Abstract
This aims to provide an understanding of the spread of pneumonia through analysis of the interaction between infected and potentially infected. Data from 2010 to 2018 on Pneumonia morbidity among older persons age 65 and above was extracted from the Department of Health Field Health Service Information System (FHSIS) annual reports. The data were used to represent the cumulative adopters by fitting them to the Bass diffusion model using the Bass Forecasting Spreadsheet. The number of new adopters was graphed to forecast the diffusion of Pneumonia. The number of cases is expected to increase. The adoption rate in 2024 will be around 45% of the current population. Morbidity of pneumonia is expected to peak in the year 2200, 190 years after the first data. The use of the model provided an insight into the cumulative nature of pneumonia infection due to the interaction between infected and the potentially infected.
Introduction
Infection due to Streptococcus pneumoniae, the pneumococcus, remains a major source of illness in older persons. Globally, it remains the most significant pathogen in respiratory infection deaths (Van Buynder & Booy, 2018). Each year, pneumococcal disease causes death in a large number of adults. Thousands more end up in the hospital because of pneumococcal disease. It can cause severe infections of the lungs (pneumonia), bloodstream (bacteremia), and lining of the brain and spinal cord (meningitis) (Center for Disease Control and Prevention, 2018).
In addition, with advancing age and inevitable development of comorbidities, viruses may also cause serious illness and pneumonia (Falsey & Walsh, 2006). Although acute respiratory infection rates steadily decrease with advancing age, rates of hospitalization and death increase substantially in persons aged over 60 years (Falsey & Walsh, 2006). Multiple factors, such as declines in respiratory and immune function, likely contribute to increased morbidity (Pasdaran et al., 2016). Immune dysregulation and waning cellular immune function may impair viral clearance, allowing spread of the virus to lower airways, with increased inflammation (Falsey & Walsh, 2006). Studies of community-acquired pneumonia in adults indicate a viral etiology, with influenza virus being the most common virus. Although distinguishing viral from bacterial pneumonia is difficult on clinical grounds (Falsey & Walsh, 2006).
Pneumonia is a serious infection that occurs when a pathogen’s virulence overcomes a person’s host defenses. Aging is associated with general deterioration of organ function in a way that dictates not only an individual’s risk of developing pneumonia, but also clinical manifestations and outcomes. In addition to increased complexity of clinical presentation and more rapid progression of disease, older patients are at higher risk to have pneumonia owing to resistant organisms, and therefore empiric as well as definitive treatment can be challenging. Furthermore, the incidence of pneumonia increases with age, as does the impact of pneumonia on morbidity and mortality. Mortality rates for pneumonia in older adults are high and have not decreased in the last decade (Henig & Kaye, 2017).
It is then necessary to provide an understanding of the spread of pneumonia through analysis of the interaction between infected and the potentially infected. Network models of epidemic spreading have rationalized the understanding of how diseases propagate through a mobile interactome like the human population (Nicolaides et al., 2012). The Bass diffusion model, the most common mathematical representation of diffusive adoption will be used in this study. It describes the number of new adopters or new cases per unit time by the additive effects of external and internal forces (Godman et al., 2016), which may be useful when examining the factors contributing to an adoption rate. It is also the aim of this study to provide basis for the decisions related to the program implementation thereby improving disease prevention efforts in older persons (Dunn et al., 2012).
Methods
A 10-year data, from 2010 to 2018, on morbidity on Pneumonia among older persons age 65 and above was extracted from the Department of Health—Philippines Field Health Service Information System (FHSIS) annual reports, publicly accessible on the website of the department. These are officially diagnosed and reported cases To get the total number of older persons in the country with pneumonia which was 239,125 cases for ten years, data segregated according to sex (male and female) and age group (65–69 years old and 70 years old and above) were merged. The data were used to represent the cumulative adopters by fitting them to the Bass diffusion model using the Bass Forecasting Spreadsheet. The number of new adopters was graphed to forecast the diffusion of Pneumonia in the coming years. Another graph on the cumulative diffusion was also generated. The analysis of the data was then based on these graphs, generating insights and conjectures.
Results
The Pneumonia Morbidity from 2010 to 2018 was fitted into the Bass diffusion model. The change in the morbidity conformed to the pattern of diffusive adoption that appears to be similar with other infectious diseases.
Figure 1 reflects that the number of cases will increase throughout the years. It predicts that the adoption rate in 2024 will be around 45% of the current population. Notably, in 2016, there is a sharp increase in the morbidity which can be attributed to the vaccination scare. An intensive campaign was done by the government to curb the very high morbidity. Even so, vaccination rates remain low. Thus, making older persons vulnerable to pneumonia infection.

New adapters.
Figure 2 shows that morbidity of pneumonia is expected to peak in the year 2200, 190 years after the first data or almost two centuries after. This is reflective of the kind of pathogen causing the disease. Even though efforts to control its existence will be made through vaccination, it will continue to exist due to the characteristic of the microorganism harboring the disease. The projected increase in older population will play a role in this scenario. With the number constantly increasing, their interaction with each other is most likely to happen, causing the easier spread of the microorganisms.

Bass Model.
Figure 3 presents the difference between the Bass Model and the actual infected cases. There is a standard error of prediction of 0.04888763 which suggests a close resemblance between the two. The Bass Model can then predict the probable cases in the future close to the actual data. Similarly, a model using birth, susceptibility, infection, and death; a modification of the susceptible infected removal (SIR) model, can be used to produce numbers that are closer to real data. It is for this reason that studying infectious disease usually uses such a mathematical model.

Fit of the Bass Model to the actual infected cases.
Discussion
Infectious diseases have for centuries ranked with wars and famine as major challenges to human progress and survival. They remain among the leading causes of death and disability worldwide. Against a constant background of established infections, epidemics of new and old infectious diseases periodically emerge, greatly magnifying the global burden of infections. Studies of these emerging infections reveal the evolutionary properties of pathogenic microorganisms and the dynamic relationships between microorganisms, their hosts and the environment (Morens et al., 2004).
Contagion generally refers to how infection spreads between the individuals in networks within an environment. The contagious dynamics can be thoroughly inspected utilizing mathematical models of contagious processes which can then be utilized to acquire exact proportions of anticipated predominance of infectious diseases. Many models do not capture the probabilistic nature of contagion, or the asymmetry intrinsic in traditional infectious diseases, where the infected state spreads through social contagion whereas the non-infected state does not (Hill, 2010).
The cumulative nature of the Bass Diffusion model tends to disregard the addition of new members of the population and the reduction due to deaths, seemingly moving towards full saturation. On the other hand, the compartmental nature of the modified SIR model can be used to explain the change in the number of people needing medical attention during an epidemic (Kuddus et al., 2014). Economic models for the diffusion of innovations, as reflected in the early works of Bass, do consider “automatic” infection. People move from “susceptible” (non-adopter) to an infected (adopter) state by the additive effects of external and internal forces. In any case, these models do not take into account recovery; in light of the fact that the innovation adoptions are thought to be permanent changes, individuals never move back to a susceptible state. This results in the whole populace turning out to be adopters at equilibrium. This does not reflect the dynamics of many infectious disease phenomena just like pneumonia which may be repeatedly acquired and lost. Through a balance of infection and recovery, a steady-state with multiple states of individuals coexisting can be reached (Hill, 2010).
In light of an increased risk of pneumococcal disease with advancing age, the costs associated with infection, and the rising rates of drug resistance, vaccination has emerged as a public health priority (Artz et al., 2003). Despite a century of often successful prevention and control efforts, infectious diseases remain an important global problem in public health, causing over 13 million deaths each year. Changes in society, technology and the microorganisms themselves are contributing to the emergence of new diseases, the re-emergence of diseases once controlled, and to the development of antimicrobial resistance (Cohen, 2000).
Vaccination is one of the effective ways to prevent pneumonia (Ellen, 2017). Clinical practice guidelines have recommended routine influenza and pneumococcal vaccinations for older persons. Quality improvement interventions, especially those that assign vaccination responsibilities to nonphysician personnel or that activate patients through personal contact, can modestly improve vaccination rates in community-dwelling adults. To meet national policy targets, more-potent interventions should be developed and evaluated (Lau et al., 2012). The effective control of infectious diseases in the new millennium will require effective public health infrastructures that will rapidly recognize and respond to them and will prevent emerging problems (Cohen, 2000).
Conclusion
The use of Bass diffusion model provided an insight on the cumulative nature of pneumonia infection due to the interaction between infected and the potentially infected. This would point out to the idea that the whole population specified would eventually be infected and reaching saturation. This nature of the model does not reflect the dynamics of many infectious disease phenomena just like pneumonia which may be repeatedly acquired and lost. Through a balance of infection and recovery, a steady-state with multiple states of individuals coexisting can be reached.
Recommendation
It is recommended to conduct a study using actual tracking of the network of the spread of disease from the infected to the potentially infected. To account for the cases in relation to the population changes per year, the following model (Figure 4) is hereby recommended for use in future studies:
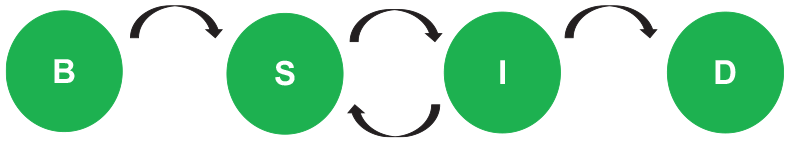
BSID Model.
Total Population is represented with:

Birth is:

Change in Susceptibility is:

Change in Infected is:

Change in Death is:

and, expected population is:
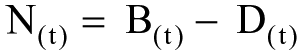
where:
Footnotes
Declaration of Conflicting Interests
The author declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author received no financial support for the research, authorship, and/or publication of this article.
