Abstract
Objectives:
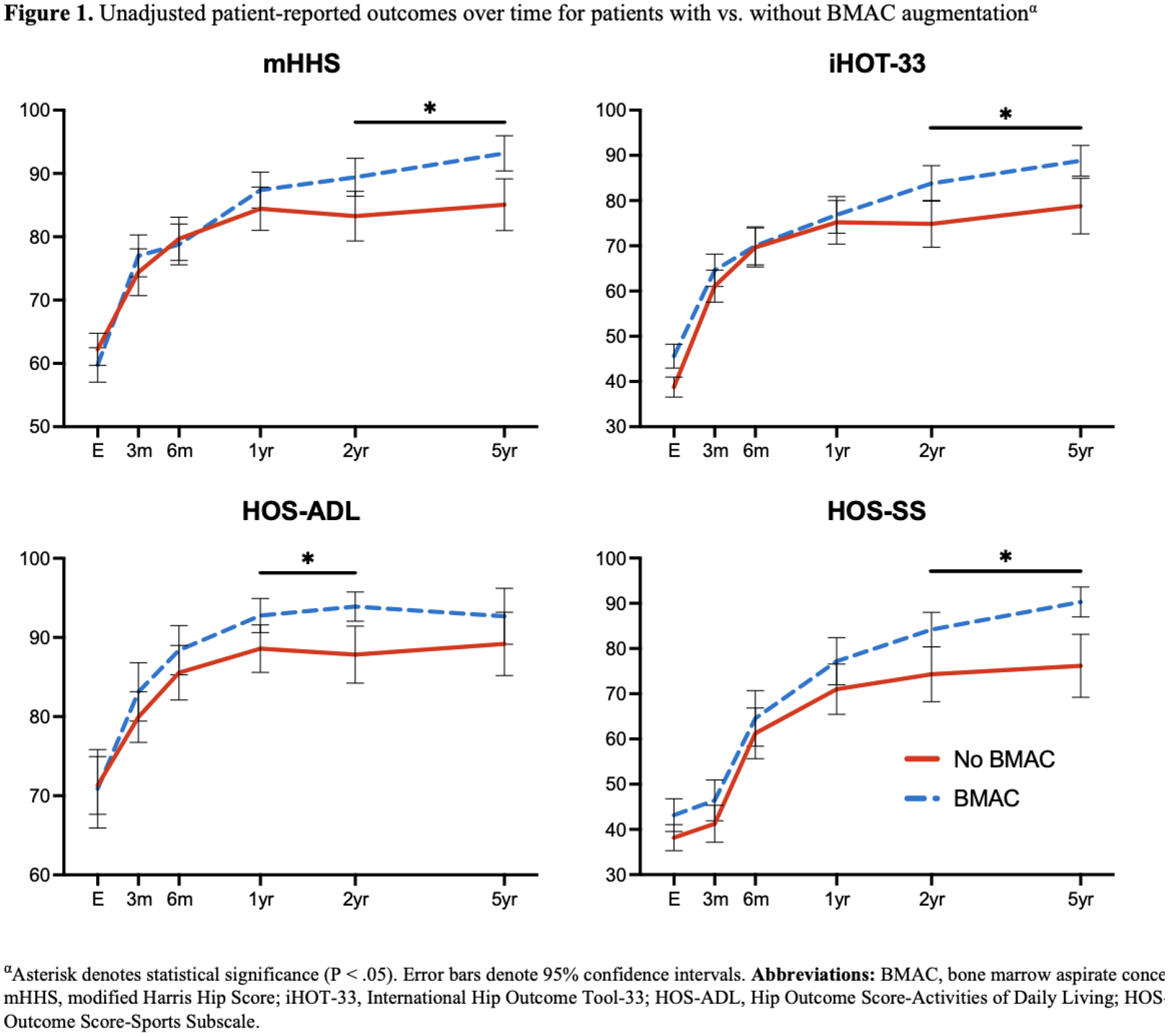
Preliminary findings in the literature suggest that treatment with bone marrow aspirate concentrate (BMAC) at the time of hip arthroscopy is a potentially viable solution to improve outcomes in patients with cartilage degradation concomitant to acetabular labral tearing; however, functional scores to date have not eclipsed 24 months. Therefore, the present study compares minimum five-year outcomes in patients treated with or without BMAC augmentation to address chondral damage during arthroscopic labral repair.
Methods:
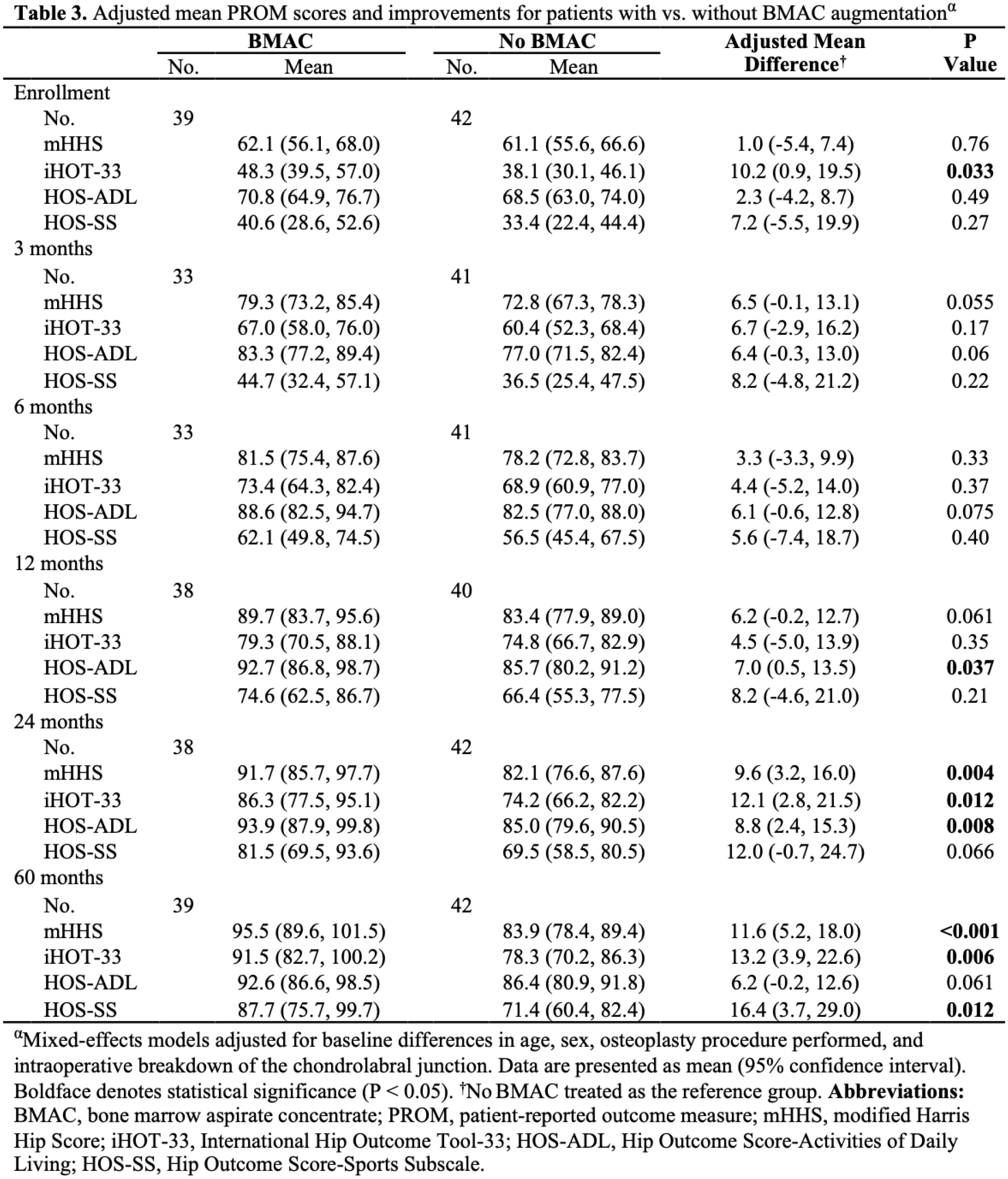
This is a case-control study analyzing prospectively collected data in patients who underwent acetabular labral repair from a single surgeon between May 2014 and January 2019. Patients were stratified into either the 1) BMAC cohort or the 2) control cohort depending on whether or not BMAC was used to address chondrolabral junction breakdown secondary to femoroacetabular impingement (FAI) and labral tearing during surgery. Patients were only included for data analysis if they: 1) underwent primary acetabular labral repair on their affected hip and 2) completed PROMs preoperatively and at 60 months after surgery. Exclusion criteria consisted of: 1) previous ipsilateral hip arthroscopy; 2) labral debridement; 3) a lateral center edge angle (LCEa) of <20º; and 4) <5 years of follow-up. Univariate analyses were performed using unpaired t test and chi-square/Fisher exact test as appropriate to draw baseline comparisons between groups. Informed by these unadjusted analyses, primary regressions included the following variables as fixed effects to compare PROMs at each timepoint via mixed-effect modeling: time (months), BMAC augmentation, BMAC*time interaction, age, sex, osteoplasty procedure performed, and intraoperative breakdown of chondrolabral junction. Statistical analysis was performed using R Version 4.2.1 or SPSS Version 29.0.2.0 and P < 0.05 was considered significant.
Results:
81 hips were included for analysis: 39 from the BMAC cohort and 42 from the control cohort. Univariate analyses demonstrated similar baseline characteristics between both groups with regard to BMI (BMAC: mean=39.0kg/m2 ± SD of 3.9kg/m2 versus no BMAC: 25.3kg/m2 ± 4.4; p=0.856); Tönnis angle (1.4º ± 7.9º vs. 2.6º ± 7.2º; p=0.502), lateral center edge angle (LCEa) (35.5º ± 7.2º vs. 35.7º ± 6.2º; p=0.879); and alpha angle (54.3º ± 14.9º versus 50.3º ± 16.6º; p=0.262) (
Conclusions:
Patients who underwent BMAC augmentation during arthroscopic labral repair outperformed patients who underwent labral repair alone without BMAC. This difference started to manifest at 12 months postoperatively and steadily increased in contrast until 5 years after surgery. These findings remain consistent with short-term reports and add mid-term outcomes to the growing body of literature that describes the patient-reported effect of BMAC as an adjuvant therapy during hip arthroscopy.