Abstract
The cannabinoid chemistry is currently being addressed in preclinical approaches as a viable therapeutic alternative for the management of a wide range of signs, symptoms, and some biochemical hallmarks of many neurological pathologies (such as neuroinflammation and neurodegeneration). This clinical orientation is grounded on the consistent promissory profile that cannabinoid compounds have shown, and the great necessity of feasible options to undergo such disorders. Even though at early research stages, metabolic disorders are starting to rise as potential targets of cannabinoid alternatives; approaches in this term could, in turn, aim to modulate the endocannabinoid response for therapeutic purposes. This review recalls the pathologic scenarios endured in the course of neurological diseases of high occurrence and the most typical metabolic disorders, while discussing the neuroprotective mechanisms of cannabinoid agonists in the central nervous system, and the potential targets of the endocannabinoid system and metabolic disorders.
Keywords
Introduction
Neurodegenerative diseases, such as Alzheimer disease (AD), Parkinson disease (PD), and multiple sclerosis (MS), are few examples of an enriched acquisition of disorders that have been studied for several decades. From its very first description, our comprehension of the intrinsic mechanisms behind such conditions has experienced substantial growth. Such a progress involves many overlapping mechanisms, including deposition and aggregation of misfolded proteins, resulting in progressive degeneration of nerve cells. Undoubtedly, such a setup has presented a unique opportunity for the alternative proposals of pathophysiological mechanisms and drug targets as well as novel pharmacological strategies in the generation of new drugs.
Frequently Expressed Neurodegenerative Disorders
As revised elsewhere, consistent pathological hallmarks of AD comprise the extracellular deposits of β-amyloid peptide, which is associated with cell death, and the consequent behavioral, memory, and cognitive alterations. Additionally, the formation of intracellular neurofibrillary tangles of tau protein constitutes a second distinctive characteristic of AD, and such a process is associated with detriment in neuronal communication. Furthermore, the role of activated microglia at the senile plaque’s fringe has been related with the antioxidant defense in AD brains. 1 –5 On the other hand, PD constitutes a second major example of the most notorious neurodegenerative diseases, and its characteristic motor and nonmotor signs are the result of a progressive loss of dopaminergic neurons residing principally in the substantia nigra pars compacta and their endings at the striatum. 6,7 Moreover, the pathological processes associated with the disease encompass the alteration of non-dopaminergic neurotransmitters and associated events, 8 and more importantly, dopaminergic metabolism as an intracellular source of reactive oxygen species (ROS). To complete the brief count, MS is a demyelinating disorder of the central nervous system (CNS) apparently caused by particular genotypes and environmental stimuli; it often stands out for its motor exacerbation manifestations, or “relapses,” which are followed by “remissions.” As known, MS leads to immune attack to the CNS and severe damage to oligodendrocytes—the glial cells that form myelin—as well as progressive inflammation throughout the brain and meninges. Therefore, the progression of the disease results in neuronal dysfunction and irreversible disability. 9 –12 Hence, countless efforts are being concentrated into the research and comprehension of these and many more neurodegenerative diseases, as therapeutics still face important challenges ranging from timely and accurate diagnoses to the generation of novel and effective therapies. For this reason, several pathogenic mechanisms are continuously being suggested and include mostly oxidative stress, local/generalized neuroinflammation, mitochondrial energy depletion, and so on, and the current ideology contemplates these examples, either running simultaneously or converging through time, as a feasible mechanism that leads to the progression observed typically in neurodegenerative diseases. 6,13
Organic Acidurias
Generically, organic acidurias (OAs) have been described as a family of inheritable disorders due to defects in metabolic pathways of amino acid degradation. These disorders are characterized by the tissue accumulation and high urinary excretion of organic acids, including glutaric acid (GA), 3-hydroxyglutaric acid (3-OHGA), methylglutaric acid (MGA), methylmalonic acid (MMA), propionic acid (PA), and so on, with special deleterious consequences to the brain. 14 Indeed, OAs are among the major causes of brain damage and other alterations in children. 15 –18 In high-risk groups, the frequency of OAs is much higher than in the general population. 19 Features such as age of onset and the severity of illness seem to depend on the accumulated levels of specific toxic metabolites. Some environmental factors, including metabolic distress and infections, are known to accelerate the severity of the clinical manifestations of these diseases, probably because of the dramatic increase in the accumulating metabolites.
Diagnosis of OA
Clinical characteristics in patients with OAs include mental retardation, seizures, coma, lethargy, vomiting, hypotonia, hepatomegaly, and cardiac malfunction. An early and accurate diagnosis (1-3 days) helps to prevent chronic events, such as mental retardation and physical dysfunction. 20 Two common laboratory features of OAs are hyperammonemia and metabolic acidosis. Other common biochemical events include hypoglycemia and ketonuria.
The OAs exclusively or predominantly affecting the brain are also known as “cerebral” OAs and are characterized by severe neurological manifestations. 18 Increased amounts of organic acids in the urine of patients with OAs are crucial for an accurate diagnosis. Current analytical methods to achieve diagnosis or OAs are gas chromatography/mass spectrometry that in some cases can be improved by tandem mass spectrometry, enzyme assays, and DNA analysis. Proton nuclear magnetic resonance and dinitrophenyl hydrazine tests can be also employed, although they are not conclusive of diagnosis. 20
Treatment
With a timely and accurate diagnosis, some OAs can be effectively treated, whereas many others do not reach a real treatment. Nutritional therapy provides essential nutrients to preserve and recover physical and mental conditions,
21
restricting the amino acids that generate the accumulating organic acids. Therefore, while alternative amino acid–based therapies constitute a constant source of energy and nutrients that can promote anabolism and growth,
20
dietary precursors of GA (mainly lysine) have to be avoided in glutaric aciduria type I (GA-I).
22
Since carnitine deficiency is also common in these disorders and helps to increase the excretion of organic acids,
Glutaric Aciduria Type I
The GA-I is a cerebral OA caused by a deficiency of glutaryl-CoA dehydrogenase (McKusick 23167; OMIM # 231670). Untreated patients show increased concentrations of GA (500-5000 μmol/L) and 3-OHGA (40-200 μmol/L) in body fluids and tissues, especially in the CNS. 24,25 Frontotemporal cortical atrophy at birth, progressive spongy formation, leukoencephalopathy, and acute damage of the caudate/putamen, are characteristically seen in this disorder during encephalopathy, that occur between 6 months and 4 years of age. 26,27 Although the pathogenic mechanisms responsible for neurological sequelae in GA-I are not fully established, several in vitro and in vivo studies suggest that the accumulating organic acids induce excitotoxicity, oxidative stress, and energy metabolism impairment. 28 –32
Methylmalonic Acidemia and Propionic Acidemia
Methylmalonic acidemia (MMAcidemia) and propionic acidemia (PAcidemia) are caused by a severe deficiency of methylmalonyl-CoA mutase (EC 5.4.99.2) and propionyl-CoA carboxylase activities (EC 6.4.1.3) and are biochemically characterized by predominant blood accumulation of MM (1-2.5 mmol/L) and PA (5 mmol/L), respectively. Clinical presentation of both OAs is similar and includes lethargy, psychomotor delay/mental retardation, focal and generalized convulsions, vomiting, dehydration, hepatomegaly, hypotonia, and encephalopathy, all leading to coma and death. 33 Cerebral magnetic resonance imaging shows delayed myelination (progressive cortical atrophy) and hypodensity of the basal ganglia. 34,35 It has been suggested that brain injury due to MMAcidemia and PAcidemia is mainly related with the toxic effects exerted by the accumulating metabolites. In this context, it has been demonstrated that MMA causes impairment of brain mitochondrial energy metabolism, as well as alterations in the redox status and glutamatergic neurotransmission. 36 –38 Neurotoxic effects of PA have also been reported in rat brain and human preparations. 39 –47
The Endocannabinoid System: Overview
The endocannabinoid system (ECS) has been known and increasingly recognized for about 2 decades. Given the emerging knowledge achieved throughout the history of Cannabis use, together with the evolving hypotheses of the overall role of cannabinoid (CB) circuitry in the human body, the ECS is now addressed as a rich matrix of receptors, ligands, and associated molecules involved in many physiological and pathological conditions. 48 –52 The ECS recruits a mechanism of intercellular communications that would execute modulatory actions in brain and peripheral systems; examples of physiological actions in which CB signaling might be associated include mood regulation (depression and anxiety), 53 control of intestinal motility, 52 urinary tract physiology, 54 vasorelaxation of healthy vasculature, 55 interference of the production of proinflammatory cytokines, and probably other immune functional activities as well as the maintenance of the immune homeostatic balance. 56 In addition, the role of CB signaling has been associated with crucial functions throughout the CNS development (both prenatal and postnatal), 50 which might play a relevant role under pathological contexts.
The ECS begins with the CB receptors 1 and 2 (CB1 and CB2, respectively), which are highly distributed within the CNS as well as in peripheral tissues. Both receptors belong to the superfamily of transmembrane-domain Guanosine triphosphate (GTP)-binding protein-coupled receptors, and it is known that they are associated with numerous cellular processes, such as the inhibition of synaptic transmission and the inhibition of the adenylate cyclase activity, resulting in the regulation of neurotransmitter release through its activation. 50 Opposite to the recurring hydrophilic cations associated with the Class A-G protein-coupled receptors’ group, its ligands have a lipophilic nature derived from the arachidonic acid, 48,53 such as fatty acid ethanolamides or glycerols found in countless CBs of endogenous nature. 49 As such, CB1 receptors are vastly expressed in the CNS, comparing in density with that of γ-aminobutyric acid or even glutamate-gated ion channels 50 ; in this form, areas such as basal ganglia (caudate, putamen, globus pallidus, substantia nigra, etc), cerebellum, and hippocampus display great number of receptors and consequently a higher endocannabinoid activity. 49 On the other hand, CB2 subtype is highly expressed in the overall immune system, with great density in B lymphocytes, but quantitatively decreasing in natural killer cells, microglia, and T lymphocytes. 56 Given such diverse distribution, the role of CB1 receptors is mainly associated with pain, inflammation, and many other responses, while CB2 receptors might have the potential as immunomodulators in various immune processes. As expected, these receptors possess an overall fixed structure of an extracellular N-terminus domain, 7 transmembrane α-helixes, and an intracellular C-terminus domain. Under the circumstances of ongoing immune processes, receptor activation stimulates the interaction with G proteins and ultimately upholds the Guanosine diphosphate/GTP exchange and further dissociation of the corresponding subunits. 49
Following the definition of the receptors, several molecules bind to CB1 and CB2 receptors and constitute ligands of endogenous or synthetic nature. Research efforts have led to the recognition and characterization of many molecules, and such progress has yielded a vast number of studies aiming to explore its potential under pathological defies. To date, 2 endogenous ligands of the CB system have been a matter of great interest: anandamide (AEA) and 2-arachidonylglycerol (2-AG). Both constitute elements of biological and physiological relevance under many circumstances, especially when considering that both are associated with the neurotransmitter-release inhibition through the adenylate cyclase inhibition. 57 Besides these molecules, other examples of endogenous ligands—and some data supporting its participation in significant biochemical events—include 2-arachidonylglycerol ether (noladin ether), 58 –61 N-arachidonyl-dopamine, 62 virodhamine, 63 and so on. On the other hand, the synthetic CB counterparts are frequently classified for its study. Such classification led in 2002 to a group of 4 components that remains valid nowadays: classic CBs (HU-210, 64 nabilone, 65,66 cannabidiol, 67,68 and other); nonclassic CBs (CP-47,497, 69,70 CP-55,244, 71 and CP-55,940 69 ), aminoalkylindoles (R-(+)-WIN 55,212-2, 72 and JWH-015 73 ), and eicosanoids (AEA 74 as the most notable as well as methanandamide 75 and arachidonoyl-2-chloroethylamide 76 ) to name a few, that account as synthetic eicosanoids. 77
Besides these main components, the ECS is enriched by a number of synthesis and degrading enzymes, transporter molecules, and minor intermediates that complete the arrangement. In this form, many molecular mechanisms take place in order to execute CB receptor signaling in anterograde and retrograde directions, as well as the corresponding cycles of synthesis, transport, and inactivation/degradation of CB agonists, which ultimately represent processes that are not entirely understood but yet remain enthralling and promissory.
Possible Neuroprotective Mechanisms of CBs in the Brain
The ECS was first recognized around the 80s, and emerging data have confirmed its relevance and intricate association with brain physiology and pathology ever since. As discussed previously, circuitry hierarchy of CB is settled with the CB1 (widely expressed in the CNS) and CB2 (both CNS and periphery) receptors, and the differential distribution points out the therapeutic potential of the ECS in neurological diseases. Although the constitutive expression of the receptors in the CNS plays a vital and consistent role in physiology, the inducible expression can also be provoked with prior inflammatory insult. Currently, the connection between the ECS and neurological diseases is not entirely understood; nevertheless, copious information proposes ECS’ hypofunction and overall dysregulation as the cause of some notorious symptoms of neurological diseases, especially when considering its neuroprotective and prohomeostatic functions, which drives the system as a whole to a potential link to mood and anxiety alterations, 78,79 major motor disorders such as PD or HD, 80,81 and other pathologies (Figure 1). Hence, most therapeutic approaches bet on pharmacological methodologies that alter the CB pathway or explore the endogenous increase in specific CB compounds that trigger desired responses.
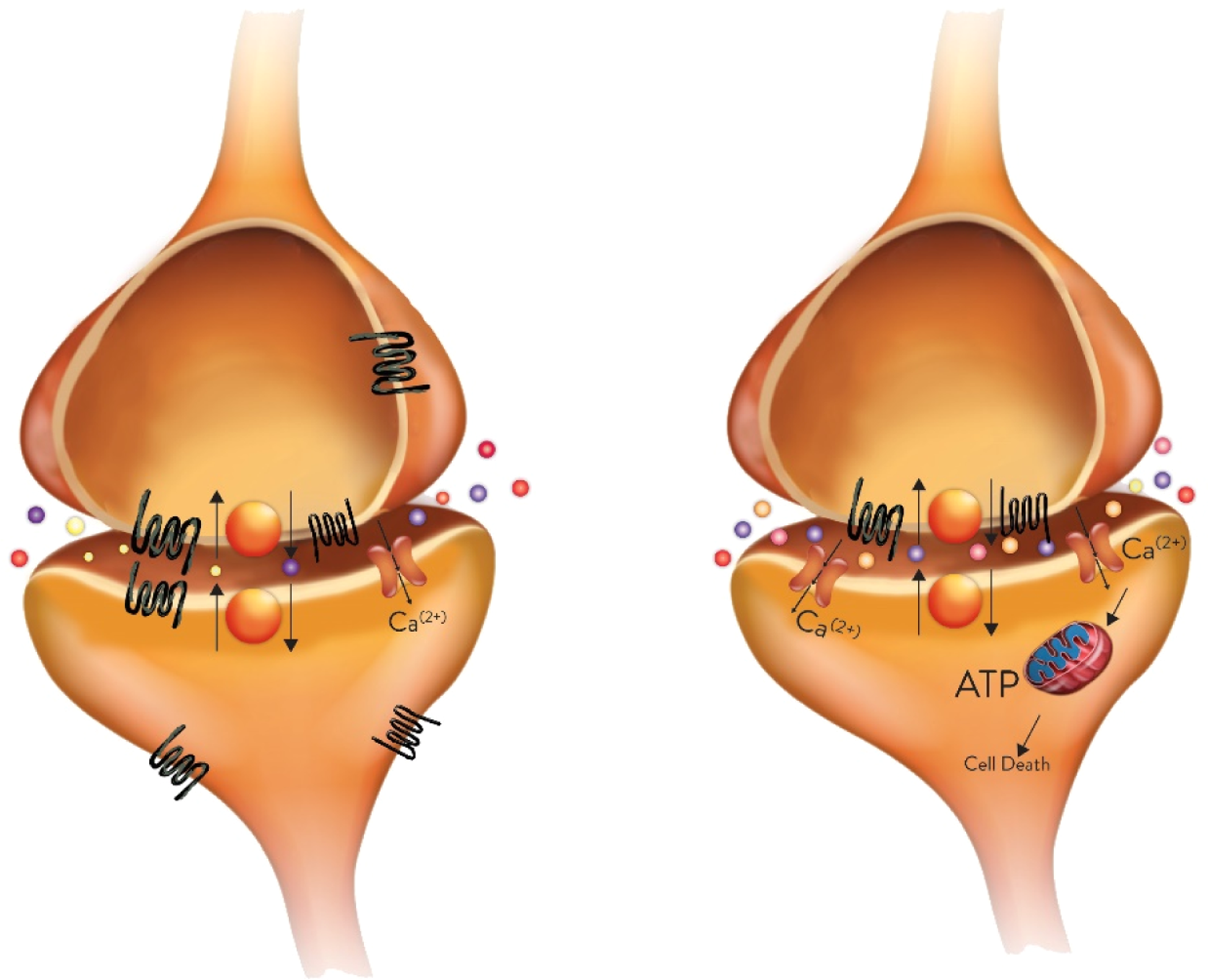
Alterations of the endocannabinoid system under pathological conditions. The image on the left is a conceptual representation of physiological conditions of pre- and postsynaptic neurons, with proportioned and functional CB1 (black) and CB2 (textured) receptors, transporters, and endogenous molecules such as anandamide (red dots), 2-arachidonoylglycerol (light yellow dots) and glutamate (purple dots). Conversely, the right image shows typical alterations of the endocannabinoid arrangement in pathological conditions, with fewer CB1 and CB2 receptors, decrease in the cannabinoid tone of anandamide and 2-arachidonoylglycerol, increase in glutamate levels, as well as the presence of glutaric (pink dots) and quinolinic (orange small dots) acids, 2 intermediates of metabolic pathways that may accumulate under pathological conditions and exert toxic effects. CB1 indicates cannabinoid receptor 1; CB2, cannabinoid receptor 2.
As mentioned previously, CBs exert its biological functions through the activation of CB1 and CB2 receptors. The 2 most noticeable CBs of endogenous nature include the AEA and 2-AG but also include diacylglycerol, diacylglycerol lipase, fatty acid amidehydrolase (FAAH), monoacylglycerol lipase, N-acylphosphatidylethanolamine, and so on. Moreover, AEA and 2-AG represent endogenous ligands released “on demand,” that subsequently suffer a hydrolysis process by the FAAH; consequently, the reduction in the normal levels of FAAH is associated with AEA concentration, which ultimately impacts the inhibitory effect of nociceptors. 82 Likewise, the neuroprotective assets of some endocannabinoids were first drawn from findings confirming that synthesis of AEA or 2-AG is Ca2+ influx dependent, implying therefore that endogenous CB tone would be determined as a response to intracellular calcium levels. 2 In this form, there is a precise distribution of CBs within the CNS and peripheral tissues, and together with the density of receptors and correlated molecules, the postactivation responses of ECS suggest the neuroprotective role of the CB matrix.
The state of knowledge of CB circuitry, along with its connection with pathological processes, discloses a great number of events that occur as part of the onset and progression of disease under many scenarios. As expected, the description of the involvement of CB signaling in pathological scenarios is currently engaged with the assessment of experimental data. Neurological diseases face challenging scenarios consisting essentially of lack of effectiveness of present pharmacological alternatives and limited emerging therapeutic proposals. Thus, the close relationship of these disorders and the ECS has directed attention to the exploration of CB chemistry to assess its antihyperkinetic, anti-inflammatory, and neuroprotective qualities through alternatives such as the effective expression of CBs, enhancement of CB synthesis, and so on, further leading to the control of motor activity and some other processes. 83,84 As a result, there is a special interest in the study of the risks and benefits implied in the use of CB-derived compounds in neurological pathology; in fact, motor-related disorders, neurodegenerative diseases, and some low-incidence pathologies show improvement under CB-administration schemes evidenced by the reduction of detrimental processes, such as excitotoxicity, oxidative stress, and inflammation. 57,81 This setup qualifies diseases from degenerative contexts such as AD, PD, and HD as ideal targets for experimental approaches but also reflects in disorders of low incidence—and rising awareness—such as OAs (GA-I, PAcidemia, MMAcidemia, etc). 85
Particular effects evoked after CB activation have attracted interest due to its advantageous applications. One of the most prominent is the antinociceptive response produced by CBs, which are mainly exerted through CB1 receptors. 86,87 Furthermore, such effects are taken to a new high when proposing the neuroprotective strategies of the CB elements in the brain. As known, the elucidation of the mechanisms that underlie the pathogenesis of neurological diseases constitutes exceptional dilemmas that therapeutics need to address. For example, a promissory finding applicable in neurodegenerative contexts involves the hypotheses in which cell survival, specifically neuronal type, is closely connected to the ECS, given that neuronal insult triggers repair mechanisms and endogenous production of CBs, such as AEA. 88 In fact, specific detrimental proteins present in neurodegenerative diseases (ie, Aβ) evoke localized and eventually general neuronal degeneration, which is also manifested in function impairment; then again, this deleterious conditions are reported to induce the production of endocannabinoids such as 2-AG, so that its neuroprotective qualities can be exerted. 89
Moreover, the ECS experiences downregulation of CBs as part of the hallmarks of some neurological diseases on early stages (usually previous to diagnosis), whereas advanced phases exhibit important receptor loss in the basal ganglia; in this form, both traits are consistent with initial hypokinetic manifestations versus advanced hyperkinetic symptoms experienced by patients in diseases such as PD or HD. 90,91 In addition, neurological pathologies of different nature show changes in the CB chemistry, as the alteration of receptors in purinergic signaling is known to be related to the decay of endocannabinoid level, thus reducing its protective qualities. 4
Potential Therapeutic Targets of the ECS in Neurodegenerative Disorders and OAs: Experimental Evidence
The aforementioned findings are currently under study with a therapeutic orientation, as the status of many neurological diseases highlights the relevance of the ECS in these pathologies. Research has led so far to great amount of information in regard to the ECS involvement in common neurological diseases such as AD, PD, MS, to name a few. Aside of the pathophysiological hallmark of AD, which has been addressed extensively, our knowledge of the participation of endocannabinoid elements has settled in several notions: Hippocampus expresses several subpopulations of CB1r, all of which contribute actively to the memory processes that suffer the deleterious effects during the neurodegenerative course of the disease. In fact, published works have stated the connection of neuronal cell survival and the CB chemistry. Such statements are possible given that such circuitry enables repair mechanisms to avoid or diminish oxidative injury or apoptotic events and could, in any given time, reduce the negative effects of molecules such as Aβ in AD. Moreover, the characteristic cognitive alterations due to hippocampal dent might be modulated by the ECS through anti-inflammatory and antioxidant means—and overall neuroprotective mechanisms—in this form, several experimental strategies explored the scopes and limitations of the ECS under the pathological hallmarks of AD and continue to provide valuable information in these regards.
88,89,92
Aside of the classical signs of AD, the overactivation of the N-methyl-
Progress has also been achieved in regard to some other neurodegenerative disorders. Notorious motor symptoms (dyskinesias, bradykinesia, tremor, rigidity, etc) accompany the development of PD; its disabling potential reduces dramatically the quality of life of the people facing the condition, reason why such symptoms constitute a major target of new therapies. As seen with some typical brain disorders, the ECS endures central alterations that occur along with the numerous degenerative processes of the disease; more precisely, early stages of PD—often presymptomatic—are associated with downregulation or desensitization of CB1r, which ultimately led to oxidative stress and excitotoxic/inflammatory events, while an upregulation of endocannabinoid agonists and receptors (CB1r specifically) is attained on advanced stages due to the influence of dopamine depletion on substantia nigra and, consequently, the striatum. 90 Under these circumstances, frequent proposals imply timely administration of molecules to inhibit the endogenous degradation of CBs in order to reduce the classic motor symptoms of PD. 94 Moreover, NMDAr antagonists are emerging as feasible options to mediate overactivation of such receptors, the consequent toxic events, and the cellular damage associated with it.
Contrasting hypotheses have risen in regard to MS, a disease that deals with severe immune attack and reportedly face a reduction in the CBs of endogenous nature as a result of the alteration of purinergic receptors 4 and, altogether, would contribute to the pathologic components of MS. The increasing awareness of CB potential has led to numerous preclinical evaluations exploring its properties, and even some advanced clinical studies following the same goal. As such, the improvement in disabling symptoms, such as spasticity and overall quality of life, might be achieved through synthetic CBs, given that such motor symptoms seem to be CB1r dependent 95 ; in fact, most of the explored applications suggest the administration of Cannabis derivatives to enhance endocannabinoid signaling. 96
As evident, these are examples of highly prevalent diseases of great interest in biomedical research, and their pathophysiological hallmarks are rather understood and studied acutely. However relevant, the awareness of and overall progress made in metabolic disorders have not shown such growth, and CB chemistry began to represent eventful alternatives only recently in this matter. The exploration of the potential modulation of some elements of the ECS and specific metabolic disorders just started to emerge and has been addressed only once with experimental purposes. In 2015, Colín-González and colleagues 85 published a synthetic approach used to evaluate the effect of a synthetic CB on early markers of some OAs, based on the understanding that its genesis comes with the convergence of events such as excitotoxicity and oxidative stress. In this form, the protective effects of WIN 55,212-2 (a synthetic CBr agonist) were evaluated in regard to its capacity to prevent oxidative damage, lipid peroxidation, decrease in antioxidant defense, and mitochondrial dysfunction, all of them being known early markers of metabolic diseases (GA, 3-OHGA, MMA, and PA as distinctive metabolites of the most typical metabolic disorders). The referred study led to interesting findings, as WIN 55,212-2 exhibited protective effects on markers related with GA-I and MMAcidemia, evaluated in terms of the prevention of mitochondrial dysfunction, formation of ROS, and lipid peroxidation in rat brain synaptosomes; the aforementioned findings support unequivocally the protective role of CBs in the toxic events present at early stages of OAs as a novel approach to assess the modulatory potential of CB compounds. 85 By the same authors, a second effort in publishing process confirmed the effective prevention of the toxicity induced by 3-MGA in brain synaptosomes elicited by low concentrations of WIN 55,212-2 when used as pretreatment (for as long as 30 minutes and prior to toxic insult). 97 Given the lack of experimental designs involving OAs and its toxic early metabolites, the future is headed toward the integration of the viable CB alternatives existing at this point into proficient experimental approaches to assess and exploit the effects of the modulation of the CB chemistry.
Concluding Remarks
As seen, the promissory character of CBs has shown remarkable properties that might enable the reduction in oxidative stress and a number of neuroinflammatory markers, while reestablishing brain homeostasis and restorative mechanisms contribute actively. In conclusion, therapeutic approaches adopting endocannabinoid strategies for common neurodegenerative diseases and even for a group of inherited metabolic disorders known as organic acidemias, that are characterized by severe impairment of the CNS. This approach may undoubtedly possess incalculable potential, and yet the necessity of additional research and conclusive data are imperative in order to clarify its participation in the pathological picture of such conditions.
Footnotes
Acknowledgments
The authors wish to express gratitude to Prof Moacir Wajner for his valuable comments and suggestions.
Declaration of Conflicting Interests
The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding
The author(s) received no financial support for the research, authorship, and/or publication of this article.
