Abstract
Objectives:
Traumatic and atraumatic labral tears are associated with different pathophysiologies and may lead to differing post-operative outcomes after arthroscopic repair. This study aims to compare the functional outcomes of arthroscopic labral repairs between patients with traumatic onset of posterior shoulder instability (PSI) and patients with atraumatic onset of PSI.
Methods:
Between 2009 and 2023, a single institution, retrospective analysis was conducted on 92 patients who underwent arthroscopic labral repairs with posterior shoulder instability and a minimum 2-year follow-up. Procedures were performed by 7 surgeons. Demographic and baseline variables were extracted from medical records. Pre-operative and post-operative outcomes of range of motion and strength were recorded.
Results:
34 traumatic PSI patients were available with a mean age of 28.5± 9.8 years, a BMI of 27.6± 5.2 kg/m2, American Society of Anesthesiologists (ASA) score of 1.4± 0.6, Charlson Comorbidity Index (CCI) of 0.0± 0.2, and follow up of 2.7± 2.9 years. 58 atraumatic PSI patients were available with the mean age of 27.7± 8.6, BMI of 28.0± 6.7 kg/m2, ASA score of 1.6± 0.6, CCI of 0.2± 0.8, and a follow up of 2.2± 3.8 years.
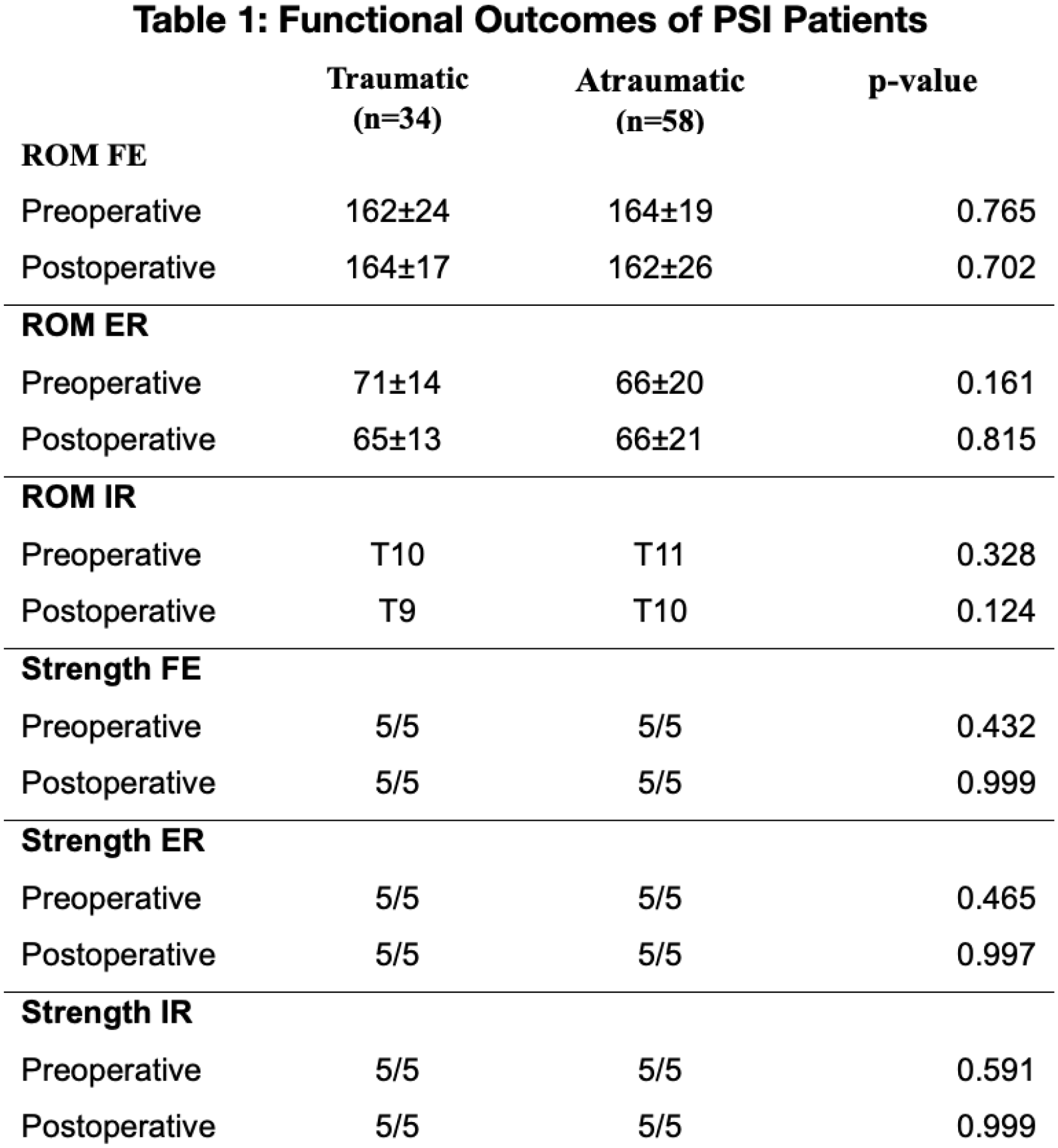
Comparison of pre-operative and post-operative measurements between the traumatic PSI and atraumatic PSI patients following arthroscopic labral repairs revealed no significant differences in active range of motion and strength measurements including pre-operative forward elevation (FE) (traumatic: 162± 24 vs atraumatic: 164± 19, p=0.765), post-operative FE (traumatic: 164± 17 vs atraumatic: 162± 26, p=0.702), pre-operative external rotation (ER) (traumatic: 71± 14 vs atraumatic: 66± 20, p=0.161), post-operative ER (traumatic: 65± 13 vs atraumatic: 66± 21, p=0.815), pre-operative internal rotation (IR) (traumatic: T10 vs atraumatic: T11, p=0.328), and post-operative IR (traumatic: T9 vs atraumatic: T10, p=0.124). There were no marked changes in functional strength scores across both groups. Implant survival rate over 5 years was (traumatic: 85% vs atraumatic: 72%, p=0.470) and instability recurrence rates were (traumatic: 6% vs atraumatic: 26%, p=0.017).
Conclusions:
Traumatic PSI patients did not have significantly worse functional measurements during pre-operative or post-operative exam than atraumatic PSI patients, but there was a significant difference in instability recurrence rates between the groups