Abstract
Background:
Hepatitis B virus (HBV) infection has a high prevalence rate in Nigeria. Disclosure of infection status to close partner and the public attracts support for infected people. This study looks at disclosure and social challenges of infected persons.
Methods:
Mixed methods of patients’ administered questionnaire and an in-depth interview conducted on HBV-infected respondents in a hospital in Nigeria were used. The study recruited all participants who satisfied the inclusion criteria. Data were entered into SPSS version 20 and analyzed using simple and inferential statistics and content analysis for the in-depth interview.
Results:
A total of 205 participants completed the questionnaire study. Mean (standard deviation) age was 35.3 (±11.0) years. There were 121 married, 37 singles with noncohabiting partners and 47 singles without partners with disclosure rates being 96.7% versus 97.9% versus 89.2%, respectively. Singles disclosed infection more to their parents while married respondents disclosed infection more to their spouses. Singles had high rate of denial of sexual relationship (22.6%), emotional trauma (34.5%), broken relationships (11.4%), and surreptitious use of contraception for protection (67.6%). Married respondents had the highest rate of HBV vaccination of their family members (40.1%). Infection prevention and allaying fears of family members were their counseling needs. In-depth interview revealed that infected respondents usually expressed shock and depression at a positive test leading to fear and deception that put close associates at risk.
Conclusion:
Hepatitis B virus–infected respondents have high rate of disclosure. Family problems of these people can therefore be solved through public enlightenment and individual counseling.
Introduction
Hepatitis B virus (HBV) is a hepadnavirus, and there are about 300 million infected people worldwide (1). Chronic hepatitis B (CHB) infection is endemic in Asia and Africa, and these 2 areas constitute about 75% of the world’s hepatitis B infection (1). Chronic hepatitis B is the leading cause of chronic liver disease in Nigeria (2,3). The prevalence rate of HBsAg among blood donors in Nigeria is between 10% and 15% (4), and sometimes could be up to 17% (5). This implies that about 18 to 27 million Nigerians are infected with the virus of the 180 million population.
The diagnosis of HBV infection as with other hepatitides usually disturbs a patient emotionally in the first few days of the test and can cause the infected person to hide the disease possibly leading to complications for the index case and the society (6 -8). In addition, members of the public usually express fear toward infected people because of the contagious nature of the virus, more so, as there are reports that the virus spreads in families where there is an infected person and among sexual partners (9 -13). When there is HBV infection in the family, mothers and the siblings are usually more affected. The male offspring as well as older children usually have a very high HBV viral load (14,15). The knowledge of HBV is high in families that are literate, and where there has been a previous experience of the infection. Knowledge of HBV is also high in families where members discuss with their friends about the infection (16). A report has shown that those who have HBV infection may not report or seek help if they have financial difficulty or are not on health insurance (17). On the other hand, disclosure of infection to a close partner and other people attracts support for infected people (18).
Hepatitis B virus infection is therefore a risk to the family and the society and infected people can hide their status. The knowledge of HBV in Nigeria is low among health-care professionals with the exception of medical doctors and therefore likely to be low in the general population (19).
Hepatitis B virus infection is endemic in Nigeria. There has not been any study to the best of our knowledge in Nigeria that looked at disclosure of infection among HBV-infected people, with the aim of reducing the spread of infection, by tackling the issue of nondisclosure and associated problems. The control of hepatitis B infection in Nigeria is important to sub-Sahara Africa if the World Health Organization projection to eradicate HBV by the year 2030 will succeed (20). This study therefore assessed disclosure of infection status within the family and among friends and their associates and the problems HBV-infected people face among these people. It specifically determined the proportion that disclose their infection, the pattern of the disclosure, and problems encountered in the family and among close associates and perceived areas of counseling needs.
Methods
This study employed a mixed method of study of patients infected with CHB presenting to a tertiary hospital in Southwest Nigeria. Patients who tested positive to HBsAg on routine laboratory tests for various medical reasons and referred to the gastrointestinal clinic of our Teaching Hospital were the target population. Chronic hepatitis B was diagnosed based on persistence of HBsAg for more than 6 months or absence of anti-HBC immunoglobulin M (IgM) and presence of immunoglobulin G in a patient who tested positive for less than 6 months. The mixed method consisted of 2 parts: A questionnaire answered by 205 participants and an in-depth interview conducted on another set of 25 respondents. The study period spanned from July 2016 to July 2018 to achieve our total sample size based on the turnout of patients with CHB seen in the gastrointestinal clinic. Sample size calculation for the questionnaire aspect was based on HBsAg prevalence rate of 15%, and this was arrived at using Fisher formula (21), n = z2p (1 − p)/d2 which puts the sample size at 195, and approximated to 200 cases. Inclusion criterion was a diagnosed case of CHB infection. All cases that fulfilled the inclusion criteria and consented to participate in the study were recruited. The questionnaire used was prepared after adequate review of the relevant literature by the authors. Face validity of the questionnaire was done by the authors to ensure that the questionnaire answered the set objectives. Pretesting was done among a population that was not included in the study.
Every diagnosed case of CHB infection that consented filled the self-administered questionnaire detailing biodata and length of period patient has tested positive to HBsAg. The questionnaire sought disclosure of HBV infection or otherwise to family and friends and the problems encountered. In addition, patients’ means of protecting others they live with, and their spouses, if married or has a sexual partner (for unmarried respondents) were sought. The patients’ concern and areas of counseling needs were inquired. Viral HBV-DNA quantitative value viral load was obtained from among investigations carried out by the patients and recorded in a proformat to assess the infectivity potential of respondents. The questionnaires were given out to respondents by 2 of the authors and trained resident doctors in our gastrointestinal clinic.
A qualitative in-depth interview was conducted on 25 patients with CHB with disclosure problems that were identified from among cases that filled the questionnaire for the quantitative study. They were purposively selected to participate in the qualitative interview. The interview was conducted by the lead author using an in-depth interview guide to get a view of participants’ experience of how the diagnosis of HBV was made and disclosure to family members and the problems encountered. It also sought patients’ opinion on how the problems could be solved. The study was approved by the Ethics and Research committee of the hospital with number; IRB/IEC/0004553 and NHREC/27/02/2009a.
Data Analysis
Data were entered into SPSS version 20 and analyzed using simple descriptive and inferential statistics. Frequencies and means were generated from patients’ responses and the results were presented in tables and figure. Categorical variables of responders were compared in tables for a clear representation of the different categories of respondents.
The qualitative data were analyzed through rapid review of the field notes identifying major pattern and preliminary themes. The in-depth interviews were transcribed with transcripts edited for accuracy. Study objectives were used to develop themes with grounded theory used till saturation was reached. Content analysis was thereafter done.
Results
Questionnaire Results
A total of 205 cases completed the study. The age range of the respondents was 18 to 72 years with a mean (standard deviation, SD) of 35.9 (11.0) years. There were 122 (59.5%) of 205 males and 83 (40.5%) of 205 females (male:female ratio of 1.5:1). There were 121 (59%) of 205 married, 78 (38%) of 205 singles, 5 (2.4%) of 205 widows, and 1 (0.5%) of 205 divorced. Civil servants 90 (43.9%) of 205, Yoruba ethnicity 190 (92.7%) of 205, and people with tertiary level of education 159 (77.6%) of 205 constituted the majority of the respondents. The mean HBV-DNA viral load of respondents was 5.7 × 10 6 IU/mL. Thirty-four (16.6%) earn income less than the minimum wage of US$50 dollars per month (Table 1). A total of 70 (34.1%) of 205 used condom, while 1 (0.5%) of 205 practiced abstinence since the diagnosis of HBV. The respondents were subdivided into 3 categories of married, 121; singles without sexual partners, 47; and singles with noncohabiting sexual partners, 37. Among all respondents, 197 (96.1%) of 205 disclosed their HBV status to various categories of family members. The disclosure pattern for the categories of the division was 97.9% versus 89.2% versus 96.7% for single with noncohabiting partners, singles without partners, and the married, respectively.
Basic Demographic Characteristics of Questionnaire Respondents.
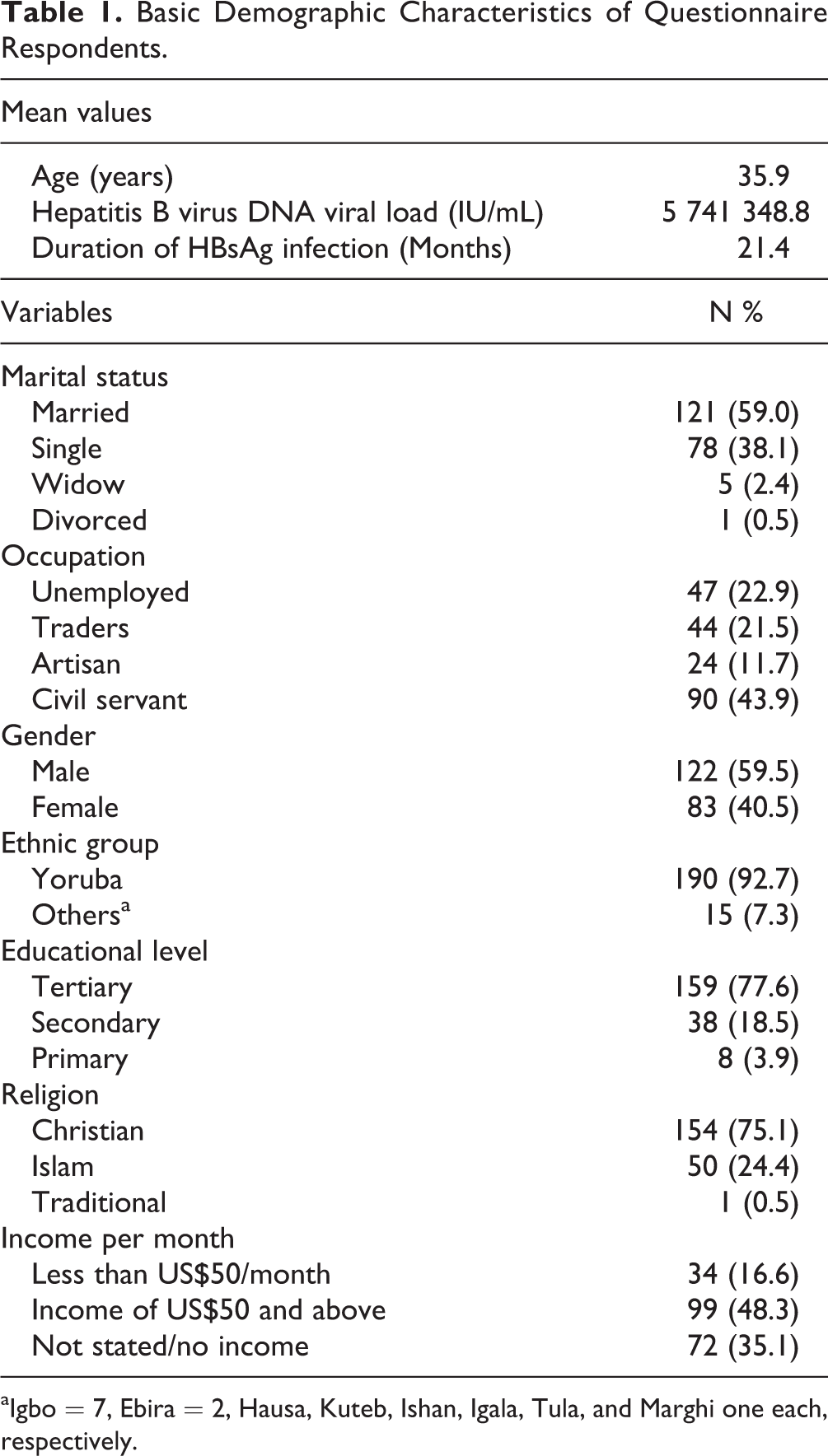
aIgbo = 7, Ebira = 2, Hausa, Kuteb, Ishan, Igala, Tula, and Marghi one each, respectively.
Among singles with noncohabiting sexual partners, those who were males had the highest percentage of HBV disclosure. They commonly disclosed to their parents. However, 7 (16.2%) of 37 reported that HBV had affected their relationships with others. The 7 respondents had broken relationships with their sexual partners. Twenty-five, 25 (67.6%) of 37, did not disclose reasons for use of male condom to their partners. This practice was seen only among males. These singles with noncohabiting sexual partners reported that their HBV infection was affecting people they relate to than other respondents. Areas of their counseling needs were how to prevent infection and allay fears in the family (Figure 1, Table 2 and Table 4).

Histogram representation of singles with hepatitis B virus (HBV) and areas affected in their life.
Comparison of Responses of Respondents in the Questionnaire Group.

Abbreviation: HBV, hepatitis B virus.
Among the group of infected singles without current sexual partners, only 2 (4.3%) of 47 reported that HBV had affected their relationship with others. Affected areas included delay in marriage, 1 (2.2%) of 47; difficulty in disclosing HBV status, 1 (2.2%) of 47. Broken relationship with a partner had occurred in 3 (6.4%) of 47 and as many as 18 (38.3%) of 47 had emotional trauma. Seventeen (26.2%) of 47 desired that their family members be counseled. How to prevent infection, allay fears in the family and understand HBV disease were the areas of their counseling needs (Table 2, Table 4, and Figure 1). They reported more emotional trauma and the need to counsel those they live with than other respondents.
Among the married, disclosure was high (96.7%) but was lower than male respondents that were single (63.1%). Married respondents reported the highest number 50 (41.4%) of HBV vaccination of their family members (Table 2). Seven (7/121) reported that HBV infection had affected their marriages. Among these 7, 4 couples said that it had stopped their sexual life in the marriage, while the other 3 couples both had HBV infection with their partners. In order to reduce HBV infection, 45 (37.2%) of 121 among the married respondents encouraged the use of condom, and among this number, 4 (3.3%) of 121, who were males, their partners were not aware of the reason for the use of the contraceptive. How to prevent infection in the family was the most important area of counseling need (Table 2). A test of association between disclosure of infection status among all respondents and age, marital status, educational level, religion, ethnicity, income, and having a sexual partner or not were found not to be significant, P > .05 (Table 3).
Demographic Characteristics of Respondents and Disclosure.

Abbreviation: HBV, hepatitis B virus.
aFisher exact test. Igbo = 7, Ebira = 2, Hausa, Kuteb, Ishan, Igala, Tula, and Marghi one each, respectively.
Interviewed Group Themes Selected Exemplar Quotations.

Abbreviation: HBV, hepatitis B virus.
In-Depth Interviewed Group Results
The interviewed group participants were 25, with age range of 21 to 46 years. The mean (SD) age was, 31.6 ± 6.9 years. Eleven (44%) were married and 14 (56%) were single. Fourteen (56%) were males and 11 (44%) females. They had an average period of HBV infection of 9.5 months and had made disclosure to an average of 3 family members. The mean HBV viral load was 27 × 106 IU/mL, and the number of sexual partners per respondent ranged from 1 to 10 in number (Table 5).
Singles With HBV and Areas Affected in Their Life.a

Abbreviation: HBV, hepatitis B virus.
aPresented in Figure 1.
Respondents got tested for the following reasons: medical tests for febrile illness, antenatal visit, visa application, general medical tests, pre-employment tests, predonation blood tests, staff screening exercise, and the mandatory national youth service medical tests. Most respondents expressed shock at a positive test thinking it was transmitted sexually as some of them claimed they were not sexually active or promiscuous. One respondent said, I carried out a pre-visa medical test, I tested positive to hepatitis B, I took my girlfriend to the same hospital thinking she infected me, she tested negative. (26-year-old male pharmacy technician)
The news of a positive test was followed by weeks of depression and fear that the illness was likely to kill soon.
One respondent said “I noticed that my fiancée was always mute and not happy, she thought I was the cause of her infection.” (39-year-old male Engineer)
Disclosure of HBV to the family
Those who disclosed fell under 2 broad categories. The first category were those who disclosed because of the wish to take care of themselves as well as those seeking information, and those who had fear of dying soon from the disease.
A respondent said: “When I was diagnosed of hepatitis B infection, I felt bad. When I travelled home, I told my parents and siblings. What I now want is how I can be cured of this virus.” (25-year-old male trader apprentice).
The second category were those who were fearful and disturbed at a positive test, those thinking of a possible stigma, and those who see the disease as a private affairs. This second category restricted disclosure to few people or none.
One respondent said: “I did not disclose the diagnosis to any person, because it is a private affair. I should find solution to it. At home I used condom for my wife whenever we had sex. I told her I was using the condom to prevent unwanted pregnancies.” (46-year-old male driver)
Impact, participants’ opinion, and suggestion for cure of HBV nondisclosure
Some responders said that testing positive was a devastating experience, their family members were equally devastated. This devastating experience was common with partners of single respondents who knew what HBV was all about but was not reported with partners of married respondents. Respondents with some knowledge of HBV, especially men, used contraceptive on their wife/sexual partners without disclosing the reason for its use. The family of married respondents on the other hand encouraged them to seek medical attention.
A woman said: “I was diagnosed at the antenatal clinic, I felt depressed thinking how I came about this infection. I told my husband, mother, and siblings, they encouraged me to come to the hospital.” (30-year-old married female trader).
On the issue of solution to HBV nondisclosure, a respondent opined that there was lack of information about HBV making people who test positive unable to take a decision. Many of the respondents said that the populace need enlightenment campaign to make people to be aware of HBV Table 6.
Sociodemographic Characteristics of the Interviewed Group.

Abbreviations: HBV, hepatitis B virus; SD, standard deviation.
Discussion
The study recruited 205 cases for the questionnaire aspect. There were more males than females which could possibly mean that males are exposed to the risk factors for acquiring HBV infection than females. This pattern is similar to a study from China that reported more men than women with CHB (22). Among all the respondents, the disclosure rate was 96%. This figure was very high and mainly among males who were single than the married respondents, but overall, married respondents disclosed infection more than the singles put together.
The reason for the high rate of disclosure among singles may be because of the emotional trauma they had and they needed people to relate with and disclose their HBV infection to. This may also be the reason why singles with or without sexual partners had a high rate of disclosure to their parents than other respondents. They probably see their parents as confidants. However, for outsiders, such as their sexual partners, they used contraceptives without disclosing the reason behind its use to them. In a report by Huang et al (22), respondents with CHB had felt that they were undesirable as spouses and brought troubles to their families, and 16% regretted disclosing their status. In another report by Rafique et al (23), marital relationship was affected in 51% of HBV- and HCV-infected people who had told their spouses their status. This pattern may be similar to the behavior of the singles in this study that disclosed their HBV status more to their parents than other people seen in the questionnaire group while the interviewed group revealed that those who were fearful and thought of possible stigmatization restricted disclosure to family members. It is also possible that some did not disclose because they were devastated because of the diagnosis of HBV. The circumstances under which the hepatitis test was carried out may in part explain the different reactions of respondents seen in the questionnaire group. Depression and fear of death could be another reason why some did not disclose their status to family members.
The response of the singles also show the need of their life at this stage, marriage and whether they were desired by people around them or not. Their relationship with their parents and family friends stand out despite HBV infection, evident by the low rate of denial of body contact. However, they had so many broken relationship and denial of sexual relationship, which may explain their behavior toward the opposite sex, exhibiting deceptive tactics. The situation these singles found themselves probably resulted in emotional trauma had more by those not into any relationship at the time of the study than those who were into one relationships or the other with the opposite sex. This is also reflected in the areas of their counseling needs, predominantly to prevent infection and allay fears. These findings may support the study by Scriphanlop et al (24) that opined that in screening for HBV, emphasis should be on privacy because fears of disclosure are distinct to Africans. Our study showed that disclosure rate was high but not to their sexual partners. This however does not agree with the report by van der Veen et al (25) that showed that having been screened for HBV was related to getting married among Dutch respondents. It also looks like those who disclosed did so to get help for treatment or solution to the problem of HBV while those who did not probably see CHB infection as a private affair as revealed by people in the qualitative group.
The disclosure level among the married respondents was high and was mainly to their spouses and less to their parents, relations, and friends. The disclosure rate was more than that reported among people with HIV, HBV, and diabetes by Kittner et al (18), where the disclosure level was up to 84% for HBV. Disclosure of infection to close partner and the public environment is often followed by supportive reactions from people toward those who have the disease (25). The high rate of disclosure among married people may be responsible for the low rate of reporting that their HBV infection had affected others to a significant level. This may equally support the report by Ishimaru et al (26) that when infected people disclose their HBV status, it was attended by positive attitude from those who are close to the respondents. However, there were still some who used contraceptive devices for which the partners were not allowed to know the reason behind such use. It is also possible that the use of contraceptive may be for other purposes other than the prevention of HBV infection. The interviewed group however revealed that married couple who exhibited fear after testing positive to HBV or were afraid to make disclosure to their wives commonly engaged in this practice. It is also pertinent to note that the reactions of a positive family member from this study was for the partner to avoid sexual relationship. Hepatitis B virus can be transmitted through several other means, and many had very high viral load from the study. Three married couples both had HBV infection and could have occurred through other routes than the sexual route.
The high rate of HBV vaccination among the married respondents may be part of the way to protect the family or could possibly be due to fear of infection. These fears could possibly have reflected in the high rate of the need to counsel those they lived with, and particularly in the area of infection prevention and allay fears in the family. It is also possible that those who had good knowledge of HBV thought more about possible complications of the virus. This could be a strong reason for nondisclosure in the questionnaire group, or the devastation effect of a positive HBsAg test. Good family support as revealed in the qualitative study could be one reason married people did not report that HBV infection affected their marriage to a large extent compared with the singles. The possible explanation for the behavior of these Nigerians to HBV is most likely the knowledge of the general public about the virus. A recent population-based awareness study of HBV in Nigeria found the awareness of the virus to be low and this correlated with the poor attitude and practice of the people toward HBV (27). It is therefore possible that the high disclosure rate and inappropriate behavior exhibited by our respondents could be explained by their level of knowledge and awareness of HBV.
Limitations of the Study
Some respondents could have given socially acceptable responses in the questionnaire study and the in-depth interviewed even though they were assured of the purpose of the study.
Conclusion
Disclosure among HBV-infected patients is averagely high and it is seen more among married than single respondents put together. Singles with HBV infection make disclosure more to their parents while the married make disclosure more to their spouses. There was a high rate of denial of sexual relationship, emotional trauma, and surreptitious use of male condom and broken relationship among singles, while married respondents had a high rate of HBV vaccination of their family members. Prevention of infection and allaying fears in the family was counseling needs common to all respondents.
It is recommended that HBV-infected people should be engaged in a constructive discussion to know their level of disclosure and counsel them appropriately. Public enlightenment as well as implementation of pretest and posttest counseling is also advocated as a way to address problems related to disclosure among infected people.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
