Abstract
Objectives:
Posterior humeral avulsion of glenohumeral ligament (PHAGL) involve an avulsion of the posterior band of the inferior glenohumeral ligament (IGHL) from the humeral neck. While rare, these lesions have been shown to contribute to recurrent instability. The purpose of this study is to compare clinical outcomes and recurrence rates of patients with PHAGL lesions undergoing surgical repair for posterior shoulder instability versus a pair-matched control group without PHAGL lesions undergoing isolated arthroscopic posterior labral repair.
Methods:
This was an IRB approved study that was a retrospective review of prospectively collected data on patients with posterior labral tears (PLT) with and without PHAGL lesions who underwent arthroscopic repair of both lesions between Dec 2008 to Aug 2021. The patients with PHAGL lesions had an injury to both the posterior band of the IGHL and the posterior labrum termed a floating posterior inferior glenohumeral ligament. These patients were classified based on a system set forth by Ames and Millet. In this classification system the injury is broken down into four subgroups; type 1 involved a PHAGL with a posterior Bankart lesion, type 2, a PHAGL with a posterior osseous Bankart lesion, type 3 a posterior bony humeral avulsion of the glenohumeral ligament (PBHAGL) with a posterior Bankart lesion, and type 4, a PBHAGL with a posterior osseous Bankart lesion These patients were matched 1-to-3 using 5 factor match criteria (age, sex, year of surgery, biceps tenodesis, isolated posterior labral tear) to patients with PLT without PHAGL lesions who underwent isolated repair of the posterior labrum and capsulorrraphy. Surgical and demographics, further surgery and revision data were collected. Demographic, surgical data, and pre and postoperative clinical outcomes scores (SF-12 PCS, ASES, SANE QuickDASH) were collected. Patient satisfaction (range,1-10,10=best) was collected. Several other activities specific questions were also documented. Paired data was compared using a Wilcoxon signed-rank test. Kaplan Meier survivorship analysis was performed. Failure was defined as recurrent instability or progression to arthroplasty.
Results:
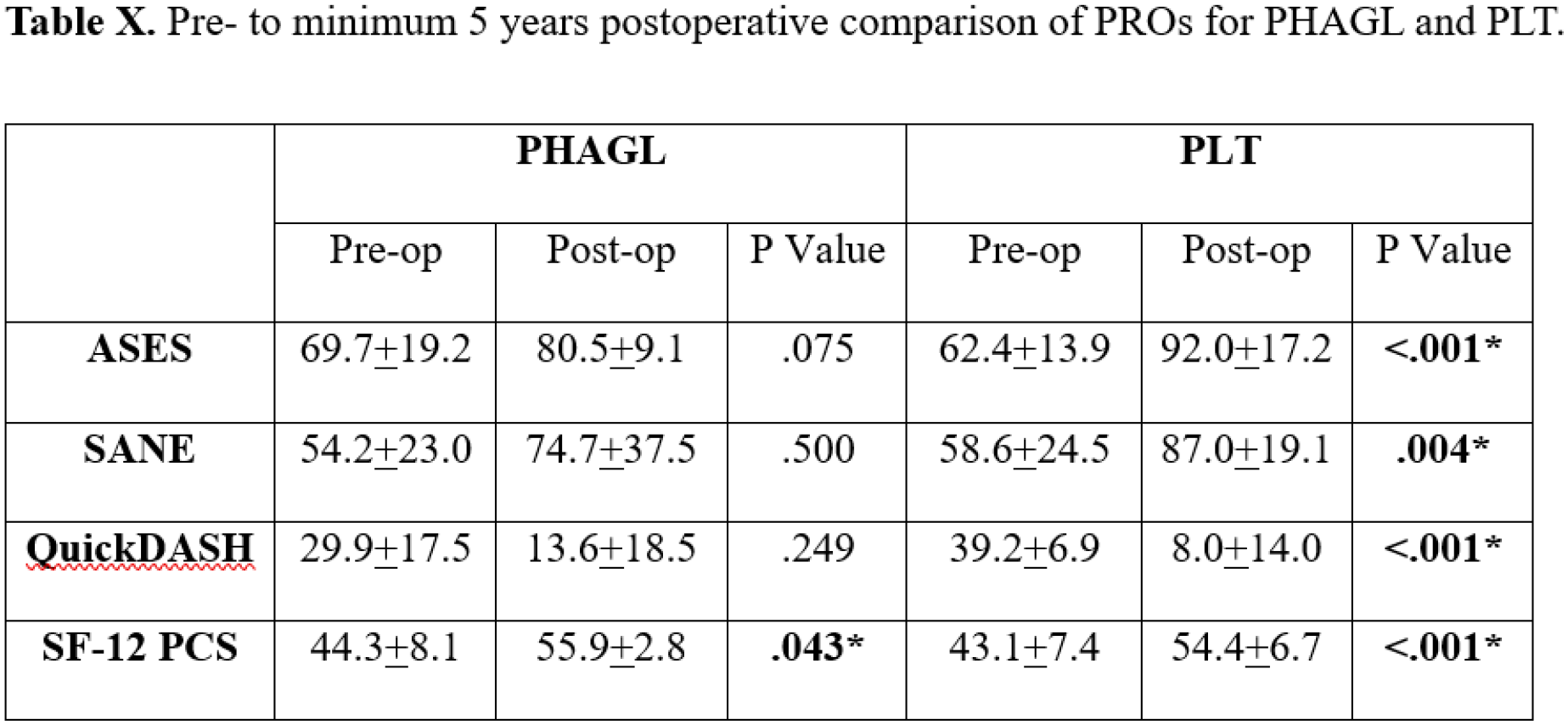
Nine patients diagnosed with PHAGL lesions who underwent primary arthroscopic repair of the PLT and PHAGL were included. The patients in the PHAGL group included seven type 1 lesions and two type 2 lesions. These 9 patients (PHAGL group) were age matched to a cohort of 26 patients with posterior labral tears who underwent repair (PLT group). Mean time from injury to surgery was 418 days (range 3-3279; p=.488). Mean age at surgery was 29.7 (range 16.3-66.4)(p=.701), all patients were male, with one worker’s compensation case. There was a mean follow-up of 5.6 years (range 2-14.2). Comparing the change in measured outcome scores between the PHAGL and PLT groups demonstrated no statistical significance: delta in ASES score was mean 20.8±24.7 vs. 31.1±20.0;p=.308, delta SANE score was mean 15.6±61.5 vs. 29.4 ±32.5;p=.496, delta QuickDASH score means were -16.3±34.6vs. -32.3±19.8; p=.163, and delta SF-12 mean was 11.6±7.3 vs. 11.9±9.6p=.940 respectively. PHAGL had a median satisfaction was 8/10 (range 1-10) and in the PLT cohort median satisfaction was 10/10 (range 6-10);p>0.075. No significant difference in functional outcome or sports specific pre-op & post-op scores was identified between the two groups (p >.05). Two PHAGL patients developed recurrent posterior instability, and one patient in the PLT group progressed to arthroplasty 12 years after the index surgery. From this cohort, Kaplan-Meier survivorship was superior in the PLT group, 100% at 2 years over the PHAGL group at 83.3%, however this was not statistically significant (p=.148).
Conclusions:
In patients with posterior shoulder instability, those who sustain an PHAGL lesion who undergo surgical stabilization demonstrate no difference in reported outcomes, functional outcomes, or sport specific outcomes with similar survivorship in the medium term when compared to a matched group of patients who underwent surgical stabilization of the posterior labrum without PHAGL lesions.