Abstract
This study aimed to investigate the role of hearing aid (HA) usage in language outcomes among preschool children aged 3–5 years with mild bilateral hearing loss (MBHL). The data were retrieved from a total of 52 children with MBHL and 30 children with normal hearing (NH). The association between demographical, audiological factors and language outcomes was examined. Analyses of variance were conducted to compare the language abilities of HA users, non-HA users, and their NH peers. Furthermore, regression analyses were performed to identify significant predictors of language outcomes. Aided better ear pure-tone average (BEPTA) was significantly correlated with language comprehension scores. Among children with MBHL, those who used HA outperformed the ones who did not use HA across all linguistic domains. The language skills of children with MBHL were comparable to those of their peers with NH. The degree of improvement in audibility in terms of aided BEPTA was a significant predictor of language comprehension. It is noteworthy that 50% of the parents expressed reluctance regarding HA use for their children with MBHL. The findings highlight the positive impact of HA usage on language development in this population. Professionals may therefore consider HAs as a viable treatment option for children with MBHL, especially when there is a potential risk of language delay due to hearing loss. It was observed that 25% of the children with MBHL had late-onset hearing loss. Consequently, the implementation of preschool screening or a listening performance checklist is recommended to facilitate early detection.
Introduction
Mild bilateral hearing loss (MBHL) is characterized by an average pure tone hearing threshold between 20 and 40 dB HL in both ears (Bess et al., 1998). The prevalence of MBHL in children varies greatly depending on several factors, including the hearing criteria employed by researchers and ethnic background (e.g., Asian, Hispanic, European) of the child. The prevalence of MBHL among newborns ranges from 0.036% to 0.05% (Sabbagh et al., 2021; Watkin & Baldwin, 1999), while that among children in the school-age group ranges from 1% to 9.2% (Bess et al., 1998; Khairi Md Daud et al., 2010; Wang et al., 2019). Currently, universal newborn hearing screening (UNHS) employs otoacoustic emission (OAE) or automated auditory brainstem response (aABR) methods, which may not effectively detect infants with hearing thresholds better than 30 or 40 dB HL or identify newborns with delayed-onset or progressive hearing loss (Joint Committee on Infant Hearing [JCIH], 2019; Wu et al., 2017). Although most children with MBHL can be identified through UNHS, some are diagnosed later during preschool or school hearing screenings. Many of these children passed the UNHS without apparent speech or language delays before preschool age (Lü et al., 2011).
The UNHS program utilizing aABR at 35 dB nHL has been fully implemented in Taiwan since March 15, 2012, with a strong emphasis on the importance of early detection and treatment of congenital deafness (Lin et al., 2018). Ample evidence suggests that children with more severe hearing loss can benefit from early intervention, as indicated by comparable speech (Yoshinaga-Itano, 2003), language skills (Yoshinaga-Itano, 2003), and socioemotional development (Yoshinaga-Itano, 2003) when compared to their peers with normal hearing (NH). However, research by Walker, Holte, et al. (2015; Walker et al., 2017), Tomblin et al. (2014, 2015), and Fitzpatrick et al. (2015) has indicated that early amplification and intervention can also prove advantageous for speech and language development in children with MBHL.
The JCIH (2007) advocated that all infants should undergo newborn hearing screening no later than 1 month of age. Additionally, they must receive a comprehensive audiological evaluation no later than 3 months of age when the infant did not pass the initial screening. Infants diagnosed with hearing loss should receive hearing device fittings within 1 month of identification and be enrolled in the intervention program no later than by 6 months of age. However, most children with MBHL do not follow this 1-3-6 principle, even when they are directly referred for a diagnostic audiology assessment following a positive result of newborn screening (Walker, Holte, et al., 2015). The prolonged confirmation of mild hearing loss is frequently attributed to multiple diagnostic examinations and the consequential waiting time between medical appointments. This process can be time-consuming (Walker et al., 2017).
In addition, parents are more likely to be skeptical about the diagnosis when their children exhibit no apparent hearing difficulties and respond well to sound (Walker et al., 2017; Walker, Holte, et al., 2015). This often results in parental indecision regarding the adoption of amplification or intervention. (Fitzpatrick et al., 2010, 2014). This is evident in the comparable speech recognition abilities of children with MBHL to those of children with NH in quiet conditions (Crandell, 1993). However, recognizing speech in noise and reverberation has been reported to be more difficult for children with MBHL than for children with NH (Crandell, 1993; Lewis et al., 2016). Furthermore, Lewis et al. (2016) emphasized that children with MBHL expend greater cognitive resources to understand speech in adverse listening conditions, indicating an increased listening effort. Collectively, the auditory challenges faced by children with MBHL emphasize the need for dedicated attention and intervention.
Walker et al. (2017) showed that only 43% (35/81) of the children were fitted with HAs within 1 month after MBHL confirmation, and 64% (54/84) received early intervention by 6 months of age. As for hearing amplification, the reasons for delayed fitting included difficulty in obtaining HA fitting services, objections by family members, delay in obtaining approval for HA insurance, and no recommendation for HA from hearing professionals (Walker et al., 2017). Fitzpatrick et al. (2014) reported that only 58.5% (138/236) of the children with minimal hearing loss received recommendations for hearing amplification within 3 months after diagnosis. Lin et al. (2022) also reported that parents received contradictory advice regarding the necessity of HA for their children with MBHL. The low usage of HA was confirmed by a recent study in which only 33.3% (28/84) of the preschool children with MBHL in Taiwan obtained HAs (Hsieh & Lin, 2022).
At present, there is no consensus among professionals regarding the clinical need for amplification or intervention in children with MBHL (Chen et al., 2022; Ching et al., 2022; Fitzpatrick et al., 2010, 2016; Fitzpatrick, Cologrosso, et al., 2019). Given the absence of conclusive evidence and guidelines for audiologists, they encounter challenges in making decisions related to HA fitting and intervention for children with MBHL. As a result, audiologists frequently rely on their individual knowledge and experience to provide services for children with MBHL. For instance, a study highlighted that pediatric audiologists in diagnostic and rehabilitation settings in Australia navigate their profession by recognizing the limitations of existing evidence, considering various child and family factors, and integrating the perspectives of parents and families. This approach involves adopting a flexible approach to deliver personalized services (Ching et al., 2022).
Although the American Academy of Audiology (2013) recommended that children with MBHL should consider using HAs or remote microphone technology, the specific degree of hearing loss (e.g., ≥ 20 dB HL or ≥ 35 dB HL) for acquiring a personal amplification device has not been specified (Walker et al., 2017). Fitzpatrick, Gaboury, et al. (2019) found that children with MBHL demonstrated aidable criteria ranging from 15 to 30 dB HL. McCreery et al. (2020) proposed that children with MBHL having an unaided speech intelligibility index below 80 should be considered candidates for amplification. Wiseman et al. (2021) noted that if the child's hearing threshold exceeded the normal hearing level at speech-important frequencies (e.g., 500, 1000, 2000 Hz), amplification should be considered. As a result, professional recommendations often depend on the severity of the worse ear (Fitzpatrick et al., 2010, 2014).
In the absence of clear professional guidance or practical evidence, parents often experience uncertainty about the benefits of HAs (Fitzpatrick et al., 2016). Furthermore, children with minimal hearing loss tend to have lower rates of HA use than those with more severe hearing loss (Walker et al., 2013). The rate of HA use among children with MBHL varied between 33.3% and 94% in studies conducted by Hsieh and Lin (2022), Fitzpatrick et al. (2010, 2015), and Walker, Holte, et al. (2015; Walker et al., 2017). The difference in HA use rates may be attributed to diverse factors, including hearing criteria for MBHL, cultural perspectives, or variations in service provision modes. Parents of children with mild hearing loss often have an ambivalent attitude towards intervention and tend to adopt a “wait-and-see” approach, especially when their children continue to meet developmental milestones. It is also important to note that eligibility for early intervention may vary depending on social welfare policies in different countries (Holstrum et al., 2008; Walker, Holte, et al., 2015).
Currently, several studies have shown that children with MBHL may have weak academic performance (Walker et al., 2020; Winiger et al., 2016), unclear speech (Winiger et al., 2016), poor language performance (Tomblin et al., 2015; Tomblin, Oleson, Ambrose, Walker, McCreery, et al., 2020; Tomblin, Oleson, Ambrose, Walker, and Moeller, 2020; Vohr et al., 2012; Winiger et al., 2016), limited social skills (Laugen et al., 2017), and psychosocial problems (Winiger et al., 2016). For example, Winiger et al. (2016) concluded that children with MBHL had poorer language skills than their peers with NH even when the test results fell within normal ranges, indicating that untreated MBHL may hamper children's full potential for language development. However, other findings suggested that amplification and intervention may be beneficial in closing the gap in performance between children with MBHL and their peers with NH. For example, auditory and language abilities were found comparable to those of children with NH where 80% (44/55) of the children with minimal hearing loss were HA users and had enrolled for the intervention (Fitzpatrick et al., 2015). Furthermore, the consistency of HA use was reported to modulate language outcomes in children with MBHL. Full-time HA users with greater than 8.7 daily wearing hours performed significantly better in vocabulary and grammar tests than non-users (Walker, Holte, et al., 2015).
Although there is increasing evidence that suggests a positive effect of HA on children with MBHL, the inclusion criteria for participants’ hearing status varied across studies. First, studies often combine MBHL, unilateral hearing loss, and high-frequency hearing loss, as they all fall under the umbrella term of “minimal hearing loss”. (Fitzpatrick et al., 2010, 2014, 2015, 2022; Fitzpatrick, Cologrosso, et al., 2019; Laugen et al., 2017). Second, mild HL classification often necessitates only the involvement of the better ear, potentially resulting in the categorization of asymmetric hearing loss (Fitzpatrick et al., 2010, 2014, 2015, 2022; Fitzpatrick, Cologrosso, et al., 2019; Laugen et al., 2017; Vohr et al., 2012; Walker et al., 2017). For example, in Fitzpatrick et al.'s (2015) study, they included children with both bilateral (24/55, 43.6%) and unilateral hearing loss (31/55, 56.4%). Moreover, although the average hearing threshold of the better ear for bilateral group was 32.4 dB HL with a maximum of 45 dB HL, the hearing range of the worse ear ranged between 23.3 and 85.0 dB HL, substantially exceeding the definition of mild hearing loss. Similarly, widely varied hearing levels in worse ear were observed in Walker, Holte, et al. (2015) with a threshold ranging from 10 to 61.25 dB HL. Thus, it remains unclear whether amplifications truly facilitate language learning in children with MBHL whose hearing levels in both ears meet the criteria for mild hearing loss.
The primary objective of this study was to enhance our understanding of the factors influencing the development of MBHL in children, with a specific focus on the potential impact of HA on language development. The study aimed to accomplish three main goals. First, we aimed to assess differences in language scores among three groups: children with MBHL using HAs, children with MBHL not using HAs, and children with NH. Second, we sought to examine the relationship between audiology-related factors, such as age at identification, aided audibility, consistency of HA use, age at intervention, and language outcomes. Third, we investigated the reasons behind the low acceptance of HAs for developing tailored counseling strategies based on parental concerns. Fourth, we aimed to explore whether the pathway of children with MBHL aligns with the 1-3-6 principle.
Methods
Participants
Eighty-two Mandarin-speaking children (44 boys) aged 36–71 months (M = 53.33, standard deviation [SD] = 9.76) were recruited, including 52 children with MBHL (26 HA users [Mage = 49.88 months, SD = 9.58, range = 36–62 months] and 26 non-HA users [Mage = 55.69 months, SD = 9.59, range = 38–70 months]) and 30 children with NH (Mage = 54.27 months, SD = 9.55, range = 37–71 months). The severity of hearing loss was controlled bilaterally to ensure that it met the definition of MBHL (i.e., 20 dB HL ≤ pure tone average at 0.5, 1, 2, and 4 kHz ≤ 40 dB HL). No additional disabilities were reported in all children.
All children underwent UNHS. Among children with MBHL, 39 children (39/52, 75%) did not pass the UNHS, while 13 children (13/52, 25%) initially passed the UNHS but were later diagnosed with bilateral delay-onset hearing loss, either through preschool screening (n = 7) or self-initiated appointment for hearing test (n = 6). Furthermore, among 13 children with late-onset hearing loss, four individuals were HA users.
All children in the HA group used bilateral HAs on daily basis and were enrolled in either auditory-verbal (n = 23) or speech therapy (n = 3). The prescriptive formula used for HA fitting was DSL v5.0a, and the verification was conducted using Audioscan. Among the 48 HAs evaluated on 24 children, 46 were assessed using simulated probe microphone measures, while 2 were measured using real-ear probe microphone techniques. In addition, the fitting accuracy of HAs was within a ± 5 dB RMS error, aligning closely with DSL v5.0a prescriptive targets. Previous research supported the consideration of this threshold for adequate proximity to prescriptive targets in evaluating the characteristics of HA fittings (Cox & Alexander, 1990; Moore et al., 2001). It is crucial to emphasize that, despite observed variances between simulated and real-ear probe microphone measures, these differences do not have a significant impact on HA fitting targets (Lin et al., 2023).
Datalog information was available for 24 HA users, with an average HA-wearing time of 6.6 h (SD = 2.8, range = 1–11). The consistency of HA use was measured using wear time percentage (WTP), which is calculated based on each child's awake time and the HA wear time obtained from the datalogs (average daily wearing hours/child's average awake hours × 100%) for further analysis (Hung et al., 2024). The mean WTP was 50% (SD = 20.43%, range = 9.09%–84.23%).
Furthermore, 27 children with MBHL (27/52, 51.92%) received the four prominent deafness-related gene tests (gap junction beta-2 protein [GJB2 mutations], SLC26A4, mitochondrial 12S rRNA, and otoferlin [OTOF]). Among them, 24 children (24/27, 88.89%) had GJB2 mutations, one (1/27, 3.7%) had GJB2 and OTOF mutations, one (1/27, 3.7%) had mitochondrial 12S ribosomal RNA, and one child (1/27, 3.7%) tested negative.
Procedures
Data for the 52 children with MBHL were obtained from the Children's Hearing Foundation (n = 21) or MacKay Memorial Hospital (n = 31). The NH data (n = 30) were retrieved from Children's Hearing Foundation, and related results have been partially published by Chen and Fu (2018). This study was approved by the Institutional Review Boards (IRB) of the Chang Gung Medical Foundation (IRB No. 201900104B0) and MacKay Memorial Hospital (IRB No. 22MMHIS460e) in Taiwan. The requirement for obtaining informed consent was waived.
Measurement
Language Assessment
The Revised Preschoolers Language Assessment (RPLA) (Lin et al., 2008) is a standardized test designed to evaluate the language comprehension (37 items) and oral expression (46 items) abilities of children aged between 36 and 71 months. The test yields an overall language development score by combining the total scores from both subscales. The subscales demonstrate strong internal consistency with Cronbach's alpha values ranging from 0.91 to 0.96, and the test–retest reliability ranges from 0.92 to 0.96. The subscales correlate strongly with the total scale score (r = 0.93 for language comprehension and r = 0.95 for oral expression), and they are also moderately correlated with each other (r = 0.78). The test's convergent validity coefficient was calculated by correlating it with the Diagnostic Assessment of Syntax in Oral Language for children in Preschool, resulting in r = 0.74 (Yang et al., 2005).
The children participated in an individual testing conducted in a quiet room. Trained speech pathologists or auditory-verbal practitioners administered the tests for children with MBHL, while research assistants administered the tests for children with NH. On average, it took the children approximately 30–40 min to complete the test.
Survey for HA Rejection
Parents of non-HA users (n = 26) were surveyed using a multiple-choice questionnaire to determine reasons for HA rejection, with the option to select multiple reasons. The choices included: (1) stigma associated with wearing HAs, (2) perceiving no need for HAs, (3) objection by family members, (4) high cost, (5) ineligibility for the subsidy, (6) discomfort, (7) limited perceived benefit, (8) non-recommendation by otolaryngologists or audiologists, and (9) wait and see. The term “discomfort” indicates that the children experienced unease while using HA.
Data Analysis
None of the demographic, audiological, and intervention-related variables exhibited problematic univariate variables as the absolute values of skewness, and the kurtosis index did not exceed 2.00, except the speech intelligibility index (SII). The SII assessment employs Speech-Std(1) stimuli to measure the intelligibility of speech audible at 65 dB SPL for listeners, evaluated through real-ear measurements. Descriptive statistics were used to summarize and describe the distribution of variables. To discern variations between HA users and non-HA users with MBHL, we utilized the independent samples t-test and Mann–Whitney U test for the analysis of background and audiological variables (quantitative variables). Additionally, the Chi-square test was applied to examine gender differences (qualitative variable). The Spearman's rho correlation was conducted to examine the relationship between HA usage and language scores; the Pearson's correlation was then conducted to explore the correlation among age at identification, age at HA fitting, duration of HA use, age at intervention, duration of intervention, unaided and aided better ear pure tone average at 0.5, 1, 2, and 4k Hz (BEPTA), unaided and aided worse ear pure tone average at 0.5, 1, 2, and 4k Hz (WEPTA), unaided and aided better ear speech intelligibility index (BESII), and unaided and aided worse ear speech intelligibility index (WESII), HA wearing time percentage (WTP), and language standard scores (i.e., normalized T-scores) for children with MBHL to provide an overview of relationships among variables.
A series of one-way analysis of variance (ANOVA) with the Bonferroni correction was conducted to investigate whether there were differences in language performance between children with NH and MBHL who were fitted with HAs or not. Based on the results of correlation, a simple linear regression was conducted to identify significant predictor of language performance in children who used HAs. In this study, all data were analyzed using the Statistical Package for the Social Sciences 23.0 version, and the significance level was defined as α < 0.05.
Results
The overall demographics, audiological and intervention information of the participants with MBHL and NH are summarized in Table 1. Among children with MBHL, a significantly worse unaided BEPTA was found in the HA group compared to the non-HA group (t = 2.23, p = .03, Cohen's d = 0.62). Furthermore, a significantly better aided BEPTA was found in the HA group compared to the unaided BEPTA in the non-HA group (t = −5.30, p = .00, Cohen's d = 1.50). Similarly, a significantly lower unaided BESII was obtained in the HA group than that in the non-HA group (U = 125.00, p = .000, r = .50), and a significantly higher aided BESII was observed in the HA group compared to the unaided BESII in the non-HA group (U = 176.00, p = .003, r = .41).
Demographics, Audiological, and Intervention Information of the Participants.

Note. HA, hearing aid; NH, normal hearing; n, number of participants; %, percent; M, mean; SD, standard deviation; BEPTA, better ear pure tone average threshold at 0.5, 1, 2, 4 kHz; WEPTA, worse ear pure tone average threshold at 0.5, 1, 2, 4 kHz; SII, speech intelligibility index.
One child underwent the language assessment 1 month prior to intervention. bWear time percentage (WTP) was available for 24 children. cAided PTA was not available for two children. dAided SII was not available for three children.
No significant differences were found among the HA, non-HA, and NH groups in chronological age (F = 2.62, p = .08, ηp2 = 0.06). Also, no significant difference in age at identification was observed between the HA group (M = 14.96, SD = 18.06) and non-HA group (M = 24.19, SD = 23.52) (t = −1.59, p = .12, Cohen's d = 0.44). There was also no significant difference in gender distribution between the HA group (57.69% boys) and the non-HA group (53.85% boys) (χ2 = 0.078, df = 1, p = .78).
According to the RPLA guidelines, a child with an average score that falls 1.5 and 2.0 SD below the age norm is deemed to be at risk for language delay and significant language delay, respectively (Lin et al., 2008). In this study, two children with MBHL were considered at risk of language delay, and one child with MBHL showed language delay. Moreover, two of them passed the UNHS but were later identified with hearing loss during the preschool hearing screening at the ages of 59 and 60 months, respectively. The unaided BEPTA values of these children were 20.00 and 23.75 dB HL, respectively. The remaining child did not pass the UNHS and was diagnosed with hearing loss at 2 months of age, with an unaided BEPTA of 27.50 dB HL. Prior to the language testing, professionals did not recommend HAs or intervention for these children, and the parents did not seek further assistance in obtaining HAs or intervention services. None of these three children underwent genetic screening, and they did not receive subsidies for low-income households.
Significant positive correlations between HA usage and language comprehension (ρ = .352, p = .011), oral expression (ρ = .330, p = .017), and language development (ρ = .362, p = .008), indicating that using HAs is associated with better language skills. Separate correlation analyses were conducted for HA and non-HA groups to examine the relationships between demographic, audiological, and intervention-related factors and the language performance. An overview of the results is displayed in Table 2. No significant correlations were found among numerous variables related to intervention and audiologic factors, including age at identification, age at intervention, age at HA fitting, duration of HA use, WTP, unaided PTA, and unaided/aided SII. Crucially, the aided BEPTA was the sole significant factor correlated with language outcome, specifically the scores of language comprehension (r = −0.51, p < .05). This signified that as the aided BEPTA improved, there was an associated improvement in the child's language comprehension ability.
Pearson's Correlation Matrix of the Study Variables.

Note. HA users for the lower triangle, shaded in gray, and non-HA users for the upper triangle.
HA, hearing aid; BEPTA, better ear pure tone average threshold at 0.5, 1, 2, 4 kHz; WEPTA, worse ear pure tone average threshold at 0.5, 1, 2, 4 kHz; SII, speech intelligibility index.
*p < .05. ** p < .01.
Language Performance: HA Usage
As shown in Figure 1, the HA group achieved higher average scores in language comprehension, oral expression, and language development compared to the other groups. Specifically, the mean normalized T-scores in the HA group were 57.38 (SD = 8.61), 52.38 (SD = 7.12), and 55.23 (SD = 7.85) for language comprehension, oral expression, and language development, respectively. The non-HA group had mean scores of 50.77 (SD = 9.16), 47.88 (SD = 6.00), and 49.19 (SD = 7.11) for the same language measures. In the NH group, the mean scores were 52.10 (SD = 7.37), 50.57 (SD = 6.27), and 51.47 (SD = 6.69) for language comprehension, oral expression, and language development, respectively.
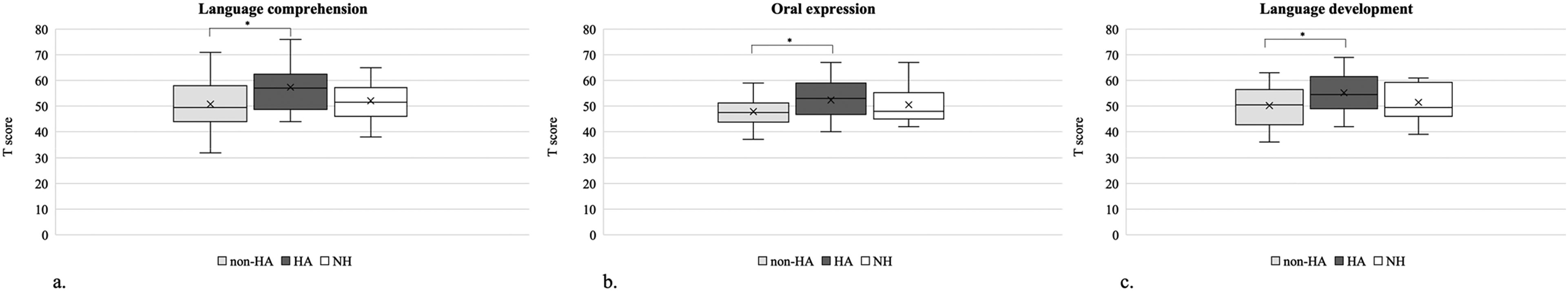
Language performance between non-HA, HA, and NH groups. a. language comprehension; b. oral expression; c. language development.
To compare language performance between the HA group (n = 26), non-HA group (n = 26), and their age-matched peers with NH (n = 30), one-way ANOVA was conducted, and no assumptions were violated. Significant differences were found between HA, non-HA, and NH groups in language comprehension (F = 4.60, p = .01, ηp2 = 0.10), oral expression (F = 3.19, p = .05 ηp2 = 0.08), and language development (F = 4.67, p = .01, ηp2 = 0.11). The post hoc analyses further revealed significantly better performance for the HA group than for the non-HA group in language comprehension (p = .02), oral expression (p = .04), and language development (p = .01).
Predictors of Language Outcomes for Children With MBHL
To first ascertain whether the use of HAs serves as a predictive factor for language outcomes, we constructed regression models. The independent variable comprised the presence or absence of hearing aids (coded as a dummy variable), while the dependent variables encompassed language comprehension, oral expression, and language development.
The results revealed that the use of HAs emerged as the sole significant predictor of language comprehension (F = 6.81, p = .012), oral expression (F = 6.27, p = .016), and language development (F = 8.31, p = .006). The models explained 12.4%, 11.6%, and 14.8% of the variance in language comprehension, oral expression, and language development, respectively. Furthermore, the effect sizes, as measured by Cohen's f2, were 0.142, 0.131, and 0.173, respectively, indicating a moderate level of influence.
Based on the aforementioned results, a simple linear regression analysis was further conducted to identify the predictive factor that influences language performance among children using HAs. The regression model included 24 HA users who had available data on aided BEPTA and were enrolled in the intervention.
The independent variable was aided BEPTA as it was the sole significant factor correlated with language outcome, and the dependent variables were the language performance scores in language comprehension, oral expression, and language development.
Aided BEPTA emerged as the sole significant predictor of language comprehension (F = 7.55, p = .012). This model explained 25.6% of the variance, with an effect size of Cohen's f2 = 0.343, indicating a moderate effect size. Additional information regarding the simple linear regression analysis can be found in Table 3.
Simple Linear Regressions for Language Performance in Children With MBHL and HA Users.

Note. For the purpose of analysis, a binary coding system was employed, with the presence of HA assigned a code of 1, while the absence of HA was assigned a code of 0; BEPTA, better ear pure tone average threshold at 0.5, 1, 2, 4 kHz.
Reasons for HA Rejection
Among the non-HA group, four children had previous experience with HAs but discontinued their use, while 22 children had never used HA. None of the non-HA users received any form of intervention. Each parent (n = 26) could provide multiple reasons, resulting in a total of 46 responses. The results are displayed in Figure 2.

Reasons for HA rejection. Each parent of the non-HA users (n = 26) could provide multiple reasons, resulting in a total of 46 responses.
Alignment With 1-3-6 Principle
All 52 children with MBHL underwent newborn hearing screening before the age of 1 month, in line with the universal implementation of this practice in Taiwan. Among the 39 who failed UNHS, the average age for receiving their diagnosis was 10.56 months (SD = 14.21, range = 1–58). HA fitting (n = 22) occurred at an average age of 16.86 months (SD = 14.44, range = 4–60), and the average age for enrollment in early intervention (n = 22) was 24.05 months (SD = 16.57, range = 7–63).
An assessment of adherence to the 1-3-6 timeline revealed that none of the children in the study conformed to this principle. The closest instances involved two children who were diagnosed at the age of 3 months, then initiated HA usage at 4 and 6 months, respectively, and subsequently entered early intervention at the age of 10 months.
Discussion
The primary objective of this investigation was to identify significant audiological factors related to language performance among children with MBHL. The study further sought to assess the potential influence of HA use on language outcomes and its predictive value in language outcomes. We also investigated the attitudes of parents towards HA use, and whether their journey aligns with the 1-3-6 principle. Furthermore, the genetic data of children was compiled to explore potential shared patterns or commonalities.
The results of this study revealed that only the aided BEPTA was significantly associated with language comprehension in a negative matter. That is, the amount of improved audibility with HAs correlated with better language outcomes in children with MBHL, particularly in language comprehension. However, while there is a strong correlation between aided SII and aided PTA outcomes, only the aided PTA outcomes show an association with language outcomes. We speculated that the observed difference could stem from the absence of a suitable Chinese version of the SII for electroacoustic assessments. Consequently, it's important to interpret the current SII values of Chinese native users cautiously, as they may not precisely represent the audibility of Chinese speech (Wong et al., 2007). Overall, these results underscored the potential importance of HA use and its benefit on language learning in children with MBHL.
This finding was further supported by the results of comparison of language abilities between HA users, non-HA users, and their age-matched peers with NH, which revealed that HA users significantly outperformed non-HA users in all linguistic domains. This included language comprehension, oral expression, and language development, even though non-HA users had significantly better unaided hearing thresholds than HA users. It is worth mentioning that HA users should, however, have access to clearer speech after HA fitting, as reflected in a significantly better aided BEPTA and aided SII than the unaided BEPTA and unaided SII in non-HA users. In addition, regardless of HA use, children with MBHL generally exhibited comparable language abilities compared to their peers with NH.
Furthermore, the presumption of benefit of HA was reinforced by the results of a regression wherein the contribution of HA and audiological-related factors to language performance were examined. The use of HAs was confirmed as a significant predictor of language performance in children with MBHL. More specifically, the findings further suggested that hearing ability improved by using HA, as indicated in aided BEPTA, was the only significant predictor of scores in language comprehension.
Taken together, this comprehensive analysis consistently highlighted the potential benefits of HA and the degree of improvement in audibility achieved through HA use was found to be an important factor in determining the language comprehension of children with MBHL. However, only 50% (26/52) of the children with MBHL were HA users on the daily basis, and the reasons for HA rejections varied. Over 80% of the parents whose children did not use HAs, perceived HAs as unnecessary. This perspective was probably based on the fact that their children generally exhibited no difficulties in understanding speech at a normal conversational level, particularly in quiet environments. Furthermore, these parents observed that their children were reaching developmental milestones without facing any notable challenges related to hearing difficulties. In addition, more than 35% of the parents did not receive professional advice to pursue HAs. Given the mild degree of hearing loss, many professionals often considered regular monitoring of the child's hearing status to prevent any further decline would be sufficient, thus, alleviating the immediate need for HAs. It is worth noting that similar hearing thresholds can be observed between children who did not receive a recommendation for HAs (BEPTA ranging from 20.00 to 38.75, M = 27.88) and those who did receive a recommendation (BEPTA ranging from 20.00 to 36.25, M = 28.28).
Thus, professionals may consider HAs as a viable treatment option for children with MBHL, especially when there is a potential risk of language delay due to hearing loss. Furthermore, it is important to acknowledge that parents may find it challenging to recognize subtle changes in their child's response to sound that result from the HA use. As a result, they might not fully recognize the advantages of HA use, particularly in the short term. Studies suggest that recognizing the substantial cumulative impact of HA on language abilities requires time, irrespective of the severity of hearing loss (Tomblin et al., 2015). To address this, professionals can employ various strategies to assist parents in recognizing and responding to these changes effectively. For example, this can be achieved by providing information about possible changes in hearing-related behaviors, such as the child being more engaged in conversations, following instructions more easily and correctly, especially in noisy environments, or demonstrating improved speech clarity and language skills. Moreover, it has been suggested that, in contrast to classification-based strategies reliant on pure-tone-based descriptors for hearing loss levels (e.g., slight, mild, and moderate), audibility-based strategies utilizing the SII as a continuous scale of audibility could offer a more effective approach in parent counseling. This approach avoids audiological terminology that might under-emphasize the developmental impact of hearing loss while also closely mirroring real-world scenarios. By reflecting compromised auditory access, audibility-based strategies may prompt a sense of urgency, potentially leading to more immediate intervention (Sapp et al., 2023).
While Walker, Holte, et al. (2015) reported similar findings that children with mild hearing loss using HAs full-time achieved significantly better scores in various language assessments compared to non-HA users, our study highlights distinctions in the daily HA usage patterns. Specifically, the present results revealed that children with MBHL had an average daily HA use time of 6.6 h, contrasting with Walker, Holte, et al. (2015) reported 8.7 h or more for children with mild hearing loss. This discrepancy may stem from variations in the inclusion criteria for mild hearing loss, with Walker, Holte, et al. (2015) incorporating children with a broader range of hearing degrees in the poor ear (ranging from 10 to 61.25 dB HL). Furthermore, they collected daily use hours either from parent reports (43%) or datalogs (57%), and it has been reported that parents may tend to overestimate HA usage (Walker et al., 2013; Walker, McCreery, et al., 2015).
Importantly, when considering individual sleeping hours, we found that children with MBHL only spent 50% of their waking hours using HAs. The consistency of HA use seemed to be generally lower than that in children with more severe hearing loss who achieved better language outcomes (Gagnon et al., 2020; Gagnon et al., 2021; Tomblin et al., 2015; Walker, Holte, et al., 2015). According to parents' feedback and our observations, many children with MBHL often wear HAs only in a more challenging hearing environment, such as at school with more noise and distant speech. However, the present study showed that despite the relatively low consistency of HA use, children with MBHL who received improved auditory quality still performed significantly better than children who were non-HA users. As the consistency of HA use in terms of WTP did not correlate with language performance in this study, it is still unclear whether the consistency of HA use had a comparatively weaker impact on language outcomes in children with MBHL when compared to those with more severe hearing loss. To gain a better understanding, future research should focus on examining the relationship between the consistency of HA use and language development in children with varying degrees of hearing loss.
However, it is essential to recognize that besides the variables examined in this study, there may be additional confounding factors that were not considered, such as family-specific characteristics like parental education level, socioeconomic status, parental self-efficacy, and family dynamics. Furthermore, it was not possible to disentangle the effects of HAs and intervention in this study, as all HA users were also enrolled in either speech therapy or auditory-verbal therapy. Considering these additional variables would contribute to a more comprehensive understanding of the interplay between these factors in determining language outcomes in children with MBHL. Therefore, based on the current data and analyses, it is crucial to exercise caution and avoid overinterpreting the benefits of HA use in children with MBHL.
The current study revealed that compared to those who were ideally identified through UNHS and followed the 1-3-6 principle, children with MBHL were more likely to receive their diagnosis and treatment at a later stage. This is especially true for children who were not identified through UNHS (n = 13). These factors pose additional challenges for early identification in children with delayed-onset or progressive hearing loss. Delays in obtaining HA fitting may be attributed to medical and parental oversights. Unlike hearing loss with greater severity, interventions, and hearing devices for children with mild hearing loss are often not consistently regarded as essential by professionals and parents (Fitzpatrick et al., 2010; Walker et al., 2017). This is probably due to a lack of recognition of potential issues associated with mild hearing loss in young children. Similar delays in diagnosis, HA fitting, and intervention were also noted for children with unilateral hearing loss (Hung et al., 2022; Hussain et al., 2021).
In addition, 14 children with delayed-onset hearing loss, seven of them underwent a gene test, and five children had GJB2 mutations (p.V37I), one child had GJB2 (p.V37I), and OTOF mutations (c.5098 G > A). It is worth noting that the p.V37I and c.235 delC variants of GJB2 are the most common causes of non-syndromic hearing loss, among the East Asian population (Chen et al., 2020; Wu et al., 2017), and the p.V37I mutation is related to mild or moderate hearing loss (Chen et al., 2020; Huang et al., 2015). Besides, Chen et al. (2020) reported that 58% of the participants with GJB2 mutations had minimal or mild hearing loss, in Taiwan. Wu et al. (2017) and Chen et al. (2020) found that people with p.V37I variants of GJB2 experienced a gradual worsening of their hearing ability at a rate of approximately 0.6–1 dB HL per year [8,39]. Overall, patients with GJB2 (p. V37I) and mitochondrial 12S rRNA mutations (m.1555 A > G) may exhibit late-onset/progressive deafness (Chen et al., 2020; Wu et al., 2007; Wu et al., 2017). This finding not only indicates that the GJB2 gene should be tested in patients with MBHL (Huang et al., 2015) but also emphasizes the importance of early detection and regular monitoring of hearing status in children with these genetic mutations to prevent further deterioration in hearing. Therefore, preschool hearing screening plays an essential role, as it can identify hearing loss, that may have been missed in infancy and can also identify any changes in hearing abilities to enable early intervention to prevent any potential delays or hearing-related challenges during development.
In addition to preschool screening, the implementation of other screening tools, such as a listening performance checklist, is also important. By administering the listening performance checklist, caregivers or educators can quickly and easily identify children who may be struggling with hearing-related issues, such as behavioral problems like inattention, repeating requests, and confusion with similar-sounding words. Children with MBHL may also exhibit speech distortion and speak too loudly or softly (Dodd-murphy & Mamlin, 2002). When caregivers or educators notice these problems in children, they should consider the need for a hearing evaluation, even if the child has passed a hearing screening (Dodd-murphy & Mamlin, 2002).
To enhance the overall development of children with MBHL, it is imperative to address this issue by implementing preschool screening or listening performance checklists to achieve early detection, thereby urging clinical professionals to provide appropriate treatment and management strategies to raise parents’ awareness of the potential negative effects of untreated mild hearing loss. Overall, the findings of this study contributed valuable information for the development of management strategies aimed at improving outcomes for children with MBHL.
Footnotes
Acknowledgments
The authors would like to thank all the children and their families who took part in this study.
Data Availability Statement
All data generated or analyzed during this study are included in this article. Further inquiries can be directed to the corresponding author.
Declaration of Conflicting Interests
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical Approval
The study was approved by the Institutional Review Boards of the Chang Gung Medical Foundation (IRB No. 201900104B0) and MacKay Memorial Hospital (IRB No. 22MMHIS460e).
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This study received funding from Children’s Hearing Foundation [CHF-2019-024-E-009-a] and Zi Ji Zhong Limited [COFxMMC-RD-110-2D-G001-01]. The funder was not involved in the study design, collection, analysis, interpretation of data, the writing of this article, or the decision to submit it for publication.
