Abstract
The Edmonton Seniors Centre Without Walls program provides free health, psychosocial, and educational telephone programming for older adults who experience multiple barriers to traditional in-person programming. The aim of this program evaluation was to assess outcomes of participation using validated scales of loneliness and psychosocial and health quality of life. Telephone interviews were conducted pre (n = 160) and post (n = 99) with participants. Given the variation in average attendance, results were assessed by level of participation: Low, Moderate, and High Users. There was statistically significant improvement in all participants’ attitudes towards their self-realization and towards energy levels, and EQ-5D-5L anxiety/depression scale after participation, along with a significant reduction in feelings of social isolation. The highest rates of improvement were seen within High Users. These findings suggest that telephone-based programs could be a useful intervention to improve the wellbeing and socially connectedness of older adults.
While today’s older adults are more active and healthier than previous generations, they are also more likely to be living with chronic conditions, disabilities, and mental health issues that put them at greater risk for social isolation (Government of Canada, 2014). Given this and the COVID-19 pandemic, the issue of social isolation has become an increasingly important topic for the future of aging. While this is an issue across the lifespan, older adults are at increased risk of becoming socially isolated, with studies suggesting the highest prevalence in those over the age of 80 (Demakakos et al., 2006; Dykstra, 2009). One in five Canadians aged 65 or older indicated that they felt lonely some of the time or often (Statistics Canada, 2012). While isolation may be by choice or by circumstance, the experience is subjective and based on the individuals’ perception. For the purpose of this study, the following definitions are used. Loneliness is the subjective experience of distress over not having enough social relationships or not enough contact (Lopata, 1969; Weiss, 1973). Social Isolation refers to an objective state rather than a subjective experience (Cohen–Mansfield & Perach, 2015). Social isolation often arises in situations where a person does not have enough people to interact with or enough social support, usually indicated by a small social network or a low number of regular social interactions (Chappell & Badger, 1989).
Loneliness and social isolation have gained increasing attention as social determinants of health given their associated physical/mental health risks. Their impacts are comparable to those of other health risk factors including physical inactivity, smoking, and obesity (MacLeod, et al., 2018). Older adults who are lonely have an increased risk of dying sooner and are more likely to experience a decline in their mobility, compared to those who are not lonely (Luo et al., 2012). Having supportive social relationships is related to decreased mortality risk (MacLeod, et al., 2018). Loneliness is related to poor subjective health (Cornwell & Waite, 2009; Havens, et al., 2004), multiple chronic illnesses (Theeke, 2010), impaired hearing (Victor et al., 2005), and poor self-reported functioning (Savikko et al., 2005). Loneliness can increase an individual’s risk of depression, anxiety (Golden, et al., 2009; MacLeod, et al., 2018; Tiikkainen & Heikkinen, 2005), and dementia (Luo et al., 2012; Wilson, et al., 2007). Loneliness is also a predictor of suicide among older adults aged 65 and older (Waern et al., 2003). Living in social isolation can also reduce self-esteem & confidence, social skills, and increase the risk of elder abuse (NICE: National Institute for the Care of the Elderly, 2015).
Experiences of social isolation are often complex and multifactorial, and poor health, chronic illnesses and disabilities can further marginalize older adults and make it harder to stay socially connected. There are many factors that can influence an older adult’s risk of social isolation including marital status, living situation, education, and financial status (Cudjoe, et al., 2020). Barriers such as lack of resources including transportation, and lack of appropriate opportunities for social connection can predict loneliness (Cohen–Mansfield & Parpura–Gill, 2007).
The peer-reviewed literature on interventions’ impacts on loneliness and isolation suggests that educational and psychosocial group interventions can help alleviate social isolation and loneliness in older adults (Cattan et al., 2005). Specifically, remote interventions that used technology to alleviate loneliness were found to be potentially effective within group formats, for older adults living both in community and institutions (Cohen–Mansfield & Perach, 2015). These interventions used multiple technological features including email programs, videoconference interaction with staff and family, as well as computer training for older adults (Cohen–Mansfield & Perach, 2015). However, there is a challenge in finding high quality evidence of impacts of loneliness and isolation interventions (Cattan et al., 2005; Cohen–Mansfield & Perach, 2015). Despite recent advances in technology usage, older adults may be reluctant to adopt and can be non-adherent in using online technology (Anderson & Perrin, 2017; Seifert et al., 2020). There are potential barriers to adoption that may explain the reluctance: concerns about privacy, access to the hardware and internet (Anderson & Perrin, 2017), socioeconomic, education, employment, and cohabitation status (Seifert et al., 2020; Hargittai & Dobransky, 2017). Age-related changes to physical and mental capability can be an impediment to technology usage, which many designers of hardware and software do not take into sufficient consideration (Hargittai & Dobransky, 2017). It is important then to select the right platform for remote programing that targets a diverse older adult population, while ensuring accessibility and efficient delivery of programming.
Telephone programming has been identified as a potential intervention for social isolation within Canada (Government of Canada, 2017). Evaluations of individual telephone programs have demonstrated some positive results (Newall & Menec, 2015) with the evidence in reviews indicating potential effectiveness (Stewart, et al., 2001) or inconclusive (Swindell & Mayhew, 1996). However, these evaluations have been limited to post-intervention questionnaires, based on participant self-reporting of perception of impact with limited sample sizes (ranging from 18 to 26). This purpose of this program evaluation was to add to the literature by utilizing validated loneliness and quality of life scales, pre-post intervention, to more clearly articulate if the services could be effective in improving participant outcomes with a larger sample.
Methods
This study was part of an evaluation process, which also provided insight into whether the program was reaching its target population, streamlining operations, and identifying gaps in service delivery and opportunities for improvement.
Program Background
In 2016, our organization was awarded a 3 year grant from the Government of Canada New Horizons for Seniors funding program, to develop a Seniors’ Centre Without Walls (SCWW) based out of primary care in Edmonton, Alberta, Canada. The concept of a SCWW was first conceived by the Dorot University in New York in 1989 (Dorot USA, 2021), and has since spread to other jurisdictions across North America. This program is also the only SCWW in North America based out of a healthcare organization, not a community social services organization, allowing for better referral pathways within primary care and more access to regular health speakers and programming, including behavioral health consultants, exercise specialists, nurses, dietitians, and respiratory therapists.
A SCWW is a telephone-based program offering a variety of interactive programming, free of charge to those aged 55 years and older. If a person requests to join and they are younger than 55, but are experiencing barriers to participating in traditional programming, they are not denied service. The goal is to support social connections for older adults who are homebound and/or isolated, through building an inclusive community atmosphere and ensuring the accessibility of social opportunities. Programming does not require any specialized equipment for participants other than a standard touch-tone or cellphone. The low-technological program provides an alternative to having older adults attend in-person programming at seniors’ centers. Free conference calls allow the older adults to join in small groups (7–10 participants on average), led by a facilitator. Participants included community-dwelling older adults and those living in institutions. Participants could self-refer, and referrals were accepted from caregivers, healthcare professionals, and community workers. The program was promoted through a local seniors’ newspaper and through local seniors-serving organizations’ newsletters. The project staff connected with incoming participants over the phone to provide additional understanding of the program and complete the registration. For each series, program schedules and supplementary materials based on program content were mailed out in participant packages. Participants chose which programs to join based on their availability and interests. Programming topics fell under three main categories: health and wellness information (e.g., chronic disease management, relaxation, exercise); recreational activities (e.g., BINGO, book clubs, museum talks, world news); and opportunities for skill building and learning (e.g., English practice, arts and culture presentation, home decluttering). The majority of programs had participatory elements with discussions, games, and activities to complete at home, alongside sessions with more traditional lecture style presentations and guest presenters. On average, the program offered two hour-long programs a day, Monday through Friday, at various times throughout the week.
Data Collection Procedure
Pre-Post data was collected through telephone surveys, between November 2016 and April 2019 (Figure 1). Participants joined the program (through both referral and self-enrollment) on a continuous basis and completed intake over the telephone with SCWW program staff to collect demographic information, risk factors of isolation, and initial responses to the validated scales. Our study excluded participants who were unable to give verbal responses to the required questions in English. The organization hired an evaluation assistant to act independently from the program staff and to complete follow-up with participants 6 months after entry into the program. Participants were invited to complete the telephone survey and were given the right to refuse any questions they did not want to answer or to opt out of the survey entirely.
Data Collection Instruments
Demographic information was collected through the intake survey including the participant’s age, gender, marital status, living arrangement, monthly income, caregiving status, primary language, general health, and vision or hearing problems. Additionally, participants were asked about their contact with friends/family, what if anything prevented them from social participation, and whether they have computer or internet access.
Participants completed the three-item version of the Revised University of California Los Angeles (UCLA) loneliness scale (Hughes et al., 2004), which enquires about frequency of feeling left out, isolated, and lacking companionship. Each question is rated on a 3-point scale: 1 = Hardly Ever; 2 = Some of the Time; 3 = Often. The scores for each individual question are combined to give a possible range of scores from 3 to 9, with higher values indicate greater loneliness. UCLA loneliness scale can be reported by grouping people who score 3–5 as “not lonely” and people with the score 6–9 as “lonely.”
Participants also completed the CASP-12 tool, based on 12 items, which assess four theoretically derived dimensions of Quality of Life (QoL) in older adults: control, autonomy, self-realization, and pleasure (Higgs et al., 2003). The CASP-12 tool is used to measure the psychosocial constructs of quality of life. The items are presented as questions or statements and are assessed on a 4-point Likert scale (“often,” “sometimes,” “rarely,” “never”). This outcome was analyzed as a continuous variable (score range of 12–48), with lower scores associated with poorer QoL (Borrat–Besson et al., 2015; Palgi et al., 2015).
The final validated tool completed was the EQ-5D-5L, a survey assessing five health dimensions with varying levels of severity and overall health visual analog scale (VAS) (EuroQol Research Foundation, 2020). The five dimensions include mobility, self-care, usual activities, pain or discomfort, and anxiety/depression. The varying levels of severity range from one to five, where one represents having no problems and five represents extreme problems. The EQ-5D-5L VAS has respondents indicate their current health status by choosing a number from 0 (worst imaginable health state) to 100 (best imaginable health state). An EQ-5D-5L Index score is calculated from responses to questions in all five domains and assessed based on the Canadian scoring algorithm range from −0.148 to 0.949. Higher scores indicated better health-related quality of life, and scores < 0 indicating a health state “worse than dead,” scores = 0 “same as dead,” and scores > 0 “better than dead” (McClure, et al., 2017).
Given the large variation in average monthly attendance (between 1–14 visits, average three visits per month), participants were classified by their average level of participation and calculated using participant attendance records. Low Users attended less than 3 times in 3 months, Moderate Users attended between three but less than 12 times in 3 months, and High Users attended at least 12 times during 3 months time period.
Statistical Analysis Methods
Data was analyzed in SPSS 24 (IBM Corporation). Descriptive statistics were used to characterize the participants. Wilcoxon Signed Rank Test and repeated Measures ANOVA were conducted to determine whether there were statistically significant group differences pre-post program. Mann–Whitney test were performed for group comparisons and paired Chi square test were performed for association testing. p-values below 0.05 were considered to be statistically significant.
Results
Demographics of Participants at Baseline by User Level.

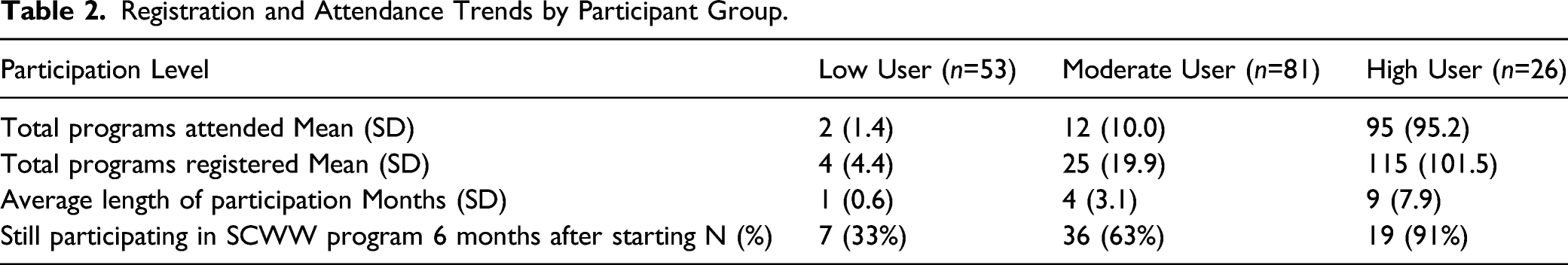
Registration and Attendance Trends by Participant Group.
UCLA Loneliness Scale
One-third (33%) of the participants reported improvement on the total UCLA loneliness score. This improvement in the total UCLA loneliness score was statistically significant for High Users of the program (Figure 2). Overall, participants reported a reduction in their feelings of isolation between baseline and follow-up measurements (2.1 vs. 1.9; p < 0.05). Participant retention flowchart
CASP—12
Participants reported less concerns than at baseline, with 36% of the participants showing improvement in the CASP-12 scores at follow-up. There was no change to nine of the domains, however, there was statistically significant improvement (p < 0.05) in the participants’ attitude towards their self-realization (Q: I feel left out of things) and towards their energy levels (Q: I feel full of energy these days). There was statistically significant decline (p < 0.05) in the participants’ attitude towards their finances (Q: I do not have enough money to do the things I want to do) Figure 3. Overall UCLA loneliness score by User Level (lower score—least lonely)
EQ-5D-5L
Comparison of EQ-5D-5L Scores.

Overall, 39% of participants reported improvement on at least one EQ-5D-5L scale. The highest improvement was on the Anxiety/Depression scale (Figure 4) and this change was statistically significant (2.36 vs. 2.05, p<0.05). Half of the participants reported improvement in EQ-5D-5L Index scores and 35% reported improvement in EQ-5D-5L VAS scores. There were no differences between different levels of participant engagement. Changes in EQ-5D-5L Index and VAS scores were not statistically significant. There was a trend for improvement in EQ-5D-5L Index score (0.6 vs. 0.64, p = 0.06) which may be clinical significant, as it meets the established minimal clinical important differences of 0.04 points for the EQ-5D Index (McClure, et al., 2017).
Discussion
At the beginning of this project, social isolation among older adults was a major concern for older adults. The need for social distancing during COVID-19 has exacerbated this problem, as almost all older adults regardless of living situation have experienced reduced social connections. Our participants indicated a greater degree of loneliness at the baseline and follow-up measurements, compared to literature rates (Luo et al., 2012). Average values for UCLA reported by ELSA Study was 4.06 ± 1.47 (Steptoe et al., 2013), while the SHARE study reported 4.29 (Luo et al., 2012). Our participants indicated lower quality of life as measured by CASP-12, compared to literature rates (Ateca-Amestoy & Ugidos, 2013) as well as higher than average health and environmental concerns. This data would suggest that the program is reaching its intended population of isolated older adults, experiencing health, mobility, and other challenges.
Previous evaluations favored more qualitative responses, focusing on the satisfaction with the program and perceived impacts (Newall & Menec, 2015; Stewart, et al., 2001). Most reported that participating older adults self-reported feeling more connected and less lonely after participation (Newall & Menec, 2015; Stewart, et al., 2001). Both studies identified emotional support from the telephone groups was a significant benefit of the intervention, which was reinforced by our participants’ comments where many shared they had made strong and meaningful relationships with the SCWW staff and made new friends on the program, with a number of participants referred to SCWW as their “only family.”
The results of our evaluation suggests a SCWW could reduce feelings of isolation as reported on the UCLA loneliness scale and anxiety/depression as reported on the EQ-5D-5L. Our evaluation also indicates that participation in SCWW programming can have a statistically significant improvement on feelings of self-realization and energy levels. While not statistically significant, there was a trend post-intervention for improvement on the EQ-5D-5L Index score, lower loneliness scores on the UCLA scale and for reporting fewer concerns on the CASP-12, which might still have clinical importance, and provide useful direction for intervention (Miller, 2007). In addition, the impact of the program can vary depending on the engagement level. High Users as a group reported the highest improvement at follow-up measurement, in feelings of connection and total UCLA loneliness score.
Limitations of the study
As there were participants lost to follow-up, we cannot make conclusions that the program was effective for every participant. While we tried to identify the reason why participants were lost to follow-up, detailed in Figure 1, we did see more lost to follow-up in the low participant category, potentially indicating an overall ineffectiveness of the program for these participants. Our participants were also predominately female and preventing us from comparing effectiveness of program by gender, though comparable proportions where reported in other evaluations of similar programs (Newall & Menec, 2015; Swindell & Mayhew, 1996; Stewart, et al., 2001). Whether this program is more acceptable and effective with female participants than males should be explored future evaluations. CASP-12 Baseline vs. Follow-up Participant Responses EQ-5D-5L score change by Dimensions.

This is a prospective study design—a pre/post evaluation designed to monitor participant changes over time. Supplementing this study with a control group (participants of similar demographics not enrolled in the SCWW program) would allow for more reliable comparison of the impact however was not appropriate, as it would involve identifying but not providing support for isolated older adults. Another limitation would be self-selection bias, as we did not assign individuals to levels of use, rather observed their participation patterns and impacts. It is possible that those who were most likely to benefit from the program self-selected into a higher use group. There was a higher representation of English as primary language speakers in the Moderate and High users groups. English language proficiency was not objectively measured by this evaluation and the impact of programming in other languages should be explored in the future.
Conclusions
The SCWW model could be a tool to help improve the wellbeing of isolated and homebound older adults by connecting them to a community, utilizing alternative technology to access the programs and services. It is important to recognize that many older adults do not have regular access to the internet or other web-based technology. Seniors-serving organizations should explore low-technology options to expand their offerings when trying to reduce the impacts of social isolation.
Footnotes
Acknowledgments
Thank you to Sandra Gad and Gayle Harper for their assistance on this project.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported in part by the Government of Canada’s New Horizons for Seniors’ grant (project number 1364716) and supported by the Edmonton Southside Primary Care Network.
