Abstract
Objectives:
Blood flow restriction (BFR) with low-load exercise has emerged as a powerful tool for rehabilitation professionals to maximize productivity and outcomes from patients who suffer from painful conditions or restrictions after injury or surgery. Post-operative knee patients often struggle regaining simple function such as ascending stairs or squatting due to reduced quadriceps strength and pain. Physical therapists implement smaller, more tolerable activities to bridge this gap and build towards higher levels of functional capacity. The utilization of BFR with these lower-level exercises has shown profound effects in pain modulation as well as neuromuscular function, allowing patients to achieve greater function in a shortened period of time. Some of the theorized mechanisms behind these benefits seen with BFR are similar to those seen in high-load or high-intensity activities, such as post-activation potentiation and exercise-induced hypoalgesia where large groups of motor units are engaged to create a higher performance potential compared to baseline. However, the acute effects of BFR and low-load exercises on post-exercise performance and muscle recruitment are currently unknown. This information would be helpful to physical therapists and other rehabilitation professionals to better refine treatment paradigms through heightened patient productivity and function with lower loads and decreased risk. The purpose of this study is to determine if low-load exercise (LLE) with BFR alters muscular activity, fatiguability, or strength of the quadriceps immediately following as compared to standard LLE or high-load exercise (HLE). The investigators hypothesize that BFR will produce similar effects as HLE, but with reduced resistances.
Methods:
Healthy subjects (18-45yo) were recruited and consented from the local area who have no recent history of lower extremity injury or neurovascular compromise. All subjects underwent three separate and randomized data collection sessions within a 2-week period with a minimum of 72h between sessions. Sessions were randomized via spreadsheet algorithm (Microsoft Excel, Redmond, WA, USA). Each session included pre- and post-intervention isometric (MVIC) and isokinetic (ISO-K, 45°/s) testing (Figure 1) as well as post-intervention 50 repetition (180°/s) fatigue testing (PEF) with an automatic dynamometer system (Biodex System 4 Pro™, Shirley, NY, USA). The randomized interventions consisted of LLE (20%MVIC), LLE+BFR (20%MVIC), and HLE (75%MVIC). Repetitions utilized for LLE and LLE+BFR were 30/15/15/15 with 30sec rest breaks and 4x5 for HLE with 60sec rest breaks between sets. The rest breaks are based on current literature standards regarding low to high-load training as well as BFR with exercise. Force output, power, and fatigue data were all collected within the Biodex system while EMG data (Delsys Trigno Research+) for quadriceps (vastus medialis, rectus femoris; vastus lateralis) activation were collected separately during intervention and post-testing. After root-mean-square transformation, data were normalized to the average EMG output analyzed from MVIC contractions whereby all EMG data were expressed as EMGa (%MVIC). A one-way ANOVA repeated across trials followed by a Bonferroni post-hoc test was used to determine if differences were present between conditions with regards to quadriceps activation or function (Type-I error set at at ∝=0.05).
Results:
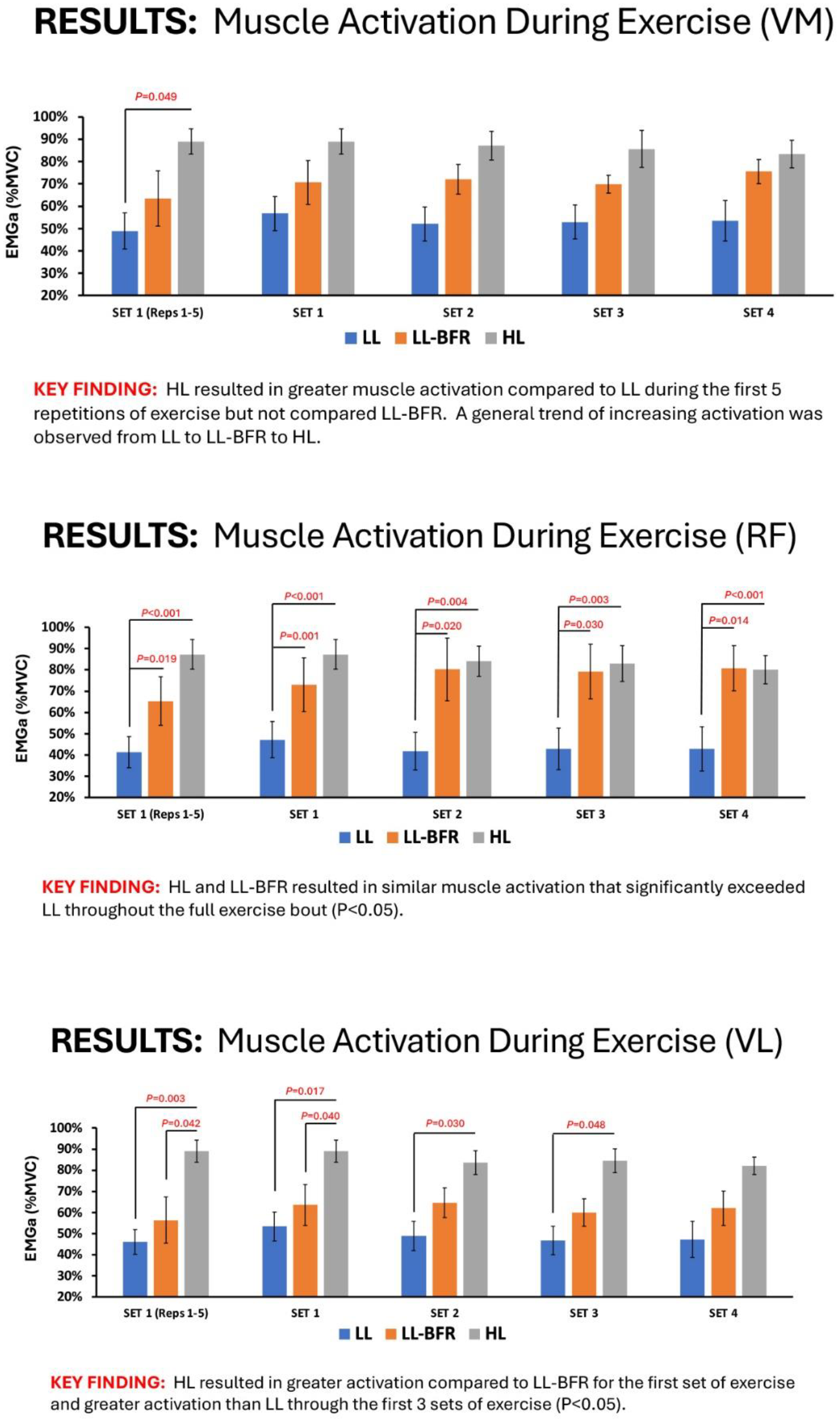
A total of 6 subjects (M =5, F =1; age = 20.8±1.7yr; body mass = 79.3±13.4kg; height = 176±11.1cm) were included for interim analysis of the ongoing study. Following exercise, muscle activation patterns favored higher EMGa for the LLE+BFR condition during MVIC and PEF testing, especially for the rectus femoris. During the ISO-K testing, EMGa remained similar to baseline for only the LLE+BFR condition, while LLE and HLE were significantly decreased. No significant changes were observed for peak torque during MVIC or ISO-K testing for either condition, though LLE+BFR produced a trend towards higher torque values. During exercise, HLE and LLE+BFR resulted in similar muscle activation that significantly exceeded LLE throughout the full exercise bout for the rectus femoris. The vastus lateralis exhibited a similar pattern of lower EMGA during the LLE condition, with HLE only achieving greater activity than LLE+BFR for the first set.
Conclusions:
The utilization of BFR with lower loads has shown significant potential for improving strength and function, especially of the quadriceps. The preliminary data from this study indicates that differences in quadriceps EMGa are present both during and following LLE, LLE+BFR, and HLE conditions. In a novel finding, we observed these differences to be specific to the individual muscles of the quadriceps and may represent an effect of proximity to the occlusive device. At this time, a general trend towards LLE+BFR seems to produce greater effects in pre-to-post force measures.