Abstract
US medical schools increasingly seek ways to reduce costs and improve productivity. One aspect of this effort has been the development of performance-based incentives for individual faculty. A myriad of such plans exist. Typically, they incentivize clinical revenue generation but vary widely in how teaching, investigation, and administrative contributions are recognized. In Pathology at Yale, we have developed a transparent metrically driven approach that recognizes all missions and allows faculty significant control over their career path. Although some metrics derive from traditional measures such as workload relative value units and one’s level of grant support, the key concept underpinning our approach is to define one’s contributions not in terms of the revenue generated, but rather on the effort devoted to each of our missions, benchmarked against national or local standards. Full-time faculty are paid a competitive rank-based salary and are expected to contribute at least 100% effort in support of the school’s missions: clinical, research, education, administration, and professional service. Metrics define the effort assigned to each activity. Faculty achieving greater than 100% effort receive bonus compensation in proportion to their excess effort. By codifying explicitly how such effort is recognized into a single metric (% effort), we achieve a process that better aligns the professional and personal goals of faculty with the aims of the school. To facilitate its implementation, we have developed a web-based software platform called SWAY (Standardized Workload Analysis at Yale) that enables faculty to monitor their progress and record their activities in real time.
Keywords
Introduction
Pathology is one of 29 departments that collectively comprise the Yale University School of Medicine. Each department is responsible for tailoring a compensation and incentive plan that meets the unique needs of their own specialty. This decentralized approach at Yale has been particularly important to pathology, given the significant differences between pathology practice and other patient-facing clinical specialties. Pathologists seldom control their own clinical volume; their potential for revenue generation varies widely depending upon their chosen subspecialty; and the use of physician work relative value units (wRVUs) correlates poorly with actual effort in pathology. 1 -3 Pathology is also a specialty with above average expectations for teaching, laboratory supervision, and administration, much of it uncompensated, and a discipline that typically counts among its faculty a significant cohort of PhD’s with no clinical responsibilities.
In response to these realities, a myriad of creative and sophisticated approaches linking compensation in pathology departments to measures of productivity have emerged. Indeed, a search of Google for the terms “pathology compensation” yields 18,000 hits. Commonly, the plans that have evolved incorporate safeguards to ensure fairness and some level of transparency, a measure of clinical productivity, recognition of seniority, and various ways that “points” are granted for contributions to nonclinical activities. A few examples (of many) would be those implemented at Johns Hopkins, 4 the University of California at Davis, 5 or Virginia Commonwealth University. 6 Prior to 2014, the compensation plan in pathology at Yale used a “points” based plan similar to those cited above, in which senior leadership annually evaluated faculty performance using wRVU-based metrics, grant success, teaching contributions, market benchmarks, and seniority. However, there were several problems with this approach.
Our practice at Yale is highly subspecialized. This has evolved to assure high quality expertise in all areas required by our quaternary medical center. Yet, when coupled with our robust outreach program in anatomic pathology, large discrepancies emerge in the volume and complexity of cases referred to our subspecialized services. Outreach captures many gastroenterology, gynecological, and cytology specimens, but not so many renal or neurological or pediatric cases. This is most apparent in the significant wRVU discrepancies across our clinical faculty (Figure 1).
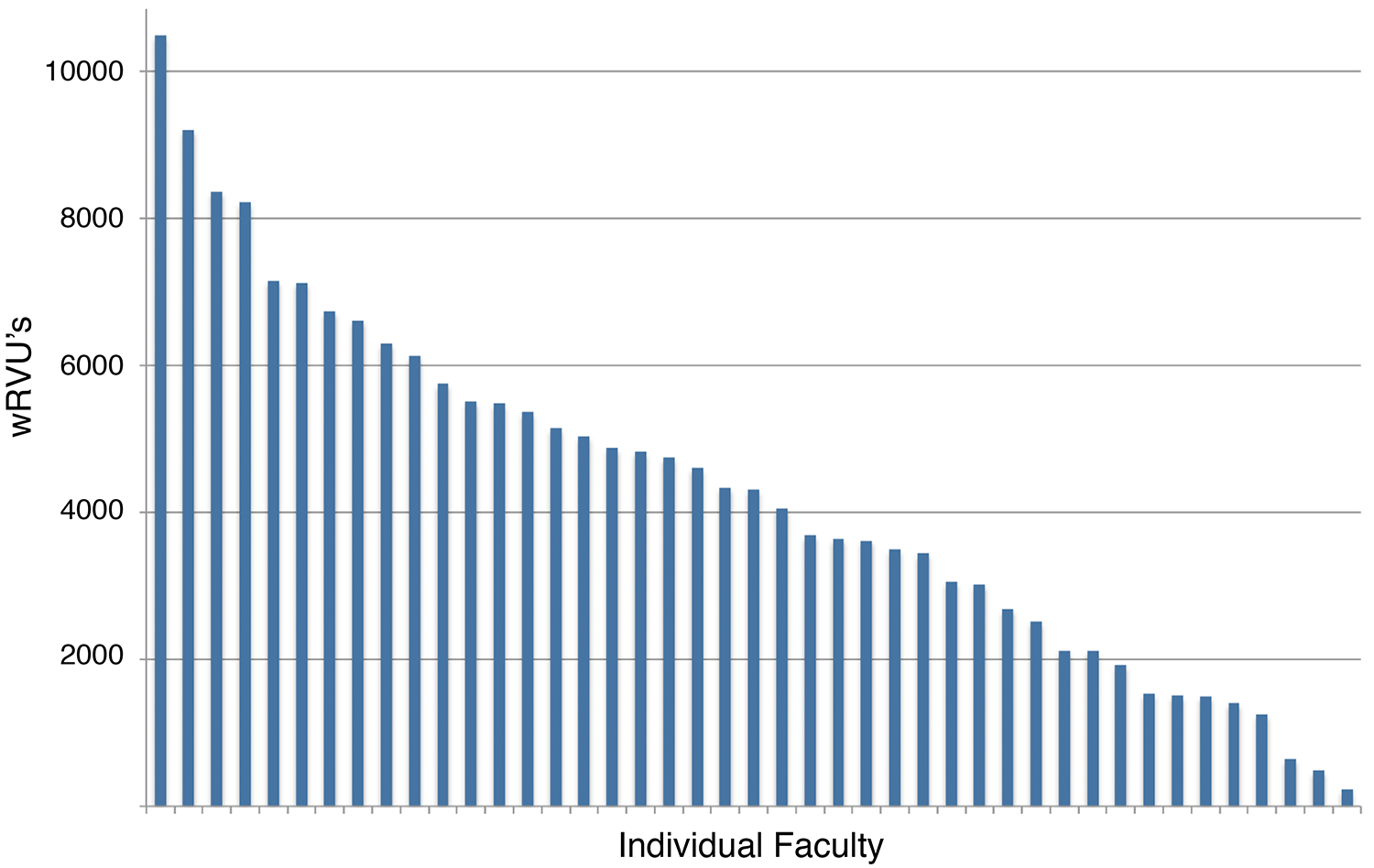
Typical distribution of wRVUs across individual clinical faculty in Yale’s subspecialty pathology practice. Each bar represents a different faculty member (2004 data). wRVUs indicates work relative value units.
A second concern as noted above 1 -3 was that wRVUs did not accurately reflect the effort involved in each subspecialty. This was particularly concerning at Yale, with most faculty practicing in just 1 or 2 subspecialty areas. Other problems motivating a change in policy included expectations from the school’s central administration that departmental compensation plans should minimize subjective evaluation and include metrics that would recognize the contributions of nonclinical PhD faculty. There was also concern across the institution that women and underrepresented minorities (URM’s) have observationally taken on more of the “housekeeping” type of administrative duties such as seminar organization, student or house staff mentoring, search committee service, and so on and that such activities were not being appropriately recognized in existing compensation plans. An approach was thus needed that reduced the subjective aspects of faculty evaluation while improving goal congruence between what was recognized and rewarded in our compensation plan versus the avowed mission of the institution.
The Yale Plan: A Focus on Faculty Effort Across Missions
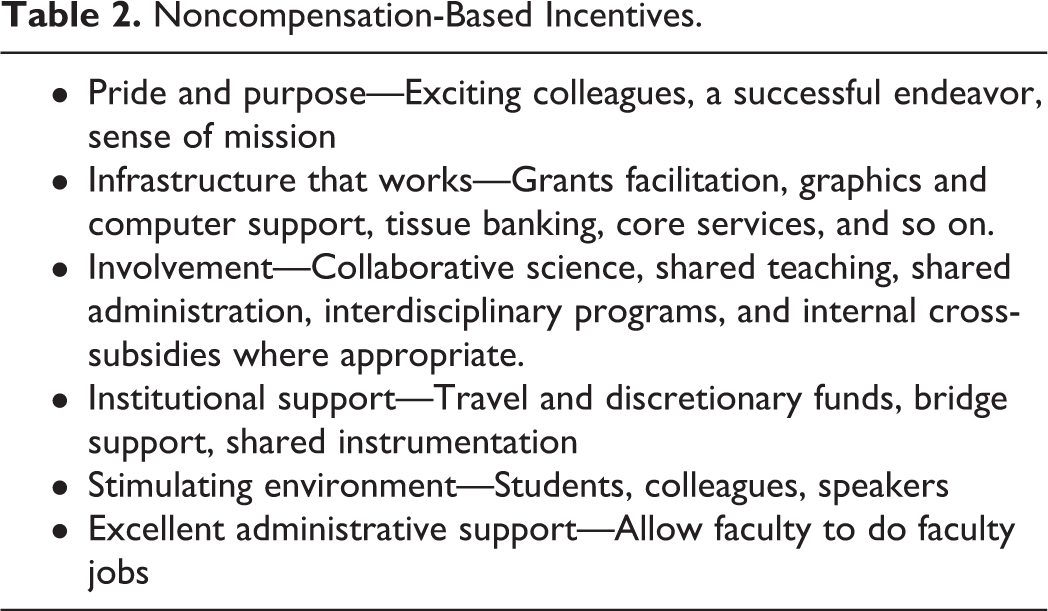
A group of senior faculty, representing different aspects of our mission, was charged with considering alternative ways to monitor faculty effort and incentivize their progress. At the onset, the group considered what it was that faculty actually wanted from the institution (Table 1), and then secondarily what incentives could be offered and how a compensation policy could play a positive role. Although their task was to derive a method for linking compensation to productivity, it was clear that not all incentives are compensation based. In fact, most are not and depend on departmental policies and hidden support systems (Table 2). A few key parameters desired in a new plan were also articulated (Table 3).
What Do Faculty Want?

Noncompensation-Based Incentives.

Key Goals of Compensation Plan.
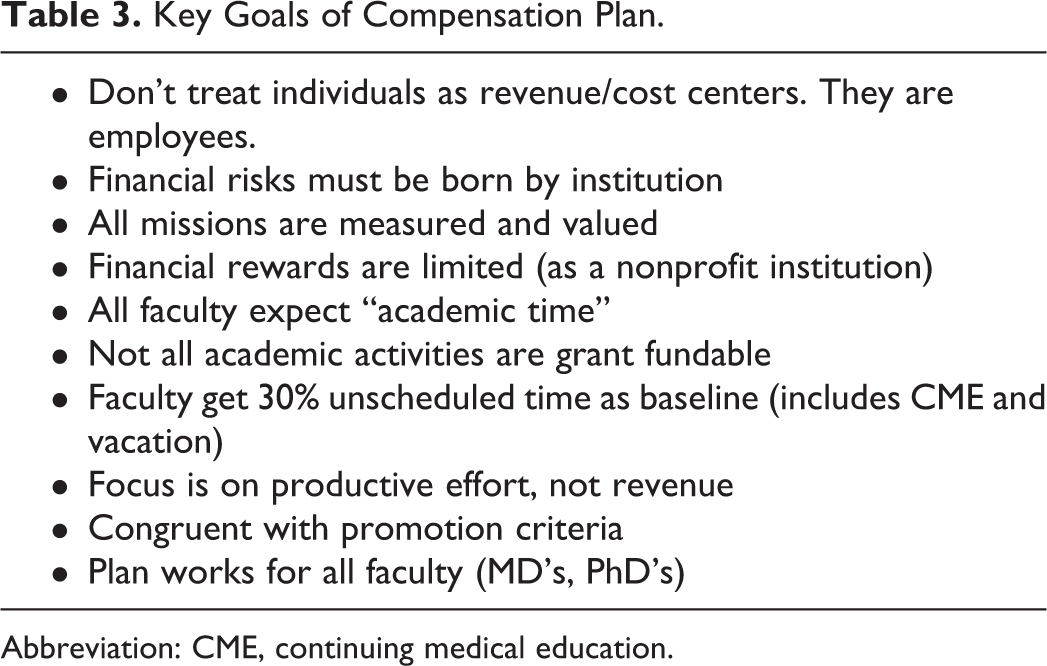
Abbreviation: CME, continuing medical education.
Percentage Effort—A Unifying Metric
A key feature of the plan that emerged is that every contribution to the mission would be expressed as a unit of “percent effort.” In this parlance, it became relatively straightforward to acknowledge that a full-time faculty member receiving a competitive full-time salary should commit 100% of their effort in the service of the school’s various missions. How effort is distributed across the different missions (clinical work, teaching, research, administration, etc) obviously varies between individuals, but in aggregate, faculty are expected to each reach 100% effort (or a lower threshold if they are employed part-time). Effort beyond 100% (or their part-time status) should provide additional bonus compensation.
It follows that conversion factors are needed to express such things as wRVUs in terms of % effort. It is also a reality that the department must remain fiscally solvent, so revenue-generating missions such as clinical practice and grants cannot be excessively sacrificed to nonrevenue generating activities. As outlined below, this is handled by tying effort metrics to national benchmarks for clinical productivity, by limiting the effort awarded in some categories and by thresholds that limit how much one can reduce their clinical activity by contributing to other missions. A related consideration is how to recognize efficiency and quality. Some tasks take longer than others; some faculty work more quickly than others. In the end, it was decided to base effort allocations on work actually accomplished (eg, papers published) and not linked to how long it might have taken someone to do it. Where possible, quality metrics (eg, impact factor) were included in the conversion. The productivity policy that emerged categorized effort into 7 categories (Table 4). All ladder faculty are treated equally, there is no distinction between “research” and “clinical” faculty. All full-time faculty are expected to devote full-time effort to university activities, that is, generate at least a total of 100% effort. Effort is allocated based on what one does in support of the school’s mission. The calculations that support each category are detailed below.
Categories of Effort.

Abbreviations: CME, continuing medical education; wRVU, work relative value unit.
Vacation and continuing medical education effort (paid time off)
Four weeks is allocated for faculty vacation. The university does not have a prescribed faculty vacation policy, but 4 weeks for vacation and/or time for continuing medical education are typical. Four weeks are 8.3% annual effort; this is automatically allocated to each full-time faculty member. For part-time faculty, this allocation is reduced proportionately. If faculty choose to take less time for vacation, or even none at all, they still receive 8.3% effort credit. Faculty on triennial or sabbatical leave, or on medical or maternity leaves, receive paid time off (PTO) credit in proportion to the length of their leave.
Clinical effort
There are no great solutions for comparing pathologist effort between different subspecialties. It is well recognized that wRVUs are imperfect, and for pathologists this system is probably inferior to metrics based on the Royal College of Pathologists or even simple slide counts. 3 However, many (most?) medical institutions in the United States, including Yale, have settled on wRVUs as the relevant standard for comparing physician productivity. The challenge was thus to assign % effort to wRVUs in a way that more fairly recognized the discrepancies in the average time and difficulty needed to generate a wRVU between subspecialties. This problem is typically addressed by asking a group of subspecialty pathologists to agree on whose work is the most challenging. After some very energetic discussions, seldom can a consensus be reached.
Our solution was guided by 3 considerations. The first was that we did not want to penalize an efficient practitioner. Someone who completed the same number of cases in the same subspecialty in less time should receive the same % effort credit. Secondly, we recognized some subspecialties such as renal pathology or ophthalmic pathology just did not have enough volume to fill one’s day, although the presence of the subspecialist on service every day is required to maintain subspecialty expertise availability as part of our clinical mission at a quaternary medical center. And finally, we observed that in some clinical subspecialties while wRVUs generated are low, diagnostic complexity was consistently high, requiring a disproportionate effort for every wRVU generated. Examples would include subspecialties such as in neuropathology or hematopathology. In contrast, other subspecialties, such as gastroenterology pathology or cytology, often allow for accumulation of high wRVUs, generated from patient cases that comprise a mixture of low and high diagnostic complexity. Based on these considerations, we constructed a model that converted wRVUs into units of % effort. The model was designed to set the median wRVU productivity for a full-time practitioner in academic pathology practice at 70% effort, which roughly correlated with our expectations of scheduled “on-service” time for our full-time academic pathologists. Our institution used the AAMC wRVU metrics that were provided to our medical group from their consulting agreement with Vizent Inc; for 2018, that benchmark at 70% effort was 4500 wRVUs. The model was also nonlinear, awarding lower wRVU subspecialty services extra % effort/wRVU in recognition of their need to be continuously available on service, regardless of available wRVUs. At the high end, the model flattens the effort awarded per wRVU, on the assumption, as noted above, that at very high wRVUs, the average effort required to generate a wRVU was less due to a larger proportion of low complexity diagnostic cases in those practices. The desired correlation was modeled as shown in Figure 2 as generated by the equation shown therein.
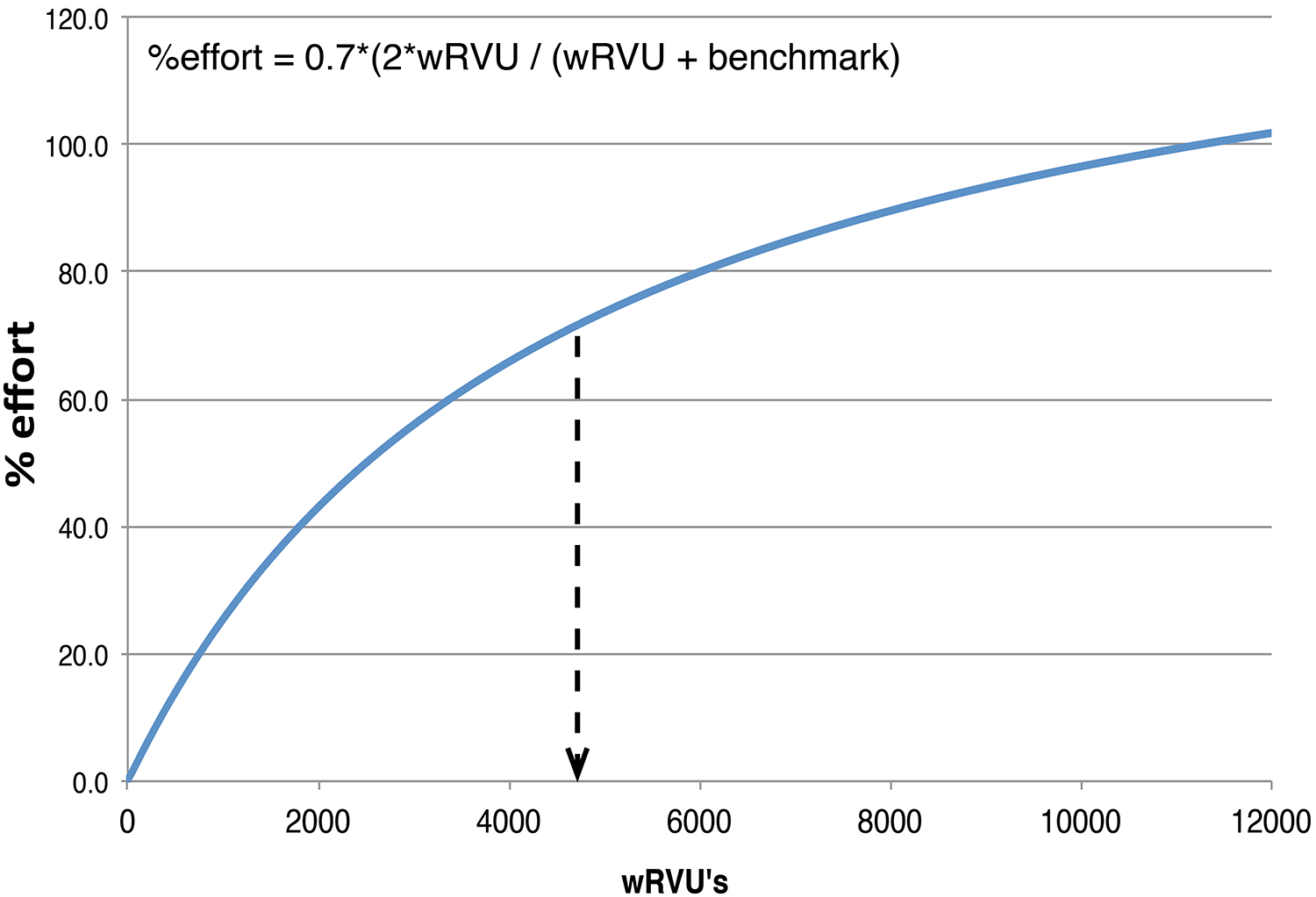
Conversion of wRVUs to % effort
Medicare Part A services such as autopsy and most laboratory services do not utilize wRVUs. Autopsy effort was thus measured on a per/case basis. The underlying assumption was that for our entire autopsy practice (about 300 cases/year), this would require 1 dedicated full-time equivalent (FTE) pathologist at 100% effort. So the % effort credit awarded for each case was scaled similar to the method utilized for wRVUs, with the benchmark that the entire service was equivalent to 1 FTE (Equation 1, where “autopsies” is the number completed by a faculty member):
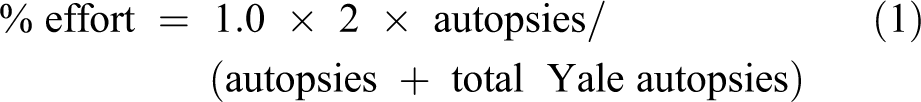
In this calculation, partial autopsies counted as full autopsies. For cases where the brain was evaluated by the neuropathology unit, credit for 1 CPT code 88309 (complex procedure) was awarded to the neuropathologist and counted in their surgical wRVU calculations. For other laboratory “Medicare Part A” services, a determination was made whether the laboratory service required the full-time presence of the pathologist, and the %effort was awarded accordingly. For example, our tumor DNA profiling laboratory required the full-time activity of the pathologist to interpret and report the results (including their presentation at the precision medicine conference), and a week of service in this laboratory was awarded a full week of % effort. Some other laboratory services such as routine molecular diagnostics required less than a full-time presence of the pathologist to oversee the laboratory and its reports and correspondingly received less effort credit for each week of service.
Research effort (and other extradepartmentally funded salary support)
This category also included extradepartmentally funded salary support from the hospital that was assigned to a specific individual. Examples of such support would be support for the Director of Anatomic Pathology (AP) or the residency program director. The % effort awarded reflects the actual % of salary (and fringe benefit costs) recovered, regardless of the stated effort on any specific award. By this approach, separate accounting for “over the NIH cap” salary or other restrictions (if any) on sponsored research awards is unnecessary; all extradepartmental funding sources are treated in a consistent way.
Teaching and conference effort
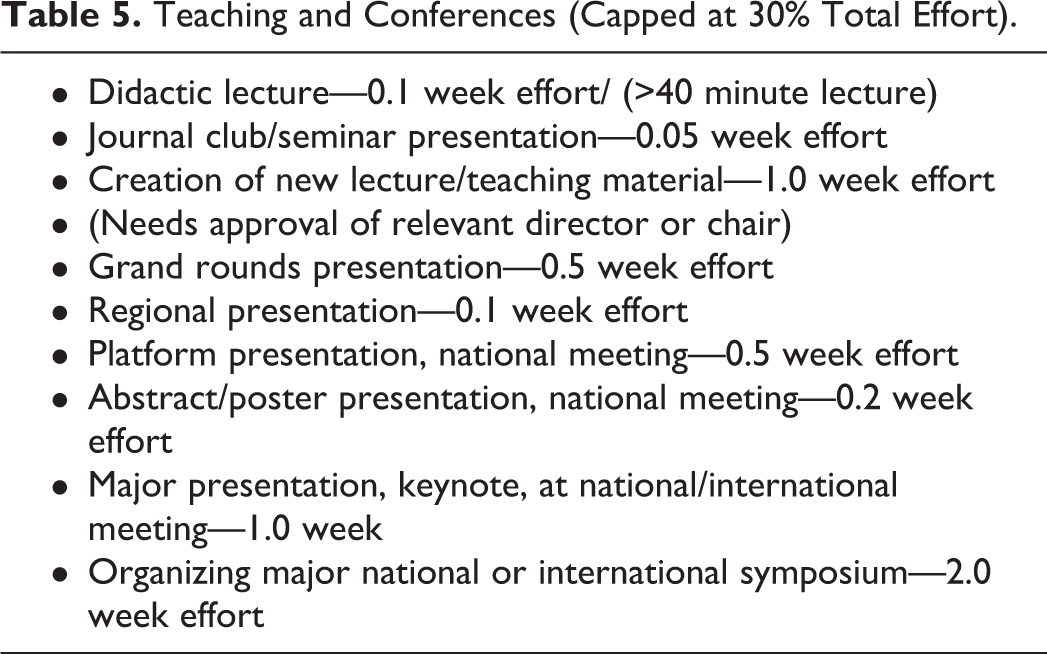
This category typically is not remunerative but is a core part of our mission. As such, it was important to recognize such effort, but in a bow to fiscal reality we limit the total credit awarded in this category to 30%. Although it seems antithetical to our mission to cap recognition for teaching and conference effort, in practice the 30% cap we arrived at did not result in limiting any of our faculty (the maximum credit in this category achieved by a faculty member in 2018 was 28.9%). If direct salary support is received for this activity from sources outside the department, then that effort would be awarded under “Research effort” as described above. This category recognizes not just local effort but also importantly national contributions that support faculty advancement and the stature of our institution. Weekly clinical tumor boards are considered to be part of clinical effort recognized by wRVUs and are not included in this category. The levels of credit awarded for activities in this category are summarized in Table 5. It can be argued that some administrative tasks take longer than the effort allocated, but in defense, the allocated effort represents full-time effort devoted to that task. At Yale School of Medicine, a faculty workweek is considered to be 50 hours, as was officially set by the Yale Medicine Board of Directors in 2016. So, for example, the assignment of 5 hours (0.1 week) to giving a didactic lecture, or 50 hours (1 week) to preparing a new lecture, or 100 hours (2 weeks) to organizing a national symposium seem reasonable if not generous. Note, as described below, all of these metrics have been incorporated into our Standardized Workload Accounting at Yale (SWAY) software, which greatly simplifies the accounting process.
Teaching and Conferences (Capped at 30% Total Effort).
Administrative effort
Many senior administrative duties receive support at least in part from the hospital or school (eg, residency director, chair, laboratory director, AP director, etc). As with teaching, such support is recognized as “research effort” since it is extramurally funded. However, beyond these positions, many administrative tasks both within and outside the department receive no extradepartmental funding, but are important, advance faculty careers, and deserve to be recognized. This is particularly true of national service, such as on NIH study sections or leadership in our national professional societies. Effort is awarded for these tasks as summarized in Table 6. Note that each 1% effort represents a full-time commitment of 24 hours to the task (assuming a total of 2400 annual work hours). So, for example, service on a CAP committee is awarded the equivalent of 1 week of full-time effort. Although of course there will be situations where the effort required exceeds that allocated, but there will also be instances where the allocations are generous. The key point is that such effort is recognized and at least in some measure rewarded. As with teaching, the total of nonremunerated administrative work that can be credited to each faculty is capped at 30%.
Administrative Effort (Capped at 30%).

Academic effort (publications)
The publication of scholarly work is at the core of the academic mission. Awarding a baseline of 3 weeks effort/paper published in the current academic year recognizes this. This baseline effort is then scaled based on the overall impact of the publication relative to the departmental average impact factor and by the contributions of the faculty member to the paper. First or last (senior) authors get full credit. Major contributors receive half credit, and other authors get 1/3 credit. This is summarized in Equation 2. Books and book chapters are assigned the mean impact factor of the department for purposes of this calculation. By this approach, exceptional high-impact papers generate substantial effort credit. As with other nonremunerative activities, we have capped this category at 30% effort. It can certainly be argued that publishing a paper requires substantially more than 3 weeks effort. This is a fair concern, but again, for high impact papers an effort credit of 6 to 9 weeks (12%-17%) for the senior and/or first author is not unlikely. This is equivalent to 300 to 400 hours of full-time effort (based on a 2400 hours work-year). It can also be argued that a substantial portion of the reward from publishing is recognized on a personal, career-investment level.
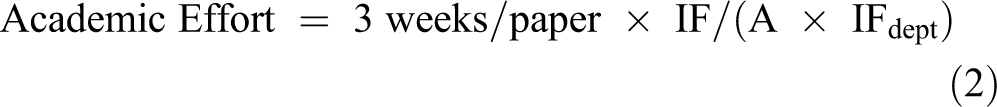
Where IF = impact factor of journal; IFdept = impact factor average of all publications by the department for that year; A = author contribution; First or last (senior) author = 1; Major author = 2; Other author = 3.
Departmental citizenship
This category recognizes exceptional activities that promote departmental well-being. Good citizenship and contributions to a respectful and mentoring environment are expected of all faculty, so additional contributions in this category are awarded effort only for exceptional performance or special circumstances. This is the only category without objective metrics, and it allows senior leadership latitude in recognizing contributions not otherwise captured. It is capped at 20% effort. Examples include exceptional activities that enhance communication within or outside the department; activities that provide role models of integrity; activities that promote patient safety, new research initiatives, interdisciplinary collaboration, or new models of education. Two specific examples would be the recognition and receipt of an award from the hospital to one of our faculty for exceptional contributions to a patient safety issue; another would be the independent initiative of one of our faculty to personally visit several local practitioners in their offices to address concerns over a biopsy interpretation. Credit is also awarded in this category to encourage early career faculty (in first 5 years) and to assist them in building their clinical, teaching, and academic program.
Strategies for contributing 100% (or greater)
The system is designed to allow individual faculty to choose as much as possible the activities that best advance their academic success and promotion. Faculty are provided a market competitive guaranteed salary that is stable. Most financial risk is assumed by the department, with some guardrails in place to assure overall fiscal stability (eg, expectations for time on clinical service, robust outreach development, caps on the effort awarded for nonremunerative activities). It falls to each faculty to chart their own balance of activities that will allow them to achieve the required effort (100% for full-time faculty, proportionately less for part-time commitments). The strategies for enhancing one’s productivity are clear (Table 7).
Strategies for Improving Productivity.

Abbreviation: wRVU, work relative value unit.
A bonus for effort that exceeds 100%
A fundamental tenet of our plan is to assure that all productive faculty receive a stable market-competitive salary. Since Yale’s triennial leave and sabbatical policies support salary but not bonus compensation, a secondary advantage of a stable salary is the opportunity for mid-level and senior faculty to use triennial and sabbatical leaves to advance their careers, gain new skills, and explore new research or academic endeavors, all without financial hardship. The 100% effort goal of our plan is tied to average or median benchmarks for full-time academic faculty, as described above. Those with greater than 100% effort receive an annual bonus in proportion to their “excess” effort. The size of this bonus is based on 3 metrics. The first is the amount of funds the department has available for bonus compensation. The second is one’s share of the total excess effort accumulated across all faculty. The third metric relates to one’s fixed salary. There is a significant spread across the salary paid, for example, between junior PhD’s versus senior MD’s. So the impact of a given bonus, derived from their excess effort, could be quite meaningful to a junior faculty but much less incentivizing to a senior colleague. However, at the same time, it seemed unfair to simply scale by their relative salaries, since that would only serve to widen the compensation spread between faculty well beyond the average market differences. Our compromise was to reduce the size of the bonus relative to one’s fixed annual salary, up to a salary of USD$200,000. Thereafter, the bonus awarded per unit of excess effort was the same for all faculty. So, bonus was calculated in 2 steps. First, for those with annual salaries below USD$200 000, their effort exceeding 100% was reduced in proportion to their salary relative to $200 000. Then, bonus was distributed in proportion to each faculty member’s scaled excess effort relative to the total effort across all faculty. The calculations are shown in Formulas (3) and (4):
Bonus Calculation
Step 1: Calculate excess effort (EEi) for each faculty member (i):
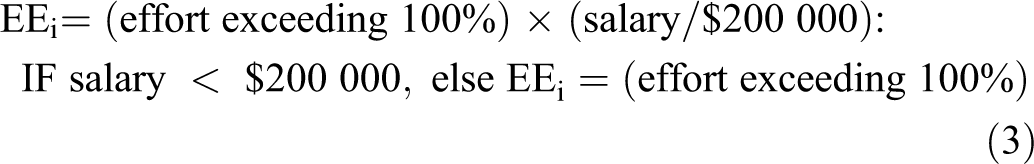
Step 2: Sum EEi across all n faculty, distribute bonus pool (BP$) in proportion to EEi
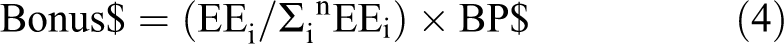
Results of the Yale Plan: A Full Accounting of Effort Across All Missions
Implementation of effort-based metrics was begun in 2014 and refined in subsequent years. To aid the transition from the earlier points-based plan to the new plan, a 2-year transition window was provided. During this time, one’s compensation and bonus were calculated by both the earlier method, and also by the new effort-based method, and the one most favorable to the faculty member was used. After 2016, only the new effort-based metrics applied. Along the way, faculty input refined the plan. The areas most of concern were the levels of effort offered for published papers, the use of impact factors as a scale factor for clinical faculty, and the level of credit awarded for various administrative tasks. A common complaint was that administrative tasks deserved more credit, but when the actual time spent in such tasks was accurately measured, in most instances the effort awarded was fair, if not overly generous. In the earliest implementations of our plan, the total of administrative effort awarded across the faculty exceeded 25% of the total faculty effort across all activities. This seemed to most faculty as unrealistic and an excessive burden on the department. In fact, as we gained experience with the system, many administrative tasks that were initially credited based on historic perceptions of the work involved were in fact deemed to be excessively credited; these allocations were then scaled back with faculty input. A related concern was the distinction between the 3 levels of administrative activity, especially when the activity was not specifically listed in the table of examples. In such cases, most faculty were reasonable if not conservative in their assignments; in only a few cases did the chair or another senior faculty need to adjudicate. Some faculty involved in high-wRVU generating subspecialties also expressed concerns about the flattening of the effort/wRVU curve (Figure 2), but accepted it when they realized that the high wRVUs of their subspecialty guaranteed that they would be well into bonus territory almost regardless of their other contributions. Another interesting result of the plan was that for the first time, a number of PhD faculty involved primarily in research and teaching received significant year-end bonuses, funds that did not come from their grants. We also gave faculty the option of taking their bonus as personal compensation or alternatively they could leave it in a departmental discretionary account and use it for purposes related to their research or academic professional expenses. Many availed themselves of this latter option. After a few years, the use of SWAY became routine and was well accepted and endorsed by most if not the entire faculty. The effort distribution of our 62 ladder faculty is shown in Figure 3A for the year 2018. All but 4 faculty reached the expected level of effort (100% for full-time faculty, proportionately less for part-time faculty, or those who were appointed for less than the full academic year). More than 2/3’s of the faculty received bonus compensation. What is most interesting is the way that different faculty contributed to our mission. Every faculty member had a unique story and built their contribution in an individual manner. In aggregate, the department’s portfolio of effort consisted of 5.5% publications, 24% extramural (grants), 8.3% teaching, 40.6% clinical care, and 10.6% administration. Vacation and PTO accounted for 14.3%. Exceptional contributions (citizenship) or support of new faculty efforts accounted for 2.3% (department).
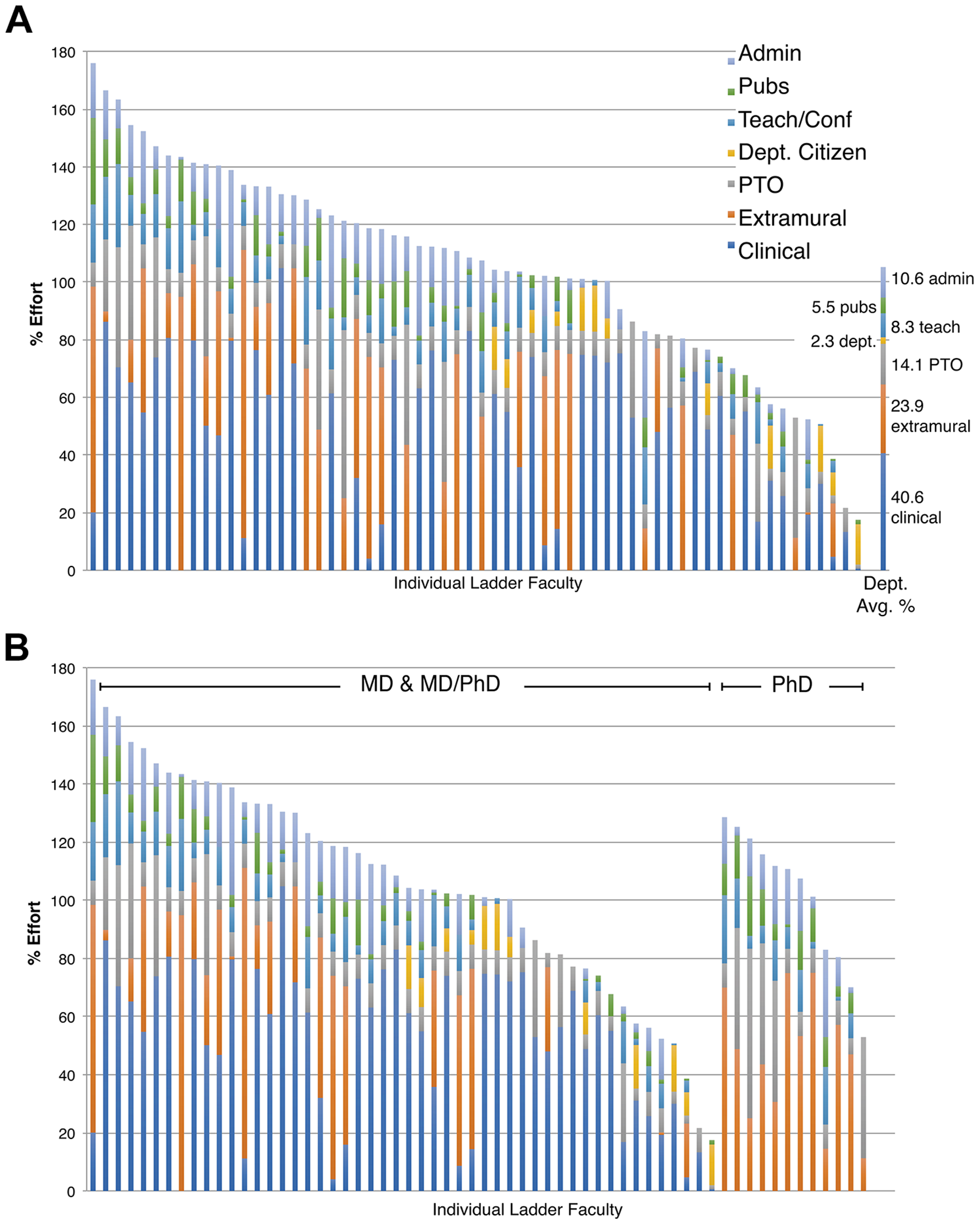
A, Distribution of individual effort at Yale pathology, 2018. B, Effort segregated by clinical (MD and MD/PhD) versus nonclinical (PhD) faculty.
It is also interesting to compare how those with clinical responsibilities (MD and MD/PHD) fared relative to those with no clinical role (PhD’s; Figure 3B).
Overall, those with significant clinical activity tended to achieve higher levels of effort, while those with the higher levels of extramural (grant) funding were generally research-oriented faculty. But this was not universally true, with some of the clinical faculty securing significant extramural support. Teaching and conference loads were similar; research faculty took greater advantage of their available sabbatical leave opportunities. Publication credit was somewhat skewed in favor of the research faculty, but only slightly. In the end, the overall percentage of clinical versus research faculty receiving year-end bonus compensation based on achieving over 100% effort was similar. In fact, when considered as a unit (Figure 3A), it is difficult to identify any distinctive differences between faculty unless one focuses solely on clinical effort, and even here there is high variability among our clinical faculty.
Development of SWAY—Standardized Workload Accounting at Yale
A significant barrier to the implementation of our plan was the complexity and difficulty of capturing the various components needed to accurately evaluate effort expended in each category and for each faculty member. Further complicating the issue was capturing the external benchmarks required to calculate some categories. Examples would include accurate wRVU capture, grant accounting, publications and impact factors for every publication updated annually, teaching loads, and so on. Fortunately, many of these data feeds were potentially at hand, although it required the expressive power of a programing language to fully capture, store, evaluate, and visualize this information. We originated at Yale in 1983 the anatomic pathology laboratory information system now commercialized as Cerner CoPath. This system provides full and accurate information on all clinical work of the department. Measuring wRVUs on a per faculty basis was thus not a problem. Similarly, the university has sophisticated grant accounting systems in place that were also electronically accessible. Publications are available via the PubMed Application Programming Interface 7 or My NCBI bibliography portal. Impact factors published each year by Clarivate are downloadable as CSV or MS Excel documents. 8 Beginning with these feeds, our software engineering team developed a web-based system to collect and organize the data needed to implement our plan. This software system, SWAY, allows individual faculty to rapidly and intuitively enter or edit their own data for publications, teaching, conferences, committees, and administrative tasks. It facilitates the entry of their publications by capturing these directly from PubMed using PubMed ID or provides options for manual entry. It tracks and displays whether a publication has been previously credited (no double dipping!). It gathers current impact factors for every publication cited by the faculty and calculates in real time the departmental impact-factor average. Specific entries for PTO, other sources of extradepartmental funding, and so on are automatically uploaded and then edited by our business office. Importantly, SWAY allows faculty to both monitor their progress over each academic year in real time and also enter their contributions as they occur throughout the year. This eliminates surprises at year’s end over their progress (or expectation of a bonus). Due to some carryover of responsibilities from year-to-year, such as in committee/administrative appointments and teaching efforts, SWAY’s historic record also makes it easier for faculty to copy over recurring activities for the year, making minor adjustments only where needed. Screen shots of some of the various modules in SWAY are shown in Figures 4, 5, and 6.
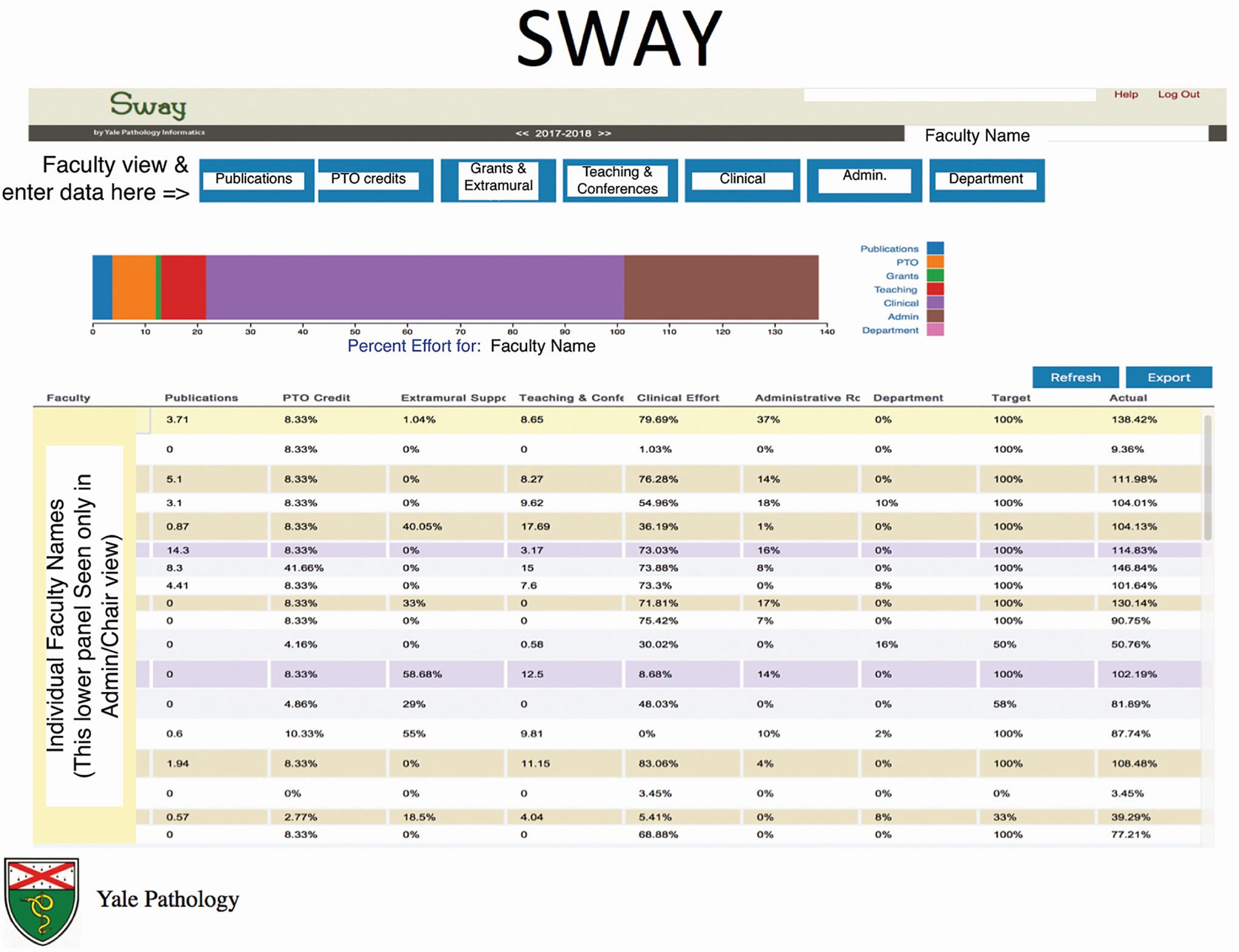
SWAY summary screen. This display is what the chair or senior administrator would see, in that it lists all the faculty and allows selection of individual faculty for review. The screen that is available to each individual faculty member lists only their own metrics. The bar at the top, in which contributions to different aspects of the mission are color-coded, summarizes this. Selecting any specific mission allows the individual to review in more detail their data and also where permitted, enter new activities. SWAY indicates Standardized Workload Accounting at Yale.
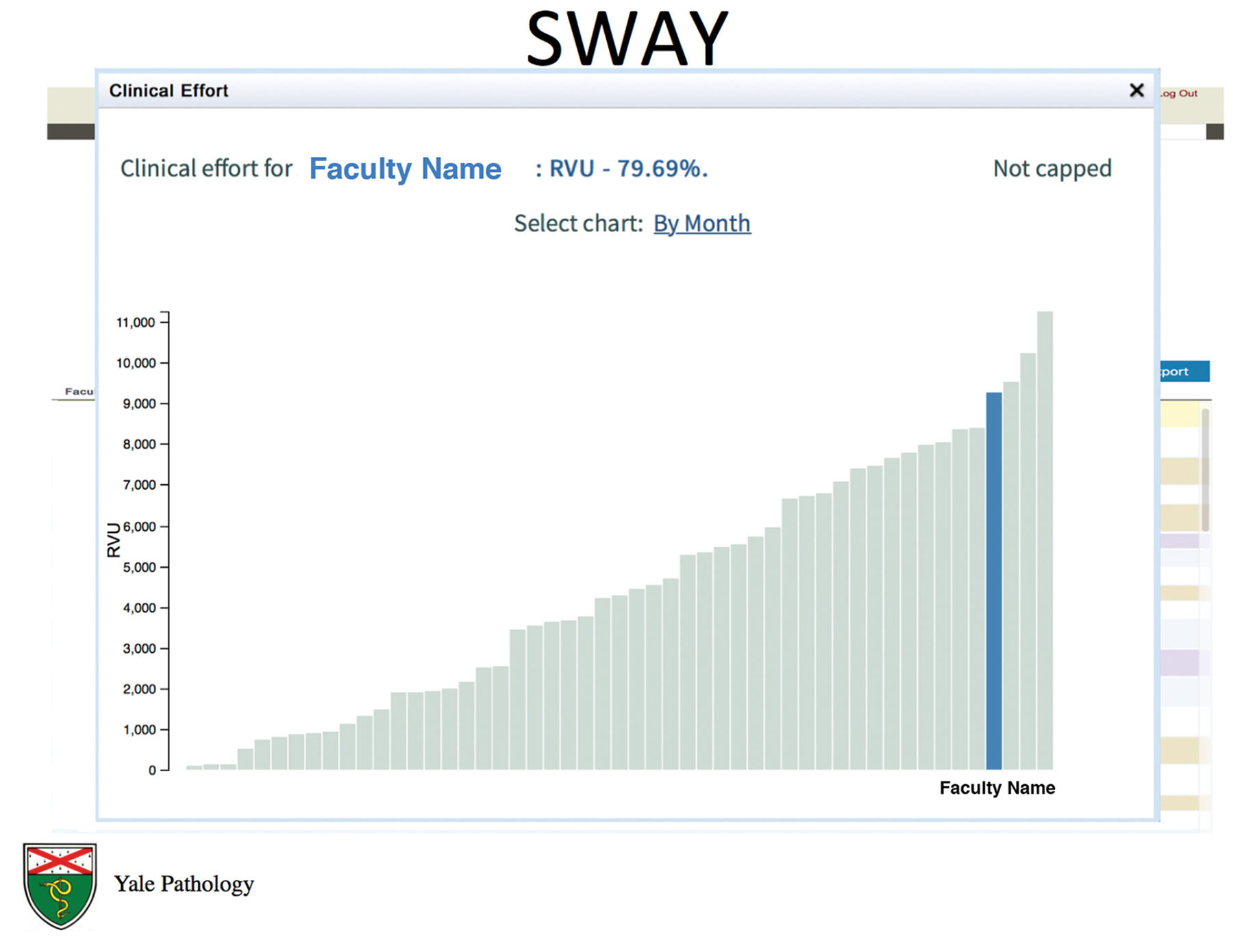
SWAY clinical effort screen. Selection of the clinical tab of the screen shown in Figure 4 opens this view of the individual faculty member’s accumulated wRVUs and its relationship to the wRVUs of other clinical faculty. The %effort awarded is shown at the top. This screen is available at any time and updated in real time throughout the academic year. The clinical activity can also optionally be presented on a per/month basis. SWAY indicates Standardized Workload Accounting at Yale; wRVUs, work relative value units.
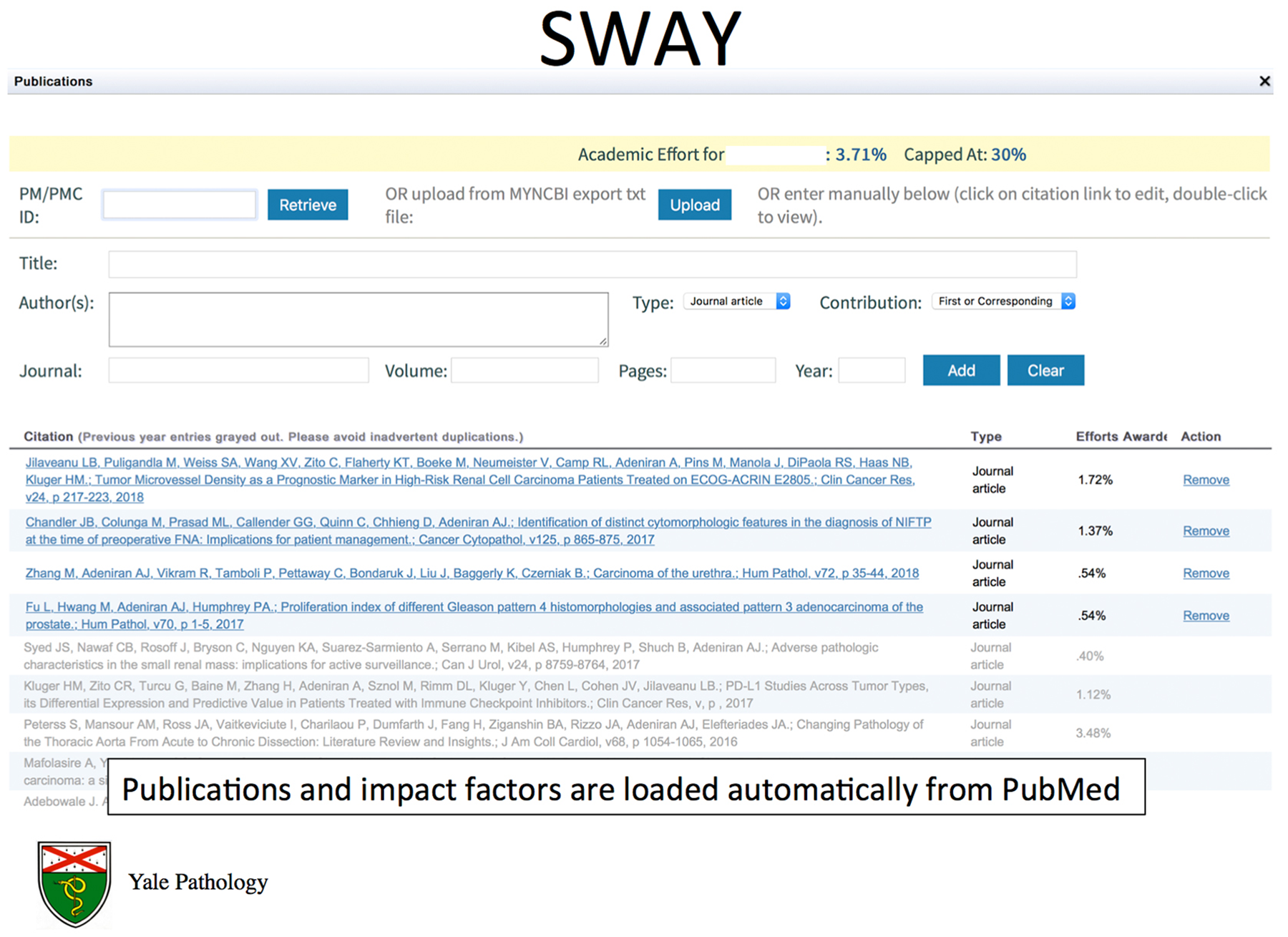
SWAY publication screen. Publications may be entered manually or automatically from PubMed using PMI/PMC IDs. Current publications not previously credited are in blue; past publications for which effort credit has already been received (in prior academic years) are in gray. SWAY indicates Standardized Workload Accounting at Yale.
Discussion
The development and adoption of our % effort-based method for monitoring faculty productivity was driven by the need for an objective and unbiased way to evaluate faculty productivity, one that incorporated and recognized all aspects of our mission. Now in its eighth year of implementation, SWAY has been well received by the faculty. Many faculty, even some outside of our department, appreciate its consideration of the diverse aspects of our mission and especially its recognition for activities beyond the walls of our institution. Over the years, several refinements have also been made in response to faculty input. The superficial complexity of our approach has been mitigated by the development of automation software to facilitate recording, benchmarking, and reporting activities. Although detailed before–after comparison is difficult, it is our sense that with the SWAY software in place, the burden imposed on the leadership, faculty, and administrative staff for documenting their productivity and annual activities is now less onerous than what used to be consumed by ad hoc “year-end” review processes that entailed updating individual resumes and manually documenting teaching, grant, clinical, and other professional activities. The accuracy of the data recorded under SWAY is also superior. Beyond improved efficiency of capturing such data, perhaps the most impactful effect of SWAY has come from holding all faculty to a single transparent standard. This has reduced the barriers between clinical and research oriented faculty and has fostered a sense of unity across faculty along with a broader understanding of how each contributes to the department.
Although our program was developed to specifically address challenges we faced as an academic pathology department, we believe our approach can be tailored to other clinical specialties. For example, some patient-facing clinical specialties may want to more strongly incentivize clinical productivity over other activities, given that their clinicians have more control (vs pathologists) over their individual clinical activity. This can be accomplished within SWAY by simply varying the parameters that award % effort to different activities. Indeed, the desired relationship between academic, administrative, pedagogic, and clinical activity can be infinitely adjusted. By changing the threshold for bonus compensation, the system can also be tailored to provide any fraction of one’s total compensation as bonus versus fixed salary. Three hypothetical examples of alternative formulas relating wRVUs to effort are illustrated in Figure 7. If any of these formulae were to be utilized in SWAY in lieu of the curve shown in Figure 2, the balance and threshold of activities that would generate bonus compensation would be substantially altered. The caveat of course is that one’s personal productivity is composed of highly nuanced activities that are often in conflict and easily biased by an adverse relationship between career goals and compensation. Medical practices should thoughtfully select a wRVU-to-effort correlation that reflects both the goals of the department and is justifiable to the faculty.
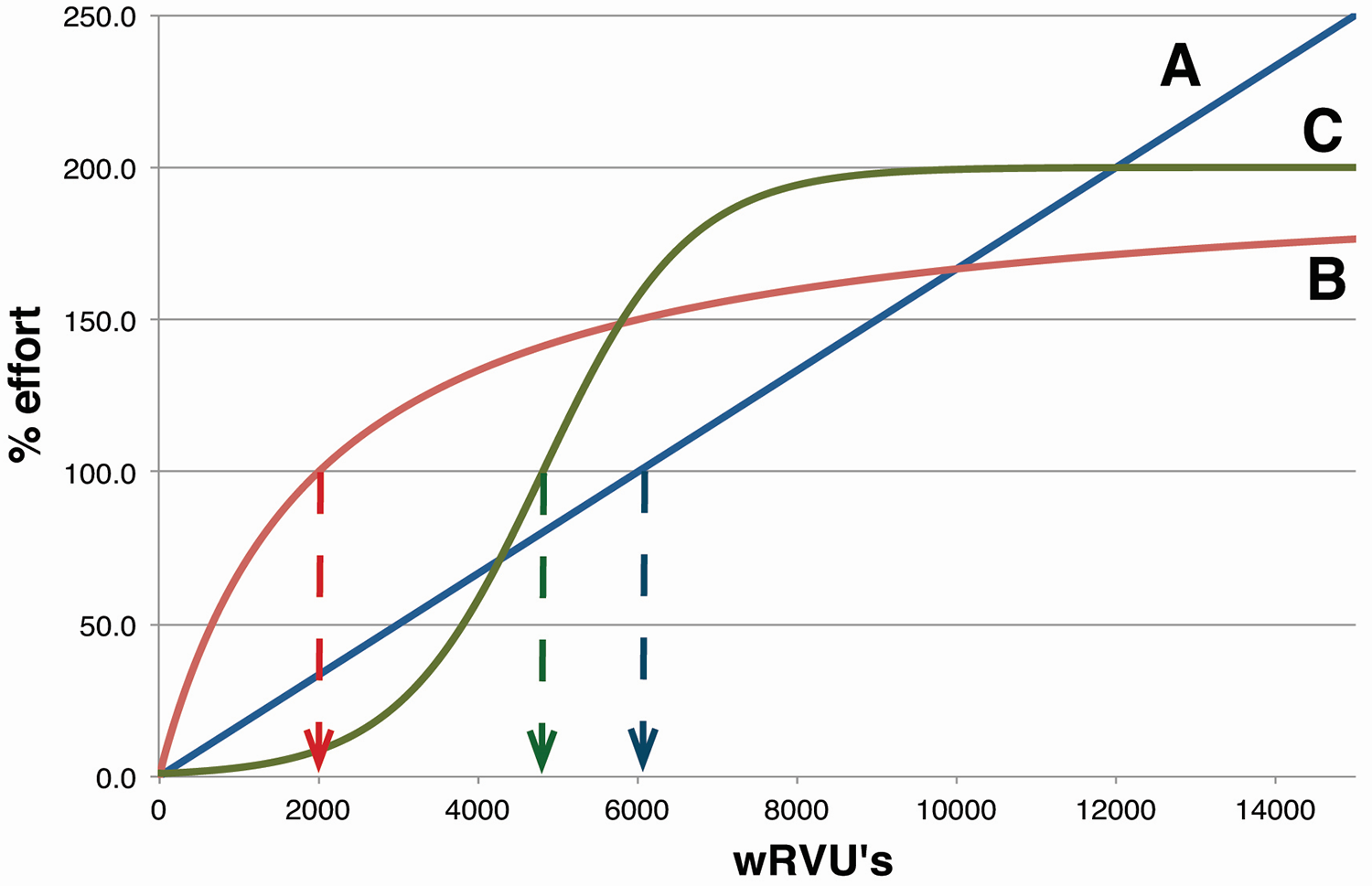
Examples of different % effort versus wRVU curves. A, In a practice where the clinical work is fairly homogeneous and equally available to all practitioners, curve could be a simple linear correlation. B, In another practice, one may set the baseline for 100% effort at a lower wRVU level, perhaps correlating with a low fixed salary relative to market. A greater portion of one’s effort (and compensation) would then derive from the bonus pool. C, Complex correlations are also possible, such as low % effort for minimal wRVU, then a very steep incentive for clinical work up to a threshold, but then capped at the high end to perhaps encourage other academic activities or encourage the sharing of cases with other faculty. The equations generating each curve were: (A) % effort = wRVU/60; (B) % effort = 2 × wRVU/(wRVU + 2000) × 100; (C) % effort = 200/((200 − 1) × EXP(−0.0011 × wRVU) + 1).
In summary, by focusing on % effort, we have implemented a single unifying metric that bridges all contributions to the school’s mission, incentivizes faculty in ways congruent with activities begetting career success, and provides an objective assessment of productivity that is independent of bias. This approach has proven to be fiscally sound and favorably endorsed by the faculty. An unanticipated result, and perhaps its most important impact, is the way it has created a greater sense of shared purpose across the entire spectrum of our faculty, from the most clinically oriented MD’s to the most research intensive PhD’s. The software that implements SWAY is available from the authors on an open-source basis.
Footnotes
Authors’ Note
Jon S. Morrow and Peter Gershkovich are cofirst authors. JSM proposed the concept of an effort-based faculty metric and all authors contributed as a senior executive team to its continued development. PG was responsible for programming the software that implemented SWAY. JSM wrote the manuscript and all authors contributed to its editing and refinement.
Acknowledgments
We thank Dr Jeffrey Golden, MD, PhD, for helpful discussions during a Northeast meeting of the Association of Pathology Chairs on the value of faculty effort as a metric. We also thank the many unnamed faculty at Yale and earlier members of the Department’s Executive Team, particularly Drs David Stern, Gerald Shadel, Zenta Walther, and Jeffrey Sklar, who contributed thoughtful suggestions throughout the development of SWAY.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study was supported in part by the Raymond Yesner Endowment to Yale University (JSM).
