Abstract
Epidermolysis Bullosa (EB) is a very rare genetic skin disorder associated with skin fragility. It results in blister formation on the skin. The purpose of this paper is to update the progress of a child with Dystrophic EB (DEB) who survived from infancy to preschool years and later died with recurrent skin blisters, bone marrow transplantation, and life support measures. A case analysis was done to evaluate the progress of the child. The mother of the child signed the written informed consent and granted permission to publish the details of the child with images and without disclosing the identifying information. The management of EB requires a multidisciplinary team approach. The care of the child should be aimed at protecting the child’s skin from injury, nutritional support, meticulous wound care, and management of complications as required. The prognosis varies from case to case.
Introduction
Epidermolysis Bullosa (EB) is a rare inherited skin disorder associated with skin fragility, which results in blister formation on the skin. The prevalence of EB is unknown, however, it is estimated to affect 1 in 30 000 to 50 000 people. In the United States, the incidence rate is 20 per million births. Children of both sexes are affected by EB. It is reported in all ethnic groups. 1 EB is a heterogeneous group of mechanobullous disorders. 2
Types of EB
EB is manifested in 4 different forms. Simplex EB (EBS) with blisters within the basal keratinocytes in the epidermis is the most common and mild form of EB. It involves only the epidermis of the skin. In Dystrophic EB (DEB), the lamina densa in the dermis is involved. The blisters occur on the feet, hands, elbows, and knees. The middle layer of the skin is involved in junctional EB (JEB). The blisters are found in the lamina lucida of epidermal-dermal junction. In Kindler EB, the blisters occur during infancy and reduce over time as the child grows. The blisters are developed at multiple levels of the skin. Dark patches, the poikiloderma is formed over the skin as the blister diminishes. This is a rare form of EB. 3
The pattern of Inheritance of EB
EBS is dominantly inherited; JEB is recessively inherited; DEB can be either dominantly or recessively inherited; Dominant dystrophic EB (DDEB) is usually mild and Recessive dystrophic EB (RDEB) is typically more generalized and severe than DDEB. 2 Some people inherit the mutation from one of the affected parents. In other people, the new mutations in the gene occur though they don’t have a history of the disorder in their family. In rare cases, EB is inherited in an autosomal recessive pattern. 4
Clinical Manifestations
EB is a chronic condition that is painful and disfiguring. Generally, patients with RDEB may have co-existing conditions such as clubbed foot or hands and fused digits. These children are usually called, “butterfly children” as their skin is very fragile like butterfly wings. 5 In DEB, the lesions can either appear at birth or occur anytime until early childhood. The lesions are usually seen as blisters that may rupture and become scars. The blisters are frequently seen at the trauma site or pressure points. This usually occurs in the feet, hands, mouth, gastrointestinal tract, genitalia, or diaper area in children. The severity of EB is not limited only to skin. It involves various systems including gastrointestinal, cardiovascular systems, joints, and bones, and leads to other conditions such as carcinomas and malnutrition. 6
Diagnosis
Skin biopsy along with transmission electron microscopy (TEM) and/or immunofluorescent antibody/antigen mapping can diagnose EB. Molecular genetic testing is recommended. 7
Management
The treatment involves the transplantation of laminin-modified stem cells through bone marrow transplantation. Another option for treatment is changing the mixture of keratins produced in the skin. 7 Systemic granulocyte colony-stimulating factor (G-CSF) is found to promote wound healing in patients with DEB. 8 Transplanting skin derived from genetically modified stem cells on the wound surface is a recent treatment. 9 There is no cure for EB. The management involves pain control, wound care, infection control, nutritional support, and prevention and treatment of complications. 10
Monitoring
Epidermolysis Bullosa Disease Activity and Scaring Index (EBDASI) objectively assesses and quantifies the severity of EB. This is a tool for clinicians and patients to monitor the severity of the disease. The other tools for monitoring include Birmingham Epidermolysis Bullosa Severity (BEBS) and an instrument for scoring clinical outcomes of research for EB (iscorEB). 11
Prognosis
Most patients with EBS have relatively mild disease and have an abnormal life expectancy. Very rarely patients with severe EBS die during infancy. Patients with DEB have a variable life expectancy depending on the subtype. Children with severe RDEB usually die in early to mid-adulthood from metastatic cancer, but others usually have an abnormal life expectancy. 12
Case Report
Family History
The case record of a 3-year-old Omani female child with DEB was evaluated. The parents had a consanguineous marriage. The child has 8 siblings and all are healthy and no one has a history of EB. However, 3 cousins of the child have EB. Two of them died at the age of 6 months and 5 years respectively. One child is alive and is 27 years old. The parents reported that there were many miscarriages in the family.
Clinical Findings
The child was born through normal vaginal delivery. The birth weight was 3.2 kg. The child started having multiple bullous skin lesions on the face and hand immediately after birth. The bullous lesions continued to appear especially after friction. Some of these bullae were fluid filled and some were not. It appeared in almost all parts of the body and affected the mouth and eyes. Figures 1 to 3 show bullous lesions in most of the body parts of the child.
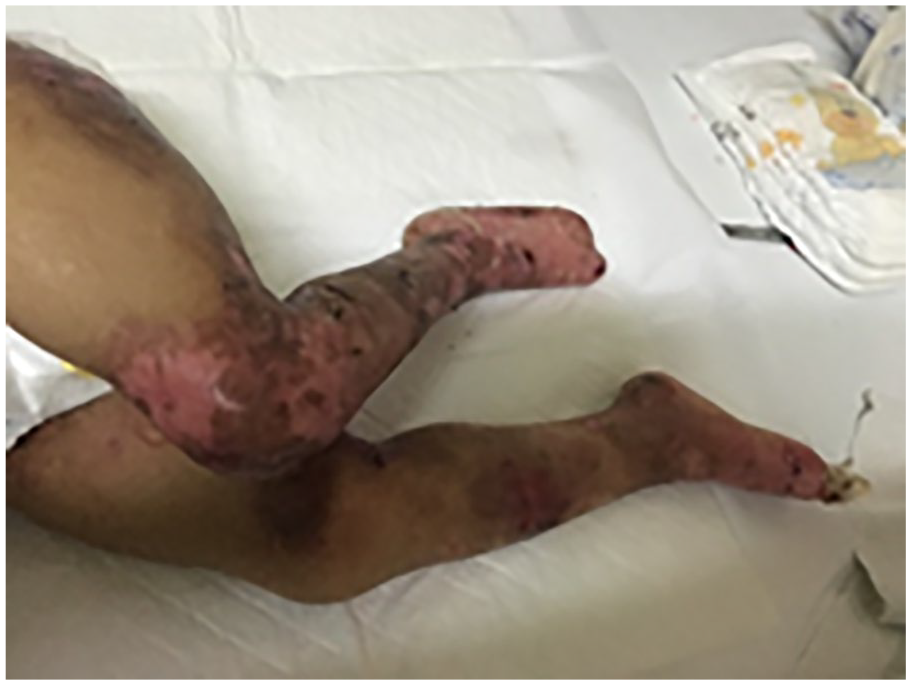
Lesions in the leg.

Lesions in the knee.
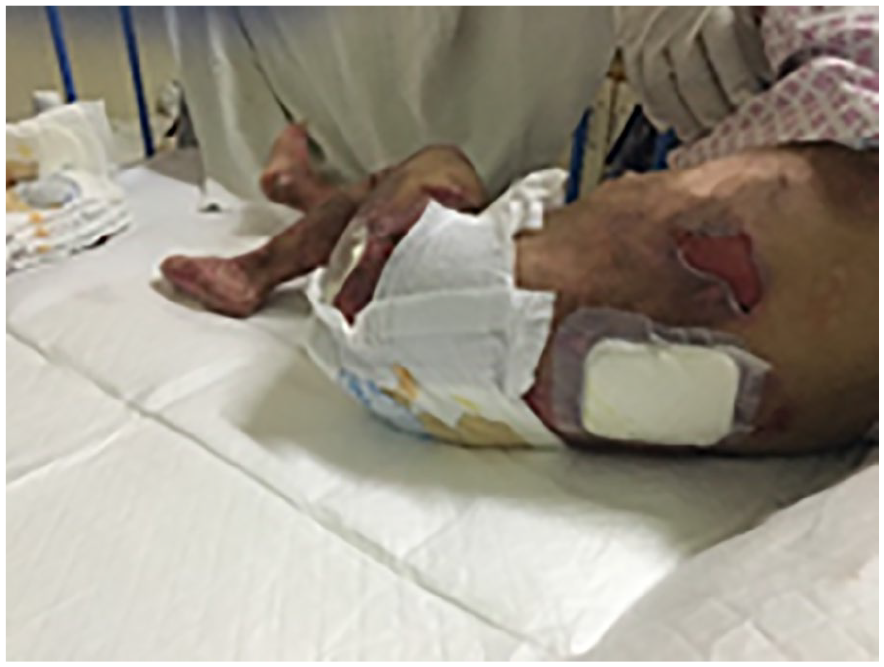
Lesions in the back.
Diagnosis
The child was diagnosed to have DEB at birth itself. Molecular genetic testing confirmed the diagnosis of DEB. It was noticed by the mother at the age of 2 months that the child had abnormal breathing sounds. She has been diagnosed to have Laryngomalacia. Recurrent admissions to the hospital were done due to aspiration.
Treatment
Following the confirmation of the diagnosis of DEB, the child was treated many times for skin infections as well as for aspiration pneumonia with IV Amoxicillin/Clavulanate potassium. The child was nebulized with salbutamol sulfate every 6 hours. Oral nystatin triamcinolone was used to treat oral thrush. The skin integrity was maintained by minimal skin handling, avoidance of pressure, avoidance of scratching, and adhesives and cling wrapping were used to protect the IV line. White soft paraffin was used to soothe the lesions on the skin and advised to cover it with Jelonet paraffin.
Post Bone Marrow Transplant (BMT) Management
The child underwent allogenic related peripheral blood stem cell transplant with the sibling allograft in India in 2017. During the post-BMT period, on day 3, the child developed erythema over the left leg without tenderness. It was managed with Mupirocin and Bactigras gluconate for skin lesions. On day 4 following BMT, new bullae appeared on the right groin, and mucosal erythema was found for which she was treated with Cefoperazone, Sulbactam, and Targocid. On day 5, she developed oral mucositis with low-grade fever and managed with the same antibiotics. On day 6, the fever was high and blood culture was done and Meropenem and Colistimethate were added. Injection Morphine sulfate was given to alleviate pain. On day 10, she had a productive cough associated with increased secretions. Saline nebulization was started. Her skin lesion healed gradually and was clinically stable. Injection Tacrolimus and Injection Methotrexate sodium were used for Graft Versus Host Disease (GVHD) prophylaxis.
The child exhibited the features of acute GVHD of skin and gut by day 17 in the form of an erythematous rash and presented with loose motion. Her skin lesions healed well and dry after the addition of Methylprednisolone ointment for mucosal lesions. Nasogastric feeding was continued. During post bone marrow transplantation period, the child had frequent hospitalization. In 2019, she was admitted with an infective exacerbation of chronic lung disease with fever and an increased volume of greenish secretions. The CRP was 24, no leukocytosis, sputum sample showed pseudomonas infection. The child was started with the medication Levofloxacin, Piperacillin/Tazobactam, and Trimethoprim/Sulfamethoxazole.
Tracheostomy was done on February 2018. MRSA was traced out from the tracheal aspirate. For better coverage of MRSA, a dose 5 mg/kg/12 hours of Sulfamethoxazole and Trimethoprim component were provided. The child also received Azithromycin 3 days/week, Folic acid, Montelukast sodium, and Budesonide inhalation. Topical eye management was applied for dryness, and topical skin care was provided. She was treated with IV Piperacillin/Tazobactam for susceptible pseudomonas infection from the tracheal aspirate. The child developed esophageal stricture for which esophageal dilatation was done twice. The last dilatation was performed in September 2019.
Progress of the Child
The child had a tracheostomy in situ. The child was on BiPAP, 10/5, FiO2 30% overnight, and daytime with O2 via Swedish nose. The saturation was maintained. The child was receiving feeding through a gastrostomy tube. The child was receiving medications such as Jelonet paraffin, Vitamin E capsule, White soft paraffin/ Liquid paraffin cream, Aqueous cream, Azithromycin suspension, Tablet Ciprofloxacin, Ferrous glycine sulfate drops, and Methylprednisolone. However, the child died on 30th March 2021 due to cardiac arrest.
Discussion
EB may occur at any stage from birth to 2 years of age. Literature shows that EB occurs in families who had consanguineous marriages in different parts of the Middle East. It has a distinctive gene mutation (mutations in LAMB3, LAMA3, and in LAMC2) 13 which is not found in EB patients in US and Europe. 8
Patients with DEB and Kindler EB tend to have chronic involvement of the esophagus with resulting scarring and stenosis. A single center experienced based study states that 6 patients with EB underwent 31 dilatations during their 4 years of follow-up. Out of these 6 patients, 4 were females and 2 were males. 9 Similarly, the case presented by us also developed esophageal stricture for which she underwent esophageal dilatation twice. This confirms that esophageal stricture is a common finding in children with DEB. Nurses must learn to care while children with DEB undergo esophageal dilatation.
EB is a life-threatening disease which has a high risk of death due to airway obstruction. Airway involvement is mainly a feature of JEB, but only very infrequently seen in other forms. Tracheostomy is rarely needed in non-JEB patients. However, airway management including tracheostomy must be a priority for EB patients having airway involvement. 9 Likewise, the child presented in this case report also developed airway obstruction for which she underwent tracheostomy management. Nurses are to be prepared to care for children receiving tracheostomy care.
Due to complications of EB, the patients usually suffer from malnutrition, decreased immune system, growth, and delay in wound healing. In addition, it affects their quality of life. 12 Therefore feeding through a gastrostomy tube is a beneficial strategy to improve the nutritional status of children with EB. Gastrostomy Tube Feeding (GTF) is very much endured and improves the nutritional status, growth and development of the patient. It ought to be provided in patients incapable to receive orally and additionally exhibiting weight and height loss in spite of routine dietary advice. 14 The child mentioned in this case report was receiving nutritional support through gastrostomy tube feeding. The child was started with gastrostomy tube feeding as the child was unable to swallow her saliva and had struggles in chewing the food. Nursing care should focus on meeting the nutritional needs of these children.
The most extreme type of EB is the recessive form of DEB which ultimately leads to the disfiguring of skin lesions, hand and foot deformities, growth retardation, and failure to thrive.15,16 In the current case, all of the listed features are seen. This indicates the need for developing nurse-led interventions to manage these deformities.
Anemia is considered to be a recurrent and serious problem in severe forms of EB specifically in recessive DEB and JEB. Hemoglobin levels less than 8 g/dl cause delay in wound healing due to diminished oxygenation in patients with venous ulcers. The suitable skin care, prevention of skin infection, and its treatment may reduce blood loss through the skin. Oral iron supplementation is commonly used to cure anemia, although it may vary in individual effectiveness. In cases where hemoglobin consistently drops below 8 gm/dl and in symptomatic patients who fail to respond to other therapies, blood transfusion is considered the best choice. 17 In the current case, the child was treated with Ferrous Sulfate and Folic acid and has undergone multiple transfusions of blood. It warrants the nurses to provide meticulous care to these children while receiving blood transfusions.
Quality of Life of Parents and Children With EB
An existence with EB significantly affects the whole family and can cause deterioration in the QoL for both the child and parents. 18 Several studies have recognized the effect of EB on the physical and emotional health of parents and caregivers. This involves challenges in establishing care, issues within their own relationship, having less vitality, the uncertainty of the sickness, and related troubles in the short and long-term plans. Such issues can affect the entire family which affects not only the ability of each member to satisfy their own needs; but also their level of life satisfaction.19,20 Likewise, the child in our case report was frequently hospitalized and had a longer stay in the hospital. This caused financial, physical, and mental burdens on parents. Also during the hospitalization, the mother as a close caregiver always remained with the child. The mother is trained by the nurses to perform wound dressing, suctioning, and feeding at home.
Parents endure immeasurable psychological stress because of their child’s pain while managing the child daily. The challenges of being a parent and caregiver who wish to save their child inflict a psychological burden on the parents which affects their wellbeing of parents. Therefore, it is very important to provide early, extensive and long-term support for family members to enable them to cope with the emotional burden that they continue to function as care providers. Psychosocial counseling is suggested to help families to oversee the existence of EB. Family support can help to reinforce family relationships, avoid family breakdown and enhance QOL and the well-being of family members. 21
Nursing Care Considerations
General
A comprehensive evaluation of vital signs, respiratory status, pain assessment, risk of infection, and need for intensive monitors should be continuously done. 22
Bathing
Patients with extreme forms of EB and open wounds when bathed in normal water are agonizing. Salt water bath significantly reduces pain. Available evidence indicates that in patients with RDEB, salt water baths significantly reduce discomfort and pain. Additionally, specific beneficial effects include the elimination of body odor and exudates of skin. 23
Skin and Wound Care
Dermatologist’s routine follow-up includes a comprehensive assessment of the body and dermatological treatment of all forms of EB and skin lesions. Oily emollients such as half fluid/half white soft paraffin to scrub napkin area in inclination to water are required. It is advised to bathe frequently in tepid to lightly warm water. The number of baths can be adjusted for each case. The skin should be dried after bathing with a towel by gentle padding. 14 Cleaning of the diaper area should be done with liquid and white soft paraffin in equal proportions or with an emollient. 24 Caregivers should be mindful of the unusual signs and motivated to report any change in the appearance of a chronic wound, a strange sensation or a rise in pain within an existing wound. 25
Feeding
Children who are receiving enteral feeding should be allowed to improve oral sucking and swallowing skills. Maintaining oral skills is critical for later-life social eating and growth. 26
Recommendations
The discharge condition should be met before the child is discharged from the hospital. The caregivers must be trained to be competent in the care of the wound and skin. In regard to patient education, EB Handouts and resource lists are to be provided to the patients and caregivers. 22
Preclinical advances in cell-based, protein replacement and gene therapies are paving the way for clinical successes with gene correction, raising hopes amongst patients and clinicians worldwide. 27
Conclusion
Therefore, the authors conclude that the management of EB requires a multidisciplinary team approach. The care of the child should be aimed at protecting the child’s skin from injury, nutritional support, meticulous wound care, and management of complications as required.
Footnotes
Acknowledgements
The authors acknowledge the mother of the child who consented to publish the data without any identifying information.
Author Contributions
HP: Collected the data and wrote the initial draft of the manuscript
JA: Added additional content, reviewed and edited the manuscript
SEJ: Collected the data and reviewed the manuscript
SCV: Collected the data and reviewed the manuscript
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
