Abstract
Objectives:
The purpose of the present study was to evaluate the relationship between the concentrations of pro- and anti-inflammatory cytokines in the knee synovial fluid (SF) at the time of arthroscopic partial meniscectomy (APM) and long-term patient reported outcomes (PRO) and conversion to total knee arthroplasty (TKA).
Methods:
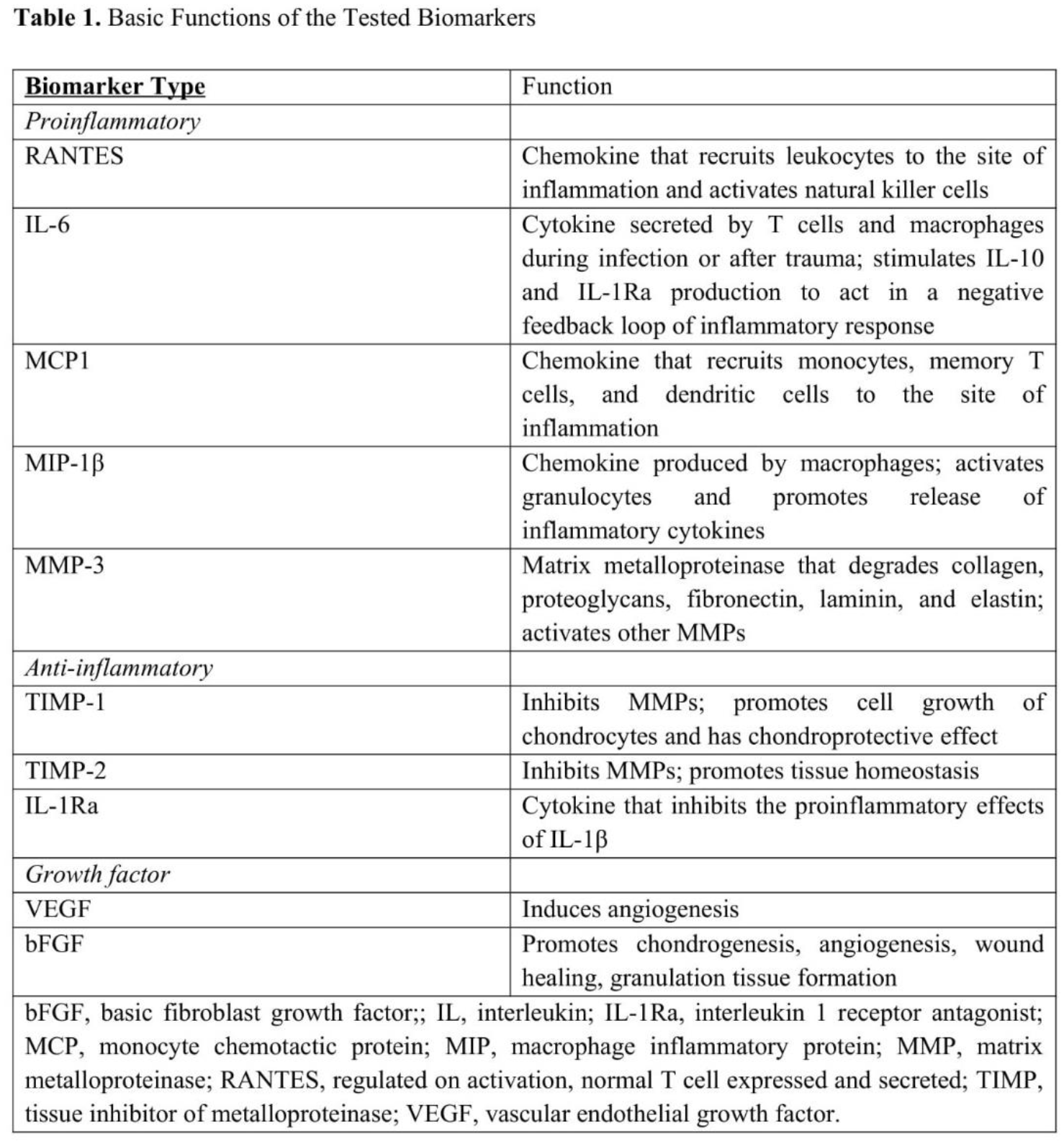
A database of patients who underwent APM for isolated meniscal injury was analyzed. At the time of surgery, SF was aspirated from the operative knee prior to the surgical incision and concentrations of pro- and anti-inflammatory biomarkers (RANTES, IL-6, MCP-1, MIP-1b, VEGF, TIMP-1, TIMP-2, IL-1RA, MMP-3, and bFGF) were quantified. Patients were asked to complete a survey prior to surgery that included VAS, Lysholm, Tegner and KOOS-PS and then again at the time of final follow-up. Clustering analysis of the 10 biomarkers of interest was carried out with the K-means algorithm.
Results:
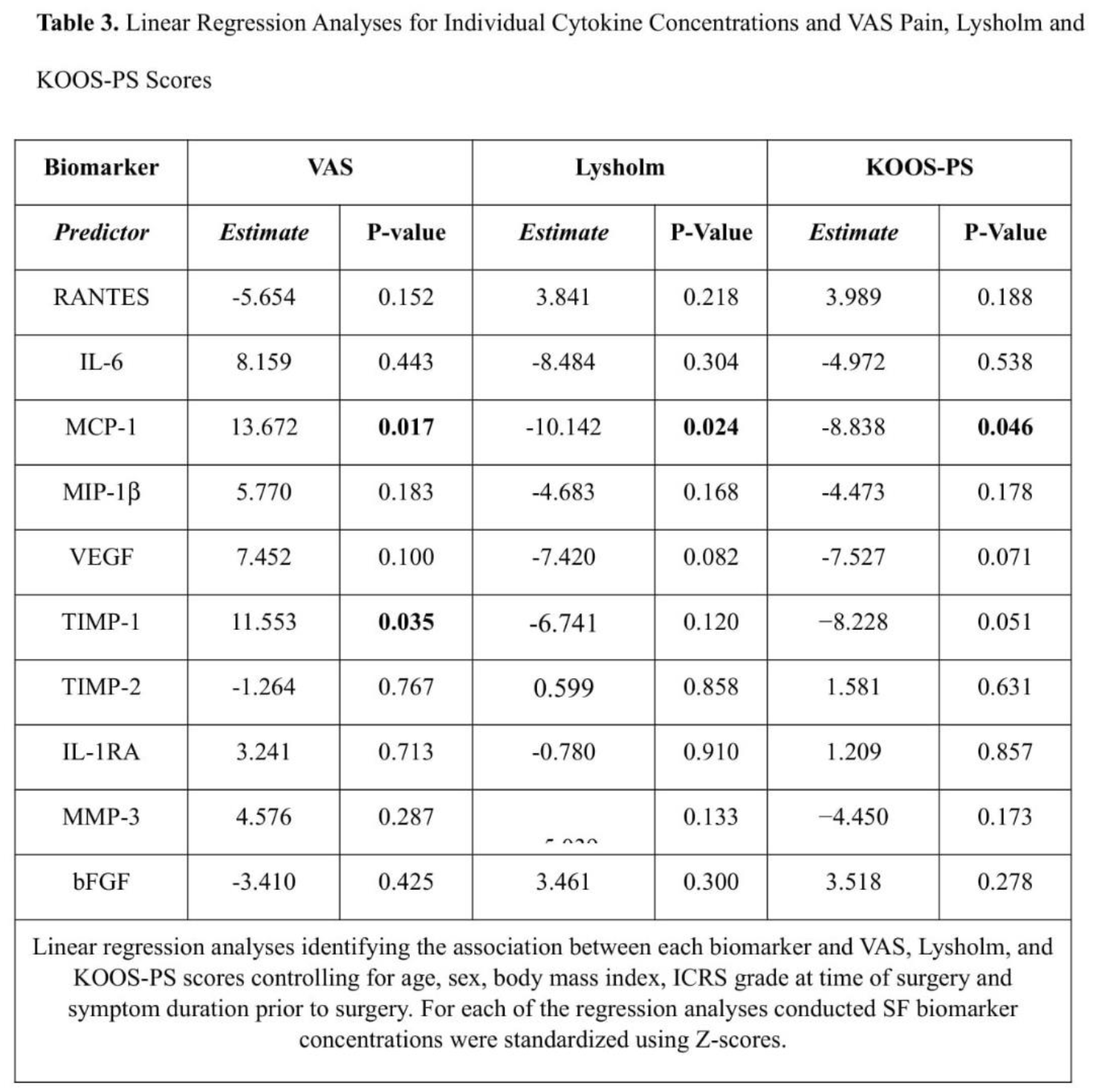
Of the 82 patients who met inclusion for the study, 59 patients did not have further ipsilateral TKA or APM and 43 (72.9%) patients completed PRO surveys. The mean follow-up time was 10.6 ± 1.3 years (range: 8.7-12.4 years). Individual pro-inflammatory cytokines including MCP-1 (b=13.672, p=0.017) and MIP-1b (b=-0.385, p=0.012) were associated with worsened VAS pain and Tegner scores respectively. K-Means clustering analysis separated the cohort of 82 patients into two groups, one with exclusively higher levels of pro-inflammatory cytokines than the second group. The “pro-inflammatory phenotype” cohort had significantly higher VAS pain score (p=0.024), and significantly lower Lysholm (p=0.022), KOOS-PS (p=0.047) and Tegner (p=0.009) scores at final follow-up when compared to the “anti-inflammatory phenotype” cohort. Rate of conversion to TKA was higher in the pro-inflammatory cohort (29.4% vs. 12.2%, p=0.064). Logistic regression analysis demonstrated that the pro-inflammatory phenotype was significantly correlated with conversion to TKA (OR=7.220 (95% CI: 1.028-50.720), p=0.047).
Conclusions:
The concentrations of SF cytokines on the day of APM can be used to cluster patients into pro and anti-inflammatory cohorts which predict PROs and conversion to arthroplasty at long-term follow-up.