Abstract
Professionalism and physician well-being are important topics in academic medicine. Lapses in professional judgment may lead to disciplinary action and put patient’s health at risk. Within medical education, students and trainees are exposed to professionalism in the institution’s formal curriculum and hidden curriculum. Development of professionalism starts early in medical school. Trainees entering graduate medical education already have developed professional behavior. As a learned behavior, development of professional behavior is modifiable. In addition to role modeling by faculty, other modalities are needed. Use of case vignettes based on real-life issues encountered in trainee and faculty behavior can serve as a basis for continued development of professionalism in trainees. Based on the experience of program directors and pathology educators, case vignettes were developed in the domains of service, research, and education and subdivided into the areas of duty, integrity, and respect. General and specific questions pertaining to each case were generated to reinforce model behavior and overcome professionalism issues encountered in the hidden curriculum. To address physician burnout, cases were generated to provide trainees with the skills to deal with burnout and promote well-being.
Introduction
Professionalism, defined as the aspiration “toward altruism, accountability, excellence, duty, service, honor, integrity, and respect for others,” 1 is undoubtedly an important component of medical education and the profession of medicine as a whole. 2 –4 Lapses in professionalism have led to disciplinary actions by state medical licensing boards and have affected board certification by various medical specialties. 5 –7 Unprofessional behavior is a cause for disciplinary action against medical students, residents, and fellows, and practicing physicians. 5 Physician well-being and professional burnout have also become important health-care issues. 8 –10
The Accreditation Council on Graduate Medical Education (ACGME) recognizing the importance of professionalism in medicine adopted professionalism along with the American Board of Medical Specialties as 1 of their 6 core competencies in 1999.
11,12
In 2013, the ACGME (Pathology Residency Review Committee [RRC]) and the American Board of Pathology in a joint initiative formulated its 27 residency training milestones that included 6 Milestones dedicated to professionalism (Table 1).
13
The ACGME updated its professionalism common program requirements (VI.B) in March 2017 (Table 2) and is in the process of formulating new milestones.
3
The proposed professionalism milestones include: professional behavior and ethical principles, accountability/conscientiousness, and self-awareness and help-seeking.
14
ACGME Common Program Requirements for Professionalism (VI.B.) 3

Abbreviation: ACGME, Accreditation Council on Graduate Medical Education.
Professional (physician) burnout and well-being are addressed in the self-awareness and help-seeking milestone and in the revised ACGME common program requirement VI.C. 3 (Table 3)
ACGME Common Program Requirements for Well-Being. (VI.C.) 3

Abbreviation: ACGME, Accreditation Council on Graduate Medical Education.
Medical education proceeds through a continuum from undergraduate (UME, medical school) to graduate (GME, internship/residency/fellowship) education by which the novice student requiring supervision develops into a physician able to practice medicine without supervision. A well-defined curriculum is an accreditation standard in all UME and GME programs (
Trainees entering GME have already started development of their professionalism based on experiences prior to residency including their UME experience. 18 The critical question is what modality or combination of modalities is most effective in continuing the development of professionalism in trainees. Role modeling by faculty is undoubtedly critical. Faculty responsible for development of trainees’ professionalism are aware that more is needed than just faculty role modeling in the health-care environment. Kirch and colleagues comment that “professionalism must be taught early, longitudinally, and deliberately using both targeted instruction and experiential learning.” 19 (p. 1798) This article outlines a vehicle that can be used by programs to address professionalism in trainees.
A Case-Based Educational Approach
As one of its mandates, the College of American Pathologists’ (CAP) Graduate Medical Education Committee (GMEC) has addressed the issue of professionalism in pathology GME in prior publications. 20,21 In Domen et al, we surveyed program directors (PDs) on how they would respond to lapses in professional behavior as depicted in case vignettes. 20 This publication was followed by Brissette et al, 21 where PDs and residents rated the professionalism of various behaviors. 21 In that survey, PDs and residents consistently identified 6 behaviors ranked from highest to lowest as being unprofessional (Table 4). In addition to the above mentioned behaviors, residents in contrast to program directors commonly rated the following behavior as unprofessional: did not promptly respond to pager or on-call responsibilities (including timely hand-offs). 21
Behaviors Most Consistently Rated Unprofessional by Program Directors and Residents. 21

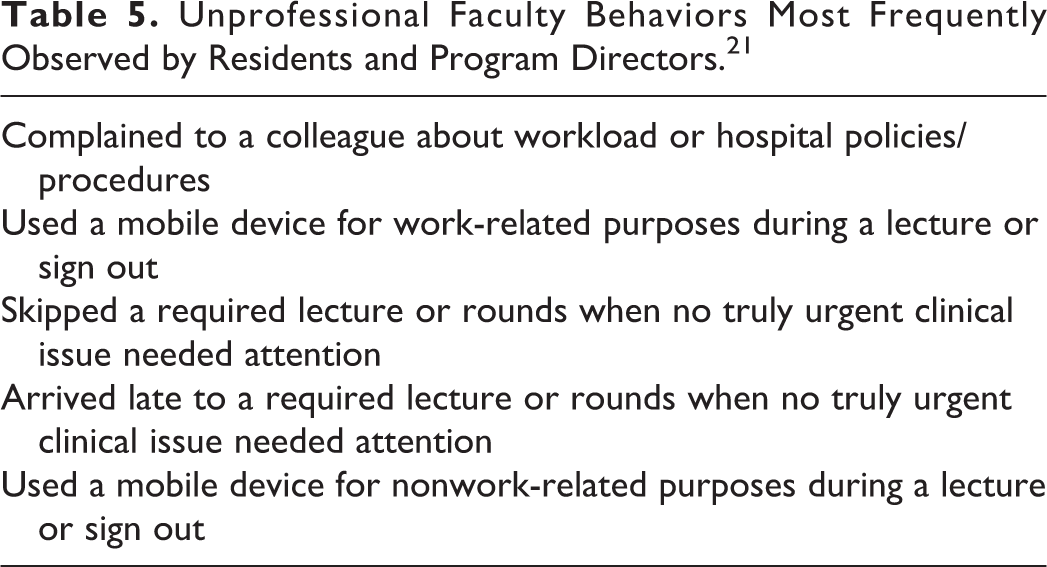
Brissette et al also surveyed residents on their participation in unprofessional behavior and observation of faculty participation in various behaviors. Program directors also reported their observation of resident and faculty behaviors. Residents and PDs most frequently observed the same unprofessional behaviors among faculty ranked from highest to lowest (Table 5). Program directors also observed these same behaviors among residents supporting the importance of the hidden curriculum in resident education.
Unprofessional Faculty Behaviors Most Frequently Observed by Residents and Program Directors. 21

Based on the cumulative experience and feedback from PDs and residents, the GMEC continues to discuss how to best incorporate professionalism development into the GME curriculum. A question that arose after reviewing the survey results from Brissette et al
21
is what curricular changes or tools PDs could use to promote professional behavior: What would be beneficial as part of the formal residency curriculum to address the ambiguities encountered by residents along with the biases they develop from the hidden curriculum? Equally important was asking how best to provide house staff with strategies to deal with the ambiguities encountered to minimize lapses in professional judgment and preclude resident burnout. Given the often situational and multifactorial nature of real-world professionalism challenges, the GMEC sees many benefits to the use of case vignettes focusing on specific themes of professionalism. Case vignettes provide subject matter and a structured format to: identify conflicts of interest, teach effective communication skills, deliver resilience skills, develop a sense of self awareness and a sense of one’s limitations, teach skills to deal with lapses in professional behavior, remediate lapses in professional behavior, develop a team approach to augmenting professional development, minimize professionalism lapses and ameliorate burnout, review key ethical issues that underlie professional behavior, and use as a vehicle for formative assessment.
Creation of Case Vignettes
Themes drawn from elements of unprofessional behavior referenced in our prior publications and from the literature were condensed into 3 domains (service, research, and education) and serve as the basis for case vignettes. The service domain, known also as the competency domain, consists of both the academic requirements and the clinical responsibilities of residency. Within this domain, residents interact with students, peers, faculty, and other health-care professionals including clinical laboratory scientists, histotechnologists, and pathologists’ assistants. The research domain deals with residents performing research with institutional requirements and federal regulations governing human and animal research. The education domain refers to residents delivering content based on curricular objectives to medical students, residents in other specialties, and other laboratory professionals including medical technologists. In this domain, a student–instructor relationship is implied.
Within each domain, the GMEC further clustered the professionalism scenarios into 4 areas: duty, integrity, respect, and resilience. Topics for the cases authored to date are included in Tables 6, 7, and 8. For each theme, cases (Table 9) were developed that could be utilized by PDs and department faculty to engage residents in a dialogue on what is appropriate professional behavior. A set of standard questions that apply to each case vignette were developed (Table 10) as were specific questions for each case (Table 9). The consensus among GMEC members suggested there was not a single correct answer but rather discussion points that need to be raised. The points include the PD’s obligations, local institutional constraints, and accreditation requirements. A subset of the cases were piloted by GMEC members at the Association of Pathology Chairs’ Program Directors Section annual meeting, CAP residency forums, and to house staff supervised by committee members to assess relevance and credibility. 20 Several were also presented at professionalism sessions at the CAP annual meeting. Themes identified as problem areas in the study by Brissette et al compose the majority of cases the GMEC authored. 21
Professionalism Themes and Topics Within the Service (Competency) Domain.
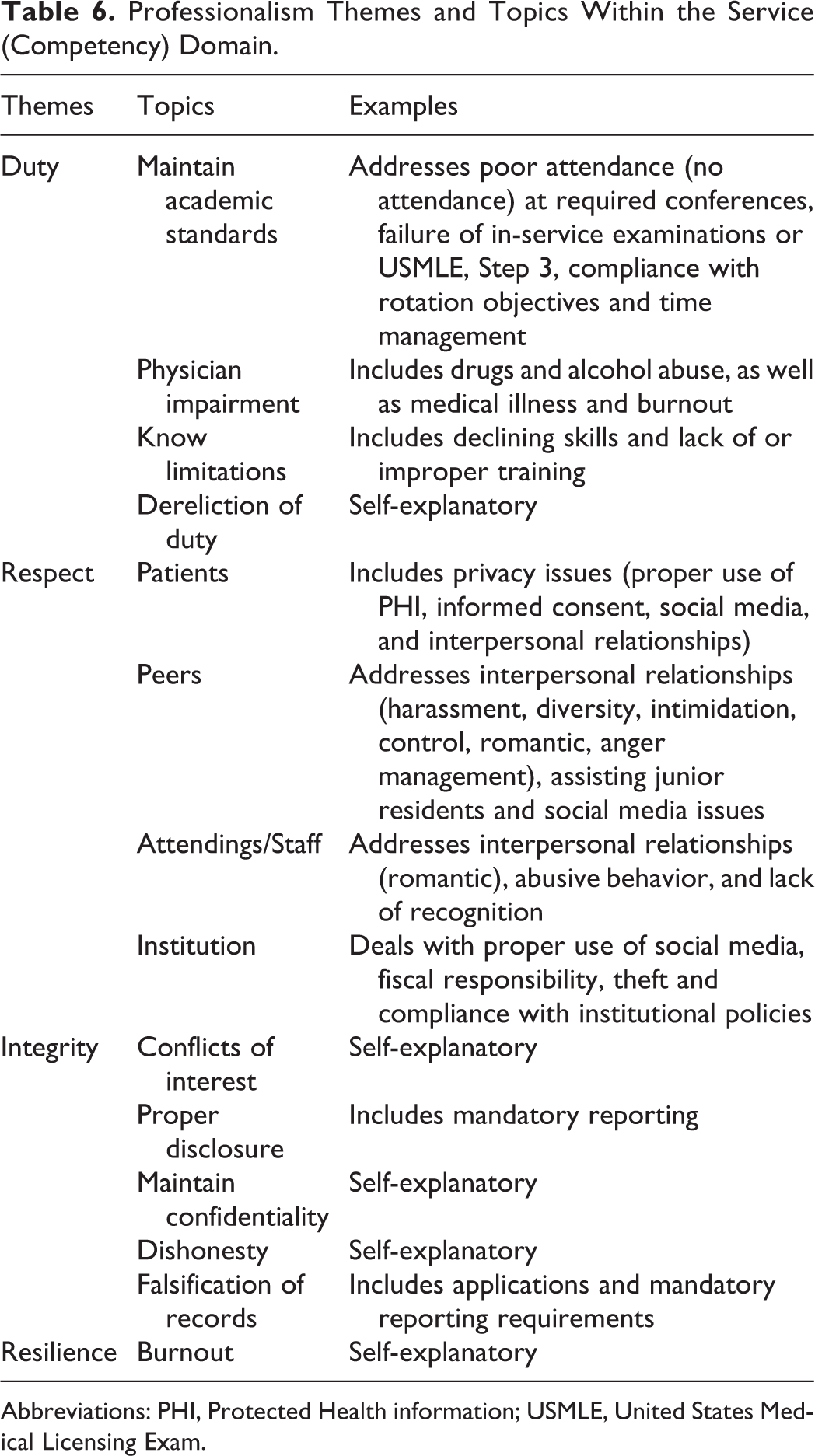
Abbreviations: PHI, Protected Health information; USMLE, United States Medical Licensing Exam.
Professionalism Themes and Topics Within the Research Domain.
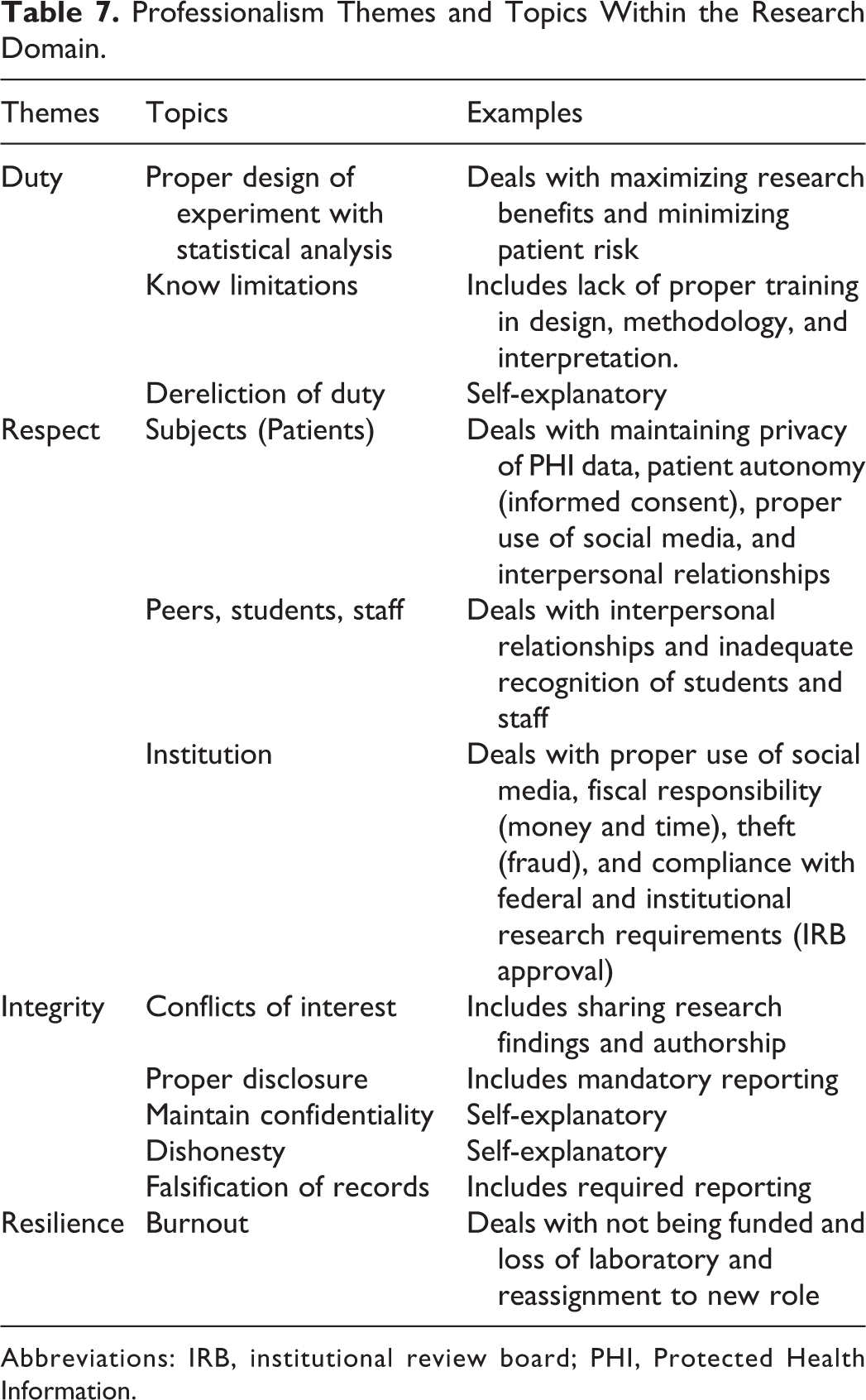
Abbreviations: IRB, institutional review board; PHI, Protected Health Information.
Professionalism Themes and Topics Within the Education Domain.
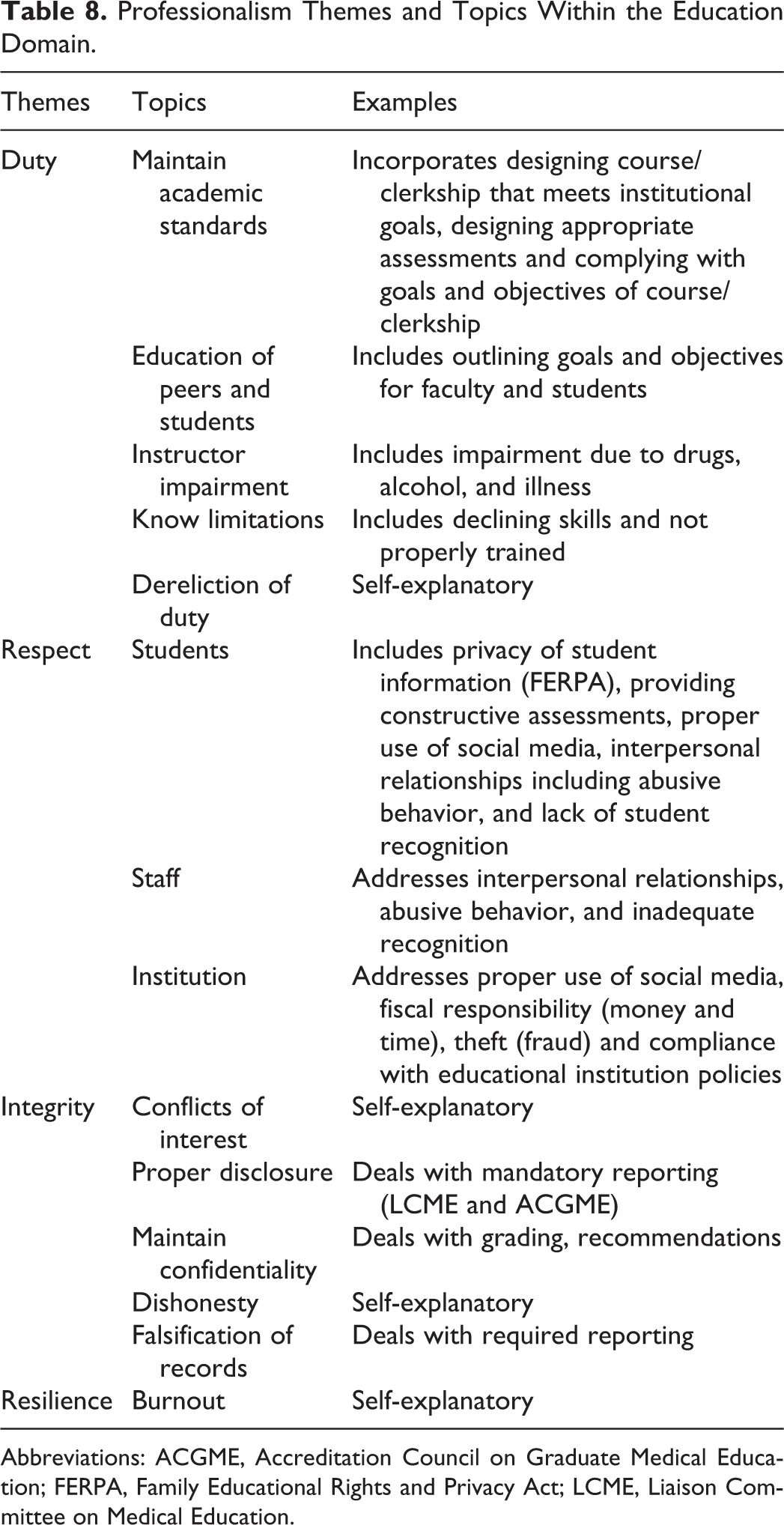
Abbreviations: ACGME, Accreditation Council on Graduate Medical Education; FERPA, Family Educational Rights and Privacy Act; LCME, Liaison Committee on Medical Education.
Selected Cases From the Service (Competency), Education, and Research Domains and on Burnout and Resilience.
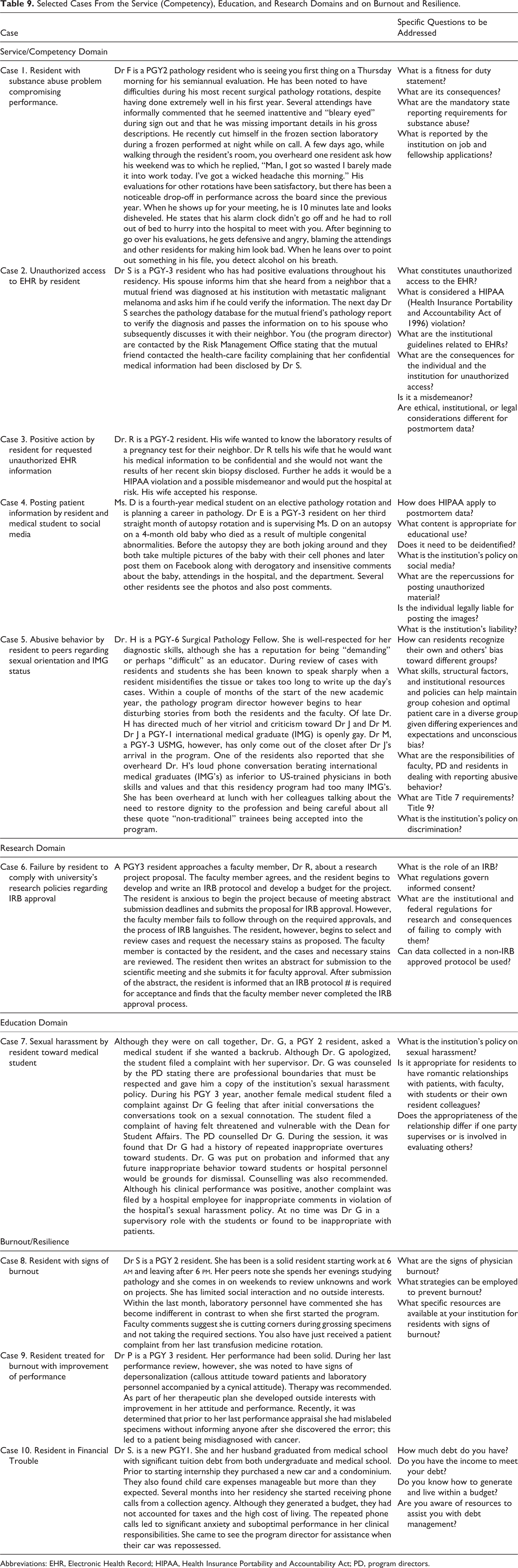
Abbreviations: EHR, Electronic Health Record; HIPAA, Health Insurance Portability and Accountability Act; PD, program directors.
General Discussion Points for All Cases.

The selected GMEC case vignettes in Table 9 from the service, research, and education domains outline common scenarios encountered in pathology GME. The key issue addressed by each case is underlined. As outlined in Tables 9 and 10, the GMEC modeled the use of these scenarios in professionalism development through key questions and discussion of the underlying professional, ethical, and legal considerations. In building these case discussion, for example, the GMEC considered feedback from residents and PDs at different levels of experience and accreditation and legal standards. Resident well-being and skills to enhance resilience were also incorporated as a goal.
Case 1 deals with substance abuse while on duty. Although the outcome in case 1 is fixed, 20 given that many states have mandatory reporting requirements for substance abuse and PDs are required to request a “fitness for duty” evaluation, there is value in discussing the legal ramifications.
There is also value in discussing the responsibility of peers in reporting the problem and whether their intervention could have prevented the case outcome. For example, did the attending pathologist and residents who suspected potential substance abuse have a responsibility to notify the PD or should the PD have been more aware? If peers overlooked the problem and later in the resident’s career, there was a poor patient outcome as a result of a known substance abuse problem, would they feel responsible? 22 Is there a team approach that could be utilized to remediate the resident? This case further allows PDs to address AMA Principles of Medical Ethics, sections 9.3.1 Physician Health and Wellness and 9.3.2 Physician Responsibilities to Impaired Colleagues. 23,24
Case 2 deals with unauthorized access to medical records. The case also raises the possibility of litigation and could be used to educate residents on the role of the institutional and hospital risk management offices and the elements of a negligence lawsuit. 25 This case further allows PDs to address postmortem information (autopsy findings) and AMA Principles of Medical Ethics, section 3.2.2, Confidentiality, Postmortem. 26
Case 3 also deals with access to medical records. In contrast to a lapse in professional judgment, it demonstrates positive behavior. Comparing positive and negative behavior is important for professional development, and the 2 cases could be discussed in tandem. Residents should be encouraged to discuss the skill sets and actions that allowed for a good outcome.
Case 4 deals with posting patient information to social media. Proper use and improper use are discussed along with the institution’s policy and ramification to the individual and institution for improper use. The autopsy authorization form can also be discussed and accepted norms for using clinical material for educational purposes.
Case 5 deals with abusive behavior in the workplace. Ramifications of this behavior on patient care and workload are discussed. The case also allows for a discussion on what should be the department’s response if such an individual applies for a faculty or private practice position. What should be disclosed in a recommendation letter? Are there legal repercussions to such disclosure?
Case 6 is in the research domain. Institutional policies and federal regulations can be discussed. The case also serves as a vehicle for addressing the Belmont report findings, respect for persons, beneficence, and justice. The concepts of informed consent, risk, and benefit assessment and selection of research participants are also part of the dialogue. 27,28
In the education domain, case 7 deals with sexual harassment. The case allows for discussion of the institution’s policy and AMA Principles of Medical Ethics section 9.1.3, Sexual Harassment in the Practice of Medicine and ACGME professionalism standards. 29,30
Cases 8 and 9 focus on time management, physician burnout, and resilience. It is important that training programs address these issues. Resident burnout has a number of associated elements, including “emotional exhaustion”, “depersonalization and cynicism,” and “feelings of inefficacy”. 8 Emotional exhaustion and/or depersonalization were identified in 76% of US medical residents on the Maslach Burnout Inventory. 8 Patient care errors have been associated with burnout. Residents should be aware of the signs of burnout and how to access appropriate interventions. Many of the cases raise these questions and provide a forum for a dialogue on the issue. The cases also allow for a discussion of AMA Principles of Medical Ethics, section 9.2.2, Resident and Fellow Physicians’ Involvement in Patient Care. 31
Case 10 deals with a resident with significant debt that lacks the skill on how to budget salary. Absent financial management skills may lead to excessive anxiety and burnout. 32,33
Discussion
“Professionalism” is a character trait medical students develop which manifests as behavioral change over the course of training.
18
Students entering medical school tend to have a positive altruistic view and a sincere desire to help patients. They expect to be treated with “respect, honesty, and tolerance.”
18
Throughout UME, their view changes as they witness behaviors, positive and negative, in the health-care arena as part of the hidden curriculum.
34
–36
Market forces and societal pressures (eg, television programs such as
Students entering GME have already started their development of professionalism. The critical question is what methods or combination of methods can be deployed to continue the development of professionalism in residents. Residents observe behavior among clinicians, their peers and attendings, and other health-care workers while influencing medical students and other health-care personnel. The hidden curriculum is constantly at work. Recent literature indicates that modifying behavior is the best way to promote professionalism. Identifying positive behaviors while minimizing negative role models is important. 17
The medical education literature deals with different modalities to deliver content, such as lectures and case-based instruction. Lectures tend to be passive and designed to cover a specific theme. Although cases may be incorporated into lectures, small groups with active discussion have a positive effect on learning. Small group teaching with well-defined goals and objectives, a proper attitude of the instructor, and development of rapport with the participants can be highly effective for teaching professionalism. 37 Most pathology residencies vary in size from 8 to 24 trainees, making small group faculty or senior resident-facilitated teaching ideal.
Case vignettes allow for self-reflection, assessment of peers, attendings, staff and patients, and allow residents to develop strategies and tools to deal with ambiguity and lapses in judgement. 38 –41 Another benefit of this approach for PDs is to gain an appreciation of the resident’s perspectives (attitude, social norms, and cultural background). Program directors can take the opportunity to refresh their own knowledge of the program/institutional background based on experience, regulatory, and legal standards and the consequences of the behavior in preparation for the discussion. Where appropriate, strategies can be incorporated into the discussion to modify behavior, promote resilience, and insure that trainees are familiar with institutional policies. Much of the professionalism curriculum in institutions focuses on lapses in judgment; we have furthered developed cases that highlight constructive responses highlighting the elements of professionalism. Another goal for utilizing case vignettes is to counter the hidden curriculum. Case vignettes can be instrumental in aligning the formal curriculum on professionalism with the hidden curriculum encountered in everyday practice. Our cases serve as a tool for program directors to make trainees aware of the hidden curriculum and develop strategies to overcome the negative biases they have encountered and promote positive behavior in their professional development. 21,42,43
The use of case vignettes with residents across medical specialties has demonstrated value in resident professional development. 38,39 Factors to consider in their use include personal attributes and characteristics including perceived identity, unconscious bias and inherent personality traits, interpersonal and interprofessional relationships including functioning in a group (group dynamics), and societal dimensions such as the political and economic framework within and external to the institution. 38 Case vignettes that are realistic and current address these factors. Reflection on case content is part of the experiential process as previously outlined. 19,41
Depending on institutional resources and the program’s curriculum, case vignettes can be employed flexibly to create a meaningful experience and promote professional development. The simplest format is a group discussion led by the PD where residents review the case as a group and answer selected questions. The PD or other facilitator would then give their perspective, followed by a group discussion. Alternatively, residents could be given the cases ahead of time and asked to write answers to the specific questions, reflect on their answers prior to the session and then modify their answers if needed post session. As part of the exercise, PDs should alert trainees to the potential of unconscious bias. Another alternative is to have residents role-play the individuals in the case vignette or to use professional actors to role play in front of a camera. Residents could review the videotapes separately or as a group prior to the discussion. Videotaping allows residents performing away rotations to participate and ensure for accreditation purposes that each resident is exposed to the same curriculum. In many of these scenarios, it is worthwhile to retain the residents’ comments and use the same cases year to year, with residents reflecting on their personal answers over all 4 years of the program to assess the change in their professional development. Based on our prior experience, it is worth seeing how residents would treat the resident who is unprofessional in each of the cases. 20 In several instances, residents felt the problem resident should be dismissed or their contract not renewed versus the PDs who advocated counseling; with repeated exposure to the scenario, residents could observe the evolution in their thinking and approach.
Assessment of resident behavior can be formative, summative, or diagnostic. 44 Norcini and McKinley outline 2 advantages of formative assessment. First, it provides feedback to residents and PDs to guide learning (professional development) and second, the act of assessment itself creates a learning environment. 44 As discussed earlier, residents should be able to perform a number of tasks by the end of training as outlined in the ACGME professionalism core competency. 11 Case vignettes have a role in formative assessment. Their role in summative assessment is open to debate. 45 Residents can be given the cases and generate a response to the general and specific questions for the cases. Although the GMEC position is that there is no single correct answer to many of the cases, there is consensus opinion and applicable guidelines or law for many of the broader issues that could be provided to the residents as formative feedback, for example, AMA Principles of Medical Ethics for service (competency) domain, and the Belmont Report for research domain. All cases allow for self-reflection, which is critical in professional development. 44
Within the medical and pathology academic communities, professionalism is identified as one of the most important ethical issues. 46,47 Employers rate areas of professionalism, including honesty, interpersonal interactions, knowing ones limitations, and knowing when to ask for help, as critical attributes in hiring recent trainees. 21,48,49 Our experience is that professional development must provide residents with the knowledge, skills, attitudes, and strategies to minimize lapses in judgment and provide them resilience skills to prevent burnout that may lead to compromised patient care. 8,10,50,51 Although there is no substitute for real-world experience, we designed our case vignettes to realistically reflect current issues encountered in GME. Through these simulated cases, residents can role-play and practice positive behaviors while being coached and provided strategies to deal with conflict.
Role-modeling by faculty is undoubtedly also an important modality in professional development. 18,21,46 Wagoner observed that when second-year students were asked what they considered as unprofessional behavior among faculty, the comments included 2 themes: dehumanization of students, colleagues, patients, and others by showing lack of respect, breach of confidentiality, displays of intolerance, or dishonesty and insensitivities based on gender, ethnicity, or cultural beliefs, particularly involving racist or sexist remarks. 18 As discussed earlier, pathology residents have identified specific faculty behaviors as unprofessional. 21
Residents need positive role models; they need to witness positive behavior in faculty to emulate. Negative behavior in role models is counterproductive. Faculty development has a role in developing positive role models and modifying behavior for residents and other laboratory personnel. The GMEC case vignettes can be utilized by institutions for faculty development and promoting faculty well-being as well.
Conclusion
Residents are diverse in their experiences and expectations, and their development of professionalism is based on multiple factors including “experiential learning.”
19
We have found case vignettes a useful vehicle to reinforce model behavior and counter the
Footnotes
Authors’ Note
For Dr Brissette: The views and opinions expressed in this manuscript are those of the author and do not reflect the official policy or position of the Department of Army/Navy/Air Force, Department of Defense or the United States Government.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.

