Abstract
Objectives:
MPFL reconstruction is currently the most popular surgical approach for patellar stabilization following patellar dislocations. While many studies report outcomes following MPFL reconstruction, the characteristics of the patient population and injured knee influencing patient satisfaction are not well characterized. The current study was performed to identify factors influencing patient satisfaction at one year following MPFL reconstruction from demographics, anatomy, characteristics of the injury, and pre-operative assessment of function.
Methods:
The study used an institutional database for characterizing outcomes at one year following knee surgery initiated in 2015. The primary outcome measures used to characterize knee function are the Knee Injury and Osteoarthritis Outcome Scores (KOOS) and Veterans Rand 12 Item Health Survey (VR-12). The database prospectively captures more than 90% of patients at the time of surgery. Analysis focused on patients of any age in the database treated with unilateral MPFL reconstruction though July 31, 2022. Patients were excluded for prior knee surgeries unrelated to patellar stabilization, injuries to other ligaments of the knee, and any procedures that included bone osteotomies, such as tibial tuberosity realignment. Patients were not excluded for soft tissue procedures in combination with MPFL reconstruction, such as lateral retinacular release or advancement of the vastus medialis obliquus. The dataset included 143 subjects evaluated from 365 to 615 days following MPFL reconstruction, capturing approximately 50% of the patients who participated at the time of surgery.
Data collected for each subject included sex, age and body mass index at the time of surgery. Smoking status was categorized as never smoked or a history of smoking. Athletic status was characterized based on self-identification as an athlete or non-athlete at the time of surgery. Presence of a loose body was recorded. Trochlear dysplasia was recorded as none vs. any grade of dysplasia. Patella alta was characterized based on Caton-Deschamps index for categories of < 1, 1-1.19, 1.2-1.4, and > 1.4. Cartilage at the time of surgery was characterized for the patella as normal vs. any grade of cartilage degradation. Autograft vs. allograft was also recorded. Knee function and overall health were recorded at the time of surgery and at follow up based on the pain, physical function, and quality of life components of the KOOS and the physical and mental health components of the VR-12. Pre-operative to post-operative differences in outcome scores were also quantified. Patient satisfaction at least one year after surgery was based on the question: “Taking into account all the activity you have during your daily life, your level of pain and also your activity limitations and participation restrictions, do you consider the current state of your knee satisfactory?”.
Multivariable binary logistic regression was used to identify factors associated with patient satisfaction. One analysis focused on all parameters collected at the time of surgery to identify potential predictors of patient satisfaction. The other analysis focused on outcome measures collected at follow up to identify those most closely linked to patient satisfaction. Statistical significance was set at p < 0.05.
Results:
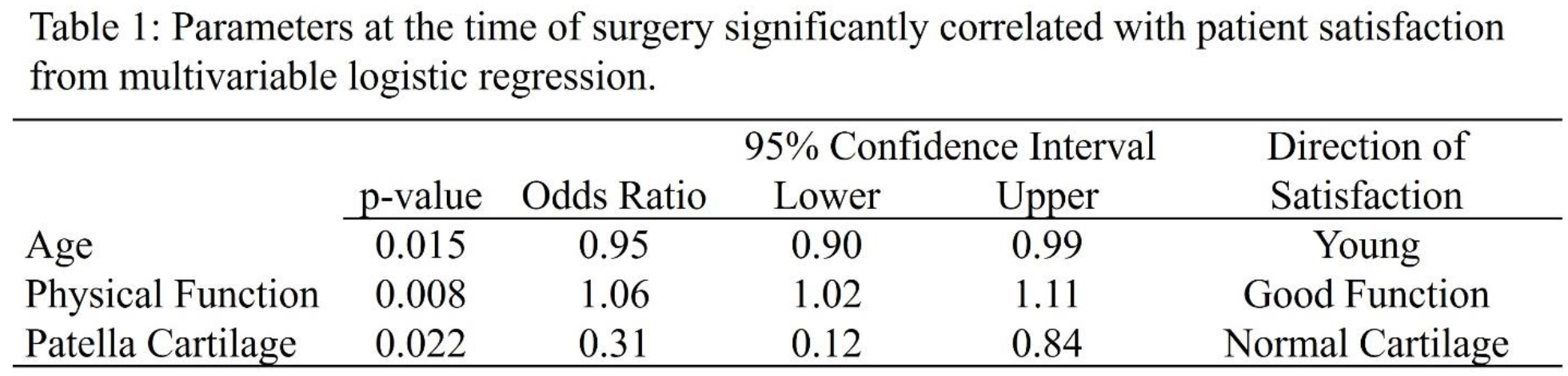
The average age and BMI (± standard deviation) of the patient population were 21.3 ± 8.6 years and 26.4 ± 6.5 kg/m2, respectively. The population included 96 females and 47 males. Pre-operative factors significantly correlated with patient satisfaction individually were age, smoking status, cartilage status, KOOS pain, KOOS physical function, VR-12 mental health and VR-12 physical health. For the multivariable regression, the final factors significantly correlated with satisfaction were age, physical function, and cartilage status, with lower age, better physical function, and normal cartilage associated with patient satisfaction at follow up (Table 1). The coefficient of determination was 0.23 based on the Nagelkerke r2.
All post-operative outcome scores were individually related to patient satisfaction other than pre-operative to post-operative changes in the VR-12 mental and physical health scores. For multivariable regression, the only parameter correlated with patient satisfaction was high KOOS quality of life at follow up (Table 2). The coefficient of determination was 0.47.
Conclusions:
Based on the current results, the primary indicators of patient satisfaction at one year following MPFL reconstruction are young age, normal patellar cartilage, and good physical function at the time of surgery. Information on the characteristics of patients most likely to be satisfied following surgery is valuable for treatment planning and educating patients. The results also indicate that patient satisfaction at one year following surgery is most closely associated with the subjective assessment of quality of life related to the injured knee. Understanding the characteristics that make patients satisfied with their outcome is also valuable for treatment planning and patient education to maximize satisfactory outcomes.