Abstract
Background:
Elbow dislocation is the second most common large joint dislocation in athletes, frequently occurring in contact and high-impact sports such as football, wrestling, and gymnastics. While these injuries typically result from a fall onto an outstretched hand with the elbow in near full extension, both nonoperative and surgical treatments have demonstrated high success rates in restoring elbow function, enabling athletes to return to sport (RTS) with favorable functional outcomes.
Purpose/Hypothesis:
The purpose of this systematic review was to evaluate RTS rate, time to return, and functional outcomes in athletes following elbow dislocation. It was hypothesized that most athletes would successfully return to their sport regardless of treatment modality and that nonoperative treatment would be associated with a shorter recovery timeline compared with surgical intervention.
Study Design:
Systematic review; Level of evidence, 4.
Methods:
PubMed, Embase, Cochrane, and Web of Science were searched through March 20, 2025, for studies that investigated the management of elbow dislocation in athletes. Data were extracted on mechanism of injury, dislocation treatment, complications, follow-up duration, and outcome parameters, including RTS, return to the same level of play, time to return, and elbow outcome scores.
Results:
A total of 9 studies covering 970 athletes met the inclusion criteria for analysis. Across the studies that reported sex and age, 328 of 417 (78.7%) of the athletes were male, with a weighted mean age of 29.6 years. The mean follow-up was 72 months across the 5 studies that provided follow-up data. Across 8 of the 9 studies, 97 of 417 athletes with elbow dislocations (23.3%) underwent surgical treatment, while 320 received nonoperative management. Across 5 studies of 161 dislocations, only 18 cases (11.2%) resulted in complications. Return to any sporting activity, reported for 274 athletes across 7 studies, was observed in 99.3% of patients (n = 272/274) after a mean of 11.4 ± 7.7 weeks. On average, athletes treated nonoperatively returned sooner (8.95 weeks) than surgically treated athletes (16.3 weeks). Mayo Elbow Performance Score, Elbow Self-Assessment Score, and subjective elbow value scores demonstrated excellent elbow performance after injury.
Conclusion:
The results supported the hypothesis that athletes with elbow dislocation demonstrated excellent functional outcomes and high RTS rates, with most returning within 10 weeks. Most returned regardless of treatment, with nonoperative management generally associated with a shorter return timeline than surgical intervention.
Elbow dislocations are the second most common joint dislocation in adults, at 5.21 per 100,000 person-years, only following shoulder dislocations in frequency; in a pediatric population, elbow dislocations are the most prevalent.2,14,22 These injuries most often occur after a fall onto an outstretched arm with the elbow in near full extension or due to direct axial loading during high-velocity impact sports.12,14 Common mechanisms of injury include hyperextension and valgus stress to the elbow, which often present in sports such as football, wrestling, and gymnastics.6,19,22 Elbow dislocations are classified as either simple, involving no associated fractures, or complex, which includes concomitant fractures or significant soft tissue injuries. Simple dislocations are associated with more favorable outcomes, with one study citing all simple dislocations being successfully treated with closed reduction, compared with nearly half of complex dislocations requiring operative management. 19
Elbow stability is maintained by its bone structure and surrounding soft tissues, specifically the ulnohumeral joint, ulnar collateral ligament (UCL), lateral collateral ligament (LCL), and joint capsule.1,4 The severity of elbow dislocation varies widely and influences treatment decisions. Nonoperative management, which typically involves joint reduction, brief immobilization, and early range of motion therapy, is often preferred for simple dislocations, especially in patients without signs of chronic instability.3,11,19 In more complex cases, surgical treatment may be justified in patients with persistent instability, soft tissue damage, or following failure of nonoperative care.13,21 Recent evidence supports this approach, showing that early mobilization following nonoperative treatment results in favorable range-of-motion and performance outcomes, while achieving clinical results comparable with surgery in appropriately selected patients. 3 Both approaches aim to restore joint function and minimize complications, with the goal of optimizing the return to sport (RTS) recovery time.
Prior studies also suggest that RTS outcomes following elbow dislocation are generally favorable. One study reported that recreational athletes demonstrated high functional scores and a strong likelihood of returning to preinjury sport, with no significant differences in RTS rates between operative and nonoperative groups. 17 Similarly, literature suggests that simple elbow dislocations typically permit early range of motion and early return to play, even in high-level contact athletes, and notes that most athletes return without significant long-term limitations. 15 Together, these findings suggest that athletes commonly resume sport after elbow dislocation, supporting the expectation of high RTS rates in this population.
Despite growing literature supporting excellent prognosis and functional recovery following elbow dislocation, 4 RTS outcomes remain inconsistently reported. There is a need to better understand the timeline, success rates, and complications associated with elbow dislocation, particularly in athletic populations. We hypothesized that most athletes would achieve high functional outcomes and successfully RTS regardless of treatment modality and that nonoperative management would be associated with a shorter RTS timeline compared with surgical intervention. This systematic review aimed to assess return to activity, functional outcomes, and complication rates following elbow dislocation by synthesizing current evidence on nonoperative and surgical management.
Methods
Literature Search
A systematic search was conducted in PubMed, Embase, Cochrane, and Web of Science through March 20, 2025. The search strategy used combinations of the following terms: “elbow dislocation,”“athletes,”“return to sport,”“conservative treatment,” and “surgical management.” The review followed PRISMA (Preferred Reporting Items for Systematic Reviews and Meta-Analyses) guidelines. Full details on the search strategy and preliminary results can be found in Appendices 1 to 4. The literature search and subsequent review were conducted in accordance with PRISMA reporting standards.
Eligibility Criteria and Study Selection
Two reviewers (A.S.A., A.K.C.) initially screened titles and abstracts, and studies were included if they reported on RTS outcomes following elbow dislocation, assessed treatment methods (surgical versus nonsurgical) and their impact on RTS, and provided quantitative outcomes such as time to return, functional scores, or complications. Studies were excluded if they were cadaveric, not in English, or categorized as reviews, technical notes, case reports, letters to the editor, or surgical technique papers. Additionally, studies that did not report RTS outcomes were excluded from the analysis. Studies underwent a second round of full-text screening based on the same criteria to exclude additional studies as needed. Any conflicts between reviewers were resolved through third-party consultations with a senior author (N.R.K).
Methodological Quality Assessment
Methodological quality and risk of bias of included studies were assessed using the JBI protocol checklist for cohort studies, case series, and prevalence studies. Each criterion consisted of unique vetting questions that evaluated the validity of methods, appropriateness of analysis, and quality of presentation for the respective study type. Two reviewers (A.S.A., A.K.C.) reviewed each included study. Any discrepancies were settled by a third reviewer (N.R.K.).
Data Extraction
Two authors (A.S.A. and A.K.C.) shared responsibility for data extraction, with each reviewer independently extracting data from half of the included studies into a spreadsheet. After completing their assigned portion, each reviewer then cross-checked the other's extracted data. Any discrepancies identified during this secondary review were resolved through discussion with a senior author (N.R.K.). Variables collected included patient demographics, treatment approach, RTS rate and timing, return to the same level of play, complications, follow-up duration, and clinical elbow outcome scores.
Statistical Analysis
Categorical variables were summed and presented as counts or proportions, and continuous variables were computed for patient means. Outcomes of interest were tabulated to highlight the findings of individual studies. A meta-analysis was not performed due to heterogeneity in patient demographics, sport type, outcome measures, and RTS definitions.
Results
Literature Search and Screening
An initial literature search through Covidence yielded 438 articles, which, after removal of 90 duplicates, led to a total of 348 unique records for title and abstract screening. Of these, 302 studies were excluded as irrelevant. The remaining 46 articles were assessed at the full-text level, with 37 subsequently excluded for not meeting the inclusion criteria, resulting in 9 studies included in the final analysis (Figure 1).
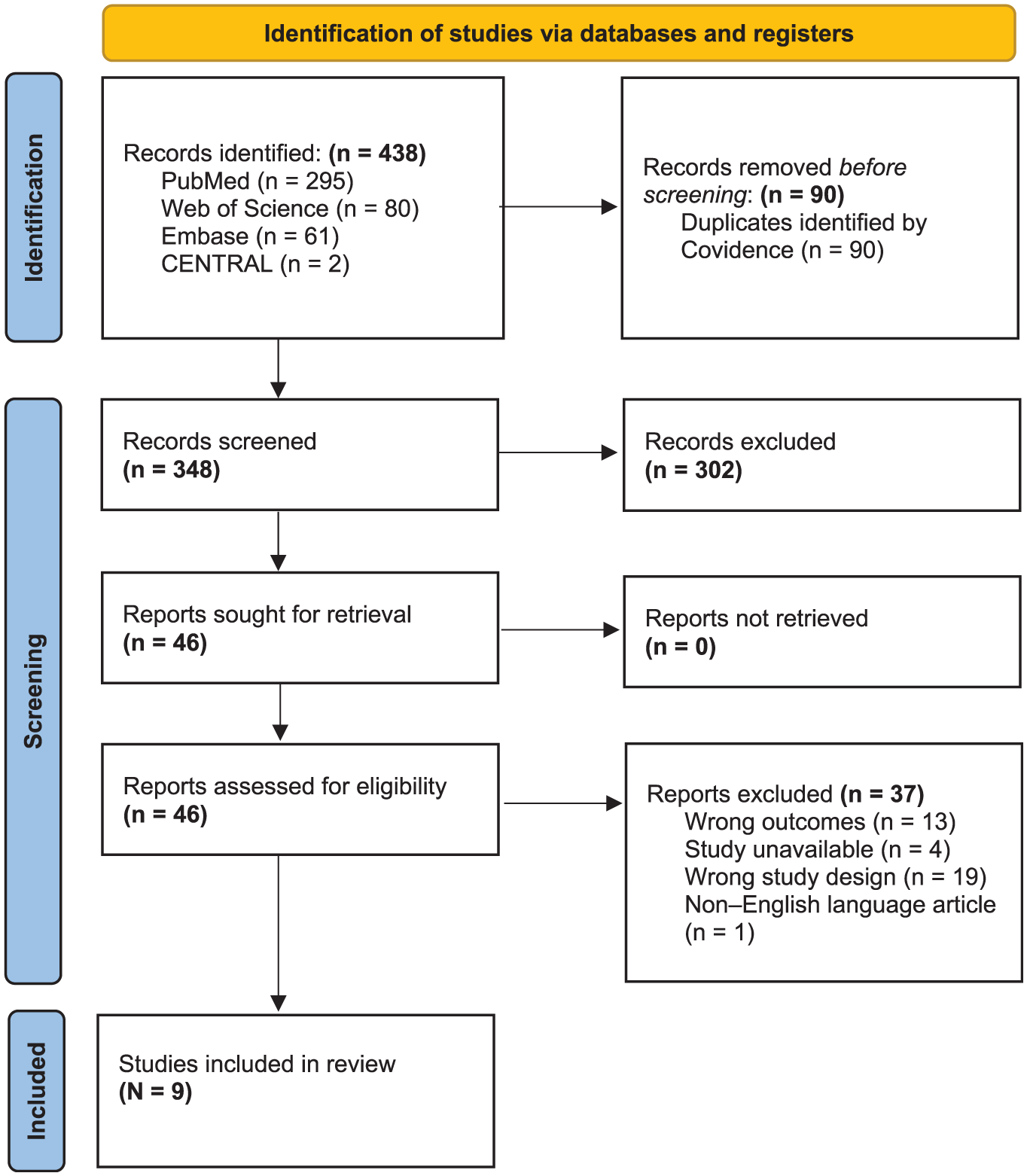
PRISMA (Preferred Reporting Items for Systematic Reviews and Meta-Analyses) 2025 flow diagram for systematic review literature search and screening.
Methodological Assessment
Initial risk of bias assessment showed that 4 cohort studies had a mean score of 8.5 out of 11.8,16,17,20 Two case series scored a mean of 7.5 out of 10,5,18 and 3 prevalence studies scored a 9 out of 9.7,9,10 All studies were deemed suitable for inclusion in this review.
Patient Demographics and Injury Mechanism
A total of 9 studies encompassing 970 athletes met the inclusion criteria. Of the 9 studies, 8 reported sex and 6 reported age; across these, the weighted mean age was 29.6 years, and 328 (78.7%) of the athletes were male. The mean follow-up across studies was 72 months. Among studies that reported the mechanism of injury, 99% of elbow dislocations resulted from contact injuries, mainly with opponents or equipment during gameplay. Other mechanisms, such as falls from height during bouldering or horseback riding, were less common.16,18 The included athlete populations spanned a wide range of competitive levels, from recreational athletes to elite professionals. Specifically, 4 studies included recreational athletes, 1 focused exclusively on high school athletes, 1 investigated collegiate-level athletes, and 2 included professional National Football League athletes. O’Brien et al 18 were unique in their use of “high-demand patients,” which included both athletes and individuals who worked with their hands, such as surgeons and construction workers. These non-athlete individuals were not included in our analysis (Tables 1 and 2).
Study Details, Patient Demographics, and Follow-up a

Data are presented as n (patients, sex), mean, or mean ± SD (age, follow-up). Dashes indicate that no data were available for extraction.
Sport, Mechanism of Injury, Dislocation Treatment, and Complications a

Dashes indicate that no data were available for extraction. HS, high school; JV, junior varsity; NCAA, National Collegiate Athletic Association; NFL, National Football League; NOT, nonoperative treatment; ST, surgical treatment.
Management and Complications
Across 8 of the 9 studies, 97 of 417 athletes with elbow dislocations (23.3%) underwent surgical treatment, including ligamentous repairs for ruptures of the LCL and UCL, as well as radial ulnohumeral ligament (RUHL) repair for posterolateral rotatory instability.8,16,17,18 In the subset of 5 studies that reported complication data for 161 dislocations, adverse outcomes were relatively uncommon, occurring in only 18 cases (11.2%). Out of the 161 dislocations with available complication data, one patient (0.6%) developed heterotopic bone formation after arthroscopic repair of the RUHL, 18 and 3 (1.8%) experienced persistent stiffness and instability. 16 When complications were stratified by treatment type, 11 complications (6.8% of the 161 dislocations) occurred in the surgical group8,17,18 and 4 (2.5%) in the nonoperative group.8,20 Three (1.9%) complications reported by Mueller et al 16 did not specify whether they occurred in the surgical or nonoperative treatment group (Table 2).
Outcome Scores, RTS, and Treatment Type
For this review, RTS was defined as any resumption of participation in the athlete's preinjury sport, regardless of whether he or she returned to the prior level of performance. Because of variability in how RTS was reported across studies, only those that provided explicit quantitative data were included in the final analysis. Seven out of the 9 studies met this criterion. Within this subset, RTS was observed in 99.3% of athletes (n = 272/274), with a mean return time of 11.4 weeks.
Among nonoperatively treated patients, RTS was 100% (n = 196/196), while for surgically managed athletes, 97.4% (76/78) returned to sport. When broken down by treatment type, athletes who underwent operative treatment had a longer recovery period, averaging 16.3 weeks, compared with 8.95 weeks for those managed nonoperatively (Table 3).
Return to Sport Metrics a
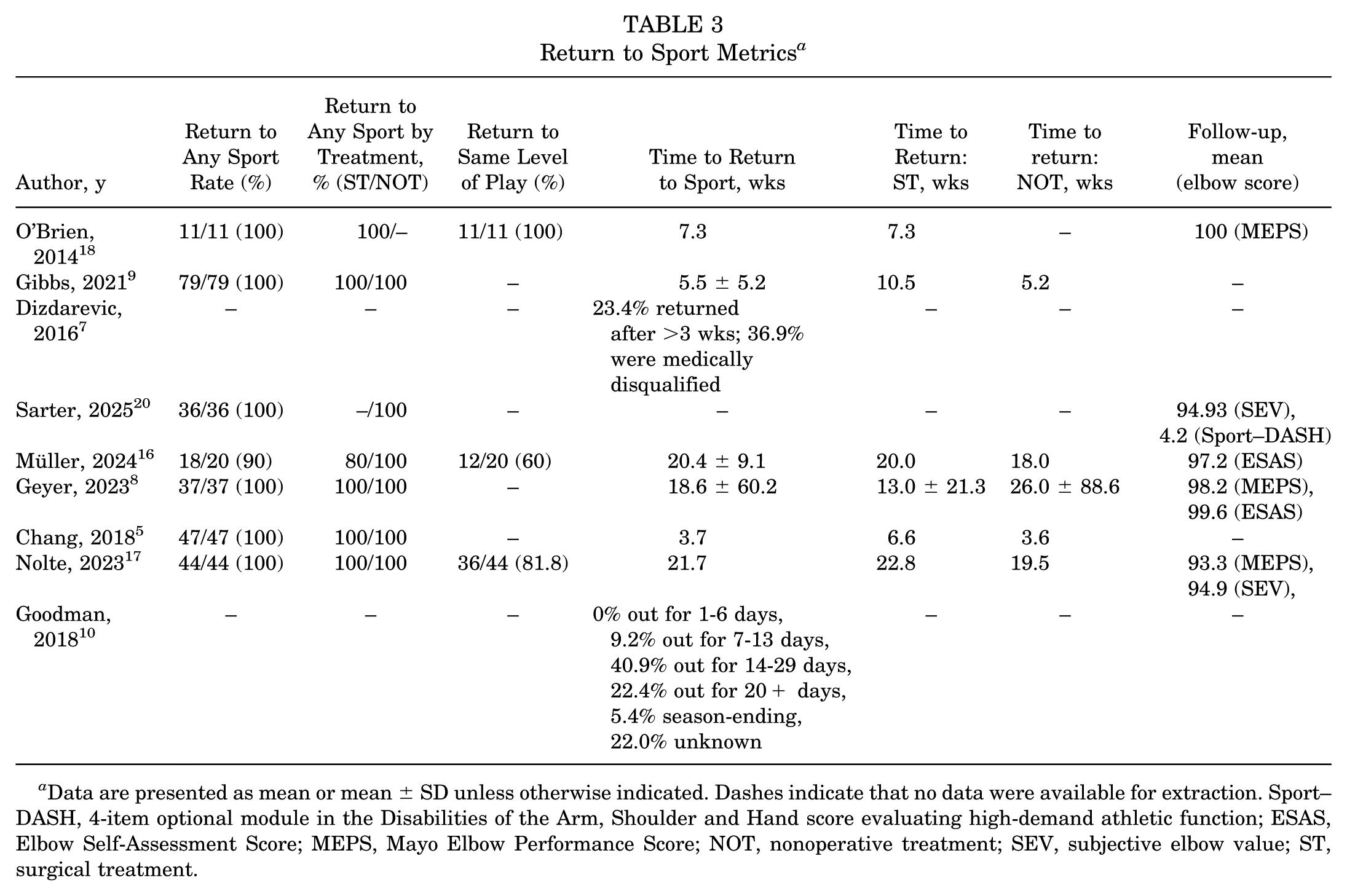
Data are presented as mean or mean ± SD unless otherwise indicated. Dashes indicate that no data were available for extraction. Sport–DASH, 4-item optional module in the Disabilities of the Arm, Shoulder and Hand score evaluating high-demand athletic function; ESAS, Elbow Self-Assessment Score; MEPS, Mayo Elbow Performance Score; NOT, nonoperative treatment; SEV, subjective elbow value; ST, surgical treatment.
Return to the same level of play was reported in 3 of the 9 studies, with rates ranging from 60% to 100%. Clinical outcome scores demonstrated excellent elbow performance. Across applicable studies, the weighted mean Mayo Elbow Performance Score (MEPS), Elbow Self-Assessment Score (ESAS), and subjective elbow value (SEV) scores were 96.07, 98.76, and 94.91, respectively (Table 3).
Discussion
This systematic review demonstrates that athletes who sustained elbow dislocations returned to sports at exceptionally high rates, approaching 100%, with a mean recovery time of approximately 10 weeks. Both surgical and nonoperative interventions resulted in low complication rates and favorable long-term outcomes, although surgery was associated with a slightly higher rate of complications and a prolonged recovery period. These findings were accompanied by high outcome scores, reflecting excellent postinjury elbow function.
The MEPS, ESAS, and SEV all use a 0 to 100 scale, with higher scores indicating less pain, better mobility, and stronger perceived function. Athletes generally recovered near-complete elbow performance following elbow dislocation, regardless of treatment approach. The consistently high elbow function scores, even years after injury, reinforce that elbow dislocations, when managed appropriately, do not tend to impair long-term joint performance in athletes.
Despite the high RTS rate, variability exists in reporting return to preinjury level, with some studies lacking performance metrics or clarity regarding athletic level. Importantly, this review focused only on RTS outcomes from individuals who were reported as physically active or participating in sport before injury. Several studies distinguished between return outcomes based on preinjury activity level, underscoring that RTS data reported here should be interpreted specifically in the context of previously active populations.8,20
While most athletes in this review returned to sport, few studies distinguished between returning to any participation in the same sport and returning to the same level of play, the latter being a more clinically meaningful benchmark for competitive athletes. Among the studies that reported return to preinjury level, rates ranged from 60% to 100%, including 60% in the bouldering athletes in Müller et al, 16 81.8% in Nolte et al, 17 and 100% in O’Brien et al. 18 Although these findings are encouraging, limited and inconsistent reporting limits definitive conclusions regarding return to prior competitive level. Future studies should distinguish between general return to participation and return to preinjury performance level to better inform athlete expectations and clinical decision-making.
RTS data offer valuable guidance for both athletes and physicians when determining the most appropriate treatment approach for elbow dislocation and setting expectations for recovery. For athletes, especially those on a professional level, understanding the typical timeline to resume athletic activity can aid in planning and goal setting. These kinds of data will help establish realistic expectations and facilitate honest conversations with patients about recovery.
For physicians and sports teams, RTS metrics provide important insight into how various treatment modalities will affect outcomes. Additionally, understanding the shorter recovery time and lower complication rates associated with nonoperative treatment can help guide its use in less severe cases. In contrast, recognizing the limitations of nonoperative management may support surgical intervention for high-demand athletes or those with more complex injuries. Two studies in particular by Geyer et al 8 and Nolte et al 17 highlighted important nuances in the relationship between treatment type and complications. Geyer et al reported a complication rate of 21.7% among surgically treated patients, the highest in our review. However, these patients also demonstrated a significantly faster RTS compared with those managed nonoperatively, with a mean of 13 weeks compared with 26 weeks (P = .036). 8 Patients with higher athletic demands or more extensive ligamentous damage were more likely to undergo surgical treatment, which may partially explain both the increased complication rate and the expedited recovery. Nolte et al observed a complication rate of 11.4% in the surgical group, with all complications occurring in surgically treated patients. Nonetheless, the study found no statistically significant difference in RTS rates between nonoperative and surgical treatment groups, further suggesting that complication rates may reflect underlying injury severity rather than treatment modality alone. This suggests that nonoperative treatment may facilitate a quicker RTS, although treatment selection is dependent on injury severity and individual factors.
A formal meta-analysis was not performed because of heterogeneity in patient demographics, sport type, outcome measures, and RTS definitions. This diversity in athletic level enhances the generalizability of findings but also contributes to variability in treatment decisions, expectations for return, and rehabilitation protocols.
Ultimately, these RTS data provide meaningful clinical insight that goes beyond traditional functional scores and helps ensure treatment strategies align with the goals of the athlete.
Limitations
This review was subject to several limitations that collectively hinder the ability to establish definitive comparisons between treatment modalities or to generalize RTS across diverse athletic populations. First, there was significant heterogeneity in the types of sports and athlete competition levels studied, ranging from recreational athletes to elite professionals. These differences likely influenced rehabilitation expectations, timelines, and access to care, complicating direct comparison and generalizability. Additionally, variation in reporting methods for RTS limited quantitative synthesis. Several studies did not provide exact timelines or metrics for RTS, and some focused more broadly on injury incidence or general outcomes.
Additionally, some studies only reported RTS outcomes for athletes with shorter recovery timelines, such as only those athletes who returned within the same season. 5 As a result, athletes injured near the end of the season who could not return before its conclusion, or those with longer recovery timelines, were excluded from the analysis. This potentially underestimated true return duration and highlighted the importance of comprehensive long-term follow-up.
Another source of variability stemmed from the proportion of patients undergoing surgical versus nonoperative treatment in each study. Some studies had disproportionately high numbers of patients in one treatment group, which may have skewed outcomes and limited comparison across treatment modalities. Furthermore, more complex injuries and higher-demand athletes were more likely to undergo surgery, potentially biasing RTS outcomes and complication rates. These treatment allocation differences were often based on clinical judgment rather than randomization, introducing potential selection bias.
Conclusion
Athletes with elbow dislocation demonstrated a strong RTS rate of >99%, with most returning within approximately 10 weeks of injury. Both nonoperative and surgical treatments were effective, with low complication rates and excellent functional scores. Nonoperative management was generally associated with a quicker RTS, which likely reflects its use in simpler and more stable injuries. In contrast, surgical treatment may be more commonly employed for cases with greater instability or associated structural damage. These findings can help guide RTS protocols and support clinicians in setting realistic expectations for recovery.
Footnotes
Appendices
Search Strategy for Web of Science

| ID | Strategy | Hits |
|---|---|---|
| 1 | TS=((elbow or elbows or ulnohumeral or radiohumeral or humeroulnar) NEAR/3 (dislocat* or instability or subluxation or unstable)) | |
| 2 | TS=(return NEAR/3 (sport or sports or play or activity or activities or participation)) | |
| 3 | 1 AND 2 | 80 |
Final revision submitted November 2, 2025; accepted December 20, 2025.
The authors have declared that there are no conflicts of interest in the authorship and publication of this contribution. AOSSM checks author disclosures against the Open Payments Database (OPD). AOSSM has not conducted an independent investigation on the OPD and disclaims any liability or responsibility relating thereto.
