Abstract
Objectives:
Capitellar osteochondritis dissecans (OCD) lesions can be challenging to treat due to difficulties with adequate exposure and healing. Traditional microfracture relies on formation of fibrocartilage over more anatomic hyaline cartilage, with only acceptable clinical outcomes reported. Compared to other body locations (e.g. knee, talus), the thin cortex of the distal humerus makes osteochondral graft technically demanding due to the risk of iatrogenic fracture when attempting to achieve press fit of the graft. Past studies have demonstrated enhanced microfracture with BioCartilage to be a viable technique for treatment of OCD of the talus, though little literature exists regarding application of biologically-enhanced microfracture for capitellar OCD lesions. The purpose of this study was to report the patient-reported outcomes (PROs) and return to sport (RTS) of pediatric patients who underwent enhanced microfracture for OCD lesions of the capitellum.
Methods:
This consecutive case series included patients aged <18 years of age with unstable, contained humeral capitellum OCD who underwent enhanced microfracture and had minimum 1 year of clinical follow-up and PRO scores. Patients who had bilateral capitellum OCD, underwent a concomitant OAT procedure, and/or concomitant injuries were excluded to limit the influence of other lesions or injuries on PROs. In each case, bone marrow is aspirated from the iliac crest and mixed BioCartilageÒ extracellular matrix (Arthrex, Naples, FL). After initial diagnostic arthroscopy, debridement, and loose body removal, a small arthrotomy is made through an anconeus-splitting approach. The OCD lesion is confirmed to be contained and then the mixture is placed into the defect and sealed with fibrin glue.
Patient demographics and surgical variables including lesion characteristics were collected from the medical record. Clinical data including elbow range of motion (ROM), RTS time, postoperative sport level, complications, and date of last follow-up were collected. Patient reported outcomes (PROs), including HSS Pedi-FABS, Quick DASH, PROMIS Mobility, PROMIS Pain Interference, and PROMIS Upper Extremity, were obtained at baseline (if available) and at least 1 year postoperatively. PRO scores and range of motion were compared pre- and post-operatively using Wilcoxon Signed-Rank tests based on normality testing with Shapiro-Wilk tests.
Results:
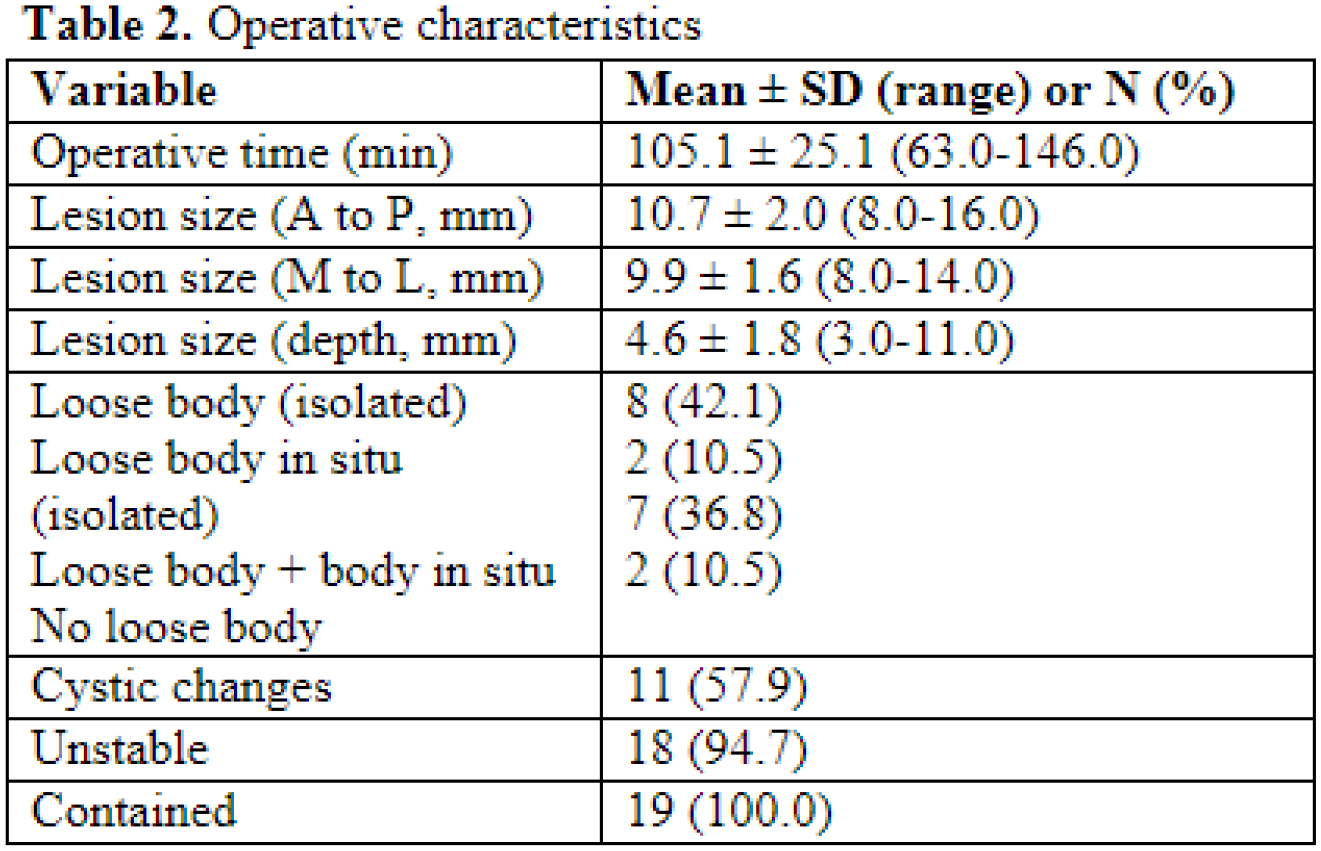
A total of 19 patients were included (mean age 12.8 ± 1.5) with an average 19.9 ± 8.4 months follow up. Fourteen (73.7%) patients were female. The most common primary sports were gymnastics (n=7, 36.8%), baseball or softball (n=2, 10.5%), and racquet sports (n=2, 10.5%) (
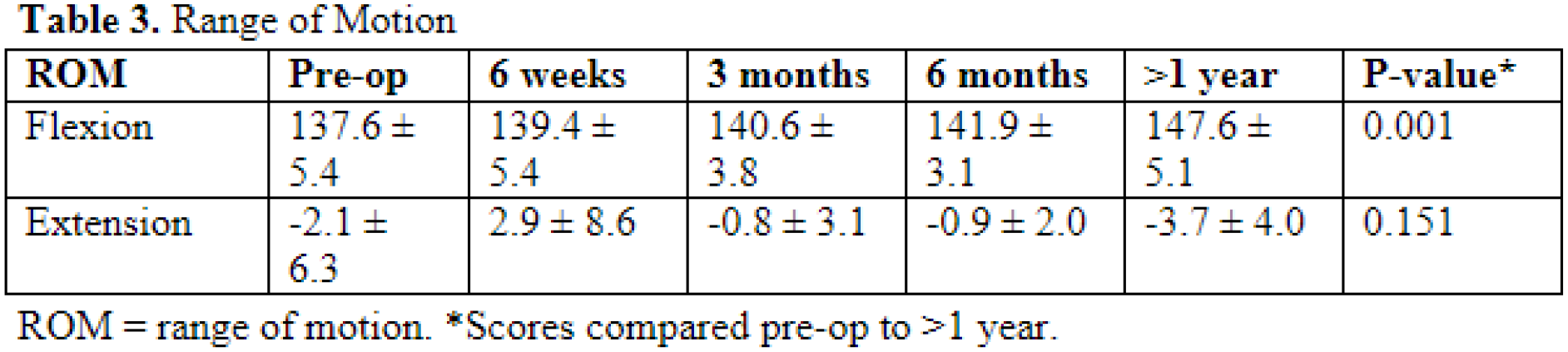
Flexion improved from 137.6 ± 5.4° pre-operatively to 147.6 ± 5.1° (p=0.001) at >1 year post-operative, while extension remained near full pre- and post-operatively (-2.1 ± 6.3° vs -3.7 ± 4.0°, p=0.151) (
Conclusions:
As an adjunct to traditional microfracture for contained capitellar OCD lesions, this study demonstrated that addition of a micronized allogeneic cartilage scaffold is a viable treatment strategy for pediatric patients. We observed favorable PROs outcomes with a ~90% RTS rate >1 year after surgery for these injuries, supportive of the results of this technique in other anatomic regions and adult populations. These results are in contrast to isolated microfracture where RTS rates are closer to 50-75%, suggesting enhanced microfracture to be a new standard for contained lesions.