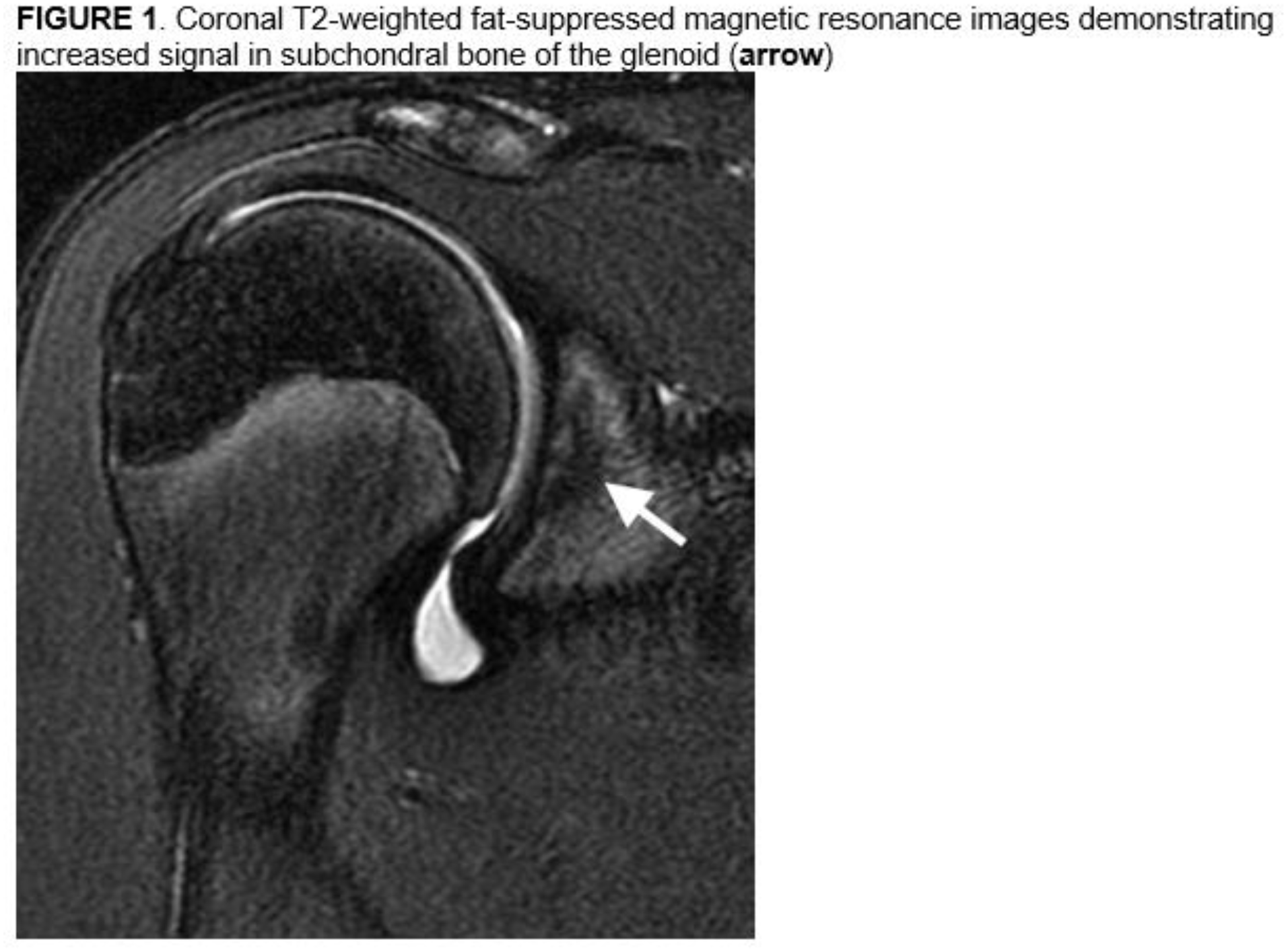
Abstract
Objectives:
Osteochondritis dissecans (OCD) is a pathologic condition in which a portion of subchondral bone and possibly surrounding articular cartilage become either partially or totally separated from the surrounding bone bed due to lack of blood supply, and this injury is distinct from focal articular cartilage defects. OCD lesions occur most commonly on convex weight-bearing joint surfaces, such as on the femoral head or femoral condyle, where convexity leads to greater axial contact loads at the articular surface and likely predisposes the joint to microvascular trauma. Non-weight-bearing convex joint surfaces such as the humeral head and capitellum, when subjected to repetitive microtrauma, have also been described to occasionally sustain OCD lesions. All such reports contain a patient clinical history of either an acute traumatic event or repetitive activities such as overhead throwing or gymnastics. However, OCD of the glenoid is especially rare, and the clinical presentation, surgical treatment, and outcomes are not well-understood. The purpose of our current study was to synthesize and describe clinical presentation, treatment, and patient-reported outcomes within a cohort of glenoid OCD lesions identified amongst baseball athletes treated at a single institution over a 26-year span.
Methods:
Over a 26-year period at our institution, we retrospectively identified shoulder arthroscopies performed by 3 surgeons within athletes. We reviewed radiographs, contrast-enhanced magnetic resonance imaging (MRI; Figure 1), and arthroscopic images (Figure 2) to identify those with glenoid OCD lesions. Intraoperatively, the glenoid OCD was identified and excised, fragmented or loose bodies were removed, and a burr was used to debride the bony bed to a bleeding surface, followed by microfracture of the lesion (Figure 2), along with surgical treatment of concomitant shoulder pathology as appropriate. All athletes underwent standardized rehabilitation, beginning with range of motion and strengthening immediately postoperatively. We collected data from the electronic health record including patient demographics, clinical presentation, sport-related information, imaging findings, surgical details, and concomitant procedures. We evaluated patient-reported outcomes at a minimum of 1 year post-operatively using the Athletic Shoulder Outcome Scoring System (ASOSS), the Short Form-36 (SF-36) health survey, and a series of questions regarding return to preinjury sport. We calculated summary statistics (means and standard deviations for continuous variables; counts/proportions for categorical variables) for demographic, clinical, surgical, and outcomes data.
Results:
From a total of 3,940 potential shoulder arthroscopies, we identified 19 (~0.5%) diagnosed cases of glenoid OCD, with a mean age of 22.7 years at surgery. All 19 patients were baseball players, including 14 pitchers, 1 outfielder, 1 second baseman, 1 third baseman, 1 shortstop, and 1 catcher. Regarding clinical presentation, the most common complaint was posterior shoulder pain (13 patients) and decreased performance and/or pitching velocity. Additionally, 17 of 19 patients had a gradual onset of pain, with no antecedent traumatic event, with an average of 18 months of pain (range, 2-36 months) prior to evaluation. Imaging review revealed cystic subchondral changes in 14 of the 19 patients, indicating underlying necrosis of the glenoid consistent with OCD (Figure 1). Isolated OCD lesions were identified in 7 patients, whereas 12 had concomitant shoulder pathology (Table 1). Specific concomitant procedures performed included partial rotator cuff tear debridement (n=7), superior labral repair (n=2), posterior labral repair (n=1), subacromial bursectomy (n=1), or debridement of thrower’s exostosis (n=1). Following surgery, 9 patients were ready to begin an interval throwing program 6 weeks post-operatively; 7 of these patients had isolated OCD lesions and the other 2 had subacromial bursectomy or debridement of thrower’s exostosis. The remaining 10 patients who underwent concomitant procedures during shoulder arthroscopy progressed through rehabilitation programs as indicated and began interval throwing programs between 12 and 20 weeks postoperatively. All 19 (100%) were successfully-contacted for follow-up data collection, at an average of 32 months (range 16-124 months) after surgery. The average ASOSS score was 78 (out of 100). When stratified by concomitant surgery/pathology, the 9 patients with isolated OCD lesions had an average ASOSS score of 85, and the 10 patients with concomitant pathology had an average ASOSS score of 73. For the SF-36 (all subscales scored out of 100), the average social function score was 93, the average pain score was 75, and the average general health score was 83. Fifteen of the 19 (79%) athletes were able to return to the same or higher level of competition postoperatively (Table 1).
Conclusions:
To our knowledge, this study represents the largest case series of rare OCD lesions of the glenoid fossa in baseball athletes. We found that arthroscopic debridement of glenoid OCD with microfracture of subchondral bone yields good outcomes and a high level of return-to-sport in a group of high-level throwing athletes, especially in athletes with isolated OCD lesions.