Abstract
Newborn skin disorders are quite common and happen to occur during the neonatal period. Most of the birthmarks are transient; however, worried parents often seek medical advice from their child’s physician regarding skin lesions. Thus, it is important to differentiate the skin lesions from pathologic ones to avoid unnecessary diagnostic or therapeutic procedures. This is the first published study in Lao neonates that carried out the data from 4 central hospitals in Vientiane Capital, Lao PDR from September 2019 to February 2020. Among 500 neonates, Sebaceous gland hyperplasia (53%), Mongolian patches (46.6%), and Erythema toxicum neonatorum (30%) were the 3 most common cutaneous conditions found in the Lao newborns. From a clinical point of view, these findings are often a source of parental anxiety and medical concern for inexperienced clinicians.
Introduction
Neonate skin disorders are common observations in the neonatal period. Most of these conditions are short lived, however, concerned parents often seek medical advice from their child’s physician regarding these skin lesions. Thus, it is important to differentiate the skin lesions from pathologic ones to avoid unnecessary diagnostic or therapeutic procedures. In Lao PDR, there are scarcely any research publication on neonatal skin lesions. A working knowledge of both normal and abnormal cutaneous lesions of the neonates is required to determine which skin lesions require early intervention. Moreover, it is also important to provide appropriate counseling to the parents. This study is the first of its kind to describe neonatal skin lesions during the first 5 days of life in the Lao neonates. The data will provide a reliable resource for Lao pediatricians to be familiar with these skin conditions and efficiently cope with the parental concerns of the cutaneous findings in the newborns.
Material and Methods
A cross-sectional research study survey was conducted to collect the skin lesions data in the newborns during the first 5 days of their life. The data collection was carried out effectively from 4 central hospitals in Vientiane Capital, Lao (Mahosot, Setthathirath, Mother and Children, and Mittaphab Hospitals). About 500 consecutive newborns and their mothers were recruited for this research study. The study was conducted from September 2019 to February 2020. After clarification, informed written and verbal consents were obtained from parents to participate in the study. Pediatric dermatologists performed the required dermatological assessments. At the end of the study, the data codification and analysis was performed using the Statistical Package for Social Science (SPSS) Version 22. The statistical analysis are as follows: descriptive statistic uses for describing the dependent and independent variables as frequency and percentage distribution, minimum, maximum, mean, and standard deviation. The inferential statistic uses to perform the association between 2 variables. The relation between birth weight, race of parents, and neonatal skin lesions will be analyzed using chi-square test. A P-value less than 0.05 considered as statistically significant.
Ethical Approval and Informed Consent
The study was approved by Institutional Review Board Ethical Committee of the University of Health Sciences, Lao PDR (#IRB No.121/19) before enrolling all the participants.
Results
Demographic Data
About 500 consecutive newborns and their mothers were enrolled in to the study. With respect to maternal nationality, most of them 497 (99.4%) were Lao, followed by only 3 (0.6%) were foreigners that included Vietnamese, Chinese, and Switzerland. Among Lao nationality, there were 3 groups of tribes in the study population: LaoLoum 450 (90.5%), LaoSoung 41 (8.3%), and LaoTheung 6 (1.2%). In terms of maternal educational level, 171 (34.2%) had completed secondary school, followed by 157 (31.4%) with university, 74 (14.8%) had completed junior high school, and 10 (2%) had no schooling. However, in terms of employment, most participants 246 (49.2%) were house workers, followed by government employees 129 (25.8%), and 4 (0.8%) had no occupation. The maternal age ranged from 13 to 42 years with a mean age of 26.80 (SD 5.14). Their mean gestation age was 38.67 weeks (SD 1.45).
There were total of 18 cases (3.6%) with underlying maternal disease and 11 cases (2.2%) of documented maternal complications during pregnancy.
Type of Delivery Method, Birth Weight, and Apgar Score
In majority of cases, the newborns 377 (75.4%) were vaginally delivered and 123 (24.6%) were born by Caesarean section. The birth weight of the participants ranged from 1840 to 4680 g with a mean birth weight of 3145.02 g. Majority of cases, 479 (95.8%) had birth weight more than 2500 g. Detailed information in Table 1.
Distribution of Frequencies and Percentage of Delivery Method, Birth Weight, and Apgar Score.

Transient Neonatal Skin Lesion
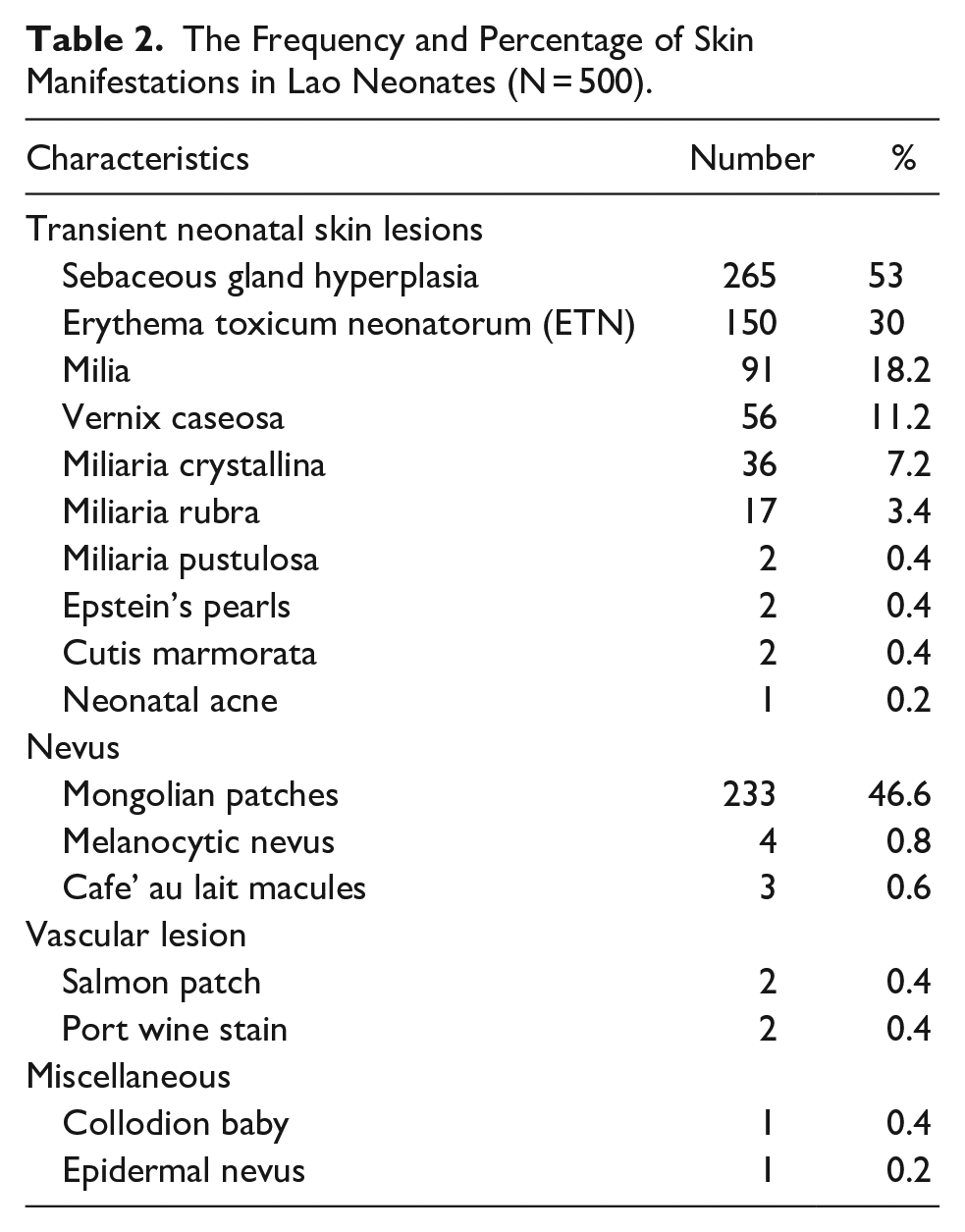
The most common transient neonatal skin lesions found at the first stage of physical examination were sebaceous gland hyperplasia 265 (53%), followed by erythema toxicum neonatorum (ETN) 150 (30%), milia 91 (18.2%), vernix caseosa 56 (11.2%), and neonatal acne 1 (0.2%). Other cutaneous findings found in this study shown in Table 2.
The Frequency and Percentage of Skin Manifestations in Lao Neonates (N = 500).
Pigmented Birthmark
The most common type of pigmented birthmarks found during the study period was Mongolian patches 233 (46.6%), the following frequent types of pigmented birthmarks were melanocytic nevus 4 (0.8%) and Cafe’ au lait macules 3 (0.6%). The majority of Mongolian patches 132 (26.4%) were <5 cm. Spot between 5 and 10 cm were documented in 63 cases (12.6%). The location of Mongolian patches were mostly occurred at the buttocks 180 cases (36%), followed by back 10 cases (2%), and legs 9 (1.8%), respectively. Detailed items in Table 3.
The Characteristic of Mongolian Patches Among the Study Population.

Vascular Lesion
Vascular lesion found during the study period were salmon patch: 2 cases (0.4%), and Port wine stain: 2 cases (0.4%).
Other Miscellaneous Skin Lesion
The present study found 1 case of collodion baby (0.2%) and 1 case of epidermal nevus (0.2%), classified as miscellaneous skin lesion in the present study.
Discussion
Neonatal birthmarks and cutaneous conditions in the newborns are the most common problems in a general neonatal pediatric practice. Some skin disorders are very specific to the neonatal period. These are mostly benign and transient and their main importance is the fact that they can imitate more serious disorders. 1 Several previous studies examined the prevalence of neonatal dermatoses in various countries and racial groups.2-6 However, there was no clinical data among Lao population. This study was thus, the first statistical and clinical study of neonatal cutaneous conditions during the first 5 days of life in Lao neonates.
Out of 500 newborns delivered at 4 central hospitals in Vientiane Capital, Lao from September 2019 to February 2020, the 2 most frequent neonatal skin lesions in the study population were sebaceous gland hyperplasia 265 (53%), and Mongolian patches 233 (46.6%). These results are comparable to the findings of the recent study that assessed the frequency of skin lesions in the newborns in Thai neonates by Techasatian et al. 7 The mentioned study revealed that Mongolian patches (66.7%) and sebaceous gland hyperplasia (60.9%) were the 2 most common. This similarity in the findings from the present study may be due the fact that the Thailand populations’ race is close to the Lao populations’ race. Thus, the cutaneous lesions that related to the 2 races and nationalities found to be in a similar distribution.
Mongolian patches are dermal pigmentation that appear as slate grey, grayish-blue, or grayish black color. These skin lesions were described to be found more often in Asian population. 8 Previous study in Turkey 9 have reported this skin lesion only 13.2% in the neonates. These findings were, however, in contrast to the study in Japan 10 that found Mongolian patches as high as 81.5%. As in Asian races, our study also showed a high number of Mongolian patches (46.6%). Beside the races and nationality, the present study found a potential risk of Mongolian patches and the birth weight of less than 2500 g compared neonates with birth weight more than 2500 g; OR (95%CI) = 1.91 (0.7-4.7); however, no statistically significant was found.
Mongolian patches are usually present on the buttocks. The sizes can be varied from less than 5 cm to a large extensive lesion. The present study revealed that the most common locations of Mongolian patches were on the buttocks and the size less than 5 cm found as the most frequent pattern. The other characteristics of Mongolian patches among the study population described in Table 3.
ETN was the third most frequent cutaneous lesion found in the study population. The onset of ETN is usually between 24 and 48 hours, but may occur at any time from birth to 14 days. 1 The characteristic lesions are poorly demarcated erythematous macules, often surmounted by central pale papules on erythematous base, some with predominantly pustules. 11 Even though, the manifestation of ETN looks threatening and overwhelming to lots of parental concerns. This cutaneous lesion is transient and benign in nature. The pathophysiology of this finding in the newborns have been discussed. Some theories such as allergic theory and a minor graft-versus-host (GVH) re-action caused by maternofetal transfer of lymphocytes prior to or during delivery have been proposed. 12 Previous study found that ETN were more frequent in dizygotic twins than in those who were monozygotic; 13 however, there were no twins in the present study to test such the same correlation. The authors tried to test the correlation of ETN and the birth weight as well as the maternal race, nevertheless, statistical correlation was not found, see Table 4.
Relationship between Birth Weight, Race of Respondents, and Erythema Toxicum Neonatorum (ETN).

There are important differences between the skin of the neonate, in particular the preterm neonate and that of the full-term born and the child. 1 Neonatal skin lesions in the newborns and their relationship to the maturity were discussed. Previous study revealed a significant correlation of some cutaneous findings (milia and sebaceous gland hyperplasia) and the maturity of the newborns. 7 In the present study; however, enrolled participants were all term neonates, thus, no correlation regarding maturity can be tested. We tried to use another possible parameter such as birth weight of above and less than 2500 g to test for a correlation between the cutaneous findings. However, no statistical correlation was found between the birth weight and the following cutaneous lesions: milia, miliaria, vernix caseosa, and sebaceous gland hyperplasia.
Salmon patch found only in 2 cases (0.4%). This finding is in contrast to the finding from previous study in Thailand 7 that found 36% of salmon patch in the neonates. Port wine stain found in a similar proportion. There was no case of infantile hemangioma in this study. This may due to the fact that the early cutaneous lesion of infantile hemangioma usually presents as a faint erythematous patch that is difficult to be seen within the first 5 days of life.14,15 More over infantile hemangiomas are more common in preterm infants, while the population in the present study were all full-term born which may affect the distribution of the cutaneous findings.
Limitations
Although our study is the one of the first to describe the frequency of neonatal skin lesion in Lao neonates, some limitations need to be acknowledged. Further studies about different factors affecting the dermatology are still of needed in this category of population. More studies with a larger number of newborns including of healthy ones, preterm, and postterm neonates are of needed.
Conclusion
Mongolian spots, sebaceous gland hyperplasia and ETN were the 3 most common cutaneous conditions found in Lao neonates. From a clinical point of view, these findings are often a source of parental anxiety and medical concern for inexperienced clinicians. Correct diagnosis and counseling the parents may relieve the anxiety and mental trauma. General pediatrician should be able to encourage and reassure the parents to understand the normal cutaneous findings commonly seen in the first 5 days of life in the newborn and point out the abnormal finding that need to be observed and concerned.
Footnotes
Acknowledgements
We would like to acknowledge Mr. Gurdeep Singh, for English editing the MS via Publication Clinic KKU, Thailand.
Author Contributions
VS and LT conceptualized and designed the study, contributed to the acquisition, analysis, and interpretation of the data, and drafted the initial manuscript. AP, SS, and AS contributed to the study concept and design. All authors reviewed and revised the manuscript and approved the final version.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
Informed Consent
The participants in this manuscript have given written informed consent to publication of their information details.
