Abstract
To enhance student learning, many health profession programs are embracing involvement of patients in their curricula, yet little is known about the impact of such an experience on patients.
Objective:
To understand the experiences of patients who contributed to the creation of a Verbatim Reader’s Theater used in health professions curriculum.
Methods:
A semi-structured interview was conducted with a focus group of 3 patients who participated in curriculum development. The interview was recorded, transcribed verbatim, and analyzed for themes using van Manen approach to hermeneutic phenomenology.
Results:
Five themes emerged: (1) contextualizing contribution, (2) addressing expectations, (3) changing health-care service delivery, (4) sharing common experiences, and (5) coordinating participation.
Conclusion:
Patients had a positive experience contributing to curriculum development and found meaning in sharing their lived experience to shape the values of future clinicians. Strategies to promote continued success in partnership between patients and health professional curriculum developers include clear communication about the project’s direction and early discussion of patient role and expectations.
Keywords
Introduction
The concepts of patient-centered care and embedded patient partnerships have been embraced as a foundation for quality health-care encounters; however, the challenge of operationalizing this overarching philosophy is well recognized (1). In this health-care delivery model, the patient is recognized as an equal contributor to the health-care team, with unique expert knowledge informed by their lived experience (2). Although the health-care field has been evolving to integrate patient partnerships over the past 2 decades, an appreciation for the role of partnerships between patients and health-care educators has lagged. Patients have traditionally been seen as the object of learning in both the classroom and at the bedside; however, roles are evolving to more active teaching (3). Additionally, communication in the field is challenged by inconsistent terminology where patients have been described as clients, health mentors, service users, consumers, and corresponding variation in perceptions and roles. For the purposes of clarity, this article will use the term “patients” to describe those who have experienced health challenges resulting in engagement with the health-care system, although the authors recognize the inherent power differential this term creates.
In the evolving field of patient engagement in curricula, there is a growing body of literature addressing the perspectives of stakeholders (4 –8). Within this body, there is a call to develop approaches to patient engagement that are rooted in theories, have enhanced conceptual clarity, and to employ rigorous evaluative methodologies in order to improve the outcome (9). Patients participate in health professions curricula at the invitation of educators, often with limited or no financial remuneration. They are generally seen as providing important contributions to the student-learning process, yet have often not been recognized as partners in the educational process. Moreover, since educators focus primarily on understanding the curricular impact on student learning and implications for knowledge transfer to future health-care practices, they rarely explore the impact on patients. Those who have suggest that patients who participate in curriculum development appreciate the opportunity to share their knowledge and feel empowered; however, these studies are few and lack rigor (10). An appreciation of the impact on patients, as well as the enablers and barriers to participation, will advance an understanding of the notion of partnership.
An opportunity to study the patient experience during curriculum development arose in 2016 when a group of patients was involved in creating an addition to the interprofessional education (IPE) curriculum for health profession students at the University of Toronto. The goal of IPE is to develop student competencies related to team-based collaboration among professionals as well as with patients and family members. A group of health profession students (2 occupational therapy, 2 medicine, and 1 speech-language pathology), guided by a faculty member, interviewed patients and practitioners to generate a Verbatim Reader’s Theater (VRT) script, which would be used to explore an understanding of partnerships in health-care delivery. Verbatim Reader’s Theater blends 2 types of theater: Verbatim Theater and Reader’s Theater. Verbatim Theater is a type of documentary theater where a script is constructed exclusively with words from interviewed subjects (11). In Reader’s Theater, audience members read from a script without the use of props, sets, or costumes, and typically engage in a facilitated critical discussion of the script’s content (12). As a combination of the 2, VRT offers an opportunity for students to cognitively engage in a text-derived directly from participants. The script, built on the interviews with 5 patients and 3 health-care practitioners, as well as accompanying discussion questions, was added to the IPE curriculum (13). All script informants were invited to attend the curriculum session which used their contribution. Upon completion, the authors, with the addition of 1 more faculty member, explored the lived experience of the patient contributors.
Purpose
The purpose of this study is to explore the experiences of patients who contributed to curriculum development (VRT script) at the University of Toronto.
Methodology
The authors selected a hermeneutic phenomenology approach, as developed and described by van Manen, to analyze the transcribed interview texts because of its attention to exploring meaning. This methodology focuses on describing how the human experience of a phenomenon was lived, as well as its effect on the person (14). Hermeneutic phenomenology allows researchers to reduce the experiences of many individuals who have interacted with a phenomenon into a description of its essence. The foundational interpretive philosophy that underpins this approach allows meaning to arise from emergent descriptions and human constructs (15). The University of Toronto Research Ethics Board granted approval for this study.
Informants
They were originally recruited to contribute to the curriculum development through their work as volunteers in the Health Mentor Program, where they shared their experiences with chronic illness and the health-care system with health profession students from the University of Toronto (dentistry, kinesiology and physical education, medical radiation sciences, medicine, nursing, occupational therapy, pharmacy, physical therapy, physician assistant, social work, and speech-language pathology) on a longitudinal basis. Three of the 5 patients were available and consented to participate in this study. Patients included 2 females and 1 male ranging in age from 40 to 65 years. All 3 live with chronic illnesses (2 living with rheumatoid arthritis and 1 living with Crohn disease). One of the 3 patients attended the first iteration of the curriculum.
Following implementation of the curriculum, investigators conducted a focus group with the patients, allowing them to build off one another’s lived experiences as they reflected on their own (16). The focus group lasted approximately 1 hour and used a semi-structured interview guide (Appendix A) followed by probing questions. Discussions were recorded and transcribed within 1 week. Pseudonyms were used in the transcription to enhance anonymity.
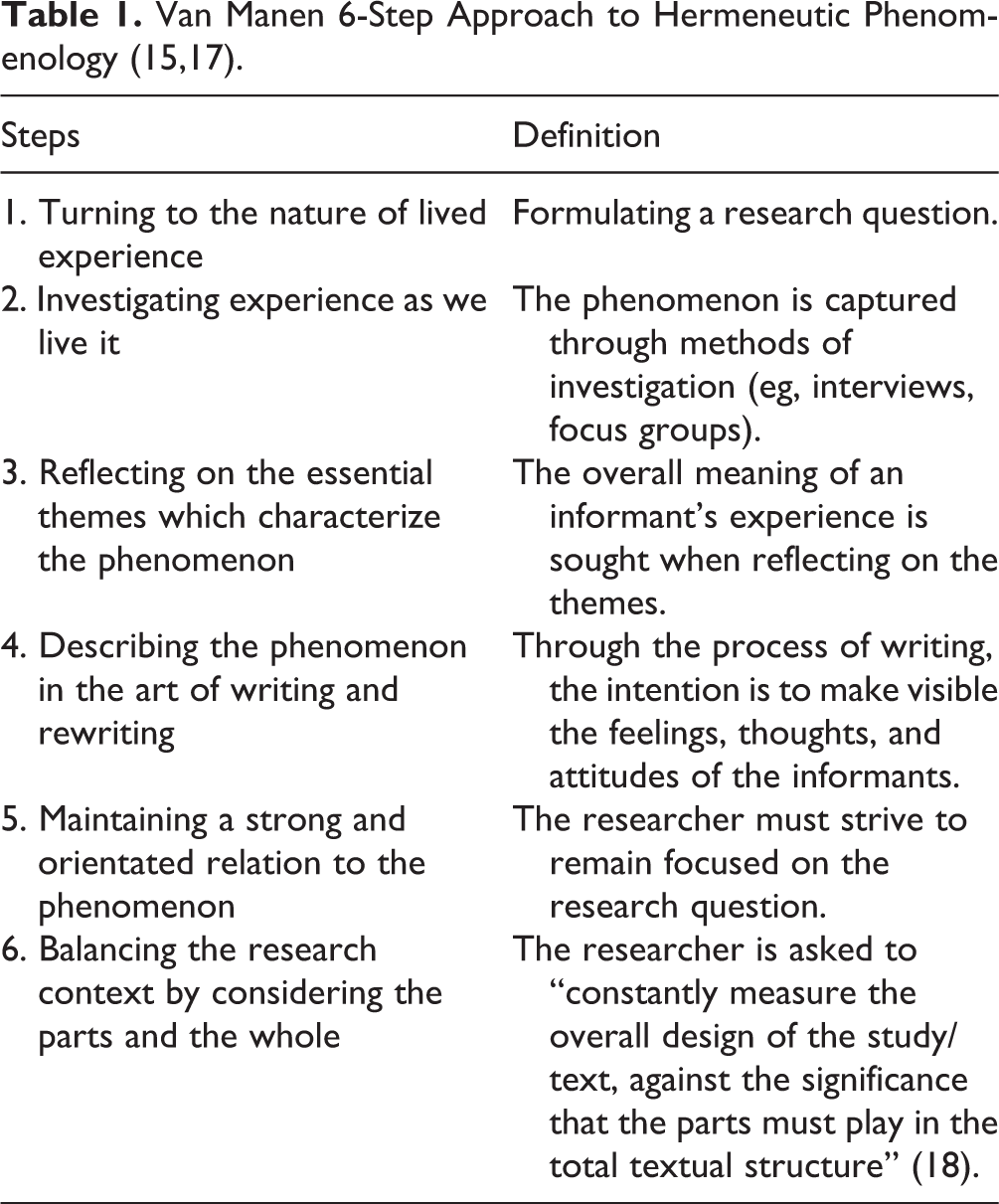
Once transcribed, patient responses were analyzed using van Manen 6-step process for hermeneutic phenomenology (Table 1). Under the guidance of authors S.L. and L.C., authors S.M. and A.D. initiated the process by independently reading the transcripts and highlighting specific sections which spoke to the human lived experience of contributing to curriculum development. Both authors tried to suspend their professional biases as much as possible when reading to allow meaning to present itself within the context of lived experience. These quotations were labeled with a code, which, upon multiple rereadings, were coalesced into concepts. S.M. and A.D. crafted definitions of these concepts, reread texts, and journaled their thoughts as to how they added to the description of the meaning of lived experience. To help reflect on the meaning, both authors imagined how the concepts differed when components were removed, in order to identify the essential elements (17). With concepts created, S.M. and A.D. compared notes to ensure they had captured as much richness from the text as possible. A unified list of concepts and definitions was created, and the authors J.T., V.J., and S.N. were engaged to collapse concepts into like-concepts and then into 5 themes. This process was cyclical, with authors often contrasting concepts to the structure of the research project and vice versa.
Findings
The following 5 themes emerged: (1) contextualizing contributions, (2) addressing expectations, (3) changing health-care service delivery, (4) sharing common experiences, and (5) coordinating participation. Illustrative quotes found in Table 2 supplement the following descriptions.
Patient Themes and Supporting Quotes.

Contextualizing Contributions
Patients highlighted the importance of ensuring the final curriculum product delivered sufficient context to students to preserve the intended meaning of their contributions. Some expressed concern that without this contextualization, students may apply their own personal experiences and misinterpret the main message. One patient explained that the final VRT script included only a part of her story, and the exclusion of the rest of the story meant to her that the context got “lost in translation.” The patients found meaning in having their voice authentically represented and wanted to ensure that their message was not lost on students.
Addressing Expectations
Critiques shared by patients regarding the curriculum development process stemmed from unmet expectations of the scope of their role in shaping the outcome of the project. One common message was that patients would have liked more control over how their contributions were incorporated in the curriculum. In this case, researchers involved in script development applied their lens to lift salient stories and arranged them to highlight key messages. Patients felt that when the authors reached out to them for feedback with drafts of the curriculum during the member-checking stage, they were only being asked to verify spelling and grammar; this felt restrictive and unfulfilling. When patient expectations were unmet, it led them to reconsider the value of their participation.
Changing Health-Care Service Delivery
The patients were hopeful that their participation in curriculum development could contribute to changing students’ values and thereby lead to improved patient care in the future. They were hopeful that this early exposure to a new set of attitudes would inform the students’ approach to service delivery and would establish the foundation of their professional development. While optimistic, the patients also recognized that cultural change at the individual and systems levels is a long process. Despite knowing that the results of their efforts would not be evident in the short term, patients still felt their contributions to this goal were meaningful.
Sharing Common Experiences
All patients identified the importance of feeling connected with others who shared similar lived experiences. The patients expressed a feeling of connection when they read other contributors’ words in the final VRT script. They identified that the shared opinions and emotions represented in the VRT script were a source of validation and support. Differences in how each patient described their experiences in the health-care system also created an opportunity to gain new perspectives. Patients found this experience enriching because it offered a sense of belonging and deepened their understanding of their own experiences.
Coordinating Participation
The patients appreciated the sensitivity with which the educators approached the coordination of partnership. While both patients and researchers had unpredictable schedules, the patients found the researchers’ willingness to work around their schedules to be critical in having their voices heard during the creation process. The researchers’ efforts to reschedule meetings and provide timely follow-up created a sense of purposeful contribution to curriculum development for patients and provided validation of the importance of their contribution.
Discussion
As health education programs consider approaches to partnering with patients to develop curricula, it is important to understand the impact this process has on patients so that a meaningful experience can be facilitated throughout. To avoid the tokenistic use of patients, their unique expertise needs to be supported and better incorporated into curricular goals (19,20). To this end, this study explores how patients experienced their involvement in a health professions curriculum development process. While patients enjoyed contributing to curricular development overall, their experiences were complex and special attention must be paid to how patients drew meaning through the process.
Meaning of Participation
An essential element to the patients’ positive experience in curriculum development came from their perceived influence in shaping the practice of future health-care providers. Patients understood that students are at a critical stage in their professional development and felt that the messages delivered in the curriculum would have a long-term impact on students’ future careers. They saw potential to alter future practice by becoming the students “guide” to professional education and service delivery. All patients hoped that their contribution to the curriculum would ultimately lead to better experiences for future health-care users. Patients who have contributed to health professions education in other contexts, but with similar proximity to affecting student learning, have also expressed a similar view (21 –23). In contexts where there is more distance between patients and students, such as consulting on precreated content, patients seem to experience less meaning in their contributions (24). While patients in this study felt their contributions were meaningful, they did not expect systemic health care changes to be immediate. They understood the limitations of education within a larger system, yet these constraints did not detract from the meaning they drew from the experience.
Patients emphasized the importance of retaining authenticity and their original intent. The less they saw of themselves and their stories in the script, the less meaning they attributed to the contribution. Even the removal of small words, a decision made by the educators to create a script that could be used within the time constraints of the learning activity, altered importance nuances in their original intent. The patients’ emphasis on reaching students at an early stage may have also contributed to their concerns regarding contextualization of their contributions. They realized that there are few opportunities to impact students and their future careers, placing greater importance on ensuring that the final product reflected their original intent as much as possible. To facilitate authentic representation and limit potential misinterpretations of patient contributions, the context of contributions should be considered when developing curriculum. Where possible, patients could provide feedback on the creative construction of the curriculum, allowing for enhanced partnership.
Patients also found the process of sharing their stories with each other to be meaningful. Although others have described that patients appreciated and felt empowered by sharing their knowledge and having their stories heard, they did not elaborate on the reason (25,26). This study suggests that empowerment is grounded in the use of the patient words. Being able to identify their specific contribution in the final product facilitated their sense of meaning in the process. Sharing stories also added to their feeling of validation when their thoughts were echoed by others, although the themes of navigating vulnerability and personal learning were not as prominent in this study as in others (27). Patients in this study were not directly speaking to students, so the context did not lend itself to self-exploration in the same way; however, it could also be argued that the patients recruited for this study had already experienced self-exploration in previous educational opportunities (28). While future studies could clarify this discrepancy, these findings were still cause for reflection as the educators were concerned with patient anonymity during curriculum development. This study suggests that sharing personal stories with other patients can positively contribute to meaningful participation and may not pose as much of a risk to confidentiality as previously thought. Future educators may consider, where appropriate, a model of participation with more openness between patients to foster a sense of shared experience.
Managing Expectations
Patients highlighted the impact that their expectations had on their experience. When expectations were not met, patients responded with a reduced sense of meaning in their contribution. For example, patients seemed disappointed that students might not interpret their contributions as originally intended. In contrast, educators value the deeper reflection and constructed learning that comes from a diversity of interpretations. Addressing each group’s expectations of the project outcomes before beginning the process could mitigate incongruent expectations. In this case, patients felt limited to checking grammar and accuracy in the member-checking phase, yet educators were seeking feedback on both structure and content.
While negotiating the partnership in curriculum development, clarity regarding the project and what each partner contributes is essential. Curriculum developers and patients should have a shared understanding of each other’s roles as well as the goals of the project to minimize the risk of confusion and unmet expectations (25,29). Strategies to identify expectations and work toward these shared goals might include task descriptions, structured decision-making frameworks, and improved orientation to the curriculum.
Limitations
As this study focused on the patient experience during of a particular curriculum development, it has inherently limited transferability. Data collection was also limited to verbal focus group interviews with a small group of patients. Patients contributing to this learning activity may not have been representative of those contributing to the broader network of curricular opportunities.
Future research should investigate the experiences of patients in a variety of contributory roles across different educational mediums in order to draw stronger conclusions. Investigating the long-term impact on patients or students from involvement in a patient-directed curriculum would also add to understanding the complexity of the patient experience.
Conclusion
Elevating the patient voice in curricula is crucial to improving health professions education. Curriculum developers should pay close attention to effective and meaningful collaboration to avoid tokenistic participation. Curriculum developers should determine what makes participation meaningful to patients and ensure their methodology reflects these values. Negotiation of the partnership, where each patient in the process has a clear appreciation of the project and expectations, is essential. Contributing factors and how they are managed will be guided by the nature of the curriculum to be developed. Open and clear communication about project direction and patient expectations prior to commitment is an important determinant of meaningful partnership. This study suggests that sharing personal experiences to shape the values of future clinicians contributed to positive and personal engagement for patients. By reflecting on the findings of this study, curriculum developers can consider how patients participating in curriculum development feel a deeper sense of value in contribution to health professions curricula.
Footnotes
Appendix A
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.