Abstract
Objective
Diabetes mellitus is an important chronic disease that is prevalent around the world. Different countries and diverse cultures use varying approaches to dealing with this chronic condition. Also, with the advancement of computation and automated decision-making, many tools and technologies are now available to patients suffering from this disease. In this work, the investigators attempt to analyze approaches taken towards managing this illness in India and the United States.
Methods
In this work, the investigators have used available literature and data to compare the use of artificial intelligence in diabetes management.
Findings
The article provides key insights to comparison of diabetes management in terms of the nature of the healthcare system, availability, electronic health records, cultural factors, data privacy, affordability, and other important variables. Interestingly, variables such as quality of electronic health records, and cultural factors are key impediments in implementing an efficiency-driven management system for dealing with this chronic disease.
Conclusion
The article adds to the body of knowledge associated with the management of this disease, establishing a critical need for using artificial intelligence in diabetes care management.
Keywords
Introduction
Diabetes mellitus (DM) is a chronic health condition that impacts millions of individuals globally, necessitating vigilant oversight and proactive management to mitigate potential complications and enhance patient well-being. Within the United States (US), recent data from the Centers for Disease Control and Prevention (CDC) 1 shows the large prevalence of DM, with approximately 11.6% of the population affected by this chronic disease in 2021. Alarmingly, a considerable portion of diabetic adults, accounting for 22.8%, remains undiagnosed, highlighting the urgent need for improved screening and detection efforts. Additionally, a substantial proportion of the adult population, approximately 38.0%, is estimated to have prediabetes, underscoring the importance of preventive measures and early intervention strategies to curb the progression of the disease. Among individuals aged 65 and older, nearly half (48.8%), are affected by DM, emphasizing the heightened susceptibility to this condition among older adults. Similarly, the situation in India mirrors the concerning trends observed in the US regarding DM prevalence and management. India ranks as the second most afflicted nation with DM globally. 2 As per the International Diabetes Federation (IDF) reports, the number of diagnosed DM cases in India surpassed 74 million in 2021, and with an expected increase to over 124 million by 2045. Between 2000 and 2019, DM was responsible for an increase of 3% in mortality. In addition, the mortality rate of individuals between the age of 30 and 70 also substantially increased within this period.
Although there is no complete cure, DM can be treated and managed, and its adverse effects can be prolonged or reduced by a healthy diet, physical activities, and regular screening and treatments. Therefore, developing early warning alarm systems, like personalized health monitoring, is essential.
India and the US face distinct challenges in managing DM due to contrasting healthcare infrastructures, cultural practices, and socioeconomic contexts. In both nations, there is a pressing need for more sophisticated automated tools to enhance screening, monitoring, and the development of personalized treatment plans for individuals with DM. Given the vast populations in both countries and the limitations in healthcare resources, leveraging advanced technologies such as artificial intelligence (AI) becomes imperative. Developing AI tools for DM management goes beyond merely early detection. AI's true potential lies in its ability to analyze vast amounts of patient data, including blood sugar levels, dietary habits, and physical activity patterns. This analysis allows AI to identify patterns and trends that may escape human observation. For instance, AI algorithms can learn to predict blood sugar spikes based on a patient's specific food intake and activity levels. This personalized approach empowers patients to make informed decisions about their diet and exercise routines, ultimately improving blood sugar control and reducing the risk of complications. 3 Furthermore, AI can play a crucial role in medication management. By analyzing a patient's medical history, current medications, and real-time health data, AI systems can recommend personalized insulin dosage adjustments or suggest alternative medications with fewer side effects. This reduces the risk of medication errors and ensures patients receive optimal treatment based on their unique needs. AI-powered tools can also provide continuous support and motivation to patients, reminding them to take medications, track their blood sugar levels, and adhere to healthy lifestyle choices. This ongoing support system can significantly improve patient engagement and self-management, leading to better long-term health outcomes. 4 By integrating AI into various aspects of healthcare delivery, including diagnostics, treatment optimization, and patient management, both India and the US can strive towards achieving better healthcare outcomes for individuals living with DM.
The primary objective of this study is to investigate the epidemiology of DM in both India and the US, analyzing factors such as prevalence, trends, and key contributors to the disease burden in both countries. Additionally, the study seeks to examine recent advancements in AI-based DM management systems implemented in both India and the US. By thoroughly examining the current state of these technologies, including their adoption rates, effectiveness, and limitations, this study aims to pinpoint challenges that may impede their widespread adoption and utilization within healthcare settings. Furthermore, the study anticipates future challenges by assessing the potential for further innovation, integration, and scalability of these systems to address evolving healthcare needs and tackle emerging challenges associated with DM care.
Diabetes: An Overview
DM is a disorder characterized by hyperglycemia (high blood glucose levels). 5 This is often a sign of uncontrolled DM, which can damage many body organs. DM is a chronic disease that occurs partly because the pancreas is unable to produce insulin—a hormone that regulates blood glucose levels—or the body may not correctly utilize the produced insulin. 6 Type 1 DM (T1DM) and Type 2 DM (T2DM) are the 2 main subtypes of DM. T1DM typically affects children or adolescents and arises from inadequate insulin secretion. Besides, T2DM usually affect middle-aged and older adults who have high blood sugar levels due to unhealthy lifestyle choices and dietary habits. Each type of DM has a different pathogenesis and requires different treatment strategies.7,8
Type 1 Diabetes Mellitus
T1DM is a chronic disorder and is also known as autoimmune DM. 9 It is caused by the loss of pancreatic β cells and, thereby, loss of insulin secretion. Although the onset of T1DM is about childhood or adolescence, the symptoms may develop at a later age. Although the reason behind T1DM is not completely understood, the disease may develop due to the obliteration of β cells by T cells. 9
Type 2 Diabetes Mellitus
T2DM is a chronic disease often observed in the onset of the adult age. 10 The prevalence of this metabolic disorder is steadily increasing all over the globe and is an epidemic in some countries due to unhealthy diets and living conditions. 10 T2DM is the dominant type of DM and accounts for 90% of the existing DM cases. 11
Gestational Diabetes
The condition called hyperglycemia detected during pregnancy is known as gestational diabetes. 11 Although it may occur at any stage of the pregnancy, it is expected to be observed from 13 weeks to 27 weeks. According to the American Diabetes Association (ADA), the adverse effect of gestational diabetes is about 7% in all pregnancies. Those who experience it are at a higher risk of developing T2DM in the future.
Symptoms of DM
The symptoms of DM are not so evident, especially in T2DM and gestational diabetes, whereas they are quick and heavy in the case of T1DM. 12 Common indicators of both T1DM and T2DM include heightened thirst, frequent urination, fatigue, nerve damage affecting sensation, and frequent mood fluctuations.
Key Complications Associated With DM
Individuals diagnosed with DM are at risk of developing numerous long-term complications that can impact various organs in the body. 13 These complications encompass severe cardiovascular and vascular issues known as macroangiopathy, which can result in conditions such as hypertension, artery narrowing, coronary artery disease, and strokes. Another significant complication is diabetic retinopathy, which involves damage to the blood vessels in the eyes, leading to a decline in vision and is a major cause of blindness in the Western world. Additionally, diabetic nephropathy may occur, leading to renal insufficiency and affecting kidney function. Diabetic neuropathy, on the other hand, presents as sensory disturbances, muscle atrophy, difficulties in mobility, and various symptoms such as tachycardia, orthostatic hypotension, urinary incontinence, and gastrointestinal issues, along with contributing to foot problems. Diabetic foot ulcers, characterized by lesions and complications in the lower extremities, including pain, sensory disorders, skin dryness, callus formation, wounds, ulcers, and infections, can also develop, with severe cases potentially leading to gangrene and requiring amputation.
Epidemiology of DM in India and the US
Based on the CDC report on DM from 2021, 1 approximately 38.4 million individuals of all age groups in the US were diagnosed with DM, roughly equating to 1 in every 10 people, with 1 in 5 unaware of their condition. The total medical costs and lost work and wages for those with diagnosed DM amounted to $413 billion. Adults with DM face a 60% higher risk of early death compared to those without the condition. While in India, an estimated 77 million individuals aged 18 years and above are afflicted with type 2 DM. CDC 14 provided the percentage of DM patients across the US. Anjana et al. 15 reported the prevalence of DM patients across different Indian states.
The study on DM prevalence in the US utilized data from the Behavioral Risk Factor Surveillance System (BRFSS) spanning from 2018 to 2022. It involved 1,867,575 surveys, with 259,476 individuals diagnosed with DM. Data for India were sourced from the Demographic and Health Surveys Program (DHS), a global effort offering detailed insights into population demographics, health, and nutritional trends from 2019 to 2021. This encompassed 715,888 surveys, revealing 12,106 individuals diagnosed with DM. Several statistics are illustrated in Figures 2 to 5. For each category, the percentage ratio of non-diabetic to diabetic patients is calculated and visualized through plotting. In both countries, the prevalence exhibits an upward trend with advancing age, as depicted in Figure 1. However, in India, DM tends to be more prevalent at a younger age when compared to the US. Furthermore, the data indicate a high correlation between the rise in body mass index (BMI) and the increased prevalence of DM, as evidenced by the findings presented in Figure 2. This trend holds true for both populations in the respective countries. Specifically, as BMI values escalate, there is a notable escalation in the prevalence of DM among individuals. This observation underscores the significant impact of BMI on DM prevalence, highlighting the importance of weight management and lifestyle factors in mitigating the risk of developing DM within populations across different demographic contexts. The dataset revealed striking differences in the prevalence of DM across various racial and ethnic groups within the US, contrasting with the relatively uniform prevalence rates observed among diverse ethnic groups in India. Notably, non-Hispanic Black and American Indian adults exhibited significantly higher prevalence rates of DM 16 when compared to their non-Hispanic Asian counterparts, as illustrated in Figure 3. This disparity suggests that ethnic factors play a crucial role in influencing DM prevalence within the US population. Moreover, socioeconomic factors, such as education disparities, were evident, with higher educated individuals having a lower prevalence of DM, as illustrated in Figure 4. This trend persisted consistently across both US and India, emphasizing the substantial impact of education on DM prevalence. These findings underscore the significance of addressing educational disparities in public health initiatives aimed at preventing and managing DM. By enhancing access to education and bolstering health literacy, endeavors can be undertaken to alleviate the burden of DM within populations and address disparities in health outcomes.

Categorized by age. (a) US statistics according to BRFSS (2018-2022). (b) Indian statistics according to DHS (2019-2021).
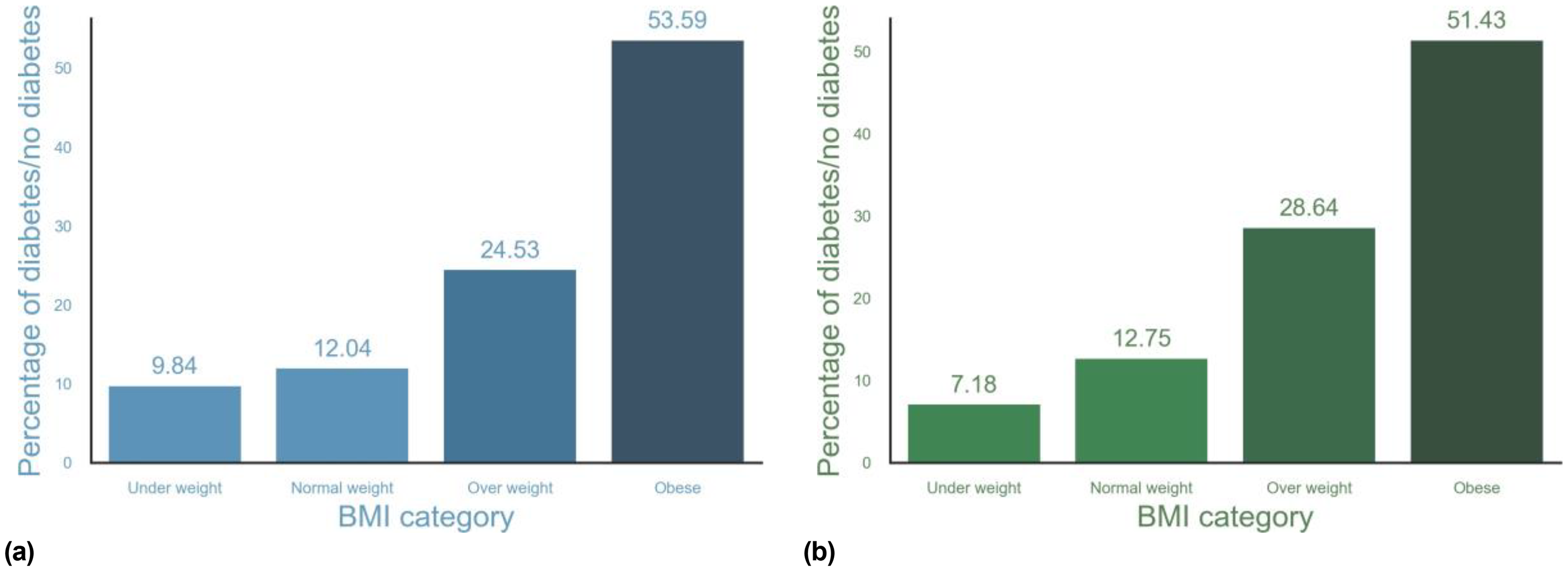
Categorized by BMI. (a) US statistics according to BRFSS (2018-2022). (b) Indian statistics according to DHS (2019-2021).

Categorized by ethnicity/race. (a) US statistics according to BRFSS (2018-2022). (b) Indian statistics according to DHS (2019-2021).
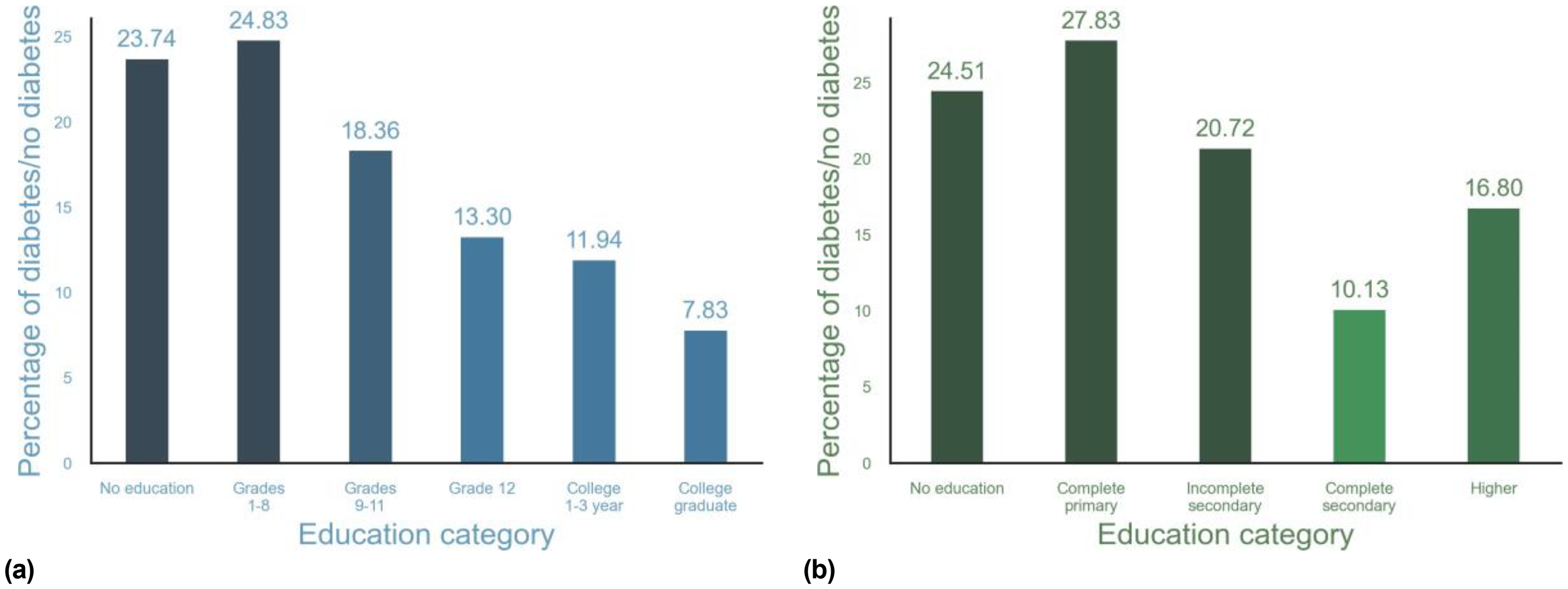
Categorized by education. (a) US statistics according to BRFSS (2018-2022). (b) Indian statistics according to DHS (2019-2021).
Approaches for Diabetes Care Management
The increasing occurrence of DM emphasizes the need to implement appropriate preventive strategies to tackle this challenge effectively. Utilizing AI can significantly enhance the ability to implement targeted interventions and preventive measures. AI-powered predictive analytics can aid in identifying individuals at elevated risk of developing DM by analyzing vast datasets and detecting patterns indicative of pre-diabetic conditions. Additionally, AI-driven health monitoring devices and mobile applications can empower individuals to track their health metrics in real time, enabling early detection of potential risk factors and facilitating timely intervention. Moreover, AI-enabled decision support systems can assist healthcare professionals in developing personalized prevention plans tailored to each patient's unique health profile and risk factors. These systems can analyze patient data, medical history, and lifestyle factors to generate evidence-based recommendations for lifestyle modifications, dietary adjustments, and targeted interventions. AI algorithms can also continuously learn and adapt based on feedback and outcomes, ensuring the ongoing optimization of preventive strategies. Furthermore, AI technology holds promise in revolutionizing population health management by enabling proactive screening programs, optimizing resource allocation, and predicting future disease complications. By leveraging AI for population-level risk assessment and stratification, healthcare organizations can prioritize preventive interventions in high-risk communities and allocate resources efficiently to achieve maximum impact. Integrating AI-driven approaches into DM prevention efforts can enhance our capacity to identify at-risk individuals, deliver personalized interventions, and optimize population health outcomes. By harnessing the power of AI, we can take proactive steps to mitigate the rising prevalence of DM and improve overall public health outcomes.
Predictive analytics driven by AI anticipate the progression of DM and its associated complications in patients. Various ML algorithms have been investigated to develop an automated predictive model aimed at estimating the likelihood of developing type 2 DM within the period of 1 to 5 years before its onset.25,26 These models utilize a broad spectrum of variables, encompassing factors such as age, gender, family history of DM, hypertension history, BMI, pre-diabetes HbA1c levels, triglyceride levels (TG), fasting blood sugar (FBS), systolic blood pressure (sBP), high-density lipoprotein (HDL), and low-density lipoprotein (LDL). These variables are employed in developing predictive models to examine the correlation between these variables and the likelihood of developing type 2 DM within different time frames. These models can identify patterns, correlations, and predictive markers that might not be apparent through traditional statistical methods. Additionally, they analyze longitudinal patient data to forecast future health paths and transitions, enabling to deploy timely interventions and customized treatment strategies.
The ADA recommends enhancing healthcare delivery at a systemic level, providing assistance for self-management and incorporating shared decision-making in the treatment of individuals with DM. 43 The continuous advancements in digitalization and DM-related technology have expanded the usefulness of tele-diabetology as a supplement to or substitute for traditional in-person consultations.44,45 Several surveys highlighted that telemedicine could effectively serve as a sustainable method of diabetic care.46,47,48,49,50,51,52 Additionally, numerous insurance companies cover telemedicine services, thus enhancing accessibility and affordability for individuals with DM. Furthermore, healthcare providers frequently integrate telemedicine platforms and remote monitoring tools into their EHRs to optimize patient data management and maintain seamless care continuity. A recent study emphasized the potential of virtual healthcare in aiding individuals with DM, particularly those dealing with obesity and T2D. 53 Telemedicine platforms powered by AI facilitate remote monitoring of diabetic patients’ health metrics, medication compliance, and lifestyle behaviors. 54 These platforms enable seamless, real-time communication between patients and healthcare providers, thereby enhancing accessibility to care and improving patient outcomes.
In the US, the market for automated insulin monitoring and automated insulin delivery (AID) systems has seen significant growth, with various devices such as insulin pumps equipped with continuous glucose monitors (CGMs) gaining popularity. Recently, the Food and Drug Administration (FDA) in the US has granted approval for AID systems, making them commercially accessible.63,64,65,66 Recent findings from clinical trials indicate improvements in glucose regulation and reductions in the burden of DM management through AI-based glucose monitoring and insulin delivery systems.67,68 Automated remote monitoring has enabled healthcare professionals to deliver personalized care to patients regardless of their location. In the US, personalized medicine approaches, including personalized DM treatment recommendations, have been advancing steadily. AI techniques have been employed to analyze individual patient data and provide tailored treatment recommendations. 69 These recommendations consider diverse factors such as medical history, genetic predisposition, lifestyle choices, and treatment responses, ultimately enhancing the management of DM for individual patients.70,71,72
Challenges and Future Directions
The collection of longitudinal data on diabetes can help trace the disease progression and transition from a single to polychronic conditions. 82 AI has the potential to revolutionize diabetes care management. However, there are indeed challenges in developing and implementing these AI systems with panel data, particularly when considering countries like India and the US with their unique contexts. Some of these challenges are elaborated below and are summarized in Table 1. AI systems rely heavily on patient data. Concerns around data privacy and security are of paramount interest. Ensuring data anonymization, secure storage, and transparent use of data are crucial hurdles. 83
Challenges Associated With AI-based Diabetes Care Management Systems.

Challenges Specific to India
In India, several challenges specific to implementing an AI-based DM management system arise due to the country's diverse healthcare landscape and resource constraints.
Challenges Specific to the US
In the US, the implementation of an AI-based DM management system faces several challenges specific to the country's intricate healthcare landscape and concerns surrounding data privacy and security.
Future Directions
Considering the multitude of challenges observed in both nations, below are a few outlined future directions aimed at improving AI-powered DM management systems.
Data-Driven Direction. Efforts in data-driven direction encompass various crucial aspects. Firstly, initiatives to standardize data collection formats and promote widespread adoption of standardized EHR systems by policymakers and healthcare organizations could greatly enhance the implementation of AI-based systems, enabling more effective access and analysis of patient data, leading to improved insights and decision-making. Secondly, implementing automated data validation processes and data cleansing or preprocessing techniques could significantly enhance data quality. These processes involve automatically identifying and correcting errors, inconsistencies, and missing values within the data, ensuring that they are accurate, complete, and reliable. By improving data quality, these techniques enable the development of more robust and generalized AI-based systems. High-quality data enhances the performance and accuracy of AI algorithms, leading to more reliable insights and predictions. Thirdly, synthetic data generation serves as a valuable tool for overcoming limitations like data scarcity and privacy concerns, while also addressing issues of data imbalance or bias, augmenting existing datasets and improving model training and validation. Additionally, ensuring secure data storage and transmission through sophisticated encryption methods and access controls is essential for safeguarding patient privacy and maintaining confidence in the security of health information. Lastly, leveraging multimodal data sources, including EHRs, wearable devices, genomic data, and social determinants of health, can enhance prediction capabilities, facilitate holistic AI-based systems, and improve decision-making processes. The longitudinal data of patients could be employed to track changes in health over time. Longitudinal data provide insights into disease progression, treatment efficacy, and the impact of lifestyle factors on DM management. AI models can leverage longitudinal data to identify trends, predict future health outcomes, and personalize treatment plans accordingly.
Model-Driven Direction. In the realm of model-driven direction for diabetes care management, several key strategies emerge. Firstly, there is a focus on personalized and adaptive AI models, which tailor recommendations and interventions to individual patient characteristics, preferences, and responses. Advancing with hybrid models integrates ML and DL techniques to balance complex pattern recognition with interpretability, crucial for clinical decision-making. Automated hyper-parameter tuning optimizes model performance and adaptability, reducing manual effort and accelerating model development. Algorithmic fairness tools are employed to identify and mitigate bias within AI models, ensuring fairness across patient populations. Dynamic model evolution allows continuous learning and adaptation based on new data and real-world outcomes. Scalable and generalizable models handle extensive data volumes and demonstrate consistent performance across diverse groups and conditions. Explainable AI techniques provide transparent insights into model reasoning, fostering trust among healthcare providers and patients. Finally, seamless integration into real-time care systems, such as mobile applications or wearable devices, aims to improve accessibility and usability, ultimately enhancing patient outcomes and quality of life in diabetes care management.
Integrative Theoretical Frameworks. The development of predictive analytics for diabetes care and outcomes research could be supplemented by a well-conceived theoretical framework that could facilitate statistical modeling and validation of testable hypotheses derived from a transdisciplinary perspective via the identification of patient (micro-level), and provider and community (macro-level) predictor variables in diabetes care research.87,88
Conclusions
In this article, the authors have provided key observations associated with DM management in India and the US. This article presents 2 main contributions: a discussion comparing management approaches for this disease in India and the US, and key observations regarding AI techniques applicable to DM management. This research work on key observations can be advanced based on the directions for future work illustrated in the previous section. It is important to note that the investigators have undertaken the critical and important task of observing variations in DM management. Additionally, a key improvement in the management of this disease using AI has been illustrated in the article. Further exploration of these AI techniques is necessary to improve healthcare outcomes for processes associated with DM management.
Footnotes
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The authors received no financial support for the research, authorship, and/or publication of this article.
Data Availability Statement
Data sharing not applicable to this article as no datasets were generated or analyzed during the current study.
