Abstract
Objectives:
The shift from volume-based to value-based care has made electronic patient-reported outcome measures (ePROMs) the focus in determining the value of an orthopedic intervention. However, the information gleaned is only as strong as the robustness of the data set. The importance of patient compliance with ePROMs cannot be understated. Interventions to increase patient compliance are critical to better understand the needs of our patients. Given the current state of limited resources, it is valuable to quantify the effect of direct patient outreach in order to optimize ePROM completion. The purpose of this study was to determine the population of patients requesting direct assistance and compare their ePROMs to those who did not request direct assistance.
Methods:
A prospective, multi-site chart review was conducted among patients with upcoming outpatient sports medicine appointments. Prospective patients were assigned ePROMs as part of standard of care. Between June 2023 and March 2024, patients with incomplete ePROMs were identified and contacted by research assistants. They were offered the option to complete the surveys over the phone with assistance and, if declined, they were emailed a link to complete the surveys independently. We compared age, race, and Area Deprivation Index (ADI) scores of patients who requested assistance over the phone versus those who asked to complete the ePROMs independently. We also compared the patient responses for the PROMIS Global survey which includes Pain Score, Mental Health Score, and Physical Health Score. Alpha level of 0.05 for ADI and pain scores in the two groups were determined by the Wilcoxon rank-sum test. Alpha level of 0.05 for these same variables across different self-reported races were determined by the Kruskal-Wallis test.
Results:
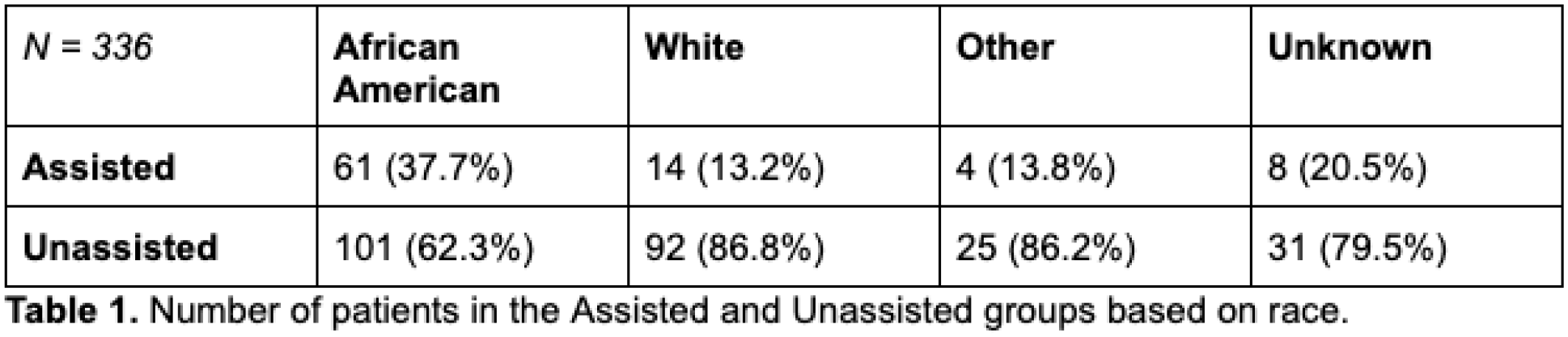
A total of 336 patients with upcoming outpatient clinic visits were directly contacted by phone prior to their appointment. 87 of those patients (25.9%) asked our study staff for assistance to complete their ePROM surveys over the phone. The average ADI score for those asking for assistance was higher than the average score for patients who requested to complete the surveys independently (5.80 vs. 4.62, p < 0.05)(Figure 1). The average pain scores were also higher in the group that requested assistance (6.11 vs. 4.37, p < 0.05)(Figure 2). Additionally, the average physical health (PH) scores were lower for the assisted group (41.92 vs. 46.61, p < 0.05)(Figure 2). When looking at race, 70.1% of patients asking for assistance identified as African American compared to the 40.6% of the independent group (Table 1). Using the Kruskal Wallis test to analyze ADI across races, the average ADI score for African Americans was significantly higher than in people who identify as White, Other, or those with Unknown race (p <0.05). Additionally, African Americans had significantly higher pain scores and worse physical health scores than people who identify as White (p < 0.05) (Figure 3).
Conclusions:
Patient Reported Outcome Measures (PROMs) help clinicians understand how their patients view their health outcomes and quality of life. Unfortunately, clinicians cannot gain this perspective when patients do not complete their ePROMs. By calling patients with incomplete ePROMs prior to their appointments, 25% of patients requested assistance. This resulted in 100% compliance in the assisted group while there was only 49.8% compliance in the unassisted group. The assisted group had significantly higher ADI scores compared to the unassisted group which suggests those most likely to request help are living in lower socioeconomic areas (Figure 1). Additionally, the significantly higher pain scores and lower physical health scores of African Americans further corroborates the relationship between health outcomes and socioeconomic conditions. Direct telephone outreach improved health outcome monitoring for minority populations and those living in areas with higher ADI scores. By making a concerted effort to directly reach out to these patient populations, improvements in pain, mental health, and physical health can be made and lead to better long term outcomes.