Abstract
The following fictional case is intended as a learning tool within the Pathology Competencies for Medical Education (PCME), a set of national standards for teaching pathology. These are divided into three basic competencies: Disease Mechanisms and Processes, Organ System Pathology, and Diagnostic Medicine and Therapeutic Pathology. For additional information, and a full list of learning objectives for all three competencies, see http://journals.sagepub.com/doi/10.1177/2374289517715040.
Keywords
Primary Objective
Objective N3.1: Morphologic Features of Neoplasia. Describe the essential morphologic features of neoplasms and indicate how these can be used to diagnose, classify, and predict biological behavior of cancers.
Competency 1: Disease Mechanisms and Processes; Topic N: Neoplasia; Learning Goal 3: Characteristics of Neoplasia.
Patient Presentation
A 39-year-old P3013 woman presented to her gynecologist with complaints of increased bleeding during menstruation, back pain, and a feeling of rectal fullness. Pregnancy test was negative. Her gynecologist palpated a large irregular, asymmetric uterus. The patient underwent hysterectomy.
Diagnostic Findings
Examination of the hysterectomy specimen in surgical pathology showed it to be enlarged and distorted by multiple tumors within the myometrium. Figure 1 is a cross section through the uterus and the largest tumor.
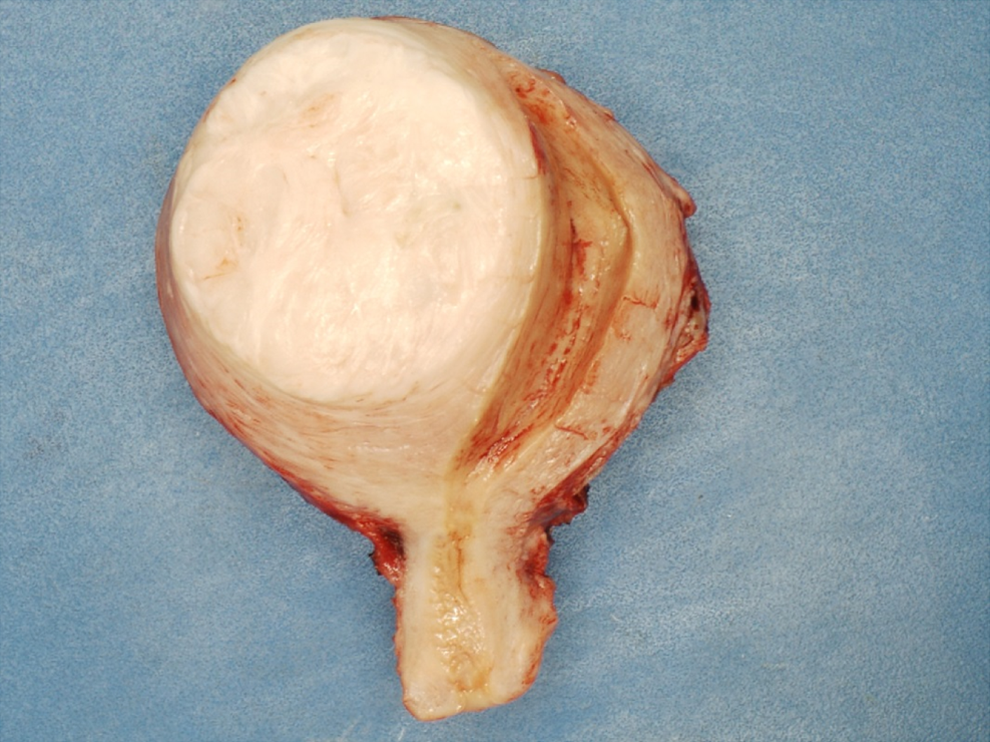
Gross image of the hysterectomy specimen. The cervix is at the bottom of the image. The intramural tumor on the left is compressing the endometrial cavity toward the right.
Questions/Discussion Points
In Figure 1, describe the cut surface of the tumor
The cut surface is homogeneously white. There are no areas of grossly recognizable necrosis or hemorrhage, which may be indicative of more aggressive tumors.
In Figures 1 and 2, how would you describe the border of the tumor nodule with the surrounding uterus?
Figure 2 is a low-power photomicrograph from the specimen. Histological section from the hysterectomy specimen, taken from the intersection of one of the nodules and the adjacent myometrium. The border of the tumor is indicated by arrows (hematoxylin and eosin stain; original magnification 20×).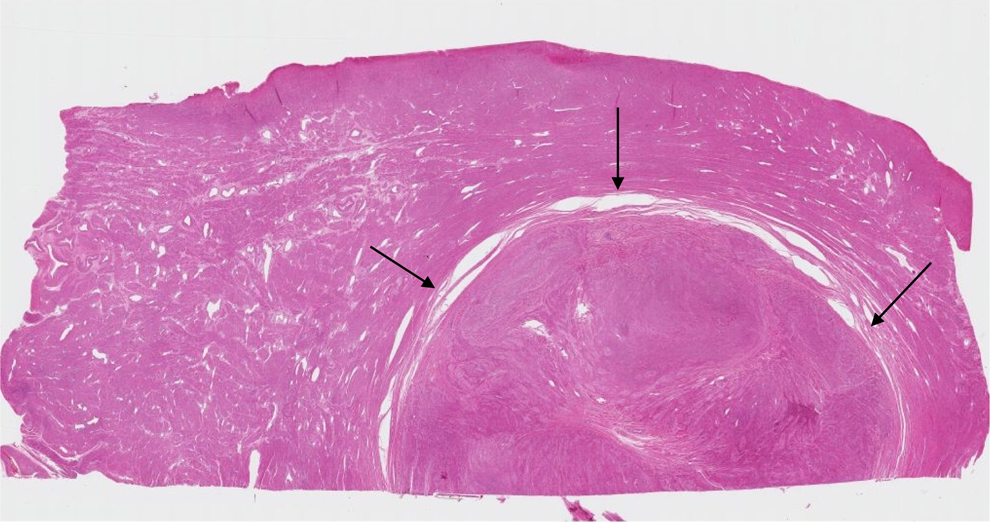
The borders are smooth and “pushing” (not infiltrating into the surrounding myometrium).
What information does this give you about the nature of the tumor?
This gross feature favors that the tumor is benign.
Compare an area from within the tumor (Figure 3) at higher power with the surrounding normal myometrium (Figure 4), viewed at the same magnification
Uterine tumor (hematoxylin and eosin stain; original magnification 100×). Normal myometrium (hematoxylin and eosin stain; original magnification 100×).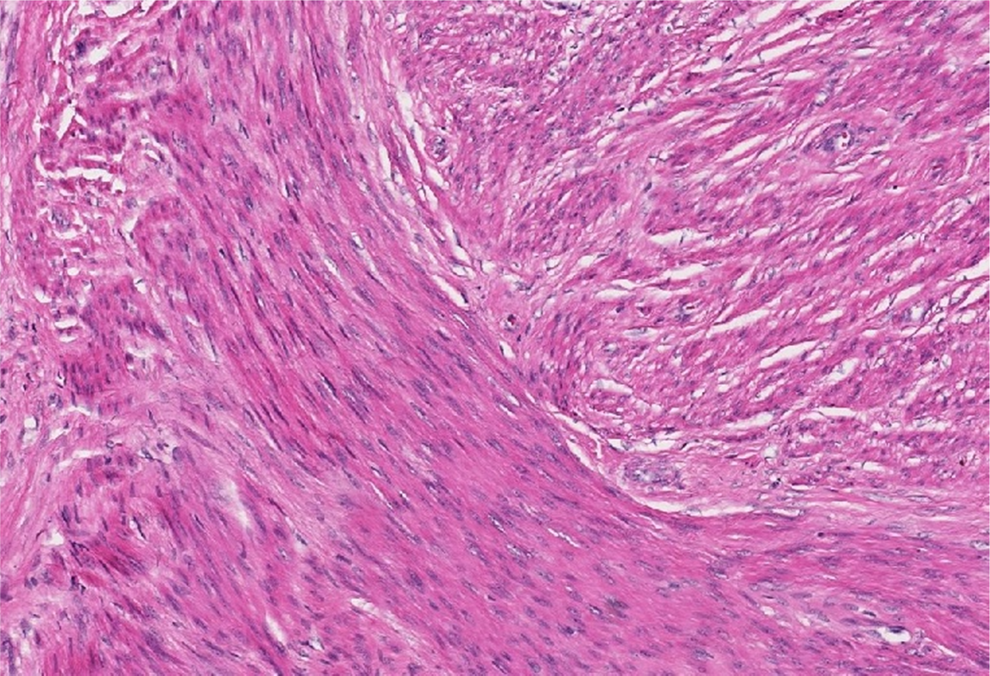
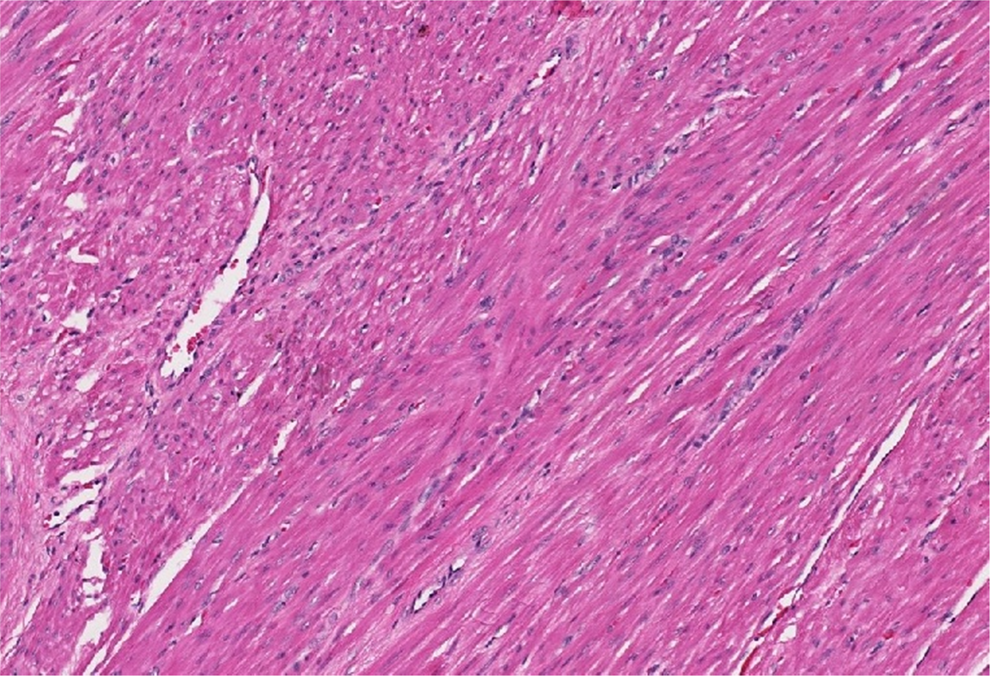
Comparing the tumor cells in Figure 3 with normal myometrial smooth muscle cells in Figure 4, would you be able to distinguish which image is from the tumor and which is from normal myometrium without the labels?
Distinguishing these 2 areas is very difficult. While the tumor may be a bit more cellular, this is a subtle change that only experienced pathologists might recognize. The point to be emphasized is that it is the presence of a mass, and not cytologic appearance, which allows one to recognize this lesion as a tumor.
Describe the cells of the tumor in more detail, utilizing the following criteria (and comparing these features to the normal myometrial cells). Nuclear size: Same as normal
Nuclear:Cytoplasmic (N:C) ratio: Same as normal
Shape of nuclei (regular vs pleomorphic [variation in size and shape]): regular elongated oval shape
Nuclear chromatin staining (normochromatic versus hyperchromatic [increased staining on hematoxylin stain]): Normochromatic
Prominent nucleoli? No
Do you see areas of necrosis? No
Is it easy to identify mitotic figures? No; Abnormal mitoses? No
Therefore, what term would you use to describe the histological appearance of the cells in this tumor?
Well-differentiated.
Note: Well-differentiated is a term applied to the histological appearance of tumor cells. It means that the cells closely resemble their normal counterparts. The tumor cells in this case so closely resemble the normal myometrial cells that is difficult at high power to conclude that one is looking at a neoplasm (see Figure 3 vs Figure 4). Benign tumors are typically well-differentiated. Malignant neoplasms may be well-differentiated but more often will show a range of decreasing differentiation that may progress to anaplasia (lack of differentiation). The histological features that are associated with decreased differentiation include increased nuclear-to-cytoplasmic ratio, pleomorphism of the nuclei and cells, hyperchromatism, and prominent nucleoli—none of which were observed in this case. Additional features suggestive of malignancy are increased mitotic activity (particularly in tissue that is not normally mitotically active), including abnormal mitotic figures, and the presence of necrosis (both grossly and/or microscopically), which were also not observed.
What is your pathological diagnosis?
Leiomyoma of the uterus (A benign tumor: leiomyo = smooth muscle; oma = benign neoplasm)
By your terminology above, you have identified the tumor as either benign or malignant.
Summarize the gross and microscopic morphological features in this case that support your classification.
Growth pattern: Expansile, pushing, noninvasive growth
Microscopic: Well-differentiated; regular nuclear size and shape and normochromatic; absent or rare mitoses (less than 5 mitoses/10 high-power fields); absence of necrosis.
Note: The classification of this tumor as benign implies absence of invasive local growth and inability to metastasize (discontinuous spread to distant sites). Nonetheless, benign neoplasms may be problematic and even fatal to the host due to growth in a sensitive location (eg, in the meninges or cardiac left atrium), other local effects (eg, ulceration in a hollow viscus), and secretion of indigenous or inappropriate hormones (ie, hormones that are normally not elaborated by the normal cellular counterpart of the tumor, resulting in a paraneoplastic syndrome). 1–2
What is the natural history of this tumor?
Leiomyomas are common benign neoplasms of the uterus. Leiomyomas show expansile growth in the uterus. On cut section, they show a white, whorled appearance that gave rise to their colloquial term, fibroid. Ultrasonography is the standard diagnostic test. They generally show growth during reproductive years and regression in menopause. They may be asymptomatic but, depending on size, location, and number, may present with abnormal bleeding, urinary symptoms from compression of the bladder or rectum, pelvic pain, and interference with fertility and maintenance of pregnancy. Symptomatic leiomyomas may be treated surgically with hysterectomy or in a woman desiring pregnancy by myomectomy. Medical therapy includes hormonal therapy, uterine artery embolization, and radiofrequency ablation.
The malignant counterpart of leiomyoma is leiomyosarcoma (leiomyo = smooth muscle; sarcoma = malignant mesenchymal neoplasm). The histological appearance of leiomyosarcomas ranges from well-differentiated tumors that show increased numbers of mitotic figures to highly anaplastic tumors with areas of necrosis. These tumors show progressive invasive growth and metastasis. Leiomyosarcomas are believed to arise de novo from the myometrial cells. Leiomyomas are generally NOT considered to be premalignant, so most asymptomatic leiomyomas do not need be excised. 3–4
Teaching Points
Leiomyoma is a common benign neoplasm of the uterus.
While frequently asymptomatic, leiomyomas may present with symptoms due to local expansion and compression within the uterus and/or into adjacent pelvic structures.
Uterine leiomyomas are not considered to be premalignant.
Benign neoplasms are characterized by expansile, smooth, and noninvasive borders.
Histologically, benign neoplasms are well-differentiated, with regular cells and nuclei, rare mitoses, and absence of necrosis.
Footnotes
Declaration of Conflicting Interests
The author declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author received no financial support for the research, authorship, and/or publication of this article.
