Abstract
Background:
Medial patellofemoral ligament reconstruction (MPFLR) using the quadriceps tendon can avoid complications related to the fixation of other graft types to the patella. However, there is concern about postoperative loss of knee extensor muscle strength because of harvesting a portion of the quadriceps tendon.
Hypothesis:
Knee extensor muscle strength after superficial slip of the quadriceps tendon MPFLR (SQ-MPFLR) decreases postoperatively, and there are specific factors that effect knee extensor muscle strength recovery.
Study Design:
Case series study; Level of evidence 4.
Methods:
A total of 26 patients who underwent unilateral primary SQ-MPFLR were enrolled. Clinical and functional outcomes were evaluated using the Kujala score and Tegner activity score preoperatively and 12 months postoperatively. Knee extensor muscle strength was examined preoperatively and 6 and 12 months postoperatively using the Biodex dynamometer. The knee muscle strength of the operated leg was compared with that of the contralateral leg using the limb symmetry index (LSI). The associations of sex, body mass index, and daily sports activity level with knee extensor muscle strengths at 6 and 12 months postoperatively were investigated and compared between the 2 groups.
Results:
The preoperative mean Kujala score was 65.0 and significantly improved to 94.7 at 12 months after surgery (P < .001). The preoperative Tegner activity score was 5.6, and the 12-month postoperative score was 5.8. The knee extensor LSI increased from 69.2% preoperatively to 82.0% at 12 months postoperatively. The patient group with a high sports activity level had a significant higher knee extensor muscle LSI (mean, 87.8%) than the group with a low sports activity level at 12 months postoperatively (P = .003).
Conclusion:
The knee extensor LSI of patients who underwent SQ-MPFLR increased from 69.2% preoperatively to 82.0% postoperatively at 12 months. The patient group with a high sports activity level had a significantly higher knee extensor LSI than the group with a low sports activity level at 12 months after SQ-MPFLR surgery.
Keywords
Acute dislocation of the patella commonly occurred among adolescents and young adults, and almost 50% of primary dislocations resulted in recurrent dislocations. 2 For many patients with recurrent patellar dislocation, surgical treatments are necessary. Many surgical methods have been developed for recurrent patellar dislocations. Among many surgical procedures, medial patellofemoral ligament reconstruction (MPFLR) has become one of the most frequently used procedures because the medial patellofemoral ligament (MPFL) is the most important stabilizer of the patella. Recently, numerous reports related to MPFLR have shown good results,7,14 and MPFLR has become the most important procedure for recurrent dislocation of the patella.
Most MPFLRs for recurrent patellar dislocation use hamstring tendons as the graft materials. However, some complications of MPFLR using the knee flexor tendon have been reported. Complications include patellar fractures resulting from patellar bone tunnel fabrication and irritation caused by the internal fixation metal, such as the Endobutton used for tendon fixation.1,9 On the contrary, MPFLR using the quadriceps tendon can avoid the aforementioned complications related to the patella. Since Steensen et al 11 mentioned their method of MPFLR using the quadriceps tendon, there have been some reports about the method and clinical results.8,13 Goyal 4 described the superficial quadriceps technique to provide anatomic patellar fixation without a bony procedure and without patellar complications. Fink et al 3 developed a new harvesting technique for the quadriceps tendon that allows not only consistent width and thickness of graft harvest but also a smaller skin incision. While there is concern regarding the postoperative loss of knee extensor muscle strength after MPFLR using the superficial slip of the quadriceps tendon (SQ-MPFLR) because of the harvesting of a portion of the quadriceps tendon, there are no studies that have verified the postoperative knee extensor muscle strength after SQ-MPFLR.
The purpose of this study was to clarify the postoperative knee muscle strength and recovery process after SQ-MPFLR, and to analyze the factors affecting extensor strength recovery. We hypothesized that knee extensor strength would decrease after SQ-MPFLR, and there are specific factors that affect knee extensor muscle strength recovery.
Methods
Study Design
A prospective case series study was conducted between October 2016 and September 2021 to investigate the outcomes of MPFLR using a superficial slip of the quadriceps tendon graft for recurrent patellofemoral instability. A total of 4 centers (Hokushin Orthopaedic Hospital, Yagi Orthopaedic Hospital, NTT Medical Center Sapporo, Hokkaido University Hospital) participated in this trial. This study was approved by the ethics committee of Hokushin Orthopaedic Hospital and the other 3 hospitals. Documented informed consents were obtained from all patients.
Clinical and functional outcomes were evaluated using the Kujala score and Tegner activity score preoperatively and 12 months postoperatively. All patients were asked about re-dislocation and complications. Radiographic evaluation included measuring the patellar tilt angle and lateral shift ratio preoperatively and 12 months postoperatively by capturing the axial view at 30° of knee flexion on plane radiographs. Knee extensor muscle strength was examined preoperatively and 6 and 12 months postoperatively. To clarify factors that affect the recovery of postoperative knee extensor muscle strength, 3 items were chosen as predictive factors. Patients were categorized based on sex, body mass index (BMI), and daily sports activity level. BMI categories were defined as >30 or <30, in accordance with the World Health Organization’s classification of obesity. The high-activity group comprised individuals who exercised ≥4 times per week, while the low-activity group consisted of those who exercised <4 times per week. Extensor muscle strength was compared between the 2 groups for each factor.
Patients
Surgical indications of SQ-MPFLR were recurrent dislocation of the patella and patellar dislocation with a patellar avulsion fracture. The inclusion criteria for this study were as follows: (1) patients who underwent primary SQ-MPFLR, (2) patients who were followed for at least 1 year, and (3) patients with knee extensor muscle strength measurements before surgery and 6 and 12 months after surgery. The exclusion criteria for this study were as follows: (1) patients who had previous surgery in the same knee, (2) patients with tibial tubercle–trochlear groove distance >20 mm on the computed tomography, and (3) patients requiring tibial tubercle osteotomy for distal re-alignment of the predisposing factors.
Between October 2016 and September 2021, a total of 51 patients underwent SQ-MPFLR at 4 hospitals. Six patients met the exclusion criteria. In addition, 19 cases were excluded because 2 cases had SQ-MPFLR on the contralateral side, complete data of knee extensor and flexor muscle strength could not be collected in 15 cases, 1 case had a psychological disease after SQ-MPFLR, and 1 case had anterior cruciate ligament reconstruction after SQ-MPFLR. A total of 26 patients (8 male and 18 female) who met the inclusion and exclusion criteria were enrolled in this study (Figure 1). The mean age was 19 years (range, 13-49 years). The mean follow-up period was 17.2 months (range, 12-31 months). Nineteen knees had recurrent patellar dislocation, and 7 knees had primary dislocation with a patellar fracture.

Flowchart of the enrolled patients. ACL, anterior cruciate ligament; SQ-MPFLR, strength after superficial slip of the quadriceps tendon medial patellofemoral ligament reconstruction.
Surgical Method
Arthroscopic examination was performed before MPFLR to manage the intra-articular injuries. The graft was harvested from the superficial slip of the quadriceps tendon. With knee flexion of 90°, a 3- to 4-cm longitudinal or transverse skin incision was made over the superior pole of the patella. After the quadriceps tendon was identified, a 10 mm–wide superficial slip was dissected proximally to the required length using a double knife (Karl Storz). The dissection interval between the superficial slip and middle laminae of the quadriceps tendon was most readily identified 3 cm proximal to the patella. After an interval between the superficial and middle laminae was identified, the thickness of the graft was determined with a 3-mm tendon separator (Karl Storz). The separator was pushed proximally to the required length. Then the tendon strip was cut at the proximal end of the strip subcutaneously by a tendon cutter (Karl Storz). The proximal end of the tendon strip was sutured using Ethibond No. 2 (Ethicon, Johnson & Johnson Ltd) in a baseball grab suture method. The native MPFL attaches at the supra-medial corner of the patella and at the midpoint of the medial margin of the patella. 12 Considering these anatomic points, the medial edge of the harvested tendon was dissected under the periosteum using a sharp chisel until approximately 6 mm distal from the superior border of the patella. The lateral margin of the strip was further dissected subperiosteally to the center of the patella in an oblique manner. The graft was left attached to the proximal part of the patella and then rotated 90° medially. Subsequently, the graft was sutured to the patella periosteum and passed through a tunnel between the capsule and the vastus medialis toward the femoral insertion of the MPFL. A 7 mm–diameter bone tunnel was created at the Schöttle point under fluoroscopy. The graft was pulled into the bone tunnel with the patella centered at the trochlea, and then the graft was fixed using an absorbable interference screw (7 × 23-mm MILAGRO Advance Interference Screw; DePuy Synthes America) under appropriate tension (10-20 N) at 30° of knee flexion (Figure 2).
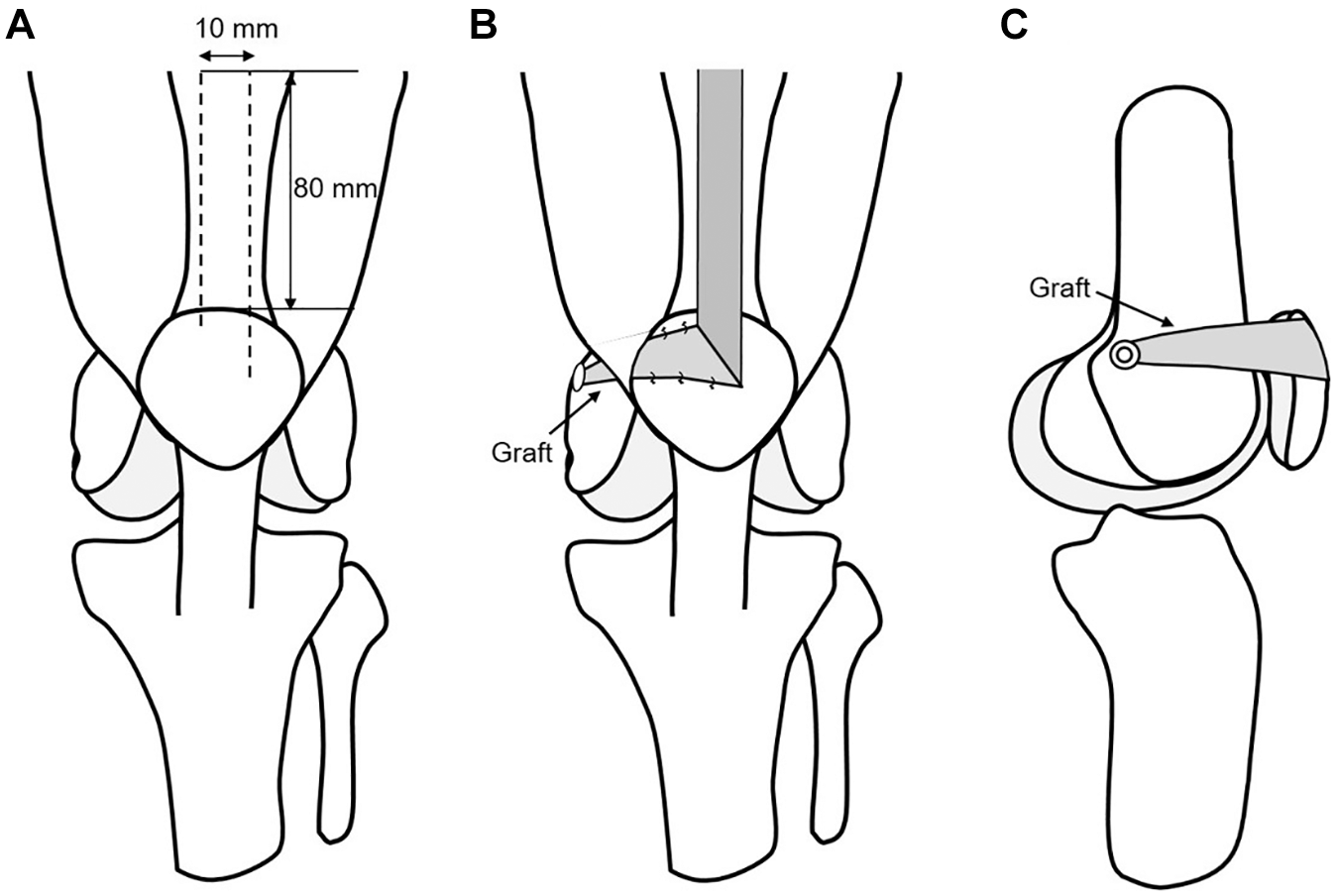
Schema of surgical methods. Diagrammatic representation of graft harvest, graft rotation, patellar fixation, and femur fixation. (A) The superior border of the MPFL is approximately 6 mm below the superior pole of the patella, and the inferior border is roughly near the midpoint of the patella. The plane and dissection points for graft harvest. (B) The graft is rotated and turned medially to mimic the anatomic position of the native MPFL. Stay sutures at the patella provide anatomic patellar fixation. (C) Creation of a bone tunnel at the Schöttle point and fixing the graft with a 7-mm absorbable interference screw.
Postoperative Protocol
Postoperatively, full weightbearing as tolerated was allowed from day 1 with a straight knee splint. The straight knee splint was discontinued when the patient had gained quadriceps control. Range of motion exercise while seated was started at 1 week postoperatively. Quadriceps sets and straight leg raise were permitted immediately after surgery, and closed kinetic chain exercises such as squat started at 3 weeks postoperatively. Stationary cycling was initiated at 4 weeks postoperatively, and jogging was permitted from 3 months postoperatively. Return to sports was permitted between 4 and 6 months postoperatively.
Knee Muscle Strength Examination
The knee extension isokinetic muscle strength of patients with patellar instability was measured using the Biodex System 3 dynamometer at an angular velocity of 60 deg/s before surgery and 6 and 12 months after surgery. The knee extensor muscle strength was evaluated using the limb symmetry index (LSI) as follows: LSI (%) = (peak torque in the affected limb/peak torque in the contralateral limb) × 100.
Statistical Analysis
All data were analyzed using R software (Version 4.1.2; R Foundation for Statistical Computing). A repeated-measure analysis of variance was performed to evaluated knee extensor LSI. Tukey-Kramer post hoc testing was performed to evaluate knee extensor LSI changes before and after surgery. The Kujala score was statistically tested using the Welch 2-sample t test between the preoperative and 12-month postoperative periods. The Tegner activity score was statistically tested using the Student t test between the preoperative and 12-month postoperative periods. The patellar tilt angle and lateral shift ratio from preoperatively to 12 months postoperative were statistically tested using the Welch 2-sample t test. The significance level was set at 5%. Knee extensor LSI and knee flexor LSI in the 2 groups (sex, BMI, and sports activity level) were statistically tested using the Mann-Whitney U test. For the Mann-Whitney U test, the significance level was set at 1%.
Results
The preoperative mean Kujala score was 65.0 (range, 27-98) and significantly improved to 94.7 (range, 78-100) at 12 months postoperatively (P < .001). The mean Tegner activity score was 5.6 preoperatively and 5.8 at 12 months after surgery (Table 1). There was no re-dislocation postoperatively and no complications such as patellar fracture or irritation due to graft fixation devices.
Kujala Score and Tegner Activity Score Before and After Surgery a

Data are reported as mean ± SD.
The preoperative mean patellar tilt angle was 18.8° (range, 1.7°-26.2°) and significantly improved to 10.6° (range, 1.6°-20.1°) at 12 months postoperatively (P < .001). The preoperative mean lateral shift ratio was 15.9% (range, 7.0%-47.4%) and significantly improved to 7.4% (range, 0%-15.9%) at 12 months postoperatively (P = .01).
The knee extensor LSI decreased from 69.2% preoperatively to 61.0% at 6 months postoperatively, but recovered to 82.0% at 12 months postoperatively. A significant difference in knee extensor LSI was found between 6 months and 12 months postoperatively (P = .04). However, there was no statistically significant difference between the preoperative and 12-month postoperative knee extensor LSI (P = .40).
Significant differences in knee extensor LSI were not recognized between the 2 groups in sex and BMI. The high sports activity group had a significantly higher knee extensor LSI (mean, 87.8% ± 13.2%) than the low sports activity group (mean, 68.9% ± 14.7%) at 12 months postoperatively (P = .003) (Table 2).
Knee Extensor LSI (%) Results From Comparison Between the 2 Groups a

Data are reported as mean ± SD. BMI, body mass index; LSI, limb symmetry index; postop, postoperatively.
Discussion
The current study showed that the knee extensor LSI of the patient who underwent SQ-MPFLR recovered from a mean of 69.2% preoperatively to 82.0% at 12 months postoperatively. We did not observe a statistically significant difference in knee extensor LSI from preoperatively to 12 months postoperatively; however, it was confirmed that knee extensor muscle strength had recovered to a level higher than its preoperative strength.
Matsushita et al 6 reported that the mean isokinetic extensor strength ratio of the operated leg at 60 deg/s after MPFLR using the semitendinosus tendon graft at 2 years postoperatively was approximately 80%. Malecki et al 5 reported the mean isokinetic extensor strength ratio of the operated leg at 60 deg/s after MPFLR using the the adductor magnus tendon at 1 year after surgery was 84.2%. The current study showed that the knee extensor muscle strength LSI of patients who underwent SQ-MPFLR recovered 82.0% at 12 months postoperatively. The knee extensor muscle strength after SQ-MPFLR was comparable to that after MPFLR using the hamstring tendon or adductor magnus tendon.
In this study, the Kujala score improved from 65.0 preoperatively to 94.7 at 12 months after surgery. Vavalle and Capozzi 13 reported that the mean Kujala score improved from 35.8 preoperatively to 88.8 at a mean follow-up of 2.6 years after MPFLR using the quadriceps tendon. Nelitz et al 8 reported that the mean Kujala score improved from 63 preoperatively to 89 at a mean follow-up of 38 months after MPFLR using the quadriceps tendon. The clinical results of this present study were satisfactory compared with those of other studies.
Rhatomy et al 10 reports that quadriceps strength was measured using a handheld dynamometer, and there was no difference in the mean quadriceps strength between the donor and contralateral knees at 6 months after MPFLR using the quadriceps tendon autograft. In this study, we utilized the Biodex dynamometer to evaluate knee extensor strength, and we are confident that this allowed us to report more accurate values compared with those obtained with the handheld dynamometer.
To obtain a better muscle strength recovery, it is necessary to identify the factors that affect recovery of postoperative knee extensor muscle strength. In the current study, knee extensor LSI at 12 months postoperatively was significantly lower in the group with a low sports activity. This result suggests that low sports activity may have affected knee extensor muscle strength recovery. For the low sports activity group, the motivation and desire to regain muscle strength and return to sports may be considered relatively low compared with the high sports activity group. Therefore, for SQ-MPFLR, it was necessary to improve the postoperative rehabilitation protocol for the low sports activity group by setting goals of knee extensor muscle strength at 3, 6, and 9 months after surgery.
Limitations
The limitations of this study include the small number of cases and the short follow-up period. Furthermore, multivariable analysis was not able to detect the factors affecting knee muscle strength recovery because of the limited numbers.
Conclusion
The knee extensor muscle strength LSI of patients who underwent SQ-MPFLR increased from 69.2% preoperatively to 82.0% at 12 months postoperatively. The patient group with a high sports activity level had a significantly higher knee extensor LSI than the group with a low sports activity level at 12 months after SQ-MPFLR surgery, suggesting that patients with low preoperative sports activity are at risk for delayed postoperative muscle strength recovery.
Footnotes
Final revision submitted October 24, 2024; accepted November 11, 2024.
The authors declared that they have no conflicts of interest in the authorship and publication of this contribution. AOSSM checks author disclosures against the Open Payments Database (OPD). AOSSM has not conducted an independent investigation on the OPD and disclaims any liability or responsibility relating thereto.
