Abstract
Objectives:
To develop a 3D Patellar instability Anatomical Severity Score (3D-PASS) that is associated with a history of instability and post-treatment outcomes.
Patellar instability treatment outcomes are variable. A third of patients who receive non-operative treatment re-dislocate, and 58% experience activity limitations 6 months after injury. Accurate prediction of treatment outcomes of conservative versus operative management would support personalized interventions to improve results.
Treatment decisions are currently based on clinical factors and anatomical information from 2D x-ray and magnetic resonance image (MRI) measures that reflect patellar tilt, patella alta, trochlear dysplasia, and the tibial tubercle–trochlear groove (TT-TG) distance. While these measures are associated with patellar instability, they do not leverage the 3D bone information captured by MRIs. This information may enhance understanding of patellar instability and its treatment.
Methods:
This study retrospectively analyzed 272 patients from the multi-center JUPITER (Justifying Patellar Instability Treatment by Results) study and 26 age-matched controls with ACL injury. Patellar instability was classified as first-time or recurrent based on history at study enrollment. Treatment decisions (non-operative or operative) were made by patients and their clinicians based on standard of care.
MRIs and x-rays were collected at study enrollment. Patellar tilt, Caton-Deschamps Index (CDI), sulcus angle, and TT-TG distance were measured. Patients completed the Kujala Anterior Knee Pain Scale (Kujala) and Banff Patellofemoral Instability Instrument 2.0 (BPII 2.0) at baseline and one year after enrollment.
To quantify 3D bony knee anatomy, we developed a statistical knee model3 using bone segmentations from MRIs. This model quantified 3D relative bone positions (rotations and translations between the patella, femur, and tibia) and used machine learning to identify 3D bone shape features that reflect bone curvature variation in the dataset (Figure 1).
We compared preliminary scores of instability severity based on four different input feature sets:
For each feature set, we developed a severity score to reflect the distance between the means of the control and recurrent instability cohorts. We normalized scores such that zero corresponded to the control mean, a unit corresponded to one standard deviation of the control cohort’s scores, and a more positive score was associated with multiple episodes of patellar instability (greater instability severity).
We compared score performances based on associations with instability history (using one-sided t-tests) and patient-reported outcomes (using Pearson correlations). We conducted a sub-analysis from the best-performing preliminary score to develop the 3D Patellar instability Anatomical Severity Score (3D-PASS), built from the subset of features with the highest mean correlation to patient-reported outcomes.
Results:
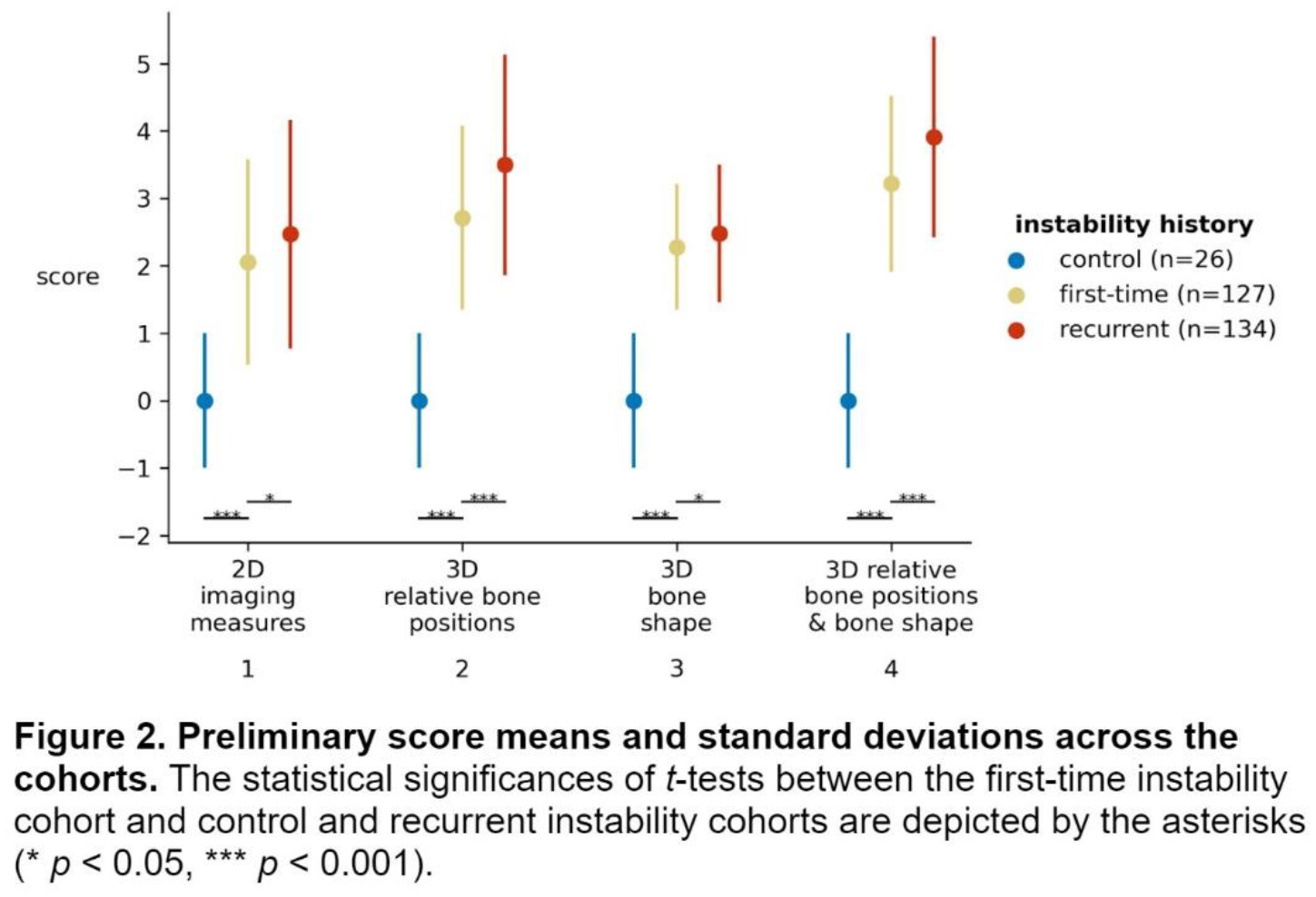
All four preliminary scores increased with instability history (Figure 2).
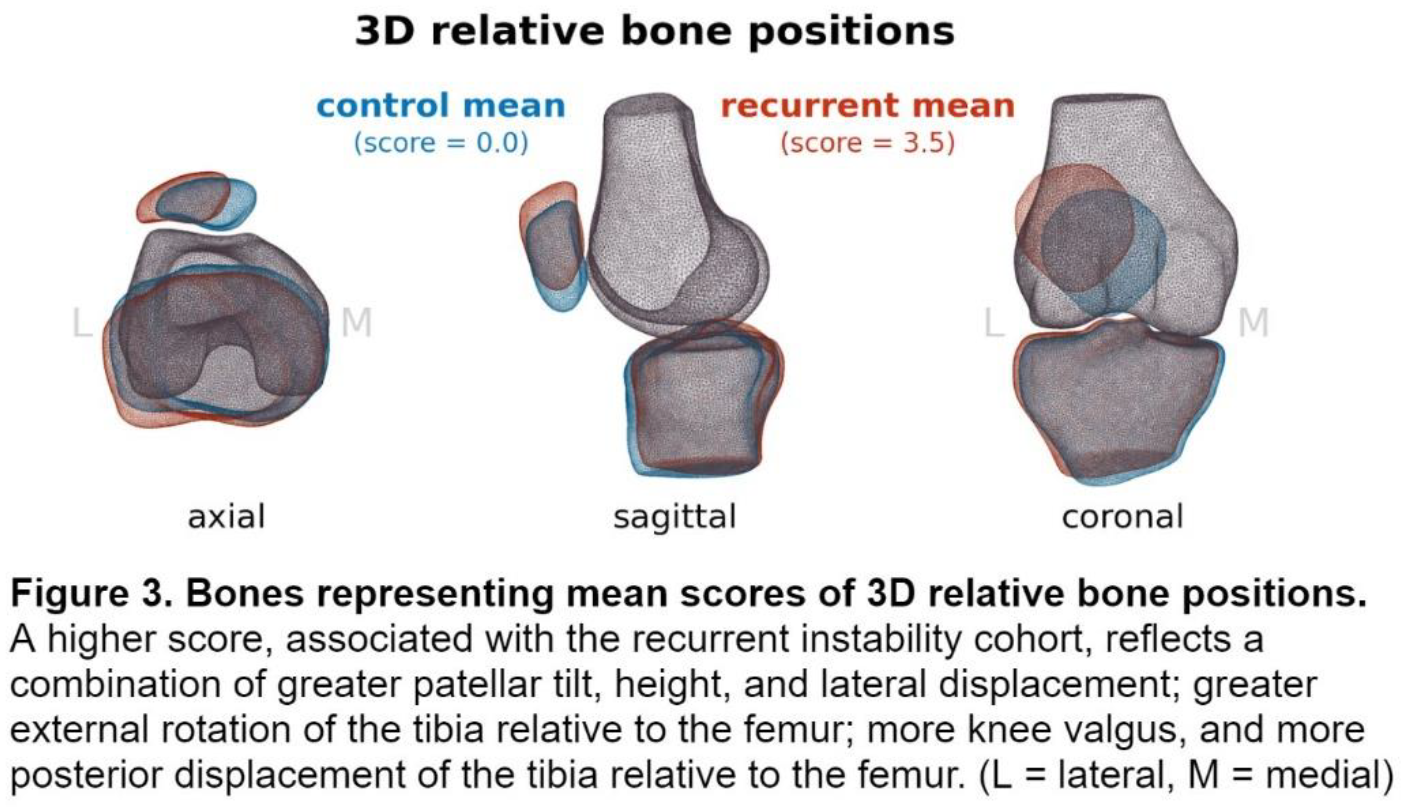
The 3D relative bone positions (translations and rotations) score (Figure 3) best distinguished between the first-time (mean score: 2.7) and recurrent instability (mean score: 3.5) cohorts (Figure 2). Of the four preliminary scores, it was the only one to correlate with one-year non-operative patient-reported outcomes (rKujala = -0.42, rBPII 2.0 = -0.49). None of the preliminary scores were correlated with one-year operative patient-reported outcomes.
3D-PASS was based on the subset of 3D relative bone position features that maximized correlations with patient-reported outcomes. Mean 3D-PASS differed significantly across the control (mean 3D-PASS: 0.0), first-time instability (mean 3D-PASS: 1.4), and recurrent instability (mean 3D-PASS: 1.8) cohorts and achieved strong correlations with one-year non-operative outcomes (Figure 4).
Conclusions:
The 3D Patellar instability Anatomical Severity Score (3D-PASS) is associated with instability history and patient-reported outcomes one year following non-operative treatment of patellar instability. 3D-PASS is based on bone positions, which had higher associations with recurrence and outcomes than traditional 2D imaging measures and 3D bone shape. In clinical practice, this novel metric has the potential to identify patients who are at risk of poor outcomes and may guide clinicians to consider earlier surgical intervention to improve patient prognosis.