Abstract
Objectives:
Regional anesthesia with interscalene nerve blocks has remained an effective method of analgesia during total shoulder arthroplasty. Purported advantages include decreased baseline pain, increased patient satisfaction, and decreased hospital length of stay; however, concerns remain about the risks of respiratory and neurologic complications as well as ’rebound’ pain. Local infiltration analgesia has been reported in several smaller series to provide equivalent pain control in total shoulder arthroplasty with the added benefits of lower complication rates and significantly lower costs. The purpose of this study was to investigate a nationwide matched cohort of shoulder arthroplasty patients to determine the effect of liposomal bupivacaine on perioperative opioid consumption, length of stay, and complications compared to peripheral nerve block.
Methods:
Adult patients who underwent primary, elective aTSA and rTSA from January 1st, 2016 to December 31st, 2020 were identified using the Premier Healthcare Database (PHD). Patients were divided on the basis of having received local infiltration liposomal bupivacaine (LB) or a peripheral nerve block (PNB) on the day of index surgery. Propensity score matching and multivariable modeling incorporating demographic, comorbidity, and medication covariables were performed. Endpoints included in-patient opioid utilization (morphine milligram equivalents [MME]), length (days) and cost (dollars) of hospitalization, infectious, bleeding, and mechanical complications.
Results:
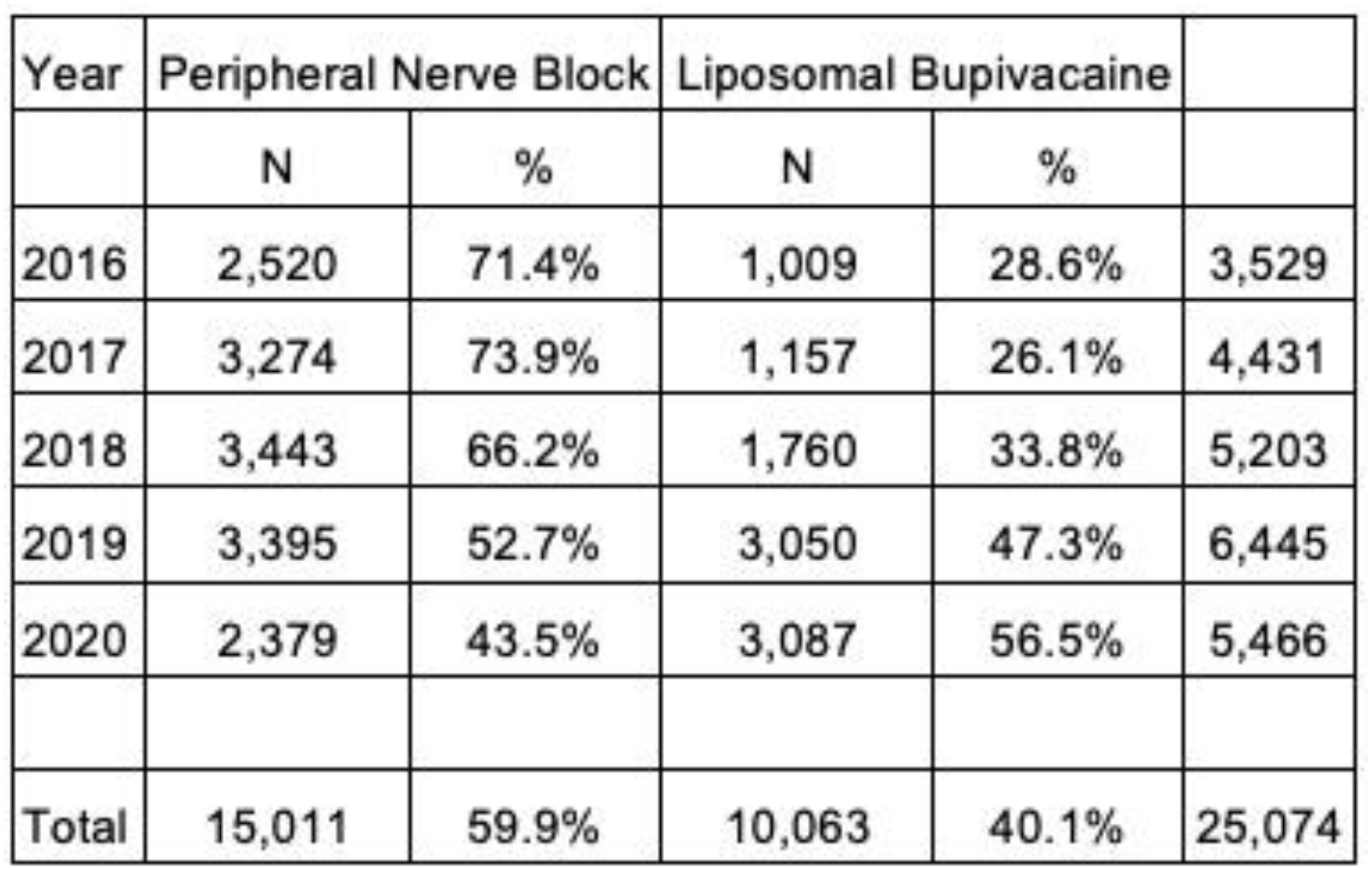
From 2016 to 2020, 10,063 (40.1%) and 15,011 (59.9%) patients received LB and PNB, respectively. After matching, 10,036 patients received LB while 10,036 received PNB. LB was associated with a reduction in inpatient opioid utilization (median: 37, interquartile range [IQR]: 21.6-60, adjusted effect [β]: -6.92, confidence interval [CI]: -8.20, -5.7, p<0.001) and length-of-hospitalization (median: 1, IQR: 1-1, β: -0.13, CI: -0.16, -0.10, p<0.001), but a slight increase in total hospitalization cost (median $17655.19, IQR: 14809.17-22011.28, β: 317.4051, CI: 102-94-531-87, p=0.004. Compared to PNB, LB was associated with a decreased risk of infectious (odds ratio [OR]: 0.62, CI: 0.39-0.97, p=0.037), blood loss related (OR: 0.88, CI: 0.79-0.98, p=0.017), and mechanical implant (OR: 0.45, CI: 0.33-0.61, p<0.001) complications.
Conclusions:
Liposomal bupivacaine is effective in reducing inpatient opioid utilization and length of hospitalization compared to peripheral nerve blocks in total shoulder arthroplasty. Furthermore, this study demonstrated local infiltration of liposomal bupivacaine is associated with a significantly decreased risk of deep wound infection, acute blood loss anemia, and postoperative stiffness. The findings of our nationwide cohort analysis support previously published case series demonstrating decreased postoperative analgesia requirements following usage of local infiltration of liposomal. Optimal combinations of multimodal pain regimens in total shoulder arthroplasty continue to warrant further investigation.