Abstract
Objectives:
The menisci play a critical role in knee stability, proprioception, lubrication and distribution of axial force in hoop like stresses. Medial meniscus posterior root tears (MMPRT) are a distinct category of meniscal tears defined as a radial tear within 10mm of the posterior horn attachment or either a bony / soft tissue avulsion of the posterior root. These injuries have become an increasingly recognized pathology due to biomechanical evidence indicating that disruption of the meniscus attachment alters joint mechanics, resulting in tibiofemoral contact pressures comparable to those of a total meniscectomy. As such, meniscus root tears have been implicated in degenerative cartilage changes and rapidly progressive knee osteoarthritis (OA). Notably, prior literature has indicated that 92.8% of adults who underwent a total knee replacement under the age of 60 had an associated meniscus root tear, further emphasizing the deleterious effects of this pathology previously referred to as a ‘silent epidemic’.
Traditionally, the management of MMPRT has involved nonoperative approaches or partial meniscectomy. However, nonoperative management has yielded unsatisfactory outcomes, with 31% of adults undergoing total knee arthroplasty (TKA) within a mean follow-up period of 30 months. Emerging evidence underscores transtibial pull-out repair as an effective surgical treatment for these injuries. Although it may not entirely prevent cartilage degradation, transtibial pull-out repair significantly decelerates OA progression compared to meniscectomy and nonoperative management at mid-term follow-up. Moreover, it has been demonstrated to be a cost-effective alternative to meniscectomy and non-operative approaches for managing MMPRT.
The purpose of this study was to report on patient-reported outcome measures (PROMs), reoperation rate, and failure rate for patients undergoing transtibial pull-out repair for isolated medial meniscus posterior root tears at a minimum of 5-year follow-up. The authors hypothesized that at mid-term follow-up, patients undergoing root repair will exhibit low rates of conversion to knee arthroplasty and high rates of MCID and PASS achievement.
Methods:
A single institution prospectively collected database was retrospectively queried for patients with isolated medial meniscus posterior root tears who underwent transtibial root repair from January 2016 to March 2019. Exclusion criteria included concurrent ligamentous or realignment procedures, all-inside suture anchor repair and concomitant lateral meniscus tears. Structural failure was defined as conversion to knee arthroplasty. Clinical failure was defined as patients who did not achieve MCID for at least one of 3 PROMs. Primary outcome measures included MCID and PASS achievement for KOOS Jr. in addition to the rates of structural and clinical failure. Secondary outcome measures included MCID and PASS achievement rates for International knee documentation score (IKDC) and Veterans Rand 12 Items Health Survey (VR 12) in addition to reoperation and complication rates.
Results:
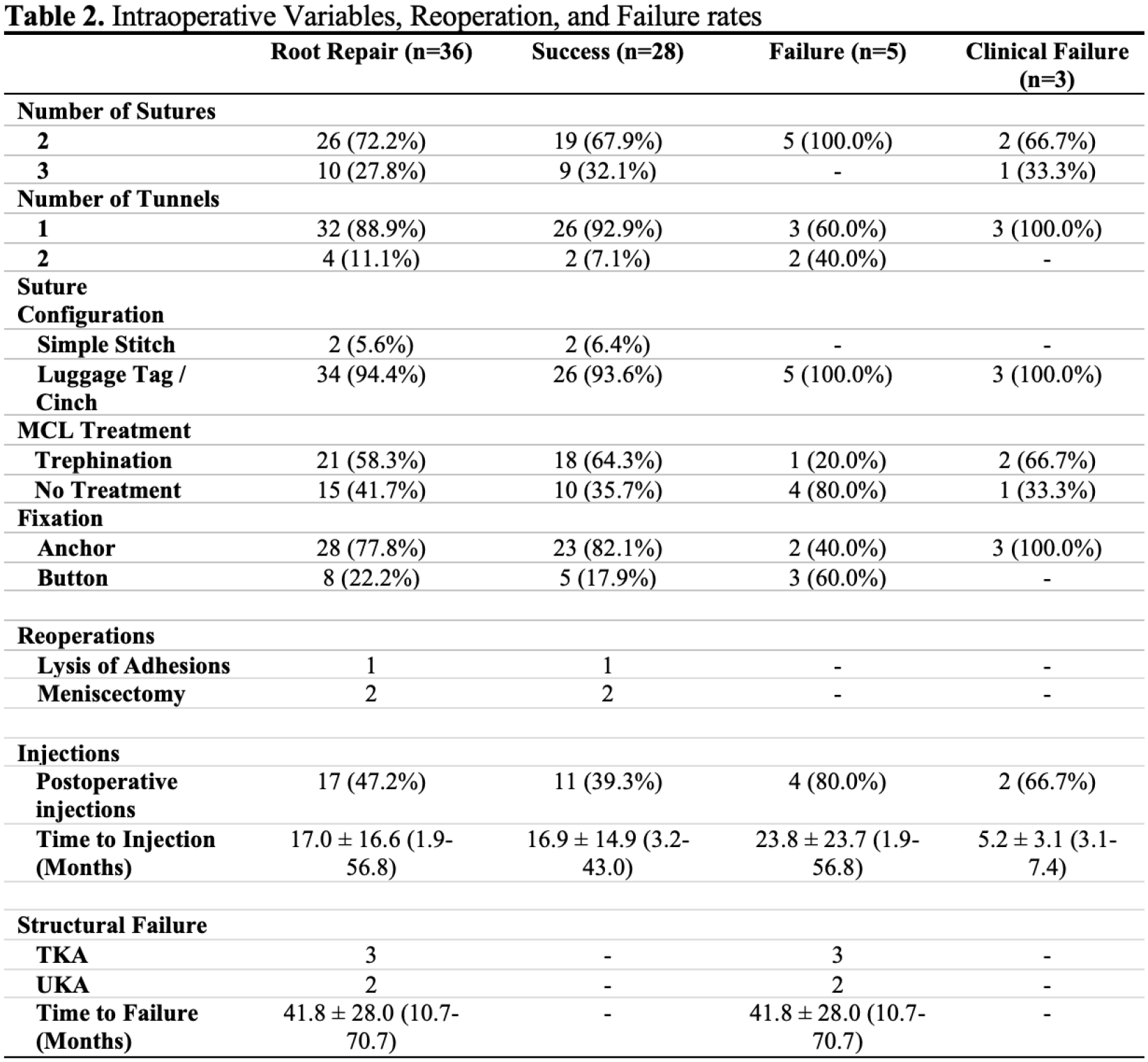
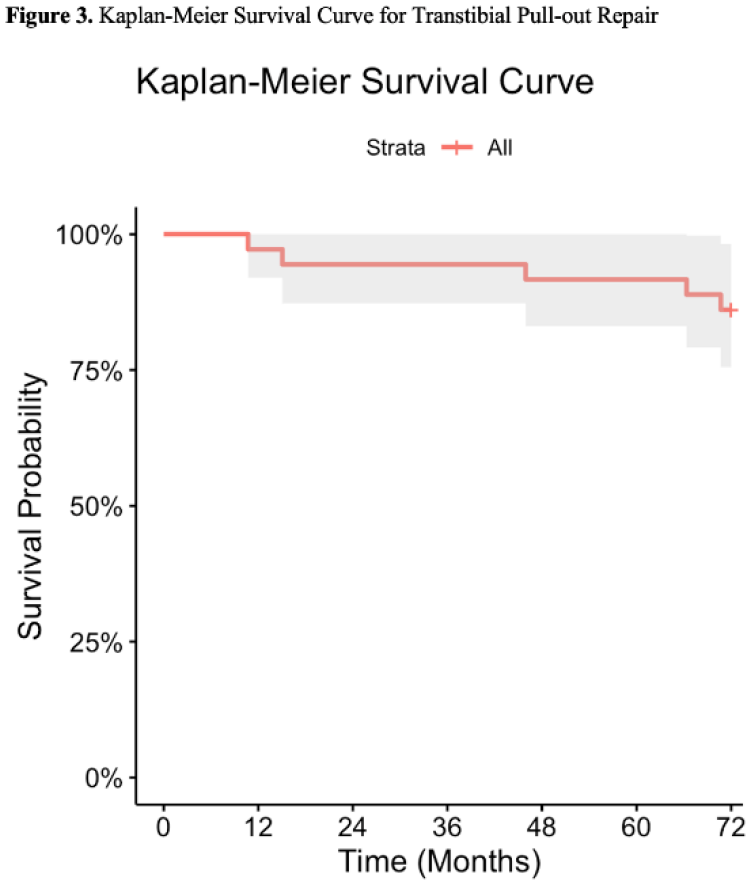
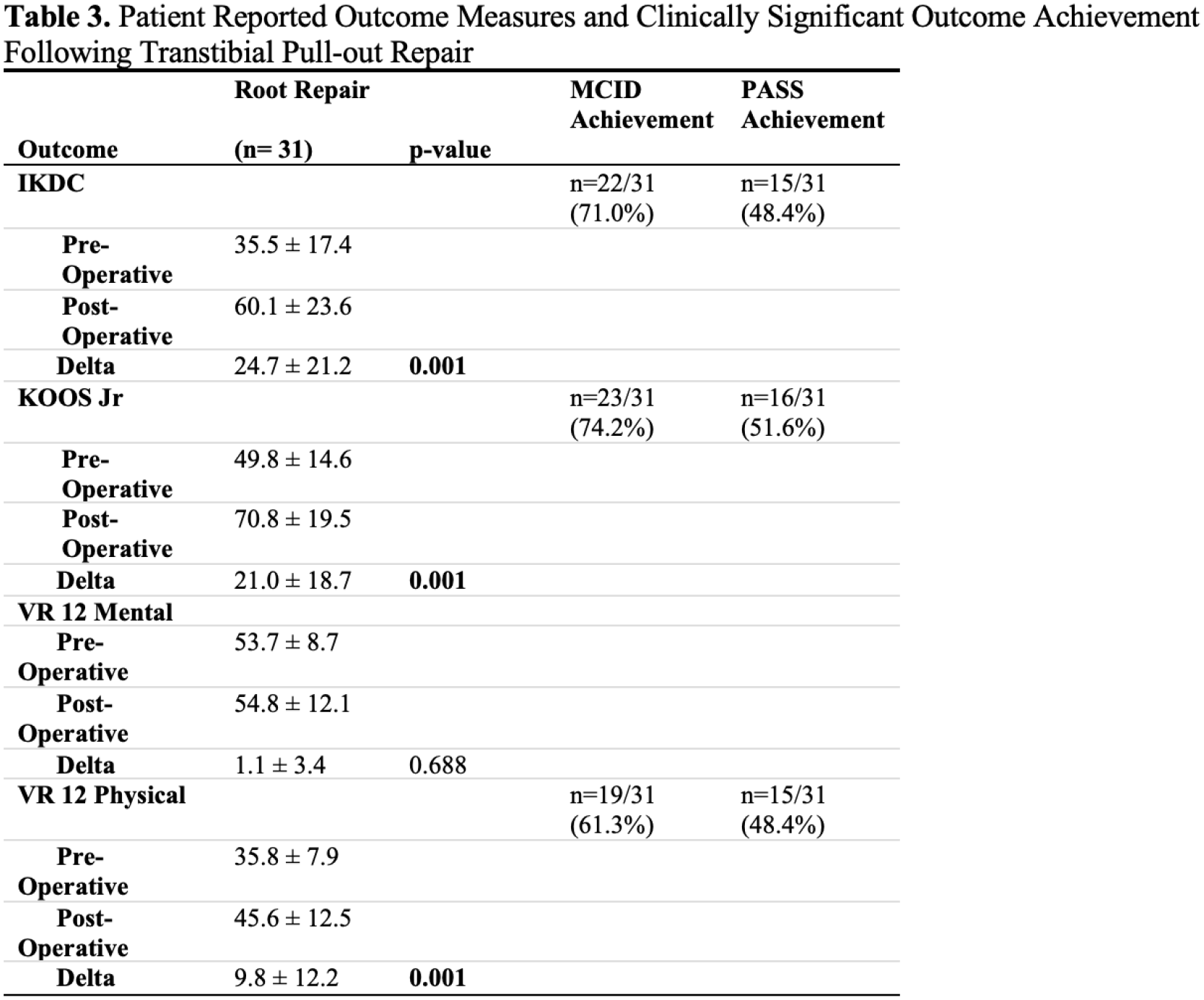
Thirty-eight patients who met inclusion criteria and underwent transtibial root repair prior to March 2019 were retrospectively identified, of which 36 (94.7%) were available for follow-up (Figure 1). Five patients (13.9%) converted to arthroplasty (mean 41.8 ± 28.0 months) (Figure 2). Transtibial pull-out repair had an overall survivorship of 97.2%, 94.4% and 91.6% at the 1-year, 2-year and 5-year timepoints while 2 patients failed after 60 months postoperatively for an 86.1% arthroplasty free survivorship at mean 65.8 months (Figure 3). MCID and PASS achievement rates at final follow-up for KOOS Jr were 74.2% and 51.6%, respectively (Figure 4). Three patients (8.3%) failed to achieve MCID for any one of 3 PROMs while 28 patients (77.8%) achieved MCID for at least one PROM.
Conclusions:
Clinically significant outcomes for osteoarthritis index scores were achieved in 74.2% of patients undergoing transtibial pull-out repair for isolated medial meniscus posterior root tears at 5-year follow-up. There was a 86.1% survivorship free of arthroplasty at mid-term follow-up.