Abstract
Background:
Patients who had received surgical services at Bellin Hospital reported anxiety with the surgical flow. This study tested the hypothesis that the introduction of a surgical navigator, someone who guided the patient and their accompanying others throughout the surgical process, would improve patient satisfaction.
Methods:
Ambulatory surgical patients were randomized to control and study groups. The study group patients were assigned a surgical navigator. Prior to discharge from the hospital, patients were asked to complete a patient satisfaction survey.
Results:
The study group had significantly higher mean scores (P value ≤ 0.026), top box scores (P value ≤ 0.021), and positive comments.
Conclusion:
The addition of a surgical navigator to the perioperative process significantly enhanced patient satisfaction in ambulatory surgical patients.
Keywords
Introduction
Patient satisfaction is an important metric to assess overall quality of the services delivered (1). The Hospital Consumer Assessment of Healthcare Providers and Systems was introduced in 2006 by the US government in an effort to standardize the survey instrument and data collection methodology for measuring the patient experience (CMS.gov) (2). Patient satisfaction data have become increasingly more important as health-care institutions strive to achieve the triple aim of improved quality, improved cost-effectiveness, and enhanced patient experience (3). The Hospital Consumer Assessment of Healthcare Providers and Systems (HCAHPS) survey is a national, standardized, publicly reported survey of patients’ perspectives of hospital care. Press Ganey and other companies have administered the survey. This information provides health-care systems with tools to help evaluate their patients’ experiences at their respective institutions. Patient satisfaction is becoming more important as health-care dollars, particularly with Medicare, are placed at risk (4). Currently, approximately 2% of the Center for Medicare and Medicaid Services (CMS) reimbursement is dependent on the performance measures closely related to the triple aim. It is expected that by 2022, the fraction of CMS payments attributable to outcome data including results of patient satisfaction surveys will increase to 8% to 10% (5). Institutions that strive to improve patient satisfaction are often left with anecdotal and empirical recommendations. Patient satisfaction has been demonstrated to be positively affected by improved interpersonal interactions (1,6). Our study sought to evaluate the surgical experience from the patient’s viewpoint, as well as the accompanying others, since they are separated for a substantial portion of the process, and interacting and keeping the family informed of their loved one’s progress could provide an improved experience. This study was conducted in order to validate the hypothesis that the addition of a surgical navigator would improve the satisfaction in patients undergoing rather than improve the satisfaction of the patient undergoing outpatient surgery at Bellin Hospital, a community hospital in Green Bay, Wisconsin.
Materials and Methods
The study was conducted at Bellin Memorial Hospital, a not-for-profit hospital, providing inpatient and outpatient acute care, medical, surgical, obstetric, diagnostic, therapeutic, and ancillary services. Currently, the hospital has 171 staffed inpatient beds. In 2015, 10 353 surgeries were performed, of which 6688 were classified as outpatients, including day surgery and 23-hour stay patients. The types of cases performed include a full spectrum of surgical cases, including general, orthopedic, obstetrical, cardiac, neurosurgical, ear nose and throat, and plastic surgery. It is representative of many community hospitals where ambulatory surgery is often performed. After obtaining approval from the institutional review board at Bellin Hospital, patients scheduled for outpatient surgical services between June 29, 2015, and August 6, 2015, were randomly assigned to study and control groups the night prior to surgery. Patients in the study group were assigned a surgical navigator, whereas the control group had no additional navigator intervention. Both groups were surveyed in the short stay area prior to discharge. The survey was presented to the patient and their accompanying others by a navigator other than the one assigned to them. They were given the option of completing the survey using a hospital-supported tablet prior to discharge or at home using instructions given to them. The survey was comprised of 9 standardized questions and a 10th question that solicited spontaneous comments regarding the patient’s perioperative experience (see Supplemental Appendix A). The survey was modeled after Press Ganey questions (while following HCAHPS guidelines), to allow comparison of our data with Press Ganey data. This enabled us to convert the raw scores to percentile rankings. Detailed work instructions were developed that the navigators used when interacting with patients and their accompanying others (see Supplemental Appendix B). Patients were excluded from the analysis if they required hospital admission, could not communicate in English, or arrived without accompanying others. The navigators were a group of premedical students enrolled in a summer internship at Bellin Hospital. They participated in an orientation program that introduced them to the surgical flow process and the concepts of patient confidentiality including the Health Insurance Portability and Accountability Act.
Results
A total of 253 patients were enrolled in the study—119 in the study group and 134 in the control group. The study and control patients were similar with regard to types and length of surgery performed, age, gender, and ethnicity (see Supplemental Appendix C). Although the initial randomization resulted in equal numbers of patients in the control and study groups, application of the exclusion criteria resulted in unequal group sizes. The navigators were responsible for 2 to 5 patients at one time and averaged 5 interventions per patient. Each survey question was assigned a score of 1, indicating minimum satisfaction, to 5, indicating maximum satisfaction. Raw percentage scores were calculated by assigning 0.00 for a response of 1, 0.25 for a response of 2, 0.50 for a response of 3, 0.75 for a response of 4, and 1.00 for a response of 5 (this is the same method utilized by Press Ganey).
Figure 1 illustrates the mean scores for each question in the control and study groups, using the Press Ganey methodology. Statistical analysis using a 2-sample 1-tailed t test revealed a P value of ≤0.026 between the control and study groups. The t test in the study group showed a 44.9% reduction in the standard deviation (0.0278-0.0154) when compared to the control group.

Raw mean satisfaction scores.
In order to gain some understanding of the significance of the level of mean score differences observed in this study, we sought to compare our mean data to Press Ganey ranking data. To most closely match our mean score with the Press Ganey rankings, we validated the similarity of the questions. Of the 9 questions on our survey, 3 were replicated and 5 were closely approximated in the Press Ganey survey. One question could not be closely approximated and was not compared (see Supplemental Appendix D). Translation of our mean score data when compared to the Press Ganey Ambulatory Means and Ranks report for July 2015 is depicted in Figure 2. This indicates that the mean score differences observed resulted in significant improvement in percentile rankings. Statistical analysis using a 2-sample 1-tailed t test revealed a P value of ≤0.018 between the control group and the study group. The t test in the study group showed a 68.5% reduction in the standard deviation (25.0-7.86) when compared to the control group.

Satisfaction Scores Translated to Press Ganey Percentile Rankings.
Figure 3 illustrates the top box raw scores between the control and study groups. Statistical analysis using a 2-sample 1-tailed t test revealed a P value of ≤0.021 between the control group and the study group. The t test in the study group showed a 48.2% reduction in the standard deviation (0.0911-0.0471) when compared to the control group.
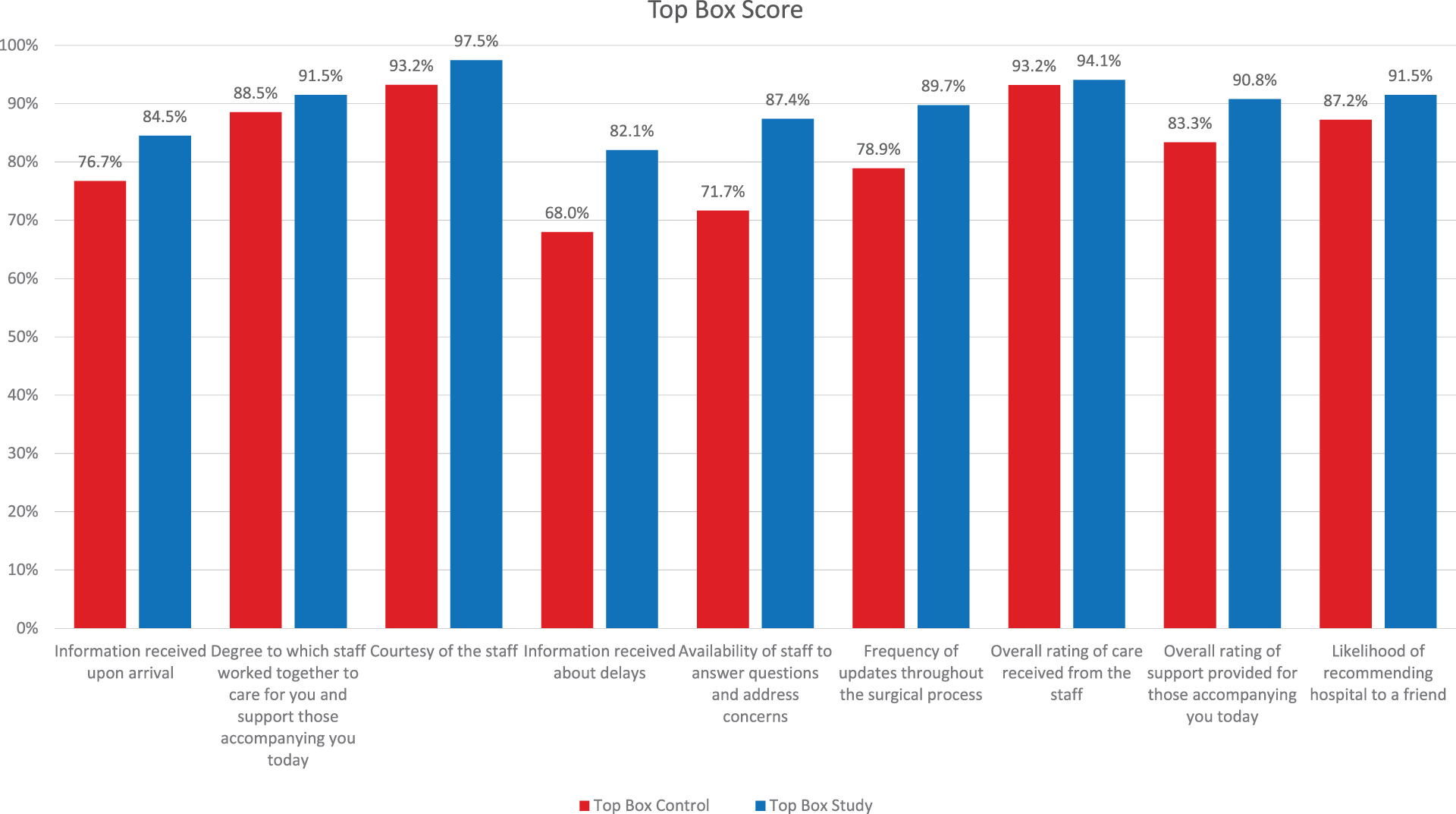
Top Box Raw Satisfaction Scores.
Figure 4 illustrates our top box data translated to percentile rankings when compared to the Press Ganey Ambulatory Means and Ranks report of July 2015. Statistical analysis using a 2-sample 1-tailed t test revealed a P value of ≤0.006 between the control group and the study group. The t test in the study group showed an 82.7% reduction in the standard deviation (23.7-4.10) when compared to the control group.

Top Box Scores Translated to Press Ganey Percentile Rankings.
Spontaneous responses allow customers to provide feedback that adds a qualitative dimension to patient satisfaction. Figure 5 demonstrates a 51.5% improvement in positive responses in the study group.

Spontaneous Positive Response Comparison.
Variation in the results measured by standard deviation is an important determinant of sustainability of a study. We used the results from the 2-sample 1-tailed t test. Table 1 depicts the standard deviation of the mean and top box scores, as well as the Press Ganey mean and top box percentile rankings.
Comparison of Standard Deviation between the Control and Study Groups.
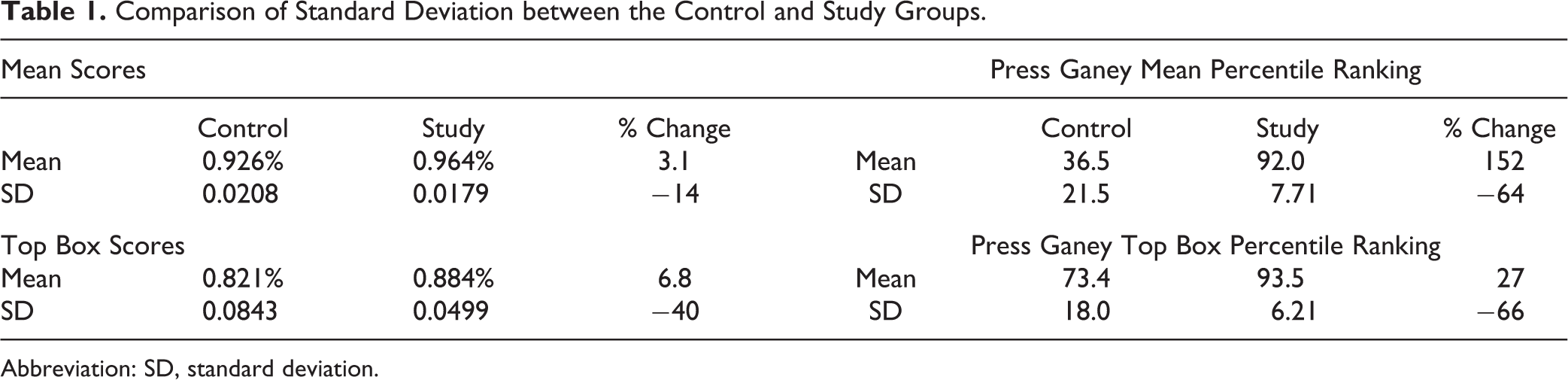
Abbreviation: SD, standard deviation.
Discussion
The introduction of a surgical navigator, who frequently connected with the patients and families, resulted in significant patient satisfaction improvement in outpatient perioperative services at Bellin Hospital. This study is consistent with the observation that in patient satisfaction surveys, small differences in mean scores can produce large differences in percentile rankings. Press Ganey permitted us to compare 8 of the 9 questions in our survey to those found in Press Ganey’s survey. We were also granted permission to use their ranks and means data from the same time period as our study in order to convert our mean and top box scores to Press Ganey comparable percentile rankings. The survey results showed improvement in scores with respect to each of the questions individually. Additionally, the top box score of the likelihood to recommend and the positive comments improved in the study group. The questions that demonstrated the greatest improvement in patient satisfaction were the “information received about delays,” “frequency of updates throughout the surgical process,” and “availability of staff to answer questions and address concerns.” The question with the smallest improvement was “overall rating of care received from the staff.” This is an interesting validation of this study since one would not expect to see a significant improvement in the overall quality of care rendered by the introduction of a surgical navigator. On the other hand, the questions that showed the greatest degree of improvement all had to do with communication received from the care team, which was the principal task of the surgical navigators. It is noteworthy that perception of the quality of care rendered was improved based on enhanced communication without any specific intervention that directly affected the quality of care. It is also of interest that the overall patient satisfaction improved, even though the surgical navigator interventions targeted the patient’s support system at least as much as the patient. This at least suggests that the patient support system is a legitimate target for efforts for improving patient satisfaction. In addition, the 51.5% improvement in the positive responses in the study group is significant. These comments provide insight into the patient’s hospital experience and can be very useful, as they may be more indicative of true patient satisfaction (7).
Although this study clearly demonstrates that the introduction of a surgical navigator resulted in statistically significant improvement in patient satisfaction, several additional questions remain to be answered. It would be of interest to determine whether our results can be replicated in other settings. For example, a number of variables must be considered when evaluating reproducibility. The general study design is straightforward, but the types of “interventions,” frequency of “interventions,” and the number of patients “navigated” need to be consistent. Future studies could be conducted to optimize these variables as they relate to patient satisfaction and manpower considerations.
Sustainability is another aspect that must be considered prior to initiating a surgical navigator program. Will replication of our materials and methods result in a similar outcome if repeated at our hospital or at any hospital? The determinants of sustainability are dependent upon variation, repeatability, and reproducibility (8). For example, conditions of repeatability in our study included an identical measurement tool in the same environment, by surgical navigators following standard operating procedures and using detailed work instructions (see Supplemental Appendix B) (9). Changed conditions might include different surgical navigators or different hospital systems. With a common measurement tool, interventions, and inclusion and exclusion criteria, reproducibility with minimal variation can be attained. Our study demonstrated decreased standard deviation in the study group when compared to the control group in the Press Ganey mean scores, the Press Ganey percentile rankings, and the mean top box scores (see Table 1). Processes with decreased variation, which support repeatability and reproducibility, are indicators of a sustainable process.
Conclusion
Our findings support the hypothesis that the introduction of a “surgical navigator” into the perioperative outpatient process in a community hospital improves patient satisfaction. This is supported by the statistically significant differences in mean scores, top box scores, and the increased percentage of positive responses in the study group versus the control group. Our data suggest the sustainability of our study, as evidenced by the reduced variation in the study group standard deviation in comparison with the control group mean scores, top box scores, and percentile rankings. To further increase reproducibility in future studies and reduce inconsistencies between navigators, the use of standard operating procedures and detailed work instructions is important. Ideally, each navigator should be interchangeable when following standard procedures and instructions.
To the extent that reimbursement for hospital services is dependent on patient satisfaction, implementation of cost-effective programs that influence patient satisfaction will become sought after. The economic feasibility of introducing a program like ours into everyday practice needs further investigation. Introduction of a surgical navigator program may indeed be an effective means of improving patient satisfaction, but its implementation and sustainability are dependent on its cost-effectiveness.
Footnotes
Acknowledgments
The authors would like to thank Bellin Health for their passionate support to this project.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research and/or authorship this article.
References
Supplementary Material
Please find the following supplemental material available below.
For Open Access articles published under a Creative Commons License, all supplemental material carries the same license as the article it is associated with.
For non-Open Access articles published, all supplemental material carries a non-exclusive license, and permission requests for re-use of supplemental material or any part of supplemental material shall be sent directly to the copyright owner as specified in the copyright notice associated with the article.
