed (12). Ratios can clearly describe the characteristics of hospitals and differentiate quality issues. For example, if a hospital hires more nurses, this hospital could have more time for patients than a same bed size hospital with fewer nurses. This study found an organizational effect (12). However, as there were only 10 hospitals in 1 small region in the study, the generalization of the study was limited.
Patients combine their attribute reactions to arrive at their overall ratings (7), and this combining process is the lower level. The combining process is influenced by hospital-level characteristics, and this influence is the higher level. These 2 levels are hierarchical and not in the same level. A multiple linear regression model can analyze only 1 level, but the hierarchical linear model (HLM) accounts for both lower and higher levels as different levels simultaneously. There is a need to conduct a HLM analysis with a larger number of hospitals in different regions with more patients to produce more generalizable findings.
Methods
Data Source
This study used patient satisfaction data collected from 100 hospitals representing a large, national, private, not-for-profit hospital system. The data were collected through regular patient experience surveys, including the Centers for Medicare and Medicaid Services (CMS)-prescribed collection protocol and the Hospital Consumer Assessment of Healthcare Providers and Systems (HCAHPS) survey. We also included questions gauging patient perceptions about the aspects of their experience thought to affect overall satisfaction and loyalty to the hospital provider. The HCAHPS instrument was created by the US Department of Health and Human Services, Agency for Healthcare Research and Quality (AHRQ). The AHRQ directed the RAND Corporation, Harvard Medical School, and the American Institutes for Research, together with Westat, to carry out a rigorous scientific process to develop and validate the HCAHPS instrument. The survey results (psychometric properties including validity and reliability, credibility, usefulness, etc) have been confirmed and published elsewhere (16,17).
The 100 hospitals in our study sample were located in the Midwest, Southeast, South, Northwest, and Northeast and represented a range of hospitals in size, services, and geography. Critical access, community, and tertiary hospitals were all represented in the data set. Data were collected by means of telephone interviews conducted on a constant and regular basis for each hospital. Patients discharged from each hospital were randomly selected and contacted, generally within a week, and they responded directly to the survey vendor. The survey vendor compiled the raw data and sent a data set to the health system’s central office. Response rates varied by hospital, but across all locations, the average response rate was 40%. This high response rate was achieved through the multiwave survey technique. The survey protocol requires up to 6 attempts to contact a sampled member. The study analyzed data collected between July 1, 2013, and October 31, 2014, from patients who were 18 years of age or older.
Measures
The dependent variable in this study is a single item that measures the overall rating of the hospital (ranging from “0” for the worst hospital possible to “10” for the best hospital possible). Four key independent variables (lower level) assessed patients’ experiences with “nursing care,” “physician care,” “staff care,” and the “hospital room.” Each of these 4 independent variables was considered to be a construct and was created with multiple survey items using a 4-point Likert-type scale (4 = always, 3 = usually, 2 = sometimes, and 1 = never) that measured the same construct. Specifically, we calculated each of the 4 independent variables (composite indexes) as an arithmetic mean of the survey items in the same construct. As long as there was at least 1 survey item responded to in a construct, the composite index was calculated. A representative question for nursing care is, “How often did nurses listen carefully to you?” (see Table 1 for a description of all items.) The reliability of each attribute (internal consistency) was assessed using Cronbach α coefficient. The Cronbach α coefficient for the room attribute was .376. Although this value is not large, there are only 2 items measuring room attribute. Thus, we decided to retain these 2 items.
Descriptive Statistics of Survey Items, Composite Indices, and Control Variables.

At the hospital level (higher level), information on each hospital’s total expenses, payroll, number of staffed beds, number of admissions, and number of personnel was available from the AHA Guide 2017 edition (American Hospital Association). By creating 4 ratio indices (total expenses per personnel, payroll per personnel, staffed bed per personnel, and admission per personnel), it was possible to investigate the effect of hospital characteristics that are related to patient care.
Control variables included patients’ gender, age, educational attainment, and race. The age variable was an ordinal scale—that is, 18-24, 25-29, 30-34,…, 90 or older. The educational attainment variable was also an ordinal scale: completed the eighth grade or less, completed some high school but did not graduate, graduated from high school or passed the general educational development (GED) test, completed some college or earned a 2-year degree, graduated from a 4-year college, and completed more than a 4-year college degree. The race variable was a dichotomous dummy variable for each race, with white used as the reference racial group.
Model and Analysis
An HLM was utilized to investigate both the individual patient-level effect on the overall satisfaction rating and the effect of hospital characteristics on the combining process of patient’s overall satisfaction rating. Thus, it was a 2-level HLM with level 1 being an individual patient effect and level 2 being a hospital effect.
Hierarchical Linear Model
This study specifies the 2-level model as follows. At the individual patient level, there are composite indices about nursing (Nur), Doctor (Doc), Staff (Sta), and Room (Rom) as well as control variables, gender (Gender), age group (Age), highest education level (Edu), and dummy variables, Asian (Asi), Pacific islander (Pac), Native American (Ind), and African American (Afr).
Level 1:

where
At the hospital level, the intercept term (β0
Level 2:

Results
There were 85 766 cases in the data set. There were more women (52 053, 61.9%) than men (32 028, 38.1%), and the largest racial group was white (62 771, 80.9%), followed by African American (10 566, 13.7%), Native American (5198, 6.8%), Asian (1503, 1.9%), and Pacific Islander (486, 0.6%). The age distribution was almost symmetrical, and the largest age-group was 60 to 64. The educational attainment variable showed that 2 groups (high school or GED and some college) were the largest groups (32.0% and 30.1%, respectively). The means and standard deviations of hospital characteristics and ratios are shown in Table 2.
Hospital Characteristics.
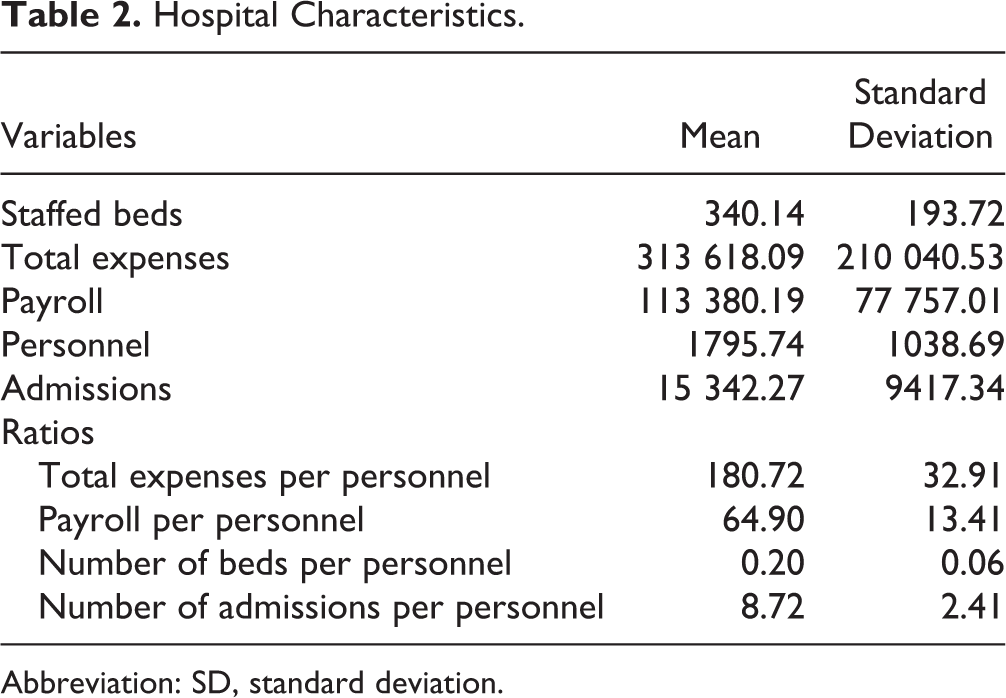
Abbreviation: SD, standard deviation.
Table 3 shows the parameter estimates, standard error of the estimates, and their respective
Result of Hierarchical Linear Model.

Abbreviations: AdmPP, number of admission per personnel; BedPP, number of staffed beds per personnel; PayPP, payroll expense per personnel; SE, standard error; TotPP, total expense per personnel.
The level-1 parameters are jointly affected by inherent intercept (γ
Discussion
The 4 attributes (nursing, doctor, staff, and room) are all positively related to overall rating, and are statistically significant at α = .05. Among those 4 attributes, the nursing care shows the largest coefficient (intercept), and it is much larger than the other 3 attributes. The lack of hospital-level effects in the nursing care attribute indicates the dominant effect of nursing care on overall rating regardless of the type of hospitals. This result is consistent with other studies for hospital patients (7,18). This study found that hospital characteristics influence overall rating of the hospital through the doctor, staff, and room attributes. The TotPP variable influences overall rating through doctor, staff, and room attributes. Hospitals that spend more money per personnel increase the doctor attribute weight positively toward the overall rating but decrease the staff and room attribute weights. It indicates that when hospitals spend more money in general budgets, patients are more influenced by the doctor attribute, while patients are less influenced by the staff and the room attributes. This finding may suggest that increased expenditures per personnel provide more funding for routine activities of physician care, especially documenting care and other substitutable care, which otherwise fall to physicians. The negative effect of spending per personnel on the staff and room attributes suggests that issues related to the staff actions or the room are less important to patients when greater expenditures overall are made. To better understand both phenomena, more detailed information on the nature of the expenditures is needed.
The admission per personnel variable influences overall rating through the doctor attribute. Hospitals with more admissions per personnel decrease the doctor attribute influence on the overall rating compared to hospitals with fewer admissions per personnel. This finding may suggest that in hospitals with more admissions per personnel increase the workload of all staff and hence shifts some routine activities for physicians which decrease their time for patient caring and communication. The payroll per personnel variable is not statistically significant with any of the 4 attributes, suggesting that a compensation level does not affect perceptions of the overall rating. Although the beds per personnel variable is not statistically significant with any of the 4 attributes either, it decreases overall rating through the intercept. Hospitals with more beds per personnel show lower overall rating than hospitals with fewer bed per personnel. There may be a possible shortage of personnel to take care of patients with relatively fewer personnel. The finding suggests that greater workload for all staff in general has a negative effect on the overall rating of a hospital.
Limitations and Suggestions
This study utilized a sound and advanced methodology in analyzing the data. However, there are several limitations. First, this is a cross-sectional study where dependent and independent variables were collected at the same time. Thus, it is not appropriate to infer a cause-and-effect relationship. This type of study can establish an association. Further studies that utilize a quasi-experimental design would be needed to clearly establish a cause-and-effect relationship. Second, this study analyzed 100 hospitals with 85 000 patients. The sample size is large, but the data came from 1 hospital system. There are different types of hospital systems. It is suggested that future studies are conducted on different types of hospital systems to generalize the findings of this study.
Conclusion
This study found that hospital characteristics influence patients’ overall rating of the hospitals through 3 attribute variables. Some previous studies included those hospital characteristics in the analysis, but these hospital characteristics were treated as control variables together with attribute reaction variables. Thus, attribute reaction variables and hospital characteristics variables were treated as all independent variables. This study used the hierarchical model approach and found these hospital characteristics do influence overall ratings through attribute reactions. These variables interact with each other. This is a new finding. Among the 4 attributes, nursing care (1.9127, 95% confidence interval [CI]: 1.5729-2.2524) is most influential followed by doctor care (0.4758, 95% CI: 0.1891-0.7625), room (0.4495, 95% CI: 0.2162-0.6829), and staff care (0.4281, 95% CI: 0.2463-0.6099). Nursing care is much more influential than the other 3 attributes, and this difference is statistically significant based on the nonoverlapping 95% CIs. There is little difference among the other 3 attributes, and these differences are not statistically significant based on the overlapping 95% CIs. Thus, to increase the rating of the hospital, nursing care should be improved first. Among hospital characteristics, the number of beds per personnel showed a strong negative association with overall rating of the hospitals. It is a noteworthy and convincing finding. The TotPP variable influenced overall rating through doctor care, staff care, and room. The number of admissions per personnel variable influenced overall rating only through doctor care. When considering the complex nature of the overall patient rating process of hospitals, it may not be appropriate to analyze data with a simple multiple linear regression. Rather, it makes more sense to assume that hospital characteristics are interacting with attribute reactions and not that hospital characteristics are independent from attribute reactions. This study clearly showed that hospital characteristics affect patients combining process of hospital attribute reactions and then influence patient overall rating of the hospitals.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
