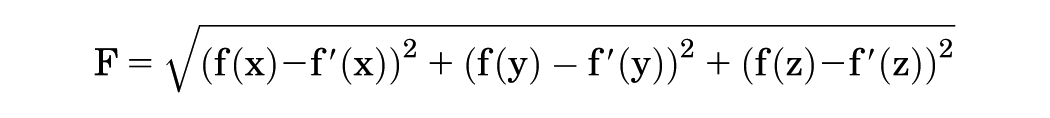Abstract
Background:
Many different suture methods have been devised for lateral meniscus radial tears but have resulted in inconsistent outcomes.
Purpose/Hypothesis:
The purpose of this study was to compare the biomechanical performance, specifically resultant force, tibial shift, and rotation, of 3 suturing techniques—horizontal, tie-grip, and cross-grip—for radial lateral meniscus tears across different flexion angles and under repetitive loading, using a 6 degrees of freedom (6-DOF) robotic simulator. It was hypothesized that the cross-grip suture would demonstrate superior biomechanical properties.
Study Design:
Controlled laboratory study.
Methods:
Fresh-frozen porcine right knees were mounted on a 6-DOF robotic simulator to mimic knee joint motion accurately. Meniscal conditions, including intact, radial tear, and horizontal, tie-grip, and cross-grip sutures, were tested on 6 specimens each in 2 experiments: (1) flexion-extension movement under valgus torque and (2) repetitive axial loading at 60° of flexion. The resultant force, which was defined as the net force transmitted through the knee joint, and the tibiofemoral relationship, which was defined as the tibial shifts and rotations relative to the femur, were recorded.
Results:
Radial tears reduced the resultant force on the lateral meniscus by 45% to 78% compared with intact. Horizontal, tie-grip, and cross-grip sutures restored resultant force to within 5% to 15% of intact levels, with cross-grip achieving the highest recovery. Radial tears caused medial shifts up to 2.15 mm and valgus rotations up to 4.88°, while sutures reduced these to within ±0.44 mm and ≤2.49°, respectively. After 300 loading cycles, sutured menisci maintained >90% of intact force, whereas radial tears declined to 33%. The cross-grip suture maintained the highest force values among the techniques. Sutures also limited abnormal tibial shifts and rotations, partially restoring joint stability.
Conclusion:
All 3 suture techniques effectively restored joint stability caused by radial lateral meniscus tears. The cross-grip suture showed the highest resultant force in dynamic testing, while all techniques demonstrated the same durability under repetitive loading. This is the first comparative study on the durability of meniscal sutures using a 6-DOF simulator, and it may provide new insights for future research on meniscal sutures.
Clinical Relevance:
The results of this study suggest that the cross-grip suture may be the preferred choice for competitive athletes with lateral meniscus radial tears who require high load tolerance.
The meniscus plays a vital role in knee joint function by providing essential stability, load distribution, and joint integrity through hoop mechanisms on the inner and outer sides.6,13 Lateral meniscus radial tears, commonly observed in young athletes, can cause significant damage by disrupting the hoop mechanism. 21 This disruption compromises the meniscal function and increases the risk of degenerative knee osteoarthritis. 2
Although partial meniscectomy is a treatment option, it fails to alleviate the load on the articular cartilage. 4 Consequently, meniscal repair surgery has gained popularity as a means of preserving knee joint function. 14
Various suture methods have been developed to reapproximate a radial tear. The horizontal suture places stitches parallel to the tibial plateau, 16 but its relatively low fixation strength and risk of gapping under load limit durability. To improve resistance to tear propagation, the tie-grip suture was introduced, anchoring vertical limbs on the meniscal periphery and passing horizontal limbs over these anchors; this configuration increases ultimate failure load but requires multiple suture limbs, raising concerns about iatrogenic cartilage damage. 18 Recently, the cross-grip suture was proposed to combine vertical mattress fixation at the posterior tear edge with a single crossing horizontal stitch toward the anterior horn, thereby minimizing suture bulk while maintaining or improving fixation strength. 12
Biomechanical evaluations of meniscal sutures traditionally involve simple “pull-to-failure” and gap tests.12,19,20 These assessments apply unidirectional tension parallel to the tear axis and measure ultimate load or gap formation.1,3,5,11,16,17 However, these tests represent “worst-case scenarios” and fail to reproduce the complex multidirectional shear and compression experienced in vivo. In contrast, 6 degrees of freedom (6-DOF) robotic simulators have recently enabled more physiologically relevant evaluations by simulating realistic knee joint motions and dynamic loading conditions.7-10 The robotic system mimics the knee joint motion by stabilizing the femur and actuating the tibia. The coordinate axes of the femur and tibia are aligned by referencing the tibial axis in full extension. As the simulator continuously records both the displacement of the tibial origin and the loads acting on the tibia during knee motion, it enables calculation of the meniscal resultant force, which was defined as the net force transmitted through the knee joint, and the tibial shift and rotation relative to the femur (ie, tibiofemoral relationship).
Despite the potential of 6-DOF robotic platforms, few studies have utilized them to compare clinical suture methods under dynamic joint loading directly. To fill this gap, we evaluated 3 suture techniques—horizontal, tie-grip, and cross-grip—using a 6-DOF simulator using 2 clinically relevant protocols:
Flexion-extension cycling motion under a constant valgus torque, measuring meniscal resultant force and tibiofemoral relationship
Repetitive axial loading for 300 cycles, tracking changes in resultant force and tibiofemoral relationship over time
By systematically assessing the restoration of load-bearing function and joint stability under both dynamic motion and repetitive loading, we aimed to identify which suture technique most robustly reinstates lateral meniscus strength and stability after a radial tear. This is the first study to investigate repetitive loading on meniscal sutures using a 6-DOF simulator. Our findings may provide valuable insights to enhance surgical outcomes and preserve long-term knee health in patients undergoing meniscal repair.
Methods
Ethical Approval
This article does not contain any studies using living animals performed by any of the authors. All knee specimens were obtained from edible swine purchased from a local butcher. Therefore, ethical approval for animal research was not required.
Specimens
This study utilized 12 fresh-frozen porcine right knees from 6-month-old swine, specifically chosen to avoid osteoarthritis or ligamentous fractures. Specimens were stored at −30°C and thawed at 4°C for 24 hours before dissection to ensure tissue integrity. The surrounding tissues, including the muscles, were meticulously dissected.
Experimental Setup
The femur and tibia were fixed using resin and mounted on a 6-DOF robotic simulator (FRS-2015; Technology Service) (Figure 1a).7,9 This system is a velocity-controlled 6-DOF manipulator—3 translational (X, Y, Z) and 3 rotational (U, V, W) axes—driven by AC servomotors and coupled to a universal force/moment sensor (UFS-6520A250; Nitta) at the tibial clamp. Force/moment data are streamed via a multifunction data acquisition system into a real-time controller (National Instruments) and a LabVIEW 2013 real-time module on a Windows 8 PC (Dell). The manipulator, controller, and servo drives communicate over EtherNet/EtherCAT, and Sanyo Denki R2EA06020FXP00M servos power all actuators. 10 The bone axis of the femur was determined to align the coordinate axes of the femur and tibia, and the tibial coordinate axis was projected when the tibia was in an extended position. A nonorthogonal knee joint coordinate system—comprising flexion-extension about the femoral fixed axis, internal-external rotation about the tibial fixed axis, and a floating axis perpendicular to both—was used for both kinematic path reproduction and force/moment transformation. 7 A universal force/moment sensor (UFS) provided motion commands to the tibia. The UFS detects the movement of the origin during tibial motion, enabling the measurement of the moment and force applied to the tibia (Figure 1b). 10 By reproducing the intact knee path without the meniscus, the UFS data also allow resultant force estimation via the principle of superposition. 9 To accommodate the extension lag in porcine knees, the extension angle at 1000 Nm of torque was considered the reference extended position, and the extension angle at each time point was adjusted as a correction value to facilitate comparable measurements in porcine knees.
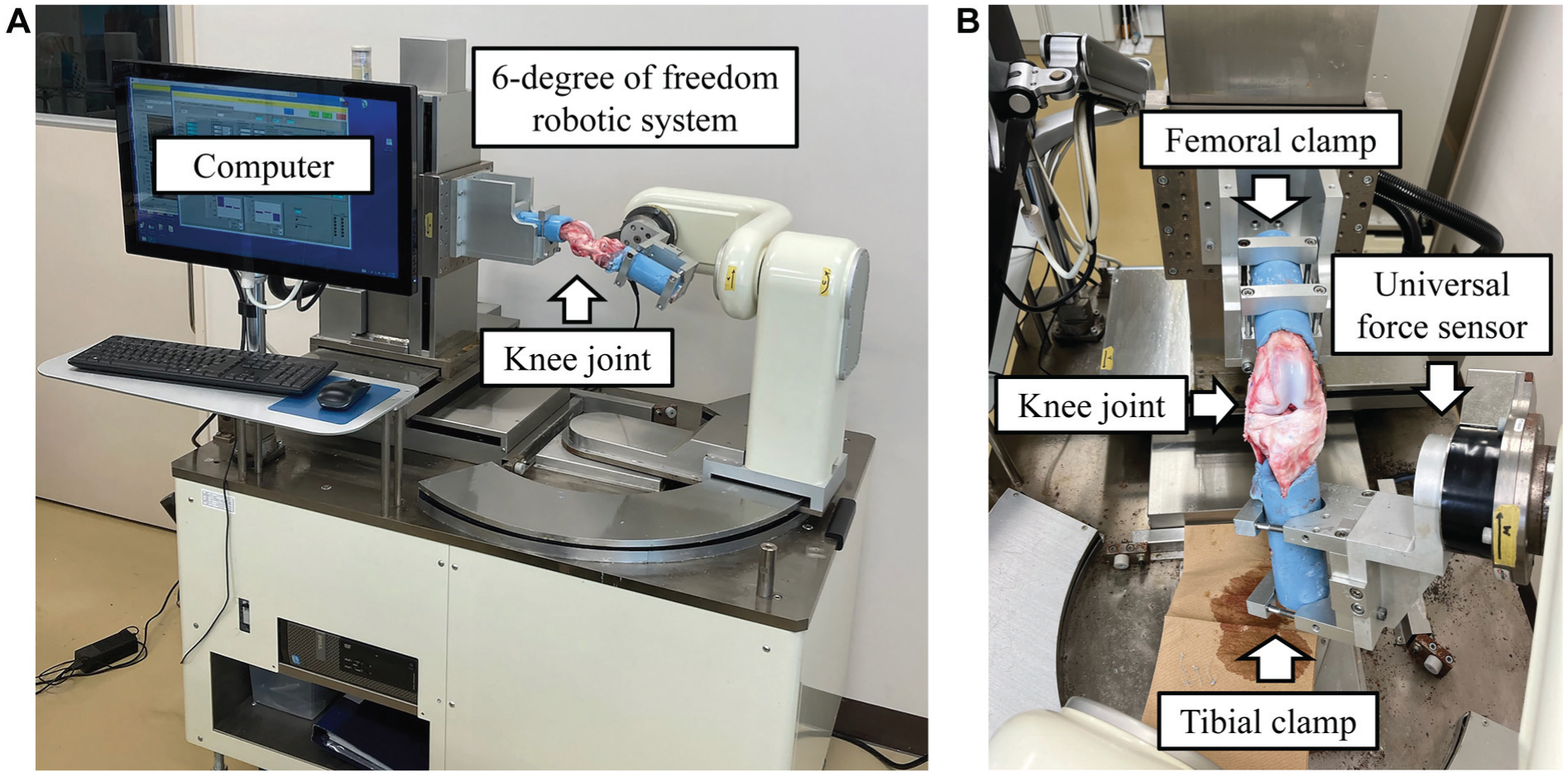
Six degrees of freedom (6-DOF) robotic simulator. (a) The 6-DOF robotic system receives movement commands from the computer and performs knee joint movements such as flexion and extension. (b) The femur and tibia are attached to the respective clamps. The universal force sensor senses the motion of the knee joint, and the coordinate data are transmitted to the computer.
Experimental Design
Two experiments were conducted. The first experiment aimed to compare knee joint flexion-extension movements (n = 6), and the second experiment compared responses under repetitive loading (n = 6).
Lateral Meniscus Conditions
The lateral meniscus was exposed without detaching or cutting ligaments, allowing direct visualization and creating tears and sutures. After attaching the knees to the 6-DOF robotic system, the lateral meniscus conditions were simulated, including intact, radial tear, horizontal, tie-grip, and cross-grip sutures (Figure 2). Each meniscal state was tested using 6 porcine knee specimens.

Lateral meniscus conditions. Five different forms of the lateral meniscus were investigated: intact, radial tear, horizontal, tie-grip, and cross-grip sutures. A radial tear was defined as a 100% tear extending from the inner rim to the outer edge (limbus). Lateral meniscus procedures were performed with the knee joint attached to a 6 degrees of freedom robotic system.
Experimental Measures
Appropriate saline irrigation was applied to prevent tissue degradation during testing. Furthermore, to minimize errors owing to meniscal tissue degradation over time, suturing was performed using the following patterns:
Horizontal suture → tie-grip suture → cross-grip suture
Horizontal suture → cross-grip suture → tie-grip suture
Tie-grip suture → horizontal suture → cross-grip suture
Tie-grip suture → cross-grip suture → horizontal suture
Cross-grip suture → horizontal suture → tie-grip suture
Cross-grip suture → tie-grip suture → horizontal suture
In the first experiment, the knee joint was subjected to a 5-Nm valgus torque and a flexion-extension test, in which the knee was flexed from the extended position to 120° at an angular velocity of 1 deg/s 3 times. The first and second tests were conducted to eliminate creep, and the data from the third test were recorded. Data were collected at knee flexion angles of 30°, 60°, 90°, and 120°.
In the second experiment, the knee joint was fixed at 60° of flexion, and an axial load of 150 N was applied to the tibia 300 times with a cycle of 10 per second. Data were collected after 0, 50, 100, 200, and 300 repetitions of the axial loading cycle with a valgus torque of 5 Nm.
Measurement of Resultant Force
The resultant force was defined as the net force transmitted through the knee joint, representing the load-bearing function of the meniscus. 8 To measure this, the 3-dimensional knee path and corresponding forces (f[x], f[y], f[z]) were recorded for each meniscal state. After completing the test protocols, the lateral meniscus was completely removed, and the simulator reproduced the previously recorded knee paths to measure forces without the meniscus (f′[x], f′[y], f′[z]). The resultant force (F) was calculated using the following formula:
This calculation allowed the evaluation of meniscal function under various loading conditions.
Measurement of Tibiofemoral Relationship
The tibiofemoral relationship was defined as the tibial shifts and rotations relative to the femur. Shifts were measured in the medial-lateral and anterior-posterior directions, whereas rotations were assessed in valgus-varus and internal-external rotation directions. In this study, tibial shifts and rotations for each test condition were expressed as the difference from the values recorded in the intact knee, following the methods of previous reports.12,18
Statistical Analysis
Statistical analysis was performed using 1-way analysis of variance and Tukey post hoc tests. Experiment 1 compared the effects of different lateral meniscus morphologies at each knee flexion angle. Experiment 2 involved 2 comparisons: (1) a comparison of the lateral meniscus morphology at each repetition cycle and (2) a comparison of the effect of different lateral meniscus morphologies at each repetition cycle. All analyses were performed using R software (2020; R Foundation for Statistical Computing). The findings are presented as mean ± standard deviation, and statistical significance was attributed to results with P values <.05.
Results
Experiment 1
The resultant forces are presented in Figure 3. Radial tear reduced the resultant force of the meniscus by approximately 50% at 30°, 45% at 60°, 54% at 90°, and 78% at 120° versus intact. Horizontal, tie-grip, and cross-grip sutures restored forces to within 5% to 15% of intact values. The cross-grip suture showed higher values in 30°, 60°, and 90° of knee flexion.

Resultant force of the lateral meniscus in the first experiment, obtained at each knee flexion angle during the flexion-extension movement with a valgus torque of 5 Nm. *P < .05 and **P < .01 versus radial tear.
The tibiofemoral relationships—defined as tibial shifts and rotations relative to the femur and expressed as differences from the intact knee—are shown in Figure 4. Anterior-posterior translation did not differ for both the tear and 3-suture states. A radial tear caused a medial shift of 2.15 mm at 30° of flexion, and only the tie-grip suture stabilized the medial shift effectively. Radial tear increased valgus rotation at all 4 flexion angles, and all 3 sutures effectively reduced the abnormal rotation. Radial tear showed an internal rotation of 5.80° at 30° and 3.77° at 60°; the horizontal, tie-grip, and cross-grip sutures reduced these to 3.88° to 4.55° at 30° and 1.91° to 4.50° at 60°, without showing a significant change.

Tibial shift and rotation in the first experiment. (a) Anterior-posterior shift. (b) Medial-lateral shift. (c) Valgus-varus rotation. (d) Internal-external rotation of the tibia during a flexion-extension movement with a valgus torque of 5 Nm. *P < .05 and **P < .01 versus radial tear.
Experiment 2
The resulting forces are presented in Figure 5. Sutured menisci maintained >90% of intact force through 300 cycles, whereas radial tears remained at up to 33%. The cross-grip suture maintained the highest values among the suturing techniques. No meaningful force reduction was observed in any of the sutured conditions after 300 cycles.

Resultant force of the lateral meniscus in the second experiment, when a valgus torque of 5 Nm was applied after repeated axial loading of 150 N. *P < .05 and **P < .01 versus radial tears.
The results of the tibiofemoral relationships are shown in Figure 6. After 300 cycles, an anterior shift in the radial tear reached 0.42 mm. In contrast, horizontal, tie-grip, and cross-grip sutures limited this to 0.26 mm, a 0.18-mm posterior shift, and 0.12 mm, respectively. Medial shift measured 4.22 mm in the tear group but was reduced to 0.19 mm, 0.40 mm, and 0.87 mm by horizontal, tie-grip, and cross-grip sutures, respectively. Valgus rotation increased to 7.23° in tears, while sutures constrained rotation to −0.07°, 1.64°, and 2.02°, respectively. Internal rotation showed 14.16° of internal rotation after tearing, with sutures partially correcting to 8.02°, 2.51°, and 1.66° for horizontal, tie-grip, and cross-grip sutures, respectively.

Tibial shift and rotation in the second experiment. (a) Anterior-posterior shift. (b) medial-lateral shift. (c) valgus-varus rotation. (d) internal-external rotation of the tibia when a valgus torque of 5 Nm is applied after repeated axial loading of 150 N. *P < .05 versus radial tear.
Discussion
Our findings confirm that horizontal and tie-grip sutures restore meniscal force transmission and correct valgus instability. This is consistent with the pressure loading comparisons by Zhang et al 22 in cadaveric knees under manually controlled valgus-varus alignment. However, unlike the study by Zhang, which reported superior tie-grip performance under static loading, and other pull-to-failure test studies,15,17 our 6-DOF robotic data revealed minimal differences in resultant force between horizontal and tie-grip sutures both during initial flexion-extension and after cyclic loading. This suggests that, under dynamic flexion angles and multiplanar loading, the mechanical advantage of the tie-grip is attenuated. Nevertheless, our model did not encompass all complex in vivo movements or long-term biological effects, so further investigation is warranted.
The newly introduced cross-grip suture demonstrated effect sizes comparable to or exceeding those of established methods at midflexion angles (30°-90°). Its design optimizes load sharing across the meniscal wedge, translating to approximately the same force restoration at 60°, and sustained performance through 300 cycles. This advantage may be particularly beneficial for athletes or individuals engaged in sports involving repetitive and varying knee flexion angles.
Comparison with previous cyclic loading studies15,17 indicates that, unlike those protocols, which often applied repeated tensile or compressive loads in isolation, our simultaneous evaluation of resultant force, translation, and rotation under 6-DOF conditions captured a more holistic picture of suture performance. Notably, while all 3 suturing techniques effectively improved medial-lateral displacement and valgus rotation, internal rotational laxity was induced by repetitive loading, and no fully corrected internal rotation was caused by radial tear. However, after repetitive loading, tie-grip and cross-grip sutures limited the internal rotation compared with the horizontal suture. These findings may underscore their greater resistance to rotational instability under repetitive stress. They also point to the need for further study, ideally with larger sample sizes and clinical assessments of rotational laxity, to determine its relevance in vivo.
Although this study provides valuable insights into the biomechanical properties of lateral meniscus suturing methods and their potential clinical applications, it has several limitations.
Animal model: This study used fresh-frozen porcine specimens, which may not fully represent the human knee’s complex anatomic and physiological characteristics. Although porcine knees are commonly used as models for orthopaedic research because of their similarities to human knees, inherent differences can affect the translation of these findings to human patients.
Short-term assessment: The biomechanical evaluations in this study were conducted at time zero after meniscal suturing, and the model does not account for restricted weightbearing or biological healing over time.
Simplified loading conditions: Axial (150 N) and valgus (5 Nm) loads under 6-DOF motion capture common stresses but do not cover the full spectrum of in vivo joint forces during daily activities or sports.
Lack of clinical outcomes: This study focused solely on biomechanical comparisons. Clinical outcomes, such as patient-reported outcomes, functional scores, and success rate of meniscal healing, were not assessed.
Sample size and statistical power: Consistent with previous studies, we used 6 porcine specimens per group to generate preliminary effect sizes; however, a larger sample may yield different results and strengthen statistical inferences.
Single robotic platform: Although the 6-DOF robotic simulator allowed for sophisticated motion analysis, this study used a single robotic platform for all evaluations. Using multiple robotic platforms or incorporating other testing methodologies can provide additional insights into the biomechanical performance of suturing methods.
Future studies should use human cadaveric specimens to evaluate biomechanical performance under more clinically relevant conditions. In addition, in vivo models may investigate biological healing processes associated with different suturing techniques. Combining biomechanical and biological assessments will allow a more comprehensive understanding of meniscal repair outcomes. Clinical trials with patient-reported outcomes and imaging follow-up will determine whether cross-grip sutures improve repair integrity and functional recovery.
Despite these limitations, using a cutting-edge 6-DOF robotic simulator to investigate lateral meniscus suturing methods is a novel approach in orthopaedic research. These findings provide a basis for future research and clinical trials to evaluate the potential benefits of cross-grip sutures. Ultimately, this may improve surgical techniques and long-term outcomes in patients with lateral meniscus tears.
Conclusion
The cross-grip suture technique offers biomechanical advantages, particularly restoring resultant force at midrange flexion angles and during repetitive loading, compared with conventional horizontal and tie-grip sutures under realistic knee motion. While all methods improved kinematics relative to radial tears, the consistent performance of the cross-grip suture suggests its promise for early rehabilitation protocols and long-term meniscal preservation. Further powered studies are warranted to confirm these effect size trends and evaluate clinical efficacy.
Footnotes
Acknowledgements
The authors thank Yasuraku Shibata, Chenxu Huang, and Daichi Ishii for their assistance with the 6-DOF robotic testing, and Yuki Shiko and Kohei Takahashi for their valuable insights on the statistical analysis.
Final revision submitted June 19, 2024; accepted July 15, 2025.
The authors declared that they have no conflicts of interest in the authorship and publication of this contribution. AOSSM checks author disclosures against the Open Payments Database (OPD). AOSSM has not conducted an independent investigation on the OPD and disclaims any liability or responsibility relating thereto.