Abstract
The transition to a value-based payment system offers pathologists the opportunity to play an increased role in population health by improving outcomes and safety as well as reducing costs. Although laboratory testing itself accounts for a small portion of health-care spending, laboratory data have significant downstream effects in patient management as well as diagnosis. Pathologists currently are heavily engaged in precision medicine, use of laboratory and pathology test results (including autopsy data) to reduce diagnostic errors, and play leading roles in diagnostic management teams. Additionally, pathologists can use aggregate laboratory data to monitor the health of populations and improve health-care outcomes for both individual patients and populations. For the profession to thrive, pathologists will need to focus on extending their roles outside the laboratory beyond the traditional role in the analytic phase of testing. This should include leadership in ensuring correct ordering and interpretation of laboratory testing and leadership in population health programs. Pathologists in training will need to learn key concepts in informatics and data analytics, health-care economics, public health, implementation science, and health systems science. While these changes may reduce reimbursement for the traditional activities of pathologists, new opportunities arise for value creation and new compensation models. This report reviews these opportunities for pathologist leadership in utilization management, precision medicine, reducing diagnostic errors, and improving health-care outcomes.
Keywords
The Opportunities for Pathology and Pathologists
Expenditures for health care in the United States were approximately $3.65 trillion in 2018, an increase of 4.4% over the prior year, and are projected to rise from 17.9% of gross domestic product in 2017 to 19.4% in 2027 if current trends continue. 1 Health-care spending also rose 4.8% in 2016 and 5.8% in 2017, well above the inflation rate, which currently is 1.6%. Absent substantive changes in the efficiency of delivering American health care, this trend is expected to accelerate due to aging of the baby boom generation and the corresponding increase in utilization of medical services. 1 Clearly, such a trend would be unsustainable, as it would result in an ever-increasing taxpayer burden for government subsidies. 2 Moreover, an increasing gap between demand and capacity without increased resources and efficiency would ultimately result in poorer outcomes and diminished access to needed care.
In vitro laboratory tests have been estimated to account for only 2.3% of total health-care dollars 3 or around $82.7 billion in 2017 (Figure 1). Laboratory testing may increase with the expansion of value-based reimbursement and precision medicine but will likely remain a small part of overall health-care expenses, especially as new and expensive therapies are implemented. However, while laboratory tests are a small portion of health-care expenditures, 94% of objective and structured data in the electronic medical record (EMR) are from the clinical laboratory. 4 Moreover, some reports suggest that 70% of all medical decisions are based on laboratory testing. 5
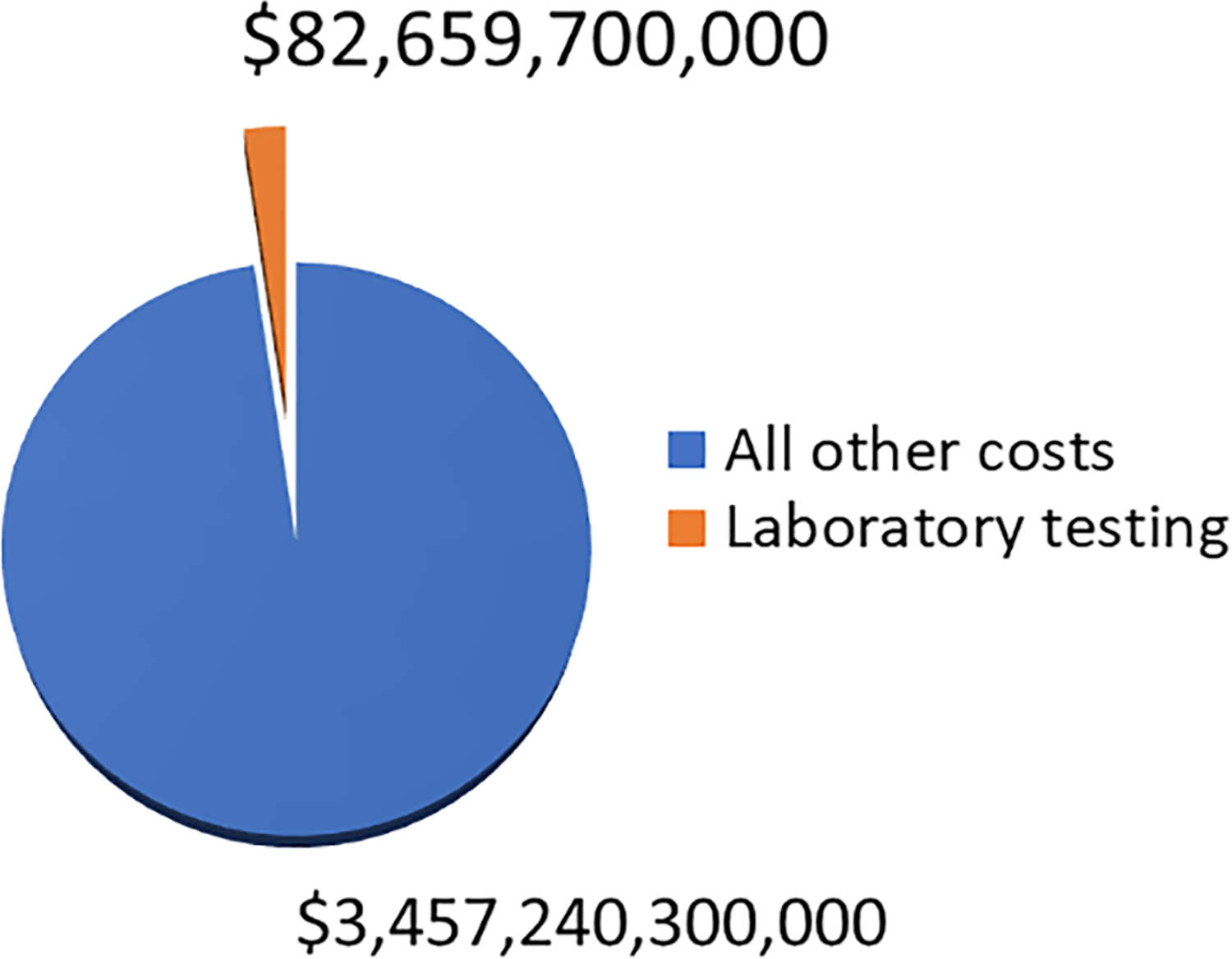
The estimated proportion of laboratory test costs when compared to all other US health-care costs in 2017 (US$).
A recent literature review, with physician specialist interviews and an Internet-based multiple choice survey, estimated that an average of 74% of cardiology and oncology patients in the United States had laboratory tests, which influenced an average of 64% of medical decisions. 3 Laboratory tests were most often used for initial diagnosis, followed by treatment and posttreatment monitoring. A report published in 2017 found that 35% of 72 196 patient encounters studied had laboratory testing. 6 However, this varied substantially: Almost all inpatients (98%) had 1 or more laboratory tests, compared to 56% of emergency clinic patients and 29% of outpatients. 6 A different perspective is that laboratory testing approaches 100% for patients being evaluated and managed for infectious diseases, genetic disorders, neoplastic diseases, myocardial infarction, therapeutic drug monitoring, and other conditions, 7 with the World Health Organization citing 58 essential diagnostic tests for diagnosis and treatment of human disease. 8
Considering base hospital and physician costs for 2017 (approximately $1.85 trillion) and using 64% as the rate of influence on treatment decisions, laboratory tests influence approximately $1.18 trillion of health-care spending (Figure 2). These “downstream effects” of laboratory tests on clinical management include choices of medical procedures and therapy as well as the ordering of additional diagnostic tests, especially in domains other than the laboratory.
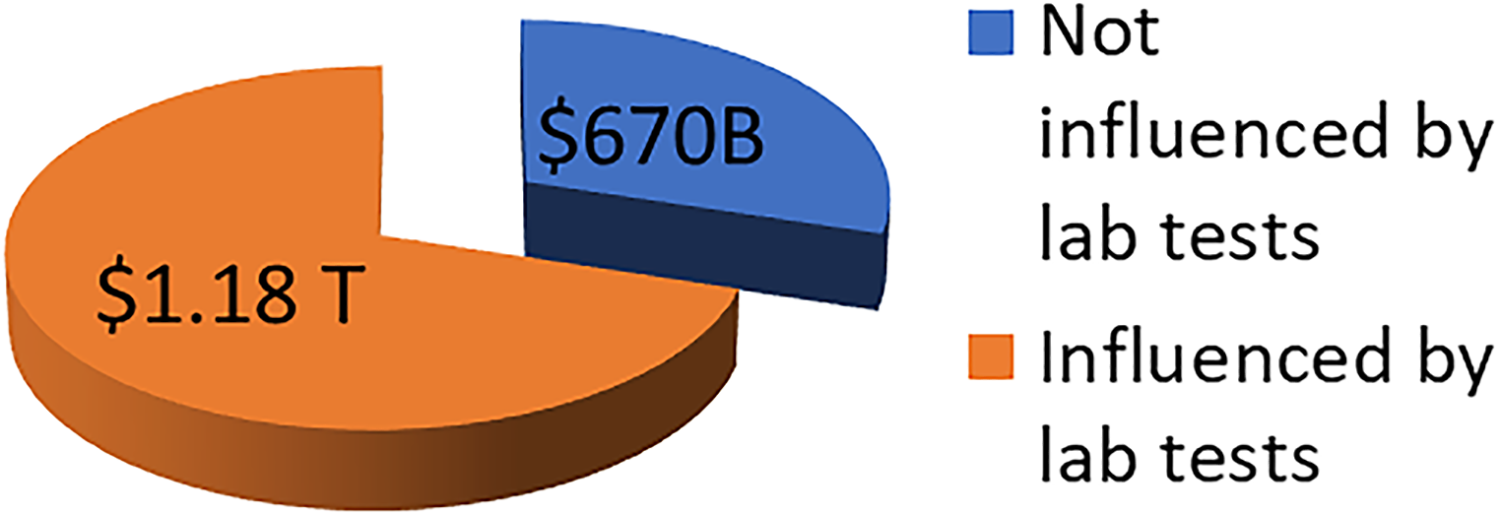
The estimated proportion of 2017 US health-care costs influenced by laboratory tests when compared to those not influenced by laboratory testing.
With diagnostic activities in anatomic and clinical pathology/laboratory medicine as the largest part of their medical specialty, pathologists can significantly impact value-based care and population health by reducing costs and improving the quality of patient care. 9,10 While increasing the speed and accuracy of providing a diagnosis has been a historic goal of pathologists, greater emphasis should be placed on optimizing the ability of a provider and/or patient to initiate appropriate intervention in a timely fashion. It is well understood that earlier intervention improves outcomes and reduces costs. For example, the engagement of a pathologist who discusses biopsy findings proactively with the treating clinician can reduce days of unnecessary waiting for a report to initiate treatment as well as increase the chances of choosing an effective treatment. Without effective engagement from experts in anatomic and clinical pathology/laboratory medicine, the converse is also true: Unnecessary delays and errors in interpretation clearly lead to poorer clinical outcomes and increased costs. 11
Historically, the quality improvement role of pathologists has been in the analytic phase of laboratory testing. 12 The ongoing pivot to a value-based health-care payment system has resulted in an increased effort by pathologists to improve appropriate test ordering (the “pre–pre” analytic phase) and test interpretation (the “post–post” analytic phase). 13 Published examples of interventions illustrate the diversity of opportunities available: pre–pre analytic utilization management (including decision supports) to address the long-standing “culture of ordering” that leads to the costs and safety hazards associated with overutilization 14 -16 and decreasing post–post analytic phase misinterpretation of test results to reduce diagnostic errors. By embracing these roles, pathologists can decrease health-care costs and improve quality, thus creating value for health-care systems. 17
Pathologists have been actively involved in many areas critical to the implementation of population health and value-based health care. Four such areas where pathologists have the opportunity to assume an even greater role and provide leadership include utilization management, precision medicine, reducing diagnostic errors, and improving health-care outcomes. Pathologists should seize the opportunity to improve health-care value in these domains. In addition to improving public health, the role for pathologists in population health and value-based care is essential for the profession to grow and thrive, particularly as reimbursement shifts away from traditional models to reward improved outcomes and efficiency.
Utilization Management
Clinical Scenario
A 45-year-old male patient arrives at the emergency department with a chief complaint of chest pain. The patient is slightly overweight and does not exercise. He has no other risk factors for coronary artery disease. An electrocardiogram is within normal limits. Blood is drawn in this hospital for creatine kinase (CK) and creatine kinase-MB (CKMB) (MB index) and troponin I. Although troponin values are negative, CK and CKMB are elevated, the patient is admitted for observation. Follow-up does not demonstrate evidence of a myocardial infarct (MI) or any evidence of myocardial ischemia.
Although the accepted standard for exclusion of an MI is a normal value for troponin, the use of redundant cardiac markers is still prevalent in the United States. Physicians often argue that the tests are inexpensive; unfortunately, they fail to consider that the cascade of decisions based upon unnecessary tests can be significant. Consider the cost of a prolonged emergency department visit and an unnecessary admission for thousands of patients across the country as well. The cost of the admission and further diagnostic workup not only contribute to national health-care expenditures but also to individual patients’ out-of-pocket costs as well as time off work and other social costs. There are significant emotional costs of fear, anxiety, and concern to patients, families, and friends during periods of diagnostic and therapeutic uncertainty, as well as significant health risks for the patient when invasive procedures such as cardiac catheterization are involved. 18
Clinicians from other specialties may be aware of guidelines but may still retain low-value practices from simple momentum bias (we do not want to change unless a great reason is provided). 16 There is evidence that pathologists need to review data from their own institutions in order to show the potential for harm associated with ordering the wrong test at the wrong time or not ordering the right test at the right time. 18,19 Data about the ordering practices linked to actual outcomes can address the optimism bias inherent in human nature that “more is better” and that unconventional reasons for intervention will improve care. 18,19
The adoption of EMR and computerized order entry (CPOE) have facilitated laboratory test ordering, data collection, and analysis, 20 as well as interventions to reduce necessary and unnecessary testing. 18,21 -23 In theory, utilization management has already become a target for inpatient clinical laboratory services, as payment for laboratory testing has been reduced, particularly in the inpatient setting. A systematic review of publications between 1997 and 2012 identified more than 34 000 citations with medical subject headings for the combination of “utilization” and “laboratory test(s).” A discouraging but not surprising finding was that a review of these studies using strict criteria found only 42 (0.1%) of them were well-done. 24
The most common targets of utilization management are unnecessary, redundant, or duplicative tests, whose elimination could potentially reduce laboratory costs 16% to 20%. 24,25 Underutilization of tests leading to delayed or missed diagnosis is 2- to 3-fold (44%-45%) more common than overutilization and likewise deserves intervention. 24 -26 In terms of health outcomes, underutilization is likely more important, yet it does not have the same current national advocacy and that lack of parallel interest is problematic. One study in a critical discipline (bleeding and thrombosis) found that underutilization of laboratory tests resulted in only 55% of patients receiving appropriate care. 25 Difficult clinical scenarios are not the only setting for serious underutilization. A minority of US patients receive all their high-priority clinical preventive services, including indicated laboratory tests. 27
Changes to CPOE, including best practice alerts, have been used to encourage orders of needed tests, to discourage duplicative and obsolete testing, and to prevent misordering of “look-alike” tests. 22,23,28 It is increasingly recognized that CPOE changes alone achieve only a part of the needed result 29,30 and that a multimodal approach involving clinical colleagues is often more effective. 18,23,31 -33 Other forms of utilization management can involve removing tests from the menu (in effect creating “test formularies”), requiring a pathologist review of specific tests, especially low-volume, high-cost reference laboratory tests, and limiting some testing to expert subspecialists. 23,28
Test algorithms are increasingly used after the clinician orders an initial test. Consistent use of laboratory recommended algorithms decreases costs significantly without concomitant decrease in quality; one large urban academic center decreased inpatient test utilization and blood component utilization (often reimbursed in a bundled payment such as a diagnosis-related group (DRG)) by 26% for the average number of tests per patient discharge and saved the hospital an estimated $1.7 million per year over 10 years. 23 Targeted tests have included both rare and expensive genetics test, and common and inexpensive tests such as basic metabolic profiles and complete blood counts. 29 The recent and important efforts of the National “Choosing Wisely” campaign have put a welcome emphasis on overutilization. 34 Pathologists can take pride in the cooperative approaches that have emphasized laboratory testing in so many of the “Choosing Wisely” recommendations for less intensive care. However, we should be concerned that there is no parallel effort to address underutilization, especially where it can improve targeted therapy.
An emerging literature suggests that utilization management at the systems level is “the” important opportunity area for pathology expertise. 21 Pathologists must be prepared to participate in and/or lead this process as a routine part of practice, particularly since inclusions of trainees in quality improvement studies are an Accreditation Council for Graduate Medical Education (ACGME) requirement for all residencies. While downstream savings associated with systems interventions are likely to lead to the greatest value for society and the biggest change in pathology practice, 18,24,28 these savings have been very difficult to quantify. 18 Absent evidence, hospital administrators may not invest, federal and other insurers may not recognize the work as having relative value, and funders of research may continue to ignore the size, scope, and importance of the opportunity. As in every other investment that is about the health of the public, the absence of evidence on the value of utilization management threatens the role of pathology and the overall performance of the health-care system. The importance of pathologists becoming engaged in health services research to demonstrate the value of laboratory utilization management cannot be overstated.
Precision Medicine
Expenditures for laboratory testing are projected to increase disproportionately to other diagnostic costs, largely due to the projected rise in genetic tests from $5 billion in 2010 to $15 to 25 billion in 2021. 35 However, the anticipated problem of increased costs for laboratory testing is small in comparison to its downstream impact. Pathologists need to initiate and be actively involved in evaluating the clinical utility of each new test at the time it is proposed for introduction. Pathology expertise is essential to accurately assess the clinical benefit and calculate the economic impact to determine true value. As an example, there is little value in performing a more accurate genetic test for cystic fibrosis in advance of performing a far less expensive chloride sweat test as a screening test. 36
Pathology trainees must be given the expectation that this test assessment will be part of their job along with the educational experience to perform test assessment effectively. This requires familiarity with record-keeping and analytics and the ability to address issues such as the concordance of marketed claims with actual test performance, 37 the health-care impact relative to the cost, and potential ethical conflicts related to the introduction of new tests demanded by clinicians.
Extensive pathology involvement can help address current public skepticism about aspects of precision medicine. 38 In particular, it is an opportunity to compare the effectiveness of next-generation sequencing-based tests. 39 The clinical utility of these tests is complicated by variations in data collected by different technical platforms and the complexity of the data generated. 37,39 In addition to traditional evaluation of diagnostic and clinical validity, more complex economic analyses may be necessary to provide justification for the costs of such tests. 40
Despite these issues, there are many situations where the significant clinical benefit and value of such tests justify their current use. A good example is the successful evaluation of companion diagnostics for targeted oncology therapies. 41 Although such testing can be quite expensive, the benefit is that only patients with the targeted genetic mutation who are likely to respond are treated with the even more expensive targeted therapeutic, while those lacking the mutation would receive futile and expensive care, with attendant risks for unnecessary adverse events. 42 -44 Another example is in the diagnosis of infections, where rapid molecular testing provides a quicker diagnosis compared to standard testing, therefore improving patient outcomes by reducing mortality, morbidity, hospital length of stay, and inappropriate antibiotic use. 45,46 Molecular testing has also been applied effectively in anatomic pathology; an example is in testing equivocal thyroid cytology to better triage patients for surgery. 47,48 An increasing number of these and other new tests demonstrate clinical efficacy and illustrate value for population health. 49
Screening tests are another important area of growth. The most well-known adjunct or replacement of a traditional screening tool is the test for high-risk human papillomavirus. 29,50 -53 Many other tests are under development with pathologists involved in creation of guidelines and algorithms. 54 Molecular testing is increasingly used for noninvasive prenatal screening. 55 When pathologists and genetic counselors work with clinicians to insure appropriateness of testing and interpretation of results, the value is maximized. 55 -57 With pathologist guidance in the preanalytic and postanalytic phases of testing, molecular tests will improve timeliness of diagnosis, reduce false negatives and false positives by defining the right population with high pretest probability for the known performance of the test, and decrease downstream medical errors and costs.
Reducing Diagnostic Errors
Measurement of error is an important step in identifying and reducing errors, and the autopsy is the historical starting point for identifying medical errors. 58 -60 This power to detect large and small diagnostic error is known to persist in numerous studies, despite increasingly sophisticated diagnostic techniques including imaging. 61 -67 Unfortunately, although the value of the autopsy in detecting diagnostic errors is well-documented, the autopsy rate continues to fall in both academic and nonacademic hospitals. 68,69
As autopsies for the sake of continuous quality improvement and trainee learning diminish in frequency at many hospitals, especially outside academic medical centers, a related concern is that uncaught errors are not entered onto death certificates, thus compromising their quality for subsequent mortality studies. Public health is degraded when error is missed and is further degraded when summary data are compromised by the absence of quality approaches. Surgical pathology diagnoses also serve as feedback for medical errors to clinicians and those in training. Pathologists reviewing surgical pathology cases can detect trends for inappropriate management, collect and review data, and intervene with clinical colleagues to improve patient outcomes and reduce cost. 19
But errors in the realm of laboratory medicine are more pernicious and, perhaps, pervasive. Misutilization—the ordering of laboratory tests that are inappropriate for the clinical questions being asked—is fostered by the ever-increasing number of available laboratory tests and the inability of busy physicians to stay abreast of their utility. 56,70 -72 Indeed, a resolution was recently passed by the House of Delegates of the American Medical Association to close potential gaps in the training of physicians in use and interpretation of laboratory tests. 73 The following case illustrates the seriousness of this issue.
Clinical Scenario
A patient receives a laboratory test to diagnose a disease with a population prevalence of 1%. The treatment for this disease carries significant risk for morbidity due to side effects of the therapy. The test is positive but actually a false-positive result. The clinician, reading the test characteristics of 95% specificity and 90% sensitivity, decides the test is very specific and treats the patient with resulting complications.
Consider the outcomes for 1000 patients. A negative result offers 99.9% probability that the patient does not have the disease. The test in this situation is very useful for excluding patients who do not have disease. However, a positive result offers no such reassurance that the patient has the disease. The chance of a patient having the disease given a positive test is less than 20%, that is, if the laboratory test is used to make the decision more than 5 patients without disease will be treated for every patient with the disease. The lower the prevalence of a disease, the more likely that a positive result is a false positive. As prevalence rises, the positive predictive value rises and the negative predictive value falls, so that a positive test result is less helpful for a rare disease and a negative result is less helpful for a common disease. The inability of many physicians to interpret tests correctly has drawn attention in the lay press. 74 The addition of Bayesian pretest probability to laboratory testing is an operational way to think of the convergence of pathology and public health. In this scenario, some readers may conclude that the test order is necessarily incorrect. That interpretation is neither implied nor precluded in this scenario; the test may well be required in order to take the next step toward a correct diagnosis. The correct message is that the clinical interpretation requires expertise informed by experience with test performance and understanding of the population context.
Reducing diagnostic error, the subject of a recent National Academy of Medicine (NAM) report, has become an important goal for American medicine, as nearly all patients will experience a diagnostic error in their lifetime.
58,75
-77
Diagnostic error is considered to be a failure of either the establishment of an accurate and timely explanation for a patient’s health problems and/or failure to accurately communicate this to the patient.
58
The diagnostic process features complex steps in the preanalytic, analytic, and postanalytic phases, with each step providing a chance for different types of critical errors (Figure 3). Reduction in true analytic errors is where pathologists have been most engaged, and there remain ample opportunities to further reduce analytic errors in quality control, sample identification, and test interference.
78
However, true analytic errors are estimated to be
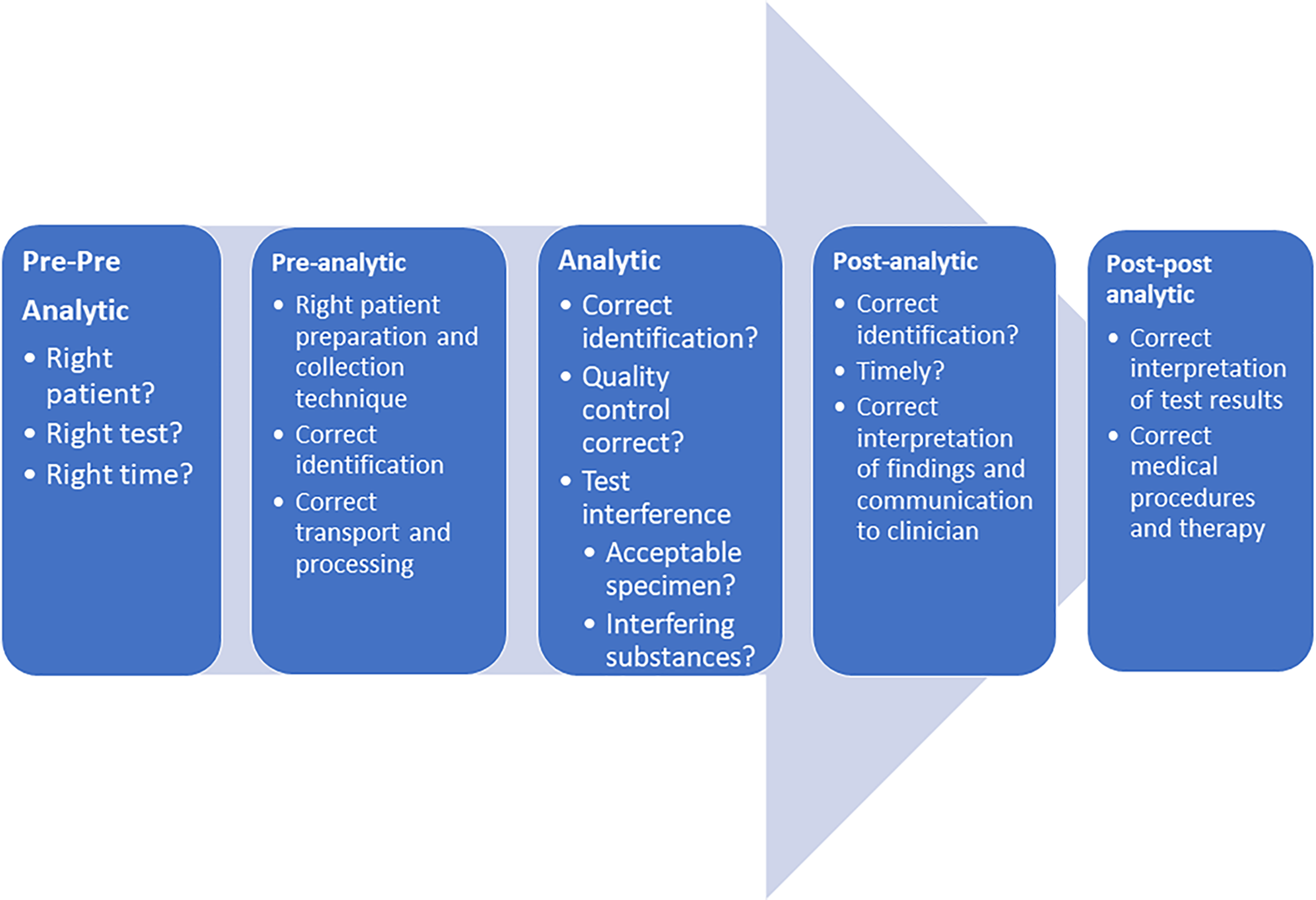
An updated view of the analytic process with steps to potentially reduce critical diagnostic errors.
As mentioned earlier, most of the errors in clinical pathology occur in the preanalytic and postanalytic phases. 78 When clinicians do not order the correct tests (pre–pre analytic) or misinterpret laboratory results (post–post analytic), misdiagnosis or delayed diagnosis are possible, 82 which diminish the quality of care and increase costs. The role of pathologists in educating clinicians, guiding utilization, and interpreting results will become even more critical, as the number and complexity of tests continue to increase. Laposata and Cohen (both members of the NAM committee) have advocated pathologist involvement in many areas to address medical errors, such as increase the teaching of laboratory medicine in medical school and beyond, optimize laboratory information systems and improve the timely reporting of results, provide feedback to clinicians on diagnostic errors and near-misses, and acknowledge and learn from their own mistakes. 83,84
There is substantial value for pathologists to become more engaged in the interpretation and application of laboratory tests, especially as consultants with clinical colleagues, educators of health providers, and investigators of diagnostic process and errors. Each of these activities can add value to health-care delivery by improving quality of care and reducing overall costs. It is largely up to pathologists to make the case to receive adequate and appropriate resources at the institutional and national level to support these activities. Thus, pathologists should be prepared to document the value of these efforts. As laboratory testing is increasingly centralized and outsourced to reference laboratory test results, a serious concern is the potential for a perceived lack of need for such activities by local pathologists. The advantage that local pathologists have is knowing the local patterns of utilization in their communities, including opportunities for improvement and direct collaboration with local medical staff as part of the integrated provider team. Several excellent examples of success have been demonstrated in both anatomic and clinical pathology. It is noteworthy that the NAM report made a major recommendation to include pathologists as diagnostic experts, providing a firm basis for pathologists to assume these roles as fully integrated members of the diagnostic team. 83 Finally, pathologists can serve as educators for provider and patients in point-of-care testing (POCT) such as glucose or international normalized ratio (INR) testing for self-management of diabetes and warfarin.
Improving Health-Care Outcomes
As noted earlier, the pathology “test” with the longest record for improving safety and outcomes has been the autopsy. Following the dawn of modern Laboratory Medicine and Anatomic Pathology in the latter half of the 19th century, the 20th century saw the maturation of these disciplines as a foundational pillar of modern medicine, with discoveries through experimental pathology to match. The challenge—and opportunity—for pathology and laboratory medicine in the 21st century is how the specialty will respond to the promise of precision medicine and population health.
Fortunately, the clinical laboratory (inclusive of Anatomic Pathology and the diagnostics of “Precision Medicine”) is ideally placed to help convert health care from “sick care” to “wellness care.” 10 Over the course of an individual’s lifetime, clinical laboratory diagnostics inform the individual and her or his health-care provider of their wellness status, their potential risk for developing morbid conditions (acute or chronic), and the actual advent of those conditions. To the extent that clinical laboratories have comprehensive records on a regional population, it is precisely those laboratories that can provide leadership in empowering population health programming to serve that region. In the simplest sense, laboratory professionals see the diagnostic data first and are the subject matter experts in test results interpretation and potential application.
In order to play this role, laboratory professionals (medical and technical alike) need first to look at their own data. In the transactional world of current medicine, the treating physician orders the diagnostic testing, the clinical laboratory provides the analytical results, those results are transmitted in atomized fashion back to the treating physician and her or his clinical care team, and patient management decisions are made on a one-by-one basis. At the very least, and on behalf of individual patients, the expertise and resources of the laboratory can be harnessed through diagnostic management teams, as described earlier. But to convert this expertise to the population level, the laboratory must provide programmatic leadership. Termed “Clinical Lab 2.0” by the Project Santa Fe Group,
10
opportunities include but are not limited to reducing time to diagnosis and time to intervention; closing gaps in care, as through alerts, notifications, improvements in patient access, and tracking of clinical outcomes; powering wellness care screening, including triggering early intervention; triggering real-time risk escalation and intervention; laboratory and pharmacy coordination, both for acute conditions (such as antibiotic stewardship) and chronic disease management; and building the evidence base for the efficacy and utility of precision medicine, pharmacogenomics, and interventions instituted at the population level.
These population health leadership activities can play out in both the inpatient and outpatient settings. 85,86 Table 1 provides examples of laboratory-led population health initiatives, which have provided quantitative evidence of realized value in improving patient outcomes and the cost of delivering health care. 87 -92 For those individuals engaged in such projects, the feeling is that we have only scratched the surface of what is possible in this 21st century.
Laboratory-Led Population Health Initiatives.*
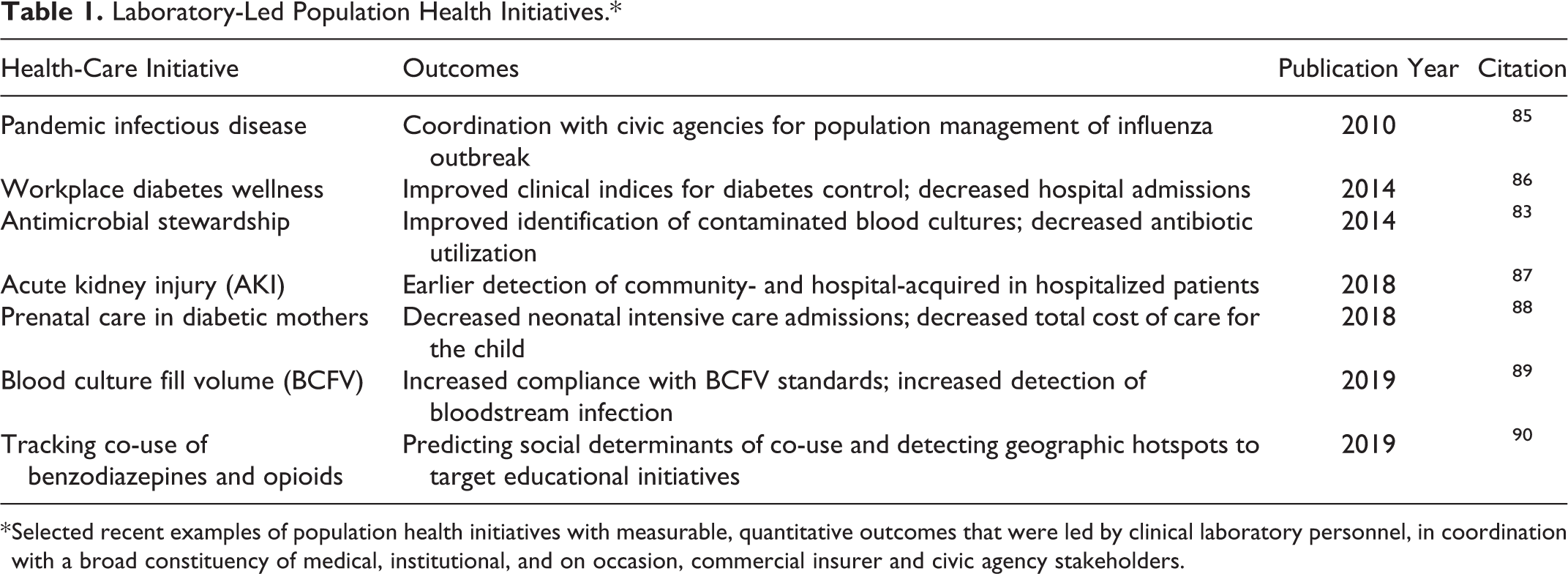
* Selected recent examples of population health initiatives with measurable, quantitative outcomes that were led by clinical laboratory personnel, in coordination with a broad constituency of medical, institutional, and on occasion, commercial insurer and civic agency stakeholders.
Informatics and emerging data sciences are critical to providing population health and precision medicine, and it is imperative that laboratory leaders, who manage, understand, and are the “first to see” the data, are actively engaged with their clinical colleagues and administrators to make such information actionable. The first priority should be addressing the needs of stakeholders:
Patients: Laboratory data analytics are essential components of clinical care management programs designed to improve safety and meet the needs of patients individually (precision medicine) and regionally (population health). In addition, most patients frequently access EMR laboratory results in advance of visits with their providers. Pathologists should explore the opportunity of using this “patient interface” to directly engage patients and improve population health.
Clinical providers: Laboratory data are necessary to develop evidence-based decision support tools to improve clinical practice efficiency and precision, reduce medical errors, manage potential gaps in patient care, and improve interpretation of laboratory testing.
Institutional quality: Laboratory data inform a substantial portion of institutional performance metrics, including gaps in care, cost-effectiveness, care coordination, and appropriate benchmark comparisons.
93
-95
Institutional finance: Payment systems, especially those that are value-based, are driven by quality metric ratings across inpatient and ambulatory settings.
96
Laboratory data are also key for “risk-adjusting” patients who are members of managed care plans; failure to properly risk adjust these patients can have strong negative impact on financial outcomes.
97
Payers: Beyond the obligate linkage of data to inform actuarial analysis and design of health-care plans, the quality and financial metrics mentioned earlier are key mechanisms by which payers assess the quality of health care being delivered to their members (patients).
Benefits design: Laboratory data initiatives will become increasingly important in Benefits Design and Benefits Coverage for managed care and value-based health plans. The recent National Coverage Decision by the Centers for Medicaid and Medicare Services (CMS) approved a major molecular diagnostic laboratory for Medicare coverage, simultaneous with FDA approval of their test offering.
98
This joint ruling by CMS and FDA was based on a process which should be kept in mind by other laboratories seeking to obtain laboratory testing coverage approvals by payers.
Discussion
We have described 4 major initiative areas that are critical to population health in which pathologists have the opportunity to provide significant additional value and a leadership role, but only to the extent and speed that the pathology community is willing and able to engage. Pharmacists have markedly improved safety and efficacy by actively participating in clinical rounds, demonstrating the importance of active engagement that should be a model for pathologists. 99 -101
A major constraint to all these initiatives is the lack of dedicated funding for the considerable amount of pathologist and informatics effort that must go into population health initiatives, even though they improve quality and reduce costs disproportionately to needed investment. 102 Unfortunately, reimbursement policies for tests can drive inappropriate utilization from both directions (ie, overutilization in a fee-for-service model and underutilization in a capitated model). However, as pointed out earlier, the test is not the important cost; the downstream costs are what matter most. Test costs should be tied to processes that put a premium on getting the most appropriate test at the right time for the right patient and assuring timely action on these results.
Investments in accurate ordering and interpretation have been limited predominantly to academic centers 102 and large integrated systems with accompanying investments in clinical pathways and outcomes. The greatest returns in value for the cost of tests are in the processes that improve patient outcomes and reduced total cost of care. Pathologists are the most knowledgeable professionals in this arena and should become more actively engaged in educating payers and hospital administrators that the incremental costs for improving safety and utilization are small in comparison to potential savings from more efficient total cost of care. 23 83
In addition, pathologists should work with clinical colleagues, health system leaders, patient advocates, and professional societies to educate federal agencies such as Centers for Medicare and Medicaid Services (CMS), National Institutes of Health (NIH), Centers for Disease Control and Prevention (CDC), Food and Drug Administration (FDA), Patient-Centered Outcomes Research Institute (PCORI), and Agency for Healthcare Research and Quality (AHRQ) to fund demonstration projects and studies addressing safety and best practices for test utilization. Pathologists should also seek to work directly with payers to achieve alignment in managed care program design and execution. Unfortunately, pathologists have not engaged effectively with these stakeholders, and not surprisingly, these federal agencies have provided inadequate funding for studying the important impact of test quality and utilization on reducing diagnostic errors and improving quality. 83 Moreover, the number of US pathologists has decreased significantly in both absolute (−17.5%; 15 568-12 839) and population-adjusted (−23.6%; 5.16-3.94 per 100 000) totals from 2007 to 2017. 76 This alarming trend has diminished the ability of pathology and pathologists to help advance population health and precision medicine and limited their contributions to the research and education needed to realize these goals. 77
Pathologists have broad expertise that impacts the care of patients across all specialties, which qualify them to be “systems-level” consultants. Some pathologists have acquired the skills to leverage this expertise to become valued members of the leadership teams of health-care organizations but more need to assume these roles to help the profession and the patients being served. Pathology training also should reflect these opportunities and the value that our profession can bring to health care, important for attracting a new generation of pathologists. Training should include a focus on data science, drawing on the rich data sources emanating from pathology and the clinical laboratory. Although pathologists already have considerable training in the statistical methods used to validate our analytic processes and in systems thinking as well as operations approaches required to direct our laboratories, most pathologists report that they would benefit from more statistics training. 103 Training in health systems science should be provided to show how the skills and knowledge of pathologists can be applied to designing and potentially leading programs to improve health-care delivery. Likewise, basic principles of public health should be provided, especially in epidemiology, as it relates to the correlation of test utilization with population health. Enhanced training in communication and negotiation will also be important for pathologists to become more engaged with practicing in clinical teams, dealing with administrators and payers, and educating stakeholders.
The next generation of pathologists must be able to recognize and seek rigorous study design for comparative effectiveness, manage and utilize summary data for error reduction studies and control of ordering, introduce alterations to medical records that guide or steer clinicians to the right test, and communicate the need to change and the consequences of current trends. Pathology training programs should reach out to other specialties to train in the laboratory as well as send pathology house staff on rounds to improve test ordering and management using laboratory test results. 104 An understanding of health economics will also be required, as pathologists help to determine which methods are cost- as well as clinically effective. Training should likewise emphasize dissemination and implementation sciences (knowledge translation or knowledge diffusion). Pathology leadership of diagnostic teams, visible beyond the walls of the laboratory, armed with data, and facilitating changes in the wards, the emergency department, and the C-suite, will attract the best and brightest of medical students to the field.
With payers moving to value-based models of compensation, traditional Part B billing and reimbursement is at risk. 105 While pathologists will continue to perform direct patient care services such as signing out surgical pathology specimens, the inexorable move toward value-based reimbursement will likely reduce payment for these services, which currently constitute a major portion of practice revenue. As laboratory test reimbursement likewise shrinks, the hospital or academic laboratory itself is at risk, which implies that Part A payments also will be at risk. 10,106 The challenge for pathologists will be not only to add value but to also quantitatively prove to payers and health systems of the value we have added and of their return on investment for supporting pathologists in these new activities.
Conclusion
The shift from fee-for-service to value-based payment and the implementation of population health and precision medicine are strong incentives for pathologists to focus on the value they can bring to patient care. For the profession to thrive, pathologists must focus on extending their role beyond the laboratory. Pathologists must become critical members of the health-care provider team as physicians and consultants, with leadership responsibility for correlating laboratory testing to patient outcomes and error prevention. Pathologists must leverage their skills and experience to improve quality and cost-effectiveness. Pathologists must train a new generation of pathologists who understand the role of pathology in value-based care and precision medicine. Pathologists must engage in health services research to generate the evidence that supports their value in health-care delivery. Pathologists must proactively engage in educating other stakeholders, both within and outside the health-care delivery system, on the value they bring to population health. Alternatively, if pathologists are unable or unwilling to take advantage of these challenges and opportunities, pathology likely will be viewed as a cost and liability and will diminish as a profession.
Footnotes
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
