Abstract
A shortage of physicians in the United States has been long projected. Because of predictions of retirement among the aging pathology workforce, there is an anticipated shortage of pathologist as well. To address the pathology workforce shortage among pathologists, the Association of Pathology Chairs assembled a subcommittee of the Association of Pathology Chairs Advocacy Committee to explore ways to identify the strengths, weaknesses, opportunities, and threats to the pathology workforce. One opportunity to encourage strong candidates to pursue pathology as a career is to explore possibility to revisit advanced credit for the post-sophomore fellowship. A survey that was designed to understand the post-sophomore fellowship training better was distributed on the listserv of the Program Directors Section of the Association of Pathology Chairs. A review of the literature on post-sophomore fellowship programs is presented in light of the findings from this survey. Many post-sophomore fellowship programs are run similar to a first-year resident experience, although programs show great diversity in curriculum, including some programs that focus on research. Post-sophomore fellowships attract medical students to the area of pathology and tend to end up in academic and research positions. A second survey of program directors served as an opinion poll of challenging issues that affect residency training. From the second opinion poll, most program directors feel that residents can use additional training to improve the outcome of our future pathologists.
Keywords
Introduction
Concern over the pathology workforce has been discussed and researched for over a quarter of a century, and the Association of Pathology Chairs (APC) has been involved in identification of various factors that have contributed to a decline in the number of US medical graduates choosing pathology as a career. 1 Continued interest over the pathology workforce shortage was highlighted by Alexander 2 who reviewed trends in the decrease in pathology residency training programs and the decrease in the total number of pathology resident positions, along with curricular changes in pathology graduate medical education (GME), and discussed the evolving roles of the pathologist of the future. In December 2013, the College of American Pathologists convened a Pathology Workforce Summit in Washington, DC, which resulted in 6 propositions and 3 recommendations. 3 Recommendation 2 charged organized pathology to “develop a plan to attract and recruit qualified medical students and science, technology, engineering, and mathematics (STEM) students to pathology and laboratory professions.” The APC and the APC Advocacy Committee responded to the call with the formation of the Pipeline Subcommittee at the July 2014 APC/Program Directors Section (PRODS) meeting in Boston, Massachusetts. Among many areas of concern, one focus of the Pipeline Subcommittee was to revisit advanced credit for pathology post-sophomore fellowships (PSFs) as a mechanism of recruiting outstanding US medical students to pathology.
Methods
A survey on PSF was conducted using SurveyMonkey on the Program Directors Section (PRODS) listserv from March 17, 2015, to March 30, 2015 (Appendix A). A total of 48 programs responded, representing a 33.8% response rate. Of these responses, 28 programs that did not have a PSF could answer the first 7 questions of the survey, which focused on the program directors’ experience with PSF graduates who were in or graduated from their residency program, and then they exited the survey. The low response rate somewhat limits the accuracy of the results discussed below. Twenty program directors who have a PSF in their institution responded to the survey. This number correlates with the number of PSF programs that are registered with Intersociety Council for Pathology Information, and the high response rate for PSF programs therefore provides reliable results. Two responded that they used to have a PSF program but no longer have one. Program directors who have a PSF in their institution were able to proceed with questions 8 through 26. The results are discussed below. A second survey was sent to program directors using SurveyMonkey on the PRODS listserv from April 6, 2015, to April 30, 2015, and received 70 responses, or a 49.3% response rate (Appendix B). This second survey was an opinion poll of program directors designed to identify challenging issues in GME in pathology.
Results From the PRODS Survey on Post-Sophomore Fellowships
The average size of a graduating allopathic medical school class in the United States is 145.2 students. The range in size of the senior graduating class varied considerably from an inaugural class of a new medical school at 29 up to 270 students. The average number of students going into pathology in the senior class was 2.8 (1.9%), with a range of 1 to 10 students. The percentage of seniors going into pathology at the smallest medical school was 1 (3.4%) of 29 seniors, whereas the percentage going into pathology at the largest school was 10 (5.9%) of 270 seniors.
It was estimated that 59.8% of PSF-trained residents pursued an academic career. When asked whether PSF-trained residents had changed specialty during or after residency or had left medicine altogether, 4 (8.3%) programs directors responded that the PSF-trained resident had changed from pathology to another specialty or left medicine altogether, 29 (60.4%) that they had remained in pathology, and 15 (31.3%) that they did not know.
The majority of PSF chose to do a combined anatomic and clinical pathology (AP/CP) residency. The number of PSF who chose to do anatomic pathology (AP) only was a distant second. Only one PSF chose to do a clinical pathology (CP)-only residency. No PSF chose to do combined anatomic pathology/neuropathology training. Many of the PSF-trained residents went on to do fellowship training after residency.
Program directors were asked to compare the performance of PSF-trained residents with the performance of non-PSF-trained residents. Post-sophomore fellowship-trained residents were more likely to receive better performance ratings than non-PSF-trained residents in the areas of patient care/procedural skills and in medical knowledge competencies. Post-sophomore fellowship-trained residents were more likely to receive about the same performance ratings or were evenly split with better performance and about the same performance in the competencies of practice-based learning and improvement, interpersonal and communication skills, professionalism, and systems-based practice. First-time board pass rate for PSF-trained residents favored about the same performance over better performance by a small margin when compared with non-PSF-trained residents. None of the program directors responded that their PSF-trained residents performed worse than non-PSF-trained residents (Figure 1).
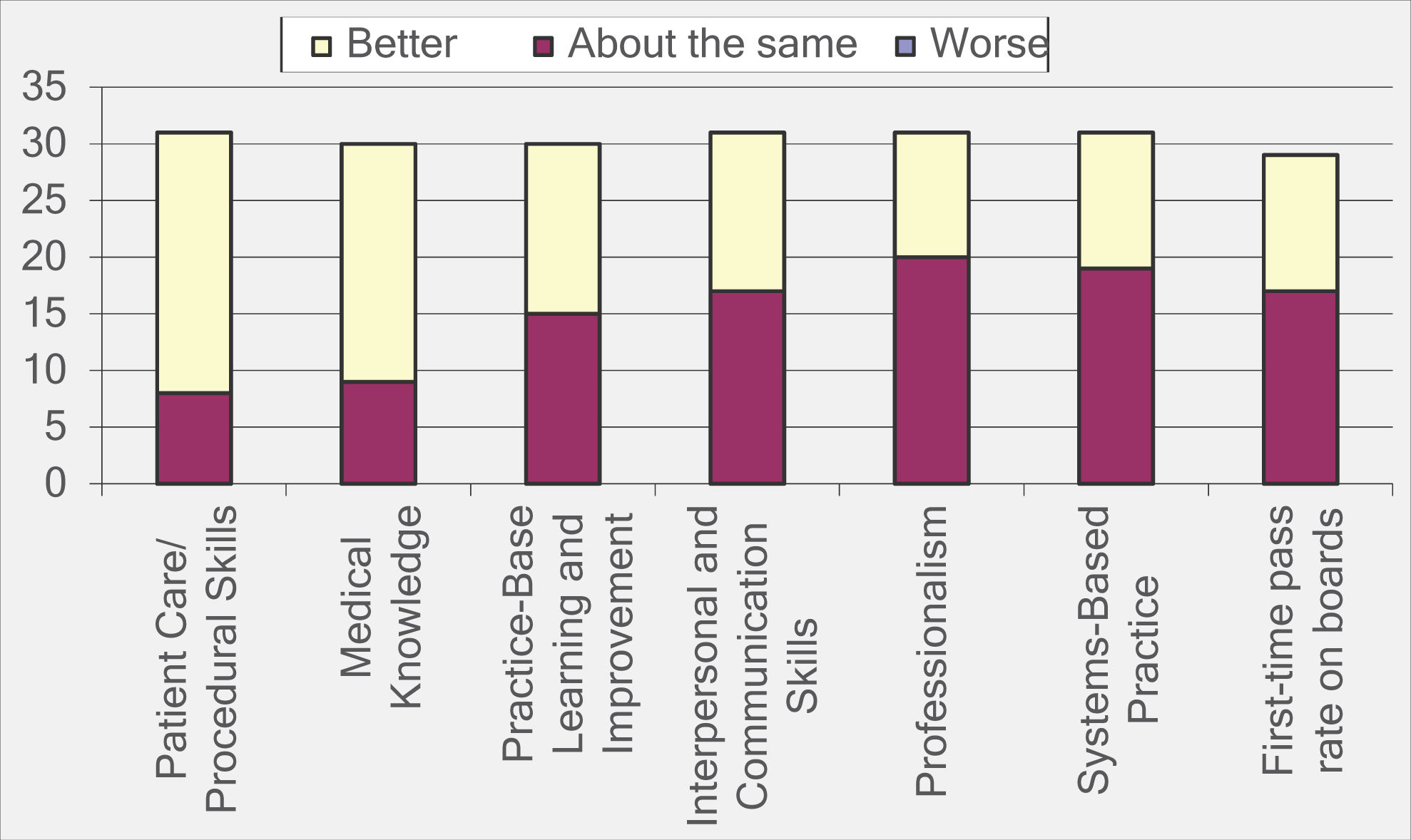
Comparison of performance by post-sophomore fellowship (PSF)-trained residents versus non-PSF-trained residents.
Of the 20 programs that offer a PSF, 7 (35%) have the pathology residency program director serve as the PSF director. In 3 (15%) programs, the undergraduate medical education director is the PSF director. Half of PSF program directors are pathology faculty members other than the residency program director or the undergraduate medical education director (10 programs, 50%). None of the PSF programs reported as having a department chair as PSF director.
Post-sophomore fellowships have been in existence for a long time. Four programs were started within the last 5 years. Four programs reported 6 to 10 years, 5 programs reported 11 to 20 years, 5 programs reported 21 to 50 years, and 2 programs have been in existence for more than 50 years. The average number of PSF graduates is 45.7 students, with a range of 3 to 180. However, the average number of PSF graduates who went on to do a pathology residency was 21.8 (47.7%), with a range of 1 to 105. Of those who trained in a PSF program, an average of 9.9 (21.7%) stayed on at the same institution for pathology residency training, with a range of 0 to 20.
At least 2 respondents in the current survey stated that they used to have a PSF program but discontinued due to funding or do not offer it every year, due to the applicant pool and budgets. During a separate Pipeline Subcommittee survey sent to the APC, PRODS, and Undergraduate Medical Education Directors Section listserv (Pipeline Subcommittee Survey #1, September 15, 2014 to October 12, 2014), additional information about PSF programs about funding was obtained. Of 19 programs that responded, 15 (78.9%) paid the PSF a stipend, 3 (15.8%) programs do not pay a stipend, and 1 (5.3%) program did not respond. The range of stipend was from US$16 000 to US$32 000, with a mode of US$20 000. Some programs responded that it was the same stipend paid to graduate students. The department of pathology was the sole source of funding at 12 (63.2%) programs. Two (10.5%) programs received funding from the department and the medical school. One program funded the PSF from the department and private practice income, 1 program from the medical school, 1 program from private practice, 1 program funded the PSF through an endowment, and 1 program received funds through a combination of Federal Work Study, medical school, and the department plus an external annual gift. None of the PSF programs charged tuition.
Program directors were asked who was responsible for direct supervision of the PSF and were asked to check all that applied. The attending staff pathologist was responsible at all 20 programs (100%), the senior resident (Postgraduate Year [PGY]3 or PGY4) and pathologists’ assistant (PA) at 19 programs (95%), the junior resident (PGY1 or PGY2) at 14 programs (70%), and the fellow at 13 programs (65%).
Program directors were asked whether there was a point in training where the PSF could be placed on “indirect supervision” as defined by Accreditation Council on Graduate Medical Education (ACGME) Common Program Requirement VI.D.3.b, 4 where direct supervision by an attending staff, fellow, resident, or PA is immediately available either in person or by telephonic means. Fourteen (70%) programs responded that they did advance the PSF to indirect supervision, whereas 6 (30%) programs did not.
Three (15%) programs had separate or dedicated learning goals and objectives for the PSF, 16 (80%) programs used the same learning goals and objectives that are used for the residents, and only 1 (5%) program had no formal learning goals and objectives for the PSF. Two (10%) programs responded that their PSF learning goals and objectives were both competency based and robust, whereas 2 (10%) programs responded that their PSF learning goals and objectives were neither competency based nor robust. Sixteen programs did not respond to that question.
Program directors were asked how the learning goals and objectives differed between PSFs and the learning goals and objectives of resident rotations. Responses included that they wanted the PSF to gain an understanding of the role of the pathologist in patient care, and thus, the goals and objectives were the same as for certain PGY1 resident rotations but that more PA assistance was provided to the PSF and there were fewer service months so the PSF could do research. Another response was that the learning goals and objectives were less detailed due to the shortened experience.
Evaluation tools for assessing the performance of PSFs were variable. Seven (35%) programs reported the use of a separate dedicated performance evaluation form for the PSF. Nine (45%) used the same evaluation forms as for the residents. Three (15%) programs replied “other,” which included using the same forms used for residents as well as using a separate dedicated form with a summary letter for dean and residency (no matter what specialty the PSF was applying to) if requested; and this form was often used in the dean’s letter. One program provided group feedback write-ups at 6- and 12-month intervals. One program replied that the PSFs are considered enrolled medical students and therefore used the evaluation forms used by the medical school. One (5%) program stated that the PSF does not receive any type of formal evaluation.
In terms of the composition of the PSF curriculum, AP had the majority of weeks at 36.15 weeks, compared to 16.85 weeks for CP. The top 5 rotations in AP were surgical pathology (14.65 weeks), subspecialty surgical pathology (6.65 weeks), autopsy pathology (6.15 weeks), cytopathology (2.62 weeks), and molecular pathology (2.07 weeks) (Figure 2). The top 5 rotations in CP were research (9.35 weeks), hematology (4.59 weeks), blood banking/transfusion medicine (2.86 weeks), microbiology (2.69 weeks), and molecular pathology (2.11 weeks) (Figure 3).
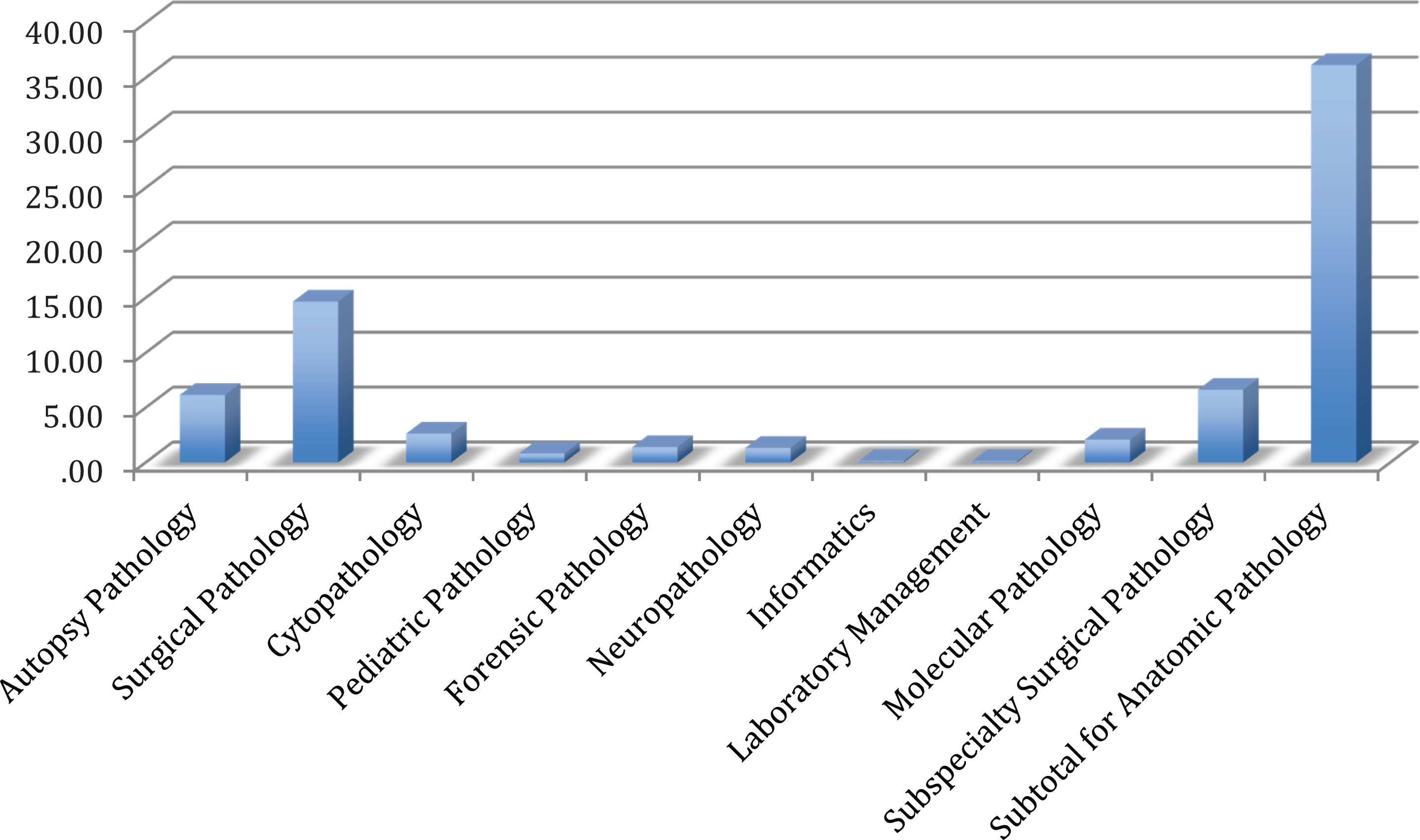
Distribution of the number of weeks in subspecialty pathology areas within anatomic pathology at post-sophomore fellowship (PSF) programs.
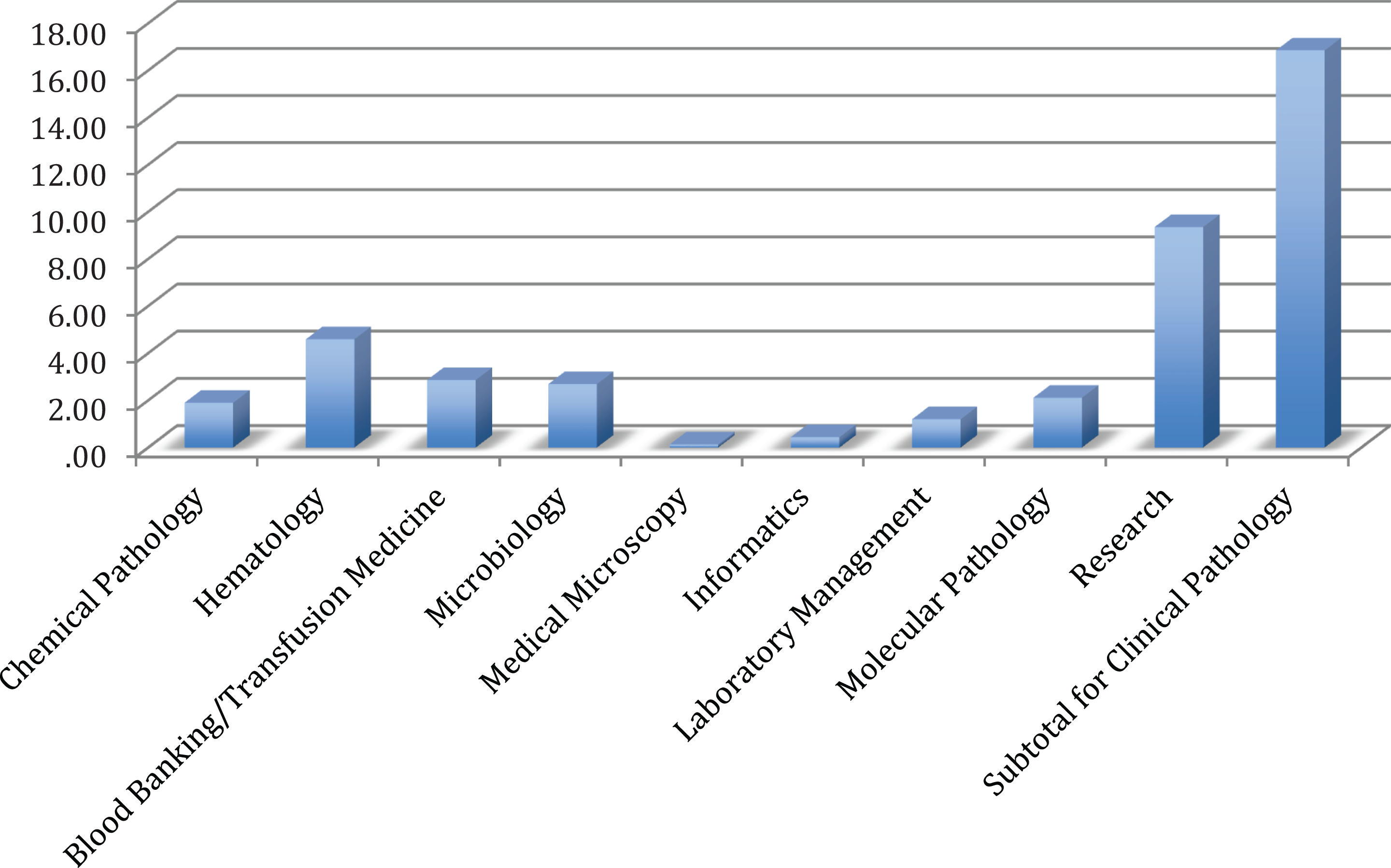
Distribution of the number of weeks in subspecialty pathology areas within clinical pathology at post-sophomore fellowship (PSF) programs.
For evaluating the quality and efficacy of PSF programs, 13 (65%) programs do an annual program evaluation, similar to that done for residency and fellowship programs. The PSF completes an evaluation on each rotation at 12 (60%) of the programs. Eight (40%) programs have the PSF complete a teaching evaluation. Five (25%) programs have no regular evaluation process for the PSF program.
All 20 programs have the PSF involved in performing autopsies. Eleven (55%) programs allow the PSF to share the autopsy with the residents. Nine (45%) programs have the PSF perform the autopsy without sharing with residents. Nineteen (95%) programs stated that their PSF participates in all components of the autopsy as defined by the ACGME Program Requirement IV.A.5.a).(4), 4 whereas only 1 (5%) program does not require their PSF to participate in all components of the autopsy.
All 20 programs have the PSF involved in surgical pathology from the gross bench to sign-outs. Program directors were asked whether the PSF takes ownership over the case like a PGY1 pathology resident (including microscopic sign-outs, synoptic reporting, cancer staging, histochemical and immunohistochemical stains, and molecular testing). Eighteen (90%) programs stated that they do allow their PSF to take ownership over the case like a first-year resident would, whereas 2 (10%) programs stated that they do not allow the PSF to take that degree of responsibility on surgical pathology cases.
Program directors were asked whether they feel that students completing a PSF should receive advanced standing toward American Board of Pathology (ABP) qualification. Thirteen (65%) program directors were in favor of reinstating some advanced standing for graduates of PSF. The response of 3 (15%) programs was neutral and 4 (20%) programs were opposed. Most of the arguments in favor of advanced standing cited that their PSF program was essentially the same training that a PGY1 resident would receive. Some cited that “the PSF graduates are usually miles ahead of the average medical student going into pathology and they always perform better at the beginning of residency.” The neutral comments were cautionary, suggesting that advanced credit should not be used to entice students to go into pathology, and giving advanced standing to the PSF may have a negative impact on developing camaraderie within their residency class. Furthermore, stepping back into medical school is not the same as being a resident with uninterrupted training. Another response noted that the PSF training has been less intense in the past years, and some PSFs are less than a year in length. Those who were opposed felt that the PSF required the same length of experience in surgical pathology as their non-PSF peers. Some PSFs are heavily supervised without the autonomy that residents experience, and some PSFs have taken on more of a research role. Another felt that advanced standing should not be given unless AP/CP residency returned to a 5-year curriculum.
When asked what agency should “accredit” the PSF programs, 13 (65%) of responses were that ACGME should oversee accreditation, 2 (10%) felt that the Liaison Committee on Medical Education (LCME) who accredit allopathic medical schools should be responsible for accreditation, and 5 (25%) stated other. Among the responses under other, 2 respondents were uncertain if PSF programs should be accredited, 2 felt that they should not be accredited, and 1 felt the ABP should accredit the PSF programs.
Results From the PRODS Opinion Poll on Graduate Medical Education Issues
The discussion concerning PSF has taken place in the context of the broader range of issues raised by the Workforce Summit of 2013. 3 For what sort of career are pathology trainees being prepared? Is the current curriculum appropriate for that future? Is the training itself a deterrent to medical students choosing a specialty; and, if so, can it be modified to be more appealing without diminishing its value?
Program directors were asked if, in general, they considered most AP/CP residents adequately prepared to enter practice after 4 years of training without further fellowship training. Opinion was strongly divided, and only 18% of respondents were neutral. The most common response was “disagree” (41%), and the second most common was “agree” at 31%. “Strongly disagree” and “disagree” combined were 47%, compared to 38% combined for “strongly agree and agree.” Program directors, however, tended to have a much more favorable opinion of their own graduates. When asked the same question about the respondent’s training program, 13% strongly agreed, 54% agreed, only 21% disagreed, and none strongly disagreed.
Program directors were also somewhat split on the topic of the importance of achieving competency in performing autopsies during residency training. Half of the respondents felt that competency in performing autopsies remains an essential goal for general residency program. However, 11% strongly agreed and 24% agreed that autopsy was no longer an essential goal for general pathologists because of changes in the scope of practice of most pathologists. When asked if the respondent’s program could competently train their residents without adhering to the numerical minimum requirement of 50 cases set by the ABP and the ACGME, 17% strongly agreed and 46% agreed, whereas only 11% disagreed and 3% strongly disagreed.
Most programs have either implemented or have the flexibility to implement training in the emerging/increasing areas of need, such as molecular pathology, clinical informatics, quality improvement, and health-care team-based practice, with 24% in strong agreement and 53% in agreement with the statement. Many of the survey participants also felt that their residents can acquire the skills necessary to manage a laboratory by the completion of residency, with 11% in strong agreement and 46% in agreement. This remains an issue for some programs, however, inasmuch as 23% disagreed and 3% strongly disagreed.
The vast majority agreed that graduated responsibility to the level of oversight supervision, defined by the ACGME as review with feedback by the attending after care is delivered, should be included within residency training in order to produce graduates who are fully prepared for practice: 61% strongly agreed and 31% agreed (total 92%), whereas only 3% were neutral, 4% disagreed, and none strongly disagreed. However, when asked if the respondent could readily implement graduated responsibility to the level of oversight supervision at their program, 20% strongly agreed, 49% agreed, 14% disagreed, and 4% strongly disagreed.
There was no consensus on whether the increased years of training to 5 to 6 years including fellowship was one of the most important deterrents to medical students choosing pathology as a career. A perfect bell-shaped distribution of answers resulted: 6% strongly agreed, 24% agreed, 37% were neutral, 26% disagreed, and 7% strongly disagreed. However, it was almost unanimous among respondents that their residents appear to feel that they need fellowship training in order to practice pathology with competence, whether the need for the fellowship training is real or not. Forty-five percent strongly agreed, 46% agreed (combined 91%), 6% were neutral, and only 3% disagreed. None strongly disagreed. In a related question, where respondents were asked if residents felt that fellowship training was needed to be employable, whether the need for fellowship training is real or not, the consensus was even greater: 74% strongly agreed and 23% agreed (combined 97%); only 1% strongly disagreed.
When asked their impression of what most employers felt about graduating residents needing at least 1 additional year of fellowship training after residency in order to practice pathology with competence, 44% strongly agreed and 41% agreed, whereas only 9% were neutral, 3% disagreed, and 3% strongly disagreed. Respondents also felt that most employers appear to be of the opinion that residents need an additional year of fellowship to fill a subspecialty focus for employability: 40% strongly agreed, 49% agreed, 7% were neutral, 1% disagreed, and 3% strongly disagreed. Most respondents also had the impression that employers seek the most highly trained applicants for employment mainly because such highly trained applicants are so plentiful in the marketplace, regardless of whether additional fellowship training is actually necessary in order to competently practice pathology: 23% strongly agreed, 49% agreed, 17% were neutral, 11% disagreed, and none strongly disagreed.
Given the option of taking a job over a second fellowship, most program directors agreed that residents would take the job; 54% strongly agreed and 43% agreed (combined 97%) and only 3% disagreed. However, given the option of taking a job over a first fellowship, the responses were more widely distributed; only 12% agreed, 36% agreed, 26% were neutral, 23% disagreed, and 3% strongly disagreed. Thus, it is the view of most program directors that a projected trend toward more plentiful jobs may reduce the number of second fellowships done by residency graduates, but there is less clarity among program directors on the effect such a trend might have on first fellowships.
Although shortening residency training might make entering pathology a more attractive option for medical students, this raises questions about the speed with which residents can explore options for choosing a subspecialty interest. Program directors disagreed on whether most residents already know that they are interested in either AP or CP upon entering residency. Six percent strongly agreed that most resident know, 33% agreed, 20% were neutral, 34% disagreed, and 7% strongly disagreed. When asked if the structure of the respondents’ curriculum can adequately expose residents to both AP and CP within the first 18 months of training to enable them to decide upon a subspecialty for the remainder of residency, or if it could easily be revised to do so, 17% strongly agreed, 30% agreed, 24% were neutral, 20% disagreed, and 9% strongly disagreed. The answers to both of these questions may reflect the existing diversity among pathology residency programs and the residents each program attracts because of its specific characteristics. A majority of respondents disagreed with the idea that a 12- to 18-month core curriculum in combined AP and CP would be sufficient experience to provide most residents fundamental training to proceed into more focused subspecialty training in their residency curriculum: 6% strongly agreed, 26% agreed, 14% were neutral, 46% disagreed, and 9% strongly disagreed. Program directors also disagreed that residents would have sufficient exposure by the end of the first half of their PGY2 year to decide what fellowship to apply to: 60% disagreed and 19% strongly disagreed (combined 79%). Only 1% strongly agreed and 11% agreed. Similarly, the majority of program directors felt that by the end of their second year in residency, residents have not developed sufficient subspecialty focus to choose and begin a subspecialized track, if such a track existed: 63% disagreed and 13% strongly disagreed (combined 76%), with only 4% strongly agreed and 10% agreed.
Programs currently appear to differ with respect to the degree of flexibility that they are able to offer their residents who might seek early subspecialization with their residency curriculum. When asked if residents at the respondents’ programs are free to switch from AP/CP to an AP-only or CP-only track as they begin their second year of training, 21% strongly agreed, 30% agreed, and 9% were neutral; however, 20% disagreed and 20% strongly disagreed. These numbers were very similar to those seen when program directors were asked if the service needs of the institution would be adversely impacted if residents could freely choose AP-only or CP-only tracks after the first 12 to 18 months of residency; 14% strongly agreed, 26% agreed, 27% were neutral, 19% disagreed, and 14% strongly disagreed. This suggests that a movement toward early subspecialization within the residency curriculum might create difficulties for some programs’ ability to cover service responsibilities.
Program directors were asked if sustained competency in both AP and CP was unrealistic and if certification should be given in AP only and CP only; 7% strongly agreed, 21% agreed, 21% were neutral, 34% disagreed, and 16% strongly disagreed. This was mirrored by the response to the question proposing that focused AP or CP training is better preparation for the immediate job market than combined AP/CP training. In contrast to the strong belief that employers favor applicants with subspecialty training, 43% disagreed and 14% strongly disagreed (combined 54%) that focused AP or CP training is better preparation for the job market, whereas 4% strongly agreed, 20% agreed, and 19% were neutral. Similarly, most program directors were in agreement that most graduates should initially certify and maintain certification in both AP and CP for the current and potential future job requirements; 29% strongly agreed, 40% agreed (combined 69%), 17% were neutral, 11% disagreed, and 3% strongly disagreed.
There was a broad range of responses to the proposition that physician scientists’ jobs require less AP or CP expertise than other pathology physician jobs: 6% strongly agreed, 33% agreed, 23% were neutral, 30% disagreed, and 9% strongly disagreed. Whether this might translate into different requirements for physician–scientist trainees or should be reflected in a different sort of certification was not addressed.
Program directors tended to disagree with exempting residents with appropriate prior experience from certain core curriculum; 49% disagreed and 14% strongly disagreed (63% combined), 6% strongly agreed, 20% agreed, and 11% were neutral. When asked if exempting residents with previous experience would adversely impact the service needs of the institution (eg, in surgical pathology, hematology, transfusion medicine, etc), 19% strongly agreed, 44% agreed, 15% were neutral, 18% disagreed, and 4% strongly disagreed. As with early subspecialization, advance credit appears to have implications for service coverage by residency programs, a fact that would need to be considered by any initiative in that direction.
Program directors also disagreed with the concept that medical student electives in pathology could easily be made to be equivalent to first-year residency experiences; 50% disagreed, 19% strongly disagreed (combined 69%), 16% were neutral, only 3% strongly agreed, and 13% agreed. This result presumably stems from the curriculum and responsibilities offered to medical students during short elective periods. However, the results from the program directors were strikingly different when asked if post-sophomore pathology fellows could function and learn at the level of a first-year (or higher) pathology resident; 24% strongly agreed, 44% agreed (68% combined), 21% were neutral, 9% disagreed, and 1% strongly disagreed. Program directors were more in favor of awarding advanced credit toward board eligibility for a graduate of a 1-year post-sophomore pathology fellowship program if it were overseen by a director of an ACGME-accredited pathology residency, where the PSF functioned as a first-year resident; 34% strongly agreed, 26% agreed (60% combined), 29% were neutral, 10% disagreed, and only 1% strongly disagreed.
Discussion
The pathology post-sophomore fellowship (PSF) is not a recent concept. The first PSF was developed by Dr George H. Whipple in 1926, when he was dean at the University of Rochester School of Medicine. 5 In Fenninger’s study, graduates of their PSF were 2.5 times more likely to pursue an academic career compared with other graduates. In a study by Longo et al, 36% of PSF graduates of the University of Missouri–Columbia School of Medicine chose pathology as a career, compared to 4% of all Missouri graduates or nationally. Also, 80% of PSF graduates pursued an academic career, which was much higher than those who had not had PSF training at their program. 6 Over a 35-year period at the University of California at Los Angeles (UCLA), Dodd et al reported 19.3% of 140 PSFs chose pathology, which was 9.3 times the percentage of their non-PSF students choosing pathology as a career. 7 A more recent publication by MacPherson studied a 47-year period at the University of Vermont, where 31% of 101 PSFs chose pathology, compared to 2.9% of their non-PSF students choosing pathology. 8 The most recent study by Summers et al was from an abstract presented at the 2012 United States and Canadian Academy of Pathology (USCAP) meeting, which discussed a national survey of 129 residency programs, of which 81 program directors responded. 9 Of those who responded, 17 (21%) offered a PSF. Only 9 of these programs had statistics on their graduates; an average of 37% of PSF graduates chose pathology as a career. The current study suggests that approximately 60% of PSFs choose pathology as a career. Commonly cited advantages for offering a PSF program are that it offers an in depth exposure to pathology (76%), it enhances general medical knowledge (59%), and it serves as a potential recruiting tool to pathology (35%).
Commonly cited disadvantages to the PSF were the additional year of training for the medical student (41%), which was also noted by Longo et al, 6 and the expense for the department (35%). In 2005, a survey of the APC Undergraduate Medical Education Committee identified 39 PSF programs. 8 In our current survey, 20 PSF programs responded; thus, the number of PSF programs has decreased over time.
In terms of accreditation of PSF programs, it is unlikely that the ACGME would accredit such programs, as they are not GME programs. It is equally unlikely that the LCME would accredit the PSF, as it accredits allopathic medical schools as a whole and not just one small aspect of the curriculum. The ABP certifies individuals, and it is not involved in accreditation of programs. Although the ACGME and ABP are not likely candidates to accredit PSF programs, the Pipeline Subcommittee is currently working on a White Paper proposal to the ACGME and ABP to seek a mechanism whereby PSF may receive some recognition for their year of pathology-specific training. Although it is not likely that the ABP would recognize advanced credit of training that is not part of an ACGME-accredited program, the APC has offered to assume the role of accrediting body for PSF programs. As noted in the current survey, the curriculum and level of teaching vary from program to program. So that more uniform training can be achieved, the Pipeline Subcommittee is also working on “program requirements” for the PSF programs. As with a beginning PGY1, a PSF requires appropriate supervision by a qualified practitioner, such as a PA, a pathology resident, a subspecialty pathology fellow, or an attending staff pathologist. Program requirements will provide structure to the curriculum and expected entrustable professional activities for the PSF to learn. Many of the lower level Pathology Milestones would be applicable to the PSF. Accountability through program requirements and an accreditation process will help ensure a uniform outcome of training the PSF. If the APC is allowed to accredit PSF training programs and that in turn is acceptable to the ABP to allow for advanced standing of the PSF, it will be necessary to monitor outcome measures. It would be reasonable to assess the progress of the PSF-trained resident’s progress during training using a common tool, such as the Pathology Milestones. That can in turn be corroborated with the pathology residency training program’s assessment of the PSF at the first semiannual performance evaluation and Pathology Milestones assessment. Systematic evaluation of the PSF-trained residents’ American Society for Clinical Pathology (ASCP) Resident In-Service Examination (RISE) First and subsequent ASCP RISE as well as first-time primary certification examination pass rate and portfolio can all serve as metrics to assess the impact of changes in the PSF training programs. This would need to be contrasted with the control group of a representative sample of pathology residents who are not PSF trained prior to residency.
MacPherson closed his article in 2005 stating the following: “Although the Board’s decision is understandable in the context of requiring only 4 rather than 5 years of postgraduate training, ignoring the student fellowship experience completely is unreasonable in this era of competency-based residency training. I would propose that the Board continue to require program directors to register their student fellowship programs, submit accurate program descriptions, provide appropriate supervision of the program, preferably by the director of the residency program, and compile data concerning the outcome of graduates from these student fellowship programs. In return, I propose that the student fellows receive partial or limited credit for their experience (e.g., credit for their autopsy experience), which would permit them to increase the flexibility (i.e., electives) of their 4-year residency program. Naturally, any credit for these activities would be awarded at the discretion of the program director.” 8(p1171)
It is the hope of the Pipeline Subcommittee of the APC Advocacy Committee that the ABP will give strong consideration to provide some advanced standing for competency-based education and training that is spent in the PSF year. Based upon the opinion poll survey discussed above, the majority of program directors are in favor of some form of advanced credit for the PSF.
Footnotes
Appendix A. Post-Sophomore Fellowships in Pathology Survey
The topic of advanced standing credit toward pathology residency for post-sophomore fellowships (PSF) will be discussed at the May 2015 Cooperative Societies Meeting of the American Board of Pathology. In order to obtain a better understanding of the existing PSF and provide more accurate statistics for reinstating advanced standing credit for PSF, please complete the following survey.
All programs can answer question 1. 1. Please provide the average number of students at your school that match into pathology annually and the average total number of students in a graduating class (Your dean’s office should provide accurate numbers). Average number of students going into pathology annually: Average number of students graduating annually:
Questions 2 to 6 apply to residents at your training program that have had PSF experience during medical school (at your institution or at another institution). 2. How many of your PSF-trained residents pursued an academic career? (If you do not know the exact number, please provide an estimate) 3. Of your PSF-trained residents, do you know if any have changed specialty during or after residency or left medicine altogether? Yes No Don’t know 4. If you answered “yes” for question 3, how many? (If you do not know the exact number, please provide an estimate) Left pathology for another specialty: Left medicine altogether: 5. Of your PSF-trained residents, how many have done: AP/CP residency: Straight AP residency: Straight CP residency: AP/NP residency/fellowship: Did a fellowship after residency: 6. How does performance of the PSF-trained resident compare with your non-PSF trained residents in the following:
Anatomic pathology
Clinical pathology
Appendix B. PRODS Issues Related to GME in Pathology
The following is an opinion poll on issues relating to graduate medical education in pathology.
For each statement below, indicate one of the following:
Strongly Agree, Agree, Neutral, Disagree, and Strongly Disagree Most residents currently are not adequately prepared to enter practice after 4 years of AP/CP pathology residency without further fellowship training. My program has the capability to adequately prepare a resident to enter practice after 4 years of AP/CP pathology residency without further fellowship training. The evolution of pathology training into a 5- to 6-year experience (including fellowships) is one of the most important deterrents to medical students choosing a career in pathology. My program has implemented or has the flexibility to implement training in emerging/increasing areas of need (molecular pathology, clinical informatics, quality improvement, health-care team-based practice). Residents in my program’s curriculum can acquire the skills necessary to manage a laboratory by the time of their graduation from residency. Most residents feel that they need additional years of fellowship training after residency in order to practice pathology with competence (whether this need is real). Most residents feel that they need additional years of fellowship training after residency in order to be employable (whether or this need is real). Most graduating fellows would take a job in preference to a second fellowship, if an adequate employment position was available. Most graduating residents would take a job in preference to a first fellowship, if an adequate employment position was available. Most employers feel that graduating residents need at least 1 additional year of fellowship training after residency in order to practice pathology with competence. Most employers feel that graduating residents need at least 1 additional year of fellowship training after residency in order to supply a subspecialty focus necessary for employability. Most employers select the most highly trained applicants for employment chiefly because such highly trained applicants are so plentiful in the marketplace, regardless of whether the additional fellowship training is necessary in order to practice pathology with competence. A 12- to 18-month core curriculum in AP/CP would be sufficient to give residents fundamental training to progress into more focused subspecialty training in their residency curriculum. Most residents enter residency training already knowing whether they are interested in AP or CP. Most residents have had sufficient exposure to options in pathology to apply to fellowships by the first half of their PGY2 year. Most residents have developed sufficient subspecialty focus to choose and begin a subspecialized track within their residency curriculum by the first half of their PGY2 year. Sustained competency in both AP and CP is unrealistic; all certification should be AP only or CP only. Focused AP or CP training is better preparation for the immediate job market than combined AP/CP training. Most pathologists should initially certify and maintain certification in both AP and CP because of current and potential future job requirements. Physician–scientist jobs require less AP or CP expertise than other pathology physician jobs. The structure of my program’s curriculum can adequately expose a resident to both AP and CP within the first 18 months of training or could easily be revised to do so. Residents in my program are free to switch from AP/CP to an AP-only or CP-only track as they begin their second year of training. The service needs of my institution would be adversely impacted if residents could freely choose AP-only or CP-only tracks after the first 12 to 18 months of training. Residents should be exempted from basic service rotations by virtue of appropriate prior experience. The service needs of my department or institution probably would be adversely impacted if residents were exempted from basic service rotations by virtue of prior experience. Pathology residents should receive credit toward board eligibility for a post-sophomore pathology fellowship in which they functioned as a first-year resident. Pathology medical student electives at my institution are or could easily be made to be equivalent to residency experiences. Most post-sophomore pathology fellows could function and learn at the level of a first-year (or higher) pathology resident. Graduated responsibility to the level of oversight supervision (review with feedback by the attending sometime after care is delivered) should be included within residency training in order to produce graduates who are fully prepared for practice. My program currently has or could readily implement graduated responsibility to the level of oversight supervision.
Acknowledgments
The authors would like to acknowledge Ms Priscilla Markwood and Ms Jen Norman for their participation in organizing and creating the SurveyMonkey surveys and collating the raw data from the surveys and organizing conference calls for the Pipeline Subcommittee of the APC Advocacy Committee.
Authors’ Note
Members of the Pipeline Subcommittee of the APC Advocacy Committee include C. Bruce Alexander, Richard Conran, Ron Domen, Don Karcher, Peter Kragel, Wesley Y. Naritoku, Suzanne Z. Powell Michael B. Prystowsky, Jacob J. Steinberg, Charles Timmons, John Tomaszewski, Katie Warfield, H. James Williams and Nadeem Zafar.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
