Abstract
Background
Radical cystectomy (RC) with urinary diversion (UD) is associated with substantial morbidity. Enhanced recovery after surgery protocols, increased robotic usage, and improvements in urinary diversion have been evaluated for their effects on health-related Quality of Life (HRQoL), however, results are mixed. How psychosocial traits inherent to the patient influence HRQoL outcomes is unknown in this population.
Objective
This study aimed to evaluate resilience and its correlation with HRQoL in a cohort of patients undergoing RC for bladder cancer.
Methods
Patients with bladder cancer undergoing RC with UD at the University of Kansas Medical Center were screened for prospective enrollment in this clinical trial (NCT06337305). The validated Connor-Davidson Resilience Scale 25 (CD-RISC), the Functional Assessment of Cancer Therapy-Bladder-Cystectomy (FACT-BL-Cys), and the PROMIS 29-v2.0 were administered preoperatively, 2–3 weeks postoperatively, and at 90 days postoperatively. Patient demographics, pathology, and complication data were collected.
Results
Between November 2020 and August 2022, 52 patients completed the survey data. Patients were stratified based on baseline resilience score. The higher resilience group scored 85.7, 85.0, and 81.9 compared to 64.9, 70.4, and 72.0 at the three time points which all remained statistically significant. Participant resilience scores using the CD-RISC did not correlate with quality-of-life measures using the PROMIS or FACT-Bl-Cys at baseline or two weeks but did correlate at 90 days (p < 0.01). Resilience did not correlate with the patient's pathology stage or 90-day complication data.
Conclusions
Patients with higher baseline resilience maintain higher levels throughout the perioperative period and correlate with QOL.
Background
Muscle invasive bladder cancer (MIBC) is associated with significant morbidity and mortality inherent to the disease process and the definitive treatments. The gold standard treatment of MIBC remains neoadjuvant chemotherapy (NAC) followed by radical cystectomy (RC), bilateral pelvic lymphadenectomy, and urinary diversion (UD). 1 This treatment offers the highest rates of prolonged cure with 5-year recurrence free survival nearing 60%.1,2 However, complication rates of RC/UD are high, ranging from 64%-80%, with some degree of morbidity from the procedure being nearly guaranteed.3,4
Given the procedure's substantial complication rates and prolonged recovery, the impact of treatment on quality of life (QoL) has become an important outcome metric in MIBC. Current AUA guidelines recommend QoL implications be discussed prior to surgical intervention. 5 Health related quality of life (HRQoL) tools exist to measure the patient's assessment of functional disease burden. 6 Numerous interventions have been implemented to improve complications and improve QoL. These efforts include postoperative pathways, use of robotic surgery and increased utilization of continent diversions.7–9 While the literature has demonstrated similar complication rates and non-inferior oncologic results with these interventions, there have not been consistent differences in QoL metrics.9–11 Given that changes in surgical approach and hospital recovery have not significantly changed QoL outcomes, the logical question is whether inherent baseline patient factors impact QoL outcomes.
One specific patient-based factor that has gained interest is the concept of resiliency. Resilience measures one's ability to withstand stress and recover from difficulties. 12 It is thought that patients with higher levels of resilience experience better functional outcomes and more significant global improvement after setbacks. 12 Resiliency was originally defined in psychological literature and had 3 main aims: (1) to quantify resilience to study the biological and stress response to adversity, (2) to devise interventions to nurture resilience, and (3) to investigate strategies for coping with stress as a tool to screen high-risk patients. 12
While resiliency was originally researched and defined in psychologic literature, its implications have been explored in surgical literature. Orthopedic surgery has long focused on PROs and has robust findings suggesting an association between resilience and surgical outcomes in arthroplasty, arthroscopy and trauma. 13 Breast cancer literature similarly has found higher resilience serve as a protective factor for positive body image following mastectomy. 14
Objective
To our knowledge, resiliency has not been studied in patients with bladder cancer or those undergoing RC. Herein, we performed a prospective clinical trial of patients undergoing radical cystectomy to determine the correlation between resilience and self-reported quality of life. Our goal was to assess whether a person's hardiness relates to their feelings of well-being reflected in validated quality of life surveys during the peri-operative period of radical cystectomy. The study hypothesis is that resilience is positively correlated with QOL.
Methods
This non-randomized prospective clinical trial was performed through the University of Kansas Health System. The study protocol was approved by the institutional review board of the University of Kansas Medical Center (IRB #146138). It was then registered as a clinical trial through the NIH (NCT06337305). All study participants provided written informed consent. Baseline demographic information and tumor staging were collected at enrollment in a HIPPAA-complaint prospectively collected database (REDCap). Additionally, complication data up to 90 days was annotated using the Clavien-Dindo scale. 15
All patients enrolled in our study underwent an open radical cystectomy as treatment for localized high risk non-muscle invasive bladder cancer or MIBC. Patients with MIBC were referred to medical oncology for consideration of neoadjuvant chemotherapy eligibility. Our program utilizes a standardized perioperative pathway including early refeeding, no nasogastric tube, carbohydrate fluids up to several hours prior to surgery, narcotics avoidance, a mu-opioid receptor antagonist and regional anesthetic blocks. Additionally, patients are offered a visit with our stoma boot camp program. 16 Three surveys were utilized to assess participant resilience, patient-reported outcomes (PROs) and health related quality of life (HRQoL). These surveys were given to participants prior to radical cystectomy, at 2–3 weeks postoperatively and again at 90 days postoperatively. Surveys were administered electronically and could be completed either during the clinic visit or from home. Of note, all patients followed the same post-operative pathways with post-operative visits at 2–3 weeks post-op and then again at 90 days, consistent with the survey administrations. 58 patients in total were enrolled, however, 6 patients did not complete surveys at all 3 time points, so there enrollments were not used in data analysis.
The Connor-Davidson Resilience Scale (CD-RISC) was administered to measure resilience. This is the most commonly utilized resilience scale in scientific literature. 17 The original CD-RISC is a validated survey assessing overall resilience via a 25-item questionnaire with survey participants answering each question on a 5-point Likert scale. Question items assessed patient characteristics including self-esteem, ability to cope, perceived strength and use of humor in stressful situations. 12 The scale has the subject rate how they felt over the prior month, with scores ranging from 0 to100. Higher scores indicated a higher level of resilience. Of note, the average score of the general population is 80.4. 12 Shorter versions of CD-RISC exist (10- and 2- item scales). However, the 25-item scale has demonstrated the highest level of internal consistency (0.90) and was therefore utilized for our study. 18
PROs were obtained via the PROMIS®29-v2.0, a measure of physical and mental health via self-reported outcomes, with the reliability of 0.98 and 0.97 respectively. 19 This NIH-validated survey characterizes physical, mental and social health via seven domains of 4 questions each, with an additional domain (question 29 of the survey), about pain intensity. 19 These domains are rated on a scale of 1–5 and assess physical function, anxiety/depression, sleep disturbance, social roles, and fatigue. The final question quantifies pain intensity on a numeric scale of 1–10. The sum of all domains results in an overall score, with lower scores reflecting better measures of health.
Finally, to assess health related quality of life (HRQoL) patients were administered the Functional Assessment of Cancer Therapy- Bladder- Cystectomy (FACT-BL-Cys). This is a condition specific HRQoL instrument validated for patients with bladder cancer undergoing RC with UD. 20 This survey assesses well-being across five domains: physical, social, emotional, functional, and the effects inherent to the cystectomy itself. The survey items are scored on a 5-point Likert scale, with higher scores indicating better HRQoL, with a maximum score of 176.
Demographic information, including age, sex, race, ethnicity, and socioeconomic status are reported using descriptive statistics (means, medians, standard deviations, frequencies, and percentages as appropriate). The study hypothesis is that resilience is positively correlated with QOL, i.e., CD-RISC is positively correlated with FACT-BL-Cys. Correlation was assessed using Spearman rank correlation. The sample size was estimated using simulation with the PASS software (v. 15.0.10). Assuming the absolute correlation coefficient ρ≥ 0.40 (i.e. a moderate level of correlation) and a significance level of 0.05, 51 subjects were required to achieve 80% power to test the hypothesis that resilience and QoL are correlated.
Results
Fifty-two patients were enrolled in this prospective clinical trial between November 2020 and August 2022. All surgeries were performed by one of 5 fellowship trained urologic oncologists. The demographic characteristics of the group are demonstrated in Table 1. The median age of the cohort was 71 years with the majority being male (76.9%). Eight (15.4%) participants had a diagnosed mental health disorder at baseline. The majority of the patients underwent ileal conduit creation. In our series 38% of patients received neoadjuvant chemotherapy. On final pathology 27 (51.9%) patients had pT2 or more significant disease with 19.2% having positive lymph nodes.
Patient demographics.
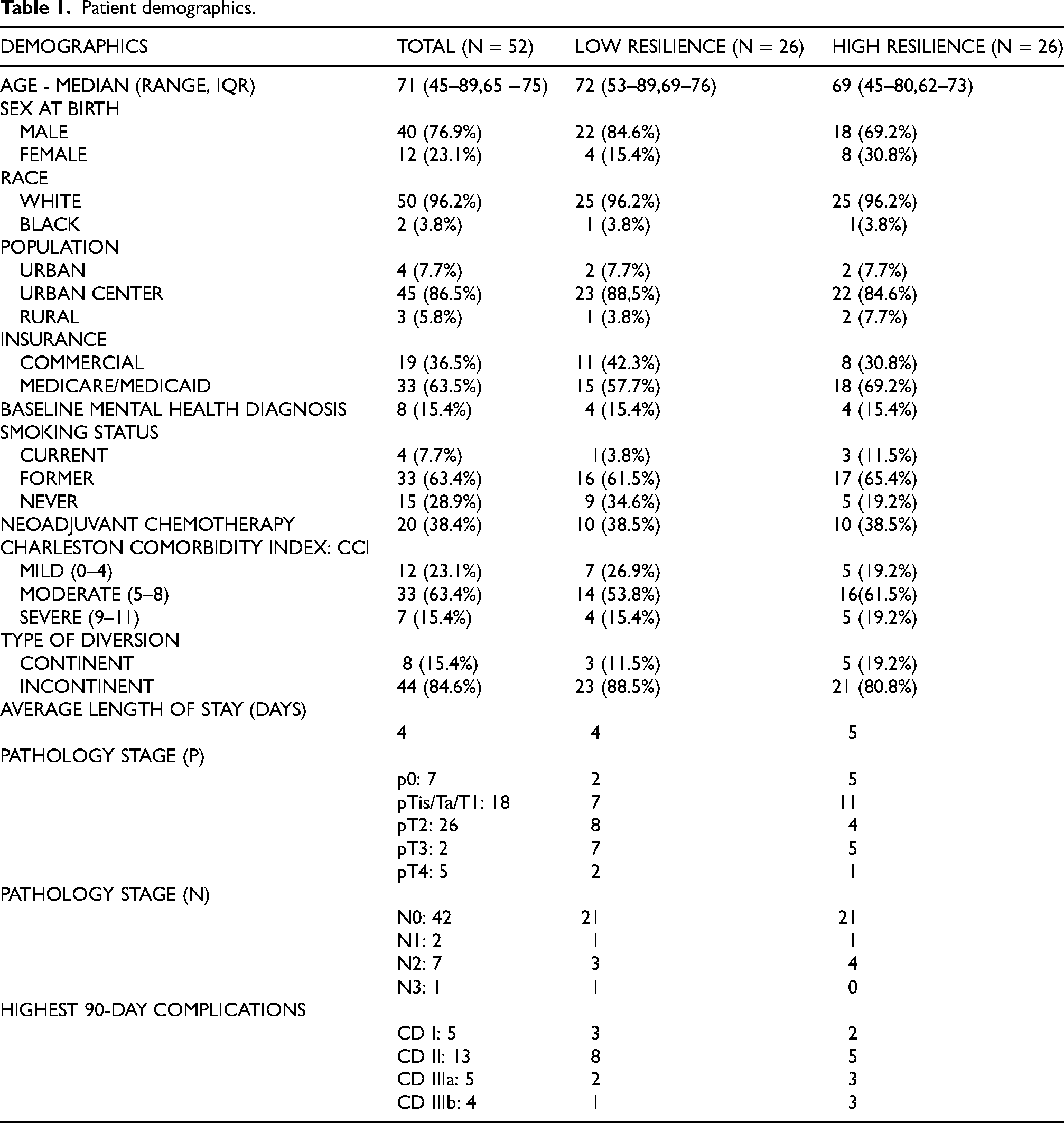
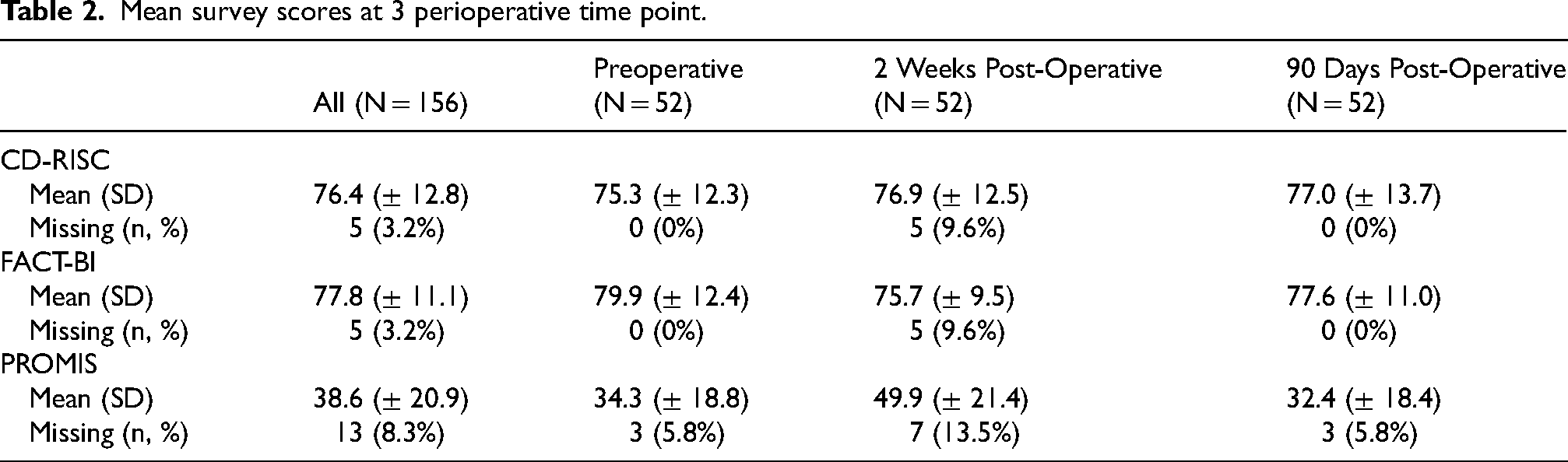
Table 2 demonstrates the results of the Connor-Davidson survey, the PROMIS survey, and the FACT-BL at each of the three time points. As expected, the PROMIS score increases from a baseline of 34.3 to 49.9 at two to three weeks postoperatively reflecting the increase in anxiety/depression, sleep disturbance, fatigue, and decrease in physical function. The score returns to baseline at 90 days (32.4). Similarly, the FACT-Bl-Cys score decreases at two to three weeks from a baseline of 79.9 to 75.7. This reflects the changes in the patient's physical and functional status inherent to radical cystectomy.
Mean survey scores at 3 perioperative time point.
Resilience assessment utilizing the Connor-Davidson survey was performed at the three corresponding perioperative time points. The mean scores preoperative, 2–3 weeks postoperative, and at 90 days were 75.3, 76.9, and 77, respectively (Table 2). The subjects were then categorized into a low versus high resilience group based on their preoperative CD-RISC at a natural cut point of 75 (Figure 1). There were 26 participants in each category. Given that no specific cut points for high or low resilience have been correlated with specific outcomes in the existing literature, as a pilot study, one of our priorities was to establish this value for our unique patient population. The mean CD-RISC score of 75.3 preoperatively, makes 75 a natural cutoff point and ensures an even distribution of participants, advantageous for statistical analysis given the sample size. Of note, Table 1 also demonstrates baseline factors in regards to the low versus high resilience groups. For preoperative CD-RISC, the mean (±SD) scores for the high and low groups were 85.73 (±7.27) and 64.92 (±5.64), respectively. The mean CD-RISC score in the high group was significantly higher than the low group, p < 0.01. This significance was maintained at two weeks postoperatively with CD-RISC of 85.0 (±9.72) and 70.35 (±10.54), p < 0.01. Further, at 90 days postoperatively, the CD-RISC score for the high group and the low group were 81.92 (±13.03) and 72.04 (±12.66) (p = 0.02). All statistical analysis was adjusted for multiple comparisons using Bonferroni correction.
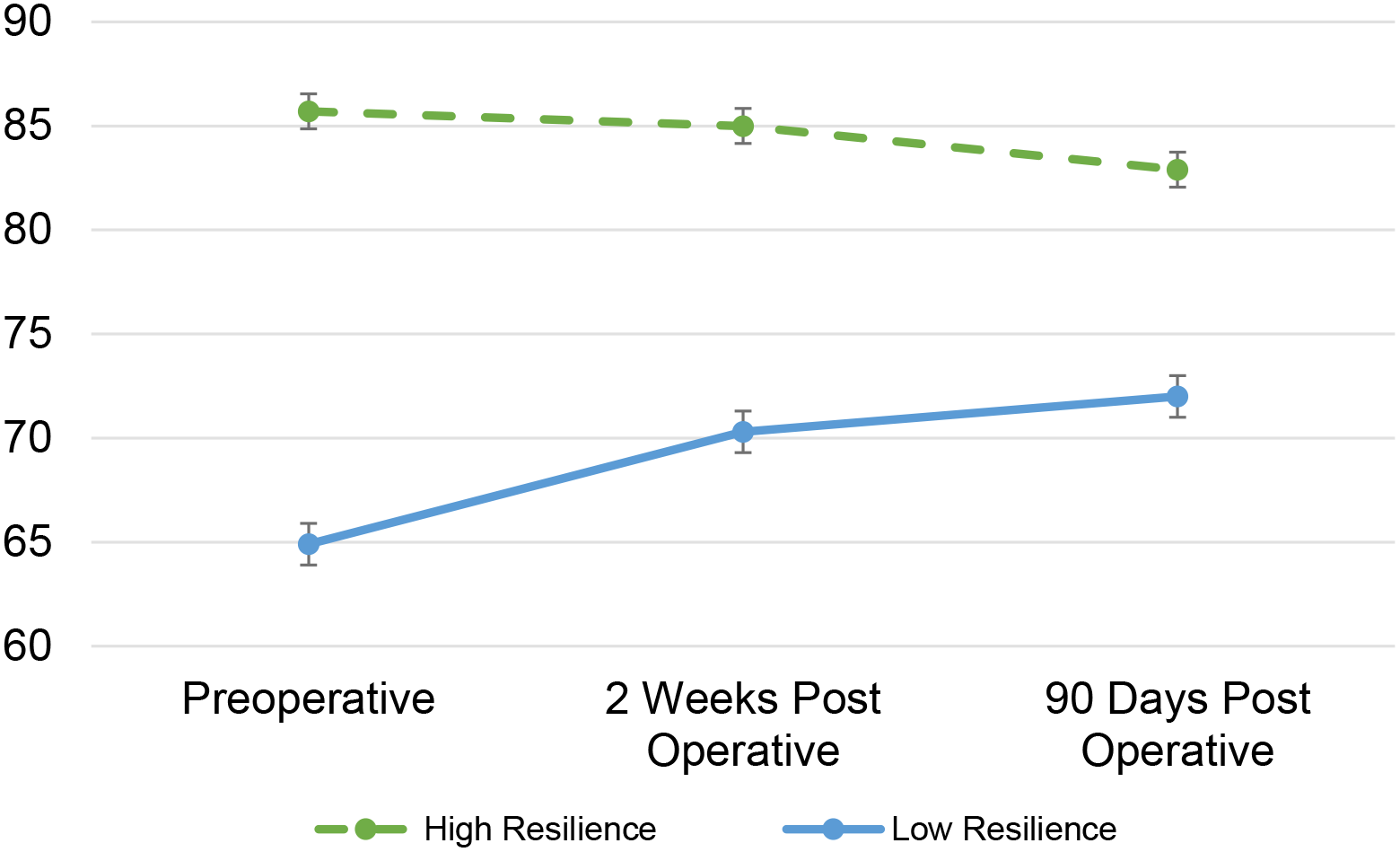
Resilience scores at 3 perioperative time points.
Participant resilience levels using the CD-RISC did not correlate with quality-of-life outcomes (FACT-BL or PROMIS) at the preoperative and 2 to 3-week postoperative time points. However, at 90-days postoperative, resilience was significantly correlated with the FACT-Bl-Cys score (r = 0.478, p < 0.01) and with PROMIS outcomes (r = -0.437, p = 0.01). Table 3. This correlation reflects that patient with higher resilience had higher self-reported quality of life at ninety days. Using the non-parametric Kruskal-Wallis p-test, resilience scores at 90 days did not correlate with the patient's final T stage (p = 0.68). Using a Spearman rank correlation, the resilience scale was also not found to be significantly correlated with peri-operative complications (r = 0.022, p = 0.88). These data demonstrate that participant resilience at 90 days did not reflect disease status or complications experienced.
Resilience, quality of life and patient reported outcomes at 3 perioperative time points.

Discussion
In this prospective clinical trial, a patient's resilience level was positively correlated with a higher QoL and improved PROs at 90 days following radical cystectomy and urinary diversion. These findings were independent of tumor stage or complications. Additionally, we found that resilience was sustained throughout the peri-operative period, with patients with higher baseline resilience scores maintaining these scores at two weeks and 90 days postoperatively, compared to those with lower baseline resilience scores. This was the first study to correlate patient resilience with QoL outcomes in bladder cancer.
Resilience is a gauge of dynamic reserve. It measures one's ability to withstand stress and recover from difficulties. 12 Early literature surrounding the concept of resilience, started as a set of constructs supporting “hardiness” as an emotional shield for mental health. 21 Literature has since defined factors that influence resilience to include: viewing stress as a challenge/opportunity, adaptability to change, engaging the support of others, optimism, faith, sense of humor and tolerance of negative effect. 12 Understanding the components of resilience has allowed for not only the quantification of the concept, but also has allowed the study of its correlation to clinical outcomes. Further, fields with early exploration of resilience have since been able to improve resilience through psychologic intervention, demonstrating that resilience itself is a coachable skill (PRISM, Mastectomy, Colorectal).
Several studies exist demonstrating the ability to improve resilience, two of which are notable for improvements in cancer patients specifically. One study provided stress management and resilience training to breast cancer survivors and demonstrated improvement in resilience, perceived stress and QoL after 12 weeks. 22 Another study utilized a similar training program, Promoting Resilience in Stress Management (PRISM), which was a skills-based intervention to improve stress management in adolescents with cancer. They again found that patients in the intervention group had improved cancer related QOL, improved resilience and decreased psychologic distress. 23
In the past, when studying QoL there was limited use of consistent, validated measures, allowing for objective, validated ways to assess QoL outcomes. Therefore, the overall quality of data has been questionable. 24 This paper aims to not only introduce the concept of resilience into the field of urologic oncology but also to demonstrate its ability to influence clinical outcomes using validated psychometric tools like the CD-RISC and FACT-Bl-Cys. While literature around this concept is sparse in the field of urology, this paper provides a landscape for future studies to explore not only how resilience affects sub-domains within HRQoL (like continence, sexual function, and body image), but also how resilience can be modified pre-operatively. Another important study will be assessing the influence of frailty as it interacts with resilience. Bladder cancer is generally a disease of the elderly and frailty in the geriatric population remains an important pre-operative factor under investigation when assessing eligibility for RC.
Several limitations to our study should be acknowledged. The Connor-Davidson scale measures psychological and mental resilience, and our study does not reflect the physical aspects of frailty or hardiness in our assessments. Also, as this is a prospective survey study, the performance of all the measures was challenging at times for participants, given the unpredictable nature of the recovery period. The missing instruments are acknowledged in our Tables. It is unclear whether the missing data points would impact the results. We did not explore the baseline mental health disorders that may impact the final results and whether certain diseases correspond to more or less resilience. One prior prospective study did assess natural fluctuations in depression and HRQoL outcomes and found that there was a peak of depression at the 3-month mark. After 12 months psycologic and HRQoL outcomes stabilized to pre-op levels. 25 We acknowledge that based on previous literature, QOL measures out to 12 months are informative and this method will be incorporated into future studies. Our patient population did not include patients who underwent robotic surgery and the number of patients who received a continent diversion were limited (15.4%). We understand that QOL studies have demonstrated improvement in robotic and continent diversions. Given that our patient population is all open and mainly incontinent diversions, we feel that the homogeneity of the population in regards to these factors actually places more focus on the effects of resilience and quality of life and strengthens our results. The homogeneity allows for internal validity in assessing the primary outcome of resilience. What we take from prior literature in the context of our current study is that there are numerous variables that can affect QoL in the peri-op and post-op period with diversion type and baseline resilience being unique factors. Whether these variables further modify the impact of resilience on QoL remains an area of future research and could explain why prior research regarding surgical approach and diversion type have been inconsistent in their QoL findings. Finally, we recognize that performing correlation analysis alone is a limitation of our current study, since the potential confounding factors may impact the association between resilience and quality of life. The main reasons we chose to perform correlation analysis are 1 as a pilot trial, our primary aim was to explore the direct relationship between resilience and quality of life. Given the exploratory nature of our research, correlation analysis was deemed appropriate for identifying initial associations; (b) our analytical approach aimed to give equal emphasis to both resilience and quality of life rather than positioning one as a dependent variable and the other as an independent predictor, which aligns with the correlational methodology we employed. Therefore, to gain a more comprehensive understanding of the relationship between resilience and QoL, future studies could benefit from incorporating regression analyses or other multivariate techniques to control for these confounding variables.
Our study is the first of its kind to explore the relationship between a patient's baseline resilience and their quality of life through the perioperative time of radical cystectomy. We demonstrate that higher resilience correlates with improved quality of life at 90 days and that resilience is independent of pathologic stage and complications. Given that resilience is dynamic and teachable, the next exciting logical steps are interventions that modify patient resilience around the time of surgery.
Footnotes
Abbreviations
Acknowledgements
The authors have no acknowledgements
Author contributions
All authors had access to the data, statistical analysis and the manuscript throughout the project. All authors approved final version for submission and significantly contributed.
Funding
The authors report no funding
Conflicts of interest
Lauren N. Kennedy, Caleb S. Miller, Danica N. May, Evan Fruhauf, Hadley Wyre, Moben Mirza, Junqiang Dai, Jeffrey M. Holzbeierlein, Hayley Stolzle, Moira Mulhern, Mihaela Sardiu and Eugene K. Lee have no conflicts of interest to report.
