Abstract
The purpose of this investigation was to determine the differences between gender, physical activity level, and balance in an older adult population. A secondary purpose was to examine the relationship between pedometer-determined ambulatory activity and balance. Forty-six older adults aged 73.7 ± 6.2 years participated in the study. Participants completed the Fullerton Advanced Balance (FAB) Scale and completed a 2-week daily step recording to determine average steps taken per day. Low-level activity participants (<5,000 steps/day) were significantly different from the high-level activity participants (>7,500 steps/day) in weight, age, and the number of medications reported. Males performed better than females on the two-footed jump test and reactive postural test FAB assessments. High-level activity participants performed significantly better than low-level activity participants on all FAB assessments except stand with feet together and eyes closed, reach forward to object, and walk with head turns.
Everyday tasks for an older adult can become dangerous and daunting when their balance has become instable. Diminished postural control increases the likelihood of falling, which can cause debilitating injury and a loss of independence, not to mention high health care costs (Bohl et al., 2010; Myers, Young, & Langlois, 1996). Balance and postural control often become a problem with aging due to both natural physiological losses and a decrease in activity level (Myers et al., 1996).
Aging is associated with a decrease in physical activity levels in both males and females. Only 39.6% of American adults aged 75 years and above reported participating in some leisure-time physical activity compared with 66.3% of younger American adults (Adams & Schoenborn, 2010). Physical inactivity may amplify physiological losses to balance and result in a lower quality of life for those who are not able to maintain adequate health and independence (Myers et al., 1996). With a loss of balance and/or balance confidence, older adults often decrease levels of activity further leading to a cycle of instability (Chandler, Duncan, Sanders, & Studenski, 1996).
Research has demonstrated that regular physical activity can improve static and dynamic balance (Karinkanta, Heinonen, Sievänen, Uusi-Rasi, & Kannus, 2005; Melzer, Benjuya, & Kaplanski, 2003). Melzer et al. (2003) found that older adults who participated in 3 days of physical activity in the form of walking had better static balance than those who were less active or sedentary, whereas Cyarto, Brown, Marshall, and Trost (2008) found no improvement in dynamic balance following a 20-week walking program. These studies used walking as a mode of activity to determine changes in dynamic balance, but they did not take into account total daily physical activity of the participants. In a cross-sectional study examining factors associated with dynamic balance, Karinkanta et al. (2005) subjectively measured physical activity levels and walking by a questionnaire and found that both are related to an increase in dynamic balance. However, self-reports of physical activity may not provide accurate estimates of total amounts of physical activity, and when an absolute measure of physical activity is needed, an objective measurement is more meaningful (Sallis & Saelens, 2000). Pedometers measure steps taken per day and have been shown to correlate well with observed physical activity levels and reflect ambulatory activity levels especially when walking is the most common type of physical activity being measured (Berlin, Storti, & Brach, 2006; Tudor-Locke, Williams, Reis, & Pluto, 2002).
Therefore, more research is needed to investigate whether physical activity, measured by steps per day, is related to an increase in balance. Walking is both cost-effective and easily accessible for the older adult population, yet it remains unclear whether the amount of steps taken per day is related to a high level of static and/or dynamic balance to help with activities of daily living.
The purpose of this investigation was to determine the gender differences in physical activity level (pedometer-determined ambulatory activity from steps per day) and dynamic balance variables in an older adult population. A secondary purpose was to examine the relationship between pedometer-determined ambulatory activity (steps/day) and balance variables.
Materials and Methods
Participants
The participants (N = 46) in this study were both males (n = 19) and females (n = 27) within the age range of 65 to 90 years (M age = 73.7 ± 6.2 years). Participants were accepted if they were ambulatory either independently or with the use of a walking assistance device such as a cane or walker. All participants were community living.
Measurement Procedures
The participants received a written and verbal explanation of the study and then gave their written informed consent prior to data collection. Each participant completed a health history questionnaire to establish their risk stratification using the American College of Sports Medicine risk stratification (Thompson, Gordon, & Pescatello, 2010). Those who were identified as low or moderate risk by the health history questionnaire were included into the study. Participants identified as high risk due to controlled diabetes mellitus (Types 1 and 2) or controlled asthma were asked to obtain medical clearance to be included in the study. Anyone identified as high risk for any other reason was excluded from the study. Participants also reported the number of prescribed medications that they were currently taking on the health history questionnaire. This investigation was approved by an institutional review board.
The Fullerton Advanced Balance (FAB) Scale consists of 10 items which were administered in the same order for each participant. Each participant was given an explanation and demonstration of each exercise before being allowed to practice any tests the participant wished to practice. After each item was performed, a score was given from 0 to 4 based on FAB criterion (Rose, 2003). Height and weight for each participant were also obtained after balance testing.
Following the balance assessment, each participant received a pedometer for daily step recording along with verbal and written instructions for the pedometer use. Each pedometer was calibrated by the researcher according to manufacturer’s instructions. Participants were directed to attach the pedometer securely and vertical to the waistband or belt, close to the center of the body. They were directed to restart the step count upon rising each day by pressing the “reset” button. Each participant was directed to record the number of steps at the end of the day on the daily step recording sheet provided by the researcher. Participants received phone calls every other day from the researcher to remind them to record their daily steps and to ensure the pedometer was worn each day. At the completion of 2 weeks, each participant returned the daily step recording sheet to the researcher for analysis.
Statistical Analysis
Descriptive statistics were used for age, height, weight, and the number of reported prescribed medications taken each day by the participant. One-way ANOVAs were performed to determine significant differences between gender and daily steps, FAB assessments, and demographic factors. Additional one-way ANOVAs were performed to determine significant differences between the levels of physical activity of steps per day (low, moderate, and high) and FAB assessments and demographic factors. A Spearman rank correlational analysis was used to determine the relationship between the number of steps taken per day to each individual item on the FAB assessments, and demographic factors. Significance for all analyses was set at a probability level of p < .05.
Results
Participants
A total of 49 older adults (age = 73.7 ± 6.2 years) passed the initial screening and were not ruled out due to risk stratification. Three participants were excluded from data analysis for the following reasons: one participant dropped out after completing balance testing with the FAB Scale due to inadequate time to participate, and two participants did not return the daily step recording sheet and data for their steps per day (see Table 1 for demographic information).
Descriptive Characteristics.

Note. BMI = body mass index.
Indicates a significant difference (p ≤ .05) between males and females.
Gender and FAB Performance
All participants performed the FAB assessment prior to daily step recording. Males performed significantly higher on the two-footed jump for distance and the reactive postural control (see Table 2 for the gender and FAB performance results).
Gender and FAB Performance.

Note. FAB = Fullerton Advanced Balance.
Indicates a significant difference (p ≤ .05) between males and females.
Activity Level Categories’ Descriptive Characteristics
Participants were classified into one of three physical activity level categories based on the average number of steps taken per day adapted from preliminary pedometer indices for public health (Tudor-Locke & Bassett, 2004). Participants who completed an average of fewer than 5,000 steps per day were classified as a low level. Participants who completed an average of between 5,001 and 7,499 steps per day were classified as a moderate level. Participants who completed an average of 7,500 steps per day or greater were classified as high level.
No significant differences were found between moderate and high physical activity levels in descriptive statistics (height, weight, age, the number of medications, or steps per day). Significant differences were found between the age of the low-level group and high-level group participants. The low-level participants were significantly different from both moderate-level and high-level participants in both weight and the number of medications reported (see Table 3).
Activity Level Descriptive Characteristics.

Indicates a significant difference between low group and moderate group. *Indicates a significant difference between low group and high group.
FAB Performance and Activity Level Categories
There were no significant differences in FAB performance between moderate physical activity level participants and high physical activity level participants. There were, however, seven significant differences between low-level participants and high-level participants: (a) turn 360° in right and left directions; (b) step up, onto, and over a 6-inch bench; (c) tandem walk; (d) stand on one leg; (e) stand on foam with eyes closed; (f) two-footed jump for distance; and (g) reactive postural control. There were significant differences between low-level participants and moderate-level participants on two FAB assessments: tandem walk and two-footed jump for distance (see Table 4).
FAB Performance and Activity Level.

Note. FAB = Fullerton Advanced Balance.
Indicates a significant difference between low group and moderate group. *Indicates a significant difference between low group and high group.
Correlations
A Spearman rank correlation was performed on activity levels and performance on FAB assessments. Activity level was significantly correlated to FAB turn in a full circle, step up and over, tandem walk, stand on one leg, stand on foam with eyes closed, two-footed jump, and reactive postural test (see Table 5).
Correlations Between Activity Level and FAB.
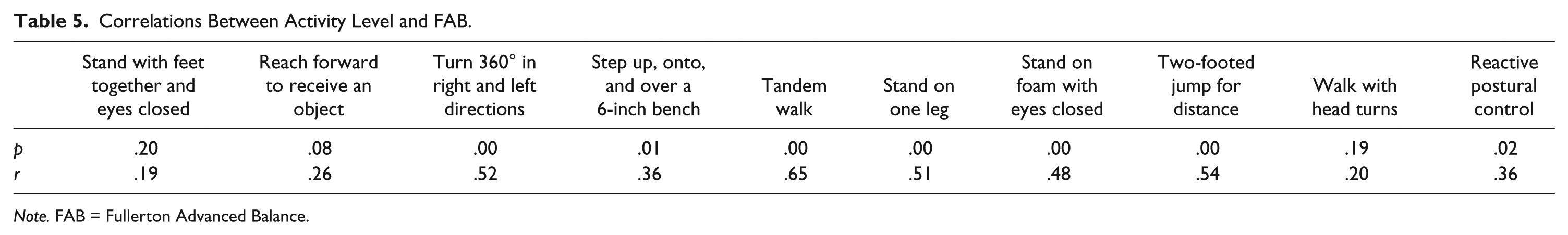
Note. FAB = Fullerton Advanced Balance.
Discussion
The purpose of this investigation was to determine the gender differences in physical activity level (pedometer-determined ambulatory activity from steps per day) and balance variables in an older adult population. A secondary purpose was to examine the relationship between pedometer-determined ambulatory activity (steps/day) and balance variables.
Previous research has found that men participate in more physical activity than women with a greater percentage of women reporting little or no recreational physical activity. Furthermore, more men report achieving the recommended amount of weekly physical activity than women, regardless of disease presence (Ashe, Miller, Eng, & Noreau, 2009; van den Hombergh, Schouten, van Staveren, van Amelsvoort, & Kok, 1995). The males in this study reported higher than average steps per day than females, although the difference was not significant. These results are consistent with other research that has reported males take more steps per day than females (Al, Fatima, Steven, & Vallance, 2016; Aoyagi & Shephard, 2009; Chan, Spangler, Valcour, & Tudor-Locke, 2003; Gonzales, Shephard, & Dubey, 2015; Togo et al., 2008; Tudor-Locke, Hart, & Washington, 2009).
In this study, males performed better than females on the two-footed jump test and reactive postural test FAB assessments. Other studies have shown that older women have poorer balance performance than males, especially in activities that require muscular strength and postural control (Vereeck, Wuyts, Truijen, & Van de Heyning, 2008). Successful completion of the two-footed jump and reactive postural test requires lower body muscular strength, power, and motor coordination. Reduced lower extremity muscular power has also been associated with lesser functional status in older women (Foldvari et al., 2000). Samuel and Rowe (2009) reported that 80-year-olds had approximately 20% lower muscle strength when compared with 60-year-olds and also reported that women produced significantly lower knee and hip strength measures when compared with males.
Low-level activity participants (<5,000 steps/day) were significantly different from the high-level activity participants (>7,500 steps/day) in weight, body mass index (BMI), age, and the number of medications reported. These findings are consistent with other research. The lower BMI of high-level activity participants compares with previous research that reported a lower BMI was associated with more steps per day (Chan et al., 2003; Strath et al., 2011; Tudor-Locke et al., 2001). In this study, low-level physical activity participants reported a greater use of medications; these results are similar to research in which physical inactivity in women was associated with an increased use of several prescription medications, such as cardiovascular drugs and alimentary tract and metabolism drugs (Milder, Klungel, Mantel-Teeuwisse, Verschuren, & Bemelmans, 2010).
Low-level activity participants performed significantly worse than the high-level activity participants on all FAB assessments except stand with feet together and eyes closed, reach forward to object, and walk with head turns. Poor performance on turn in a full circle, step up and over, tandem walk, stand on one leg, two-footed jump, and reactive postural tests is suggestive of poor dynamic center of gravity control and decreased input or use from either vestibular or visual sensory cues. The results of this study are consistent with previous research by Melzer et al. (2003) who found that non-walkers required more effort to keep the center of pressure within stability limits to maintain postural control. Karinkanta et al. (2005) also found that self-reported walking time improved dynamic balance variables measured using a step-on-a-stair, similar to step up and over.
Sedentary older adults have been shown to have difficulty in discriminating sensory conflicting situations, and these problems have been suggested to be a result of how the cues are integrated into the postural control system. High performance on dynamic balance assessments in this study agrees with Prioli, Júnior, and Barela (2005) who found that physically active older adults were better able to process information from the sensory systems and make appropriate muscular responses to maintain balance. Messier et al. (2000) used a standing balance with eyes closed test to find that an aerobic walking program can limit the rate of decline of balance performance when visual inputs are absent and vestibular and somatosensory input must be used.
Walk with head turns requires the participant to walk to a designated cadence while turning their head at that same cadence. Poor performance on this assessment suggests possible vestibular impairment and poor use of vision which both would not be moderated by a regular walking routine. Improvements in postural control seem to be training specific; thus, the walking with head turns produces a postural challenge that may be unfamiliar to even highly active older adults (Desai, Goodman, Kapadia, Shay, & Szturm, 2010) which is in agreement with our results.
The finding in this study is contrary to Melzer et al. (2003) who found that regular walking may have the potential to improve static postural stability in older adults and Messier et al. (2000) who demonstrated that walking programs improved performance in a standing balance task with eyes closed. Our findings did not show any significant differences in standing balance with eyes closed between activity groups.
Ten thousand steps per day have been popularized in the media as the number that will elicit health benefits, but according to this study, the relationship between steps per day and balance variables reveals that habitually taking more than 5,000 steps per day is related to better balance performance. Dynamic balance control uses sensory information to appropriately determine a motor program to maintain postural stability while the body is in motion. All FAB assessments that were significantly correlated to steps per day assess dynamic balance variables, with the exception of stand on one leg which is a static balance assessment. These results are in agreement with Desai et al. (2010) who found that physical activity levels were related to dynamic balance measures. This study used subjective means of assessing physical activity, whereas our study used an objective assessment.
There was a positive but non-significant correlation found between ambulatory daily steps taken and stand with feet together and eyes closed. This is a static balance assessment that removes visual sensory input during quiet standing, thus challenging the somatosensory and vestibular postural control. These findings agree with research by Kuh, Bassey, Butterworth, Hardy, and Wadsworth (2005) who found that low levels of physical activity, measured by questionnaire, have been shown to be associated with poor balance performance in both older men and women when assessed using a timed one-legged standing balance time.
In conclusion, this study found that males performed significantly better than females on two-footed jump test and reactive postural test FAB assessments that required both postural control and lower extremity muscular strength. Greater amounts of physical activity by means of steps per day were associated with improved performance on seven of the 10 balance assessments, most of which required dynamic balance. However, no significant relationship was found between steps per day and stand with feet together and eyes closed, reach forward to object, and walk with head turns. As the number of older adults in the United States increases, finding cost-effective, evidence-based methods for maintaining dynamic balance, functional independence, and quality of life in this population is crucial.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
