Abstract
Background:
A decreased hamstring tendon (HT) autograft diameter has been associated with higher rates of failure in primary anterior cruciate ligament reconstruction (ACLR).
Purpose:
To determine whether an HT autograft diameter ≥8 mm has an effect on the risk of graft failure and subsequent knee surgery after ACLR in a prospective cohort.
Study Design:
Cohort study; Level of evidence, 2.
Methods:
Patients undergoing primary ACLR with an HT autograft were included and followed prospectively for 2 years to capture subsequent surgery events performed in either knee. The effect of HT autograft diameter on the risk of subsequent surgery was analyzed using multivariable regression modeling that adjusted for patient age, sex, body mass index, and Marx activity score.
Results:
Of 421 eligible patients, 381 (90.5%) had a minimum 2-year follow-up and were included in analysis. The median autograft diameter was 8.5 mm (interquartile range, 8.0-9.0 mm); 90.8% of patients received an autograft with a diameter ≥8 mm. There were 59 patients (15.5%) who underwent subsequent ipsilateral knee surgery, including 27 patients (7.1%) who had graft failure and underwent revision ACLR within 2 years. HT autograft diameter was not associated with the risk of all subsequent ipsilateral knee surgery (odds ratio [OR], 0.87 [95% CI, 0.56-1.36]; P = .536) or revision ACLR (OR, 0.71 [95% CI, 0.38-1.33]; P = .286). A Marx activity score ≥12 was associated with an increased risk of all subsequent ipsilateral knee surgery (OR, 2.55 [95% CI, 1.41-4.59]; P = .002). Younger age was associated with an increased risk of revision ACLR (OR, 0.16 [95% CI, 0.05-0.51]; P = .002).
Conclusion:
A minimum HT autograft diameter of 8 mm was not associated with the risk of revision ACLR or other subsequent surgery in the ipsilateral or contralateral knee. This study may guide intraoperative decision making regarding HT autograft implementation in ACLR.
Keywords
An anterior cruciate ligament (ACL) rupture remains a common injury, with studies suggesting a cumulative lifetime incidence of up to 3.5% in female athletes and 2.0% in male athletes. 23 ACL reconstruction (ACLR) has proven to be a successful surgical procedure for patients wishing to limit symptoms of instability and return to athletic activity.24,37,41 However, ACL graft failure endures as a persistent complication in the present era of ACLR, with modern cohort studies continuing to demonstrate failure rates of up to 9.2%. 25
Cohort studies investigating long-term ACLR outcomes have identified patient and injury characteristics that help delineate the optimal graft choice for individual patients.14,15,20,25 The hamstring tendon (HT) autograft continues to demonstrate robust clinical outcomes for most patients.15,25,26 Contrary to the bone–patellar tendon–bone autograft, which is traditionally harvested with a width of 10 mm, HT autograft diameter is less predictable secondary to variable patient anatomy and versatile surgical techniques for graft harvesting and preparation.6,7,27 Magnussen et al 18 published a retrospective study in 2012 that demonstrated an association between an HT autograft diameter ≤8 mm and surgical failure after ACLR, thereby encouraging surgeons to incorporate the largest HT autograft diameter possible in ACLR. Multiple studies have subsequently found a similar association between a smaller HT autograft diameter and inferior patient outcomes, including an increased risk of graft failure.16,18,19,29,35,36,38 Historically, studies have shown equal and perhaps superior biomechanical properties of HT autografts in ex vivo settings.9,27,45 However, more recent biomechanical studies have demonstrated significantly inferior biomechanical performance in smaller HT grafts.2,11 Additional studies have investigated the utility of patient characteristics and imaging findings to predict the HT autograft diameter preoperatively and identify patients with limited HT autografts available for harvesting.8,17,34,40 Clinical studies have assessed whether smaller HT grafts require modifications with additional strands or augmentation with an allograft.4,30,43
The primary goal of this study was to determine whether an HT autograft diameter ≥8 mm reduces the risk of graft failure and subsequent knee surgery after ACLR in a prospective cohort. Our hypothesis was that an HT autograft diameter ≥8 mm would be associated with improvements in the rates of surgical failure and subsequent knee surgery within 2 years of index ACLR.
Methods
Study Population
This prospective longitudinal cohort study received institutional review board approval, and its patient enrollment, data collection, and study design were in compliance with the Health Insurance Portability and Accountability Act. Patients individually consented and were enrolled preoperatively to have their data prospectively collected, filed, and examined within a blinded institutional electronic data capture system. 28 A total of 1193 patients (age range, 13-66 years) consented to participate in the study and underwent primary ACLR from February 2015 to February 2018. Additional details regarding the methodology for completing enrollment, alteration of consent, patient-reported outcome collection, and surgical documentation with intraoperative findings and procedural aspects have been published previously.28,42 Inclusion criteria were skeletally mature patients undergoing primary ACLR using an HT autograft. Exclusion criteria were non–HT autografts, allograft augmentation, skeletally immature patients and/or physeal sparing reconstruction, revision ACLR, prior contralateral ACLR, and multiligament injuries.
Of the initial 1193 patients, 772 patients were excluded: 116 for undergoing revision ACLR, 51 for prior contralateral ACLR, 561 for not having HT grafts, and 44 for having allografts, resulting in 421 patients. Minimum 2-year follow-up data were collected for 381 patients (90.5%). Inclusion/exclusion criteria and follow-up data are outlined in Figure 1.
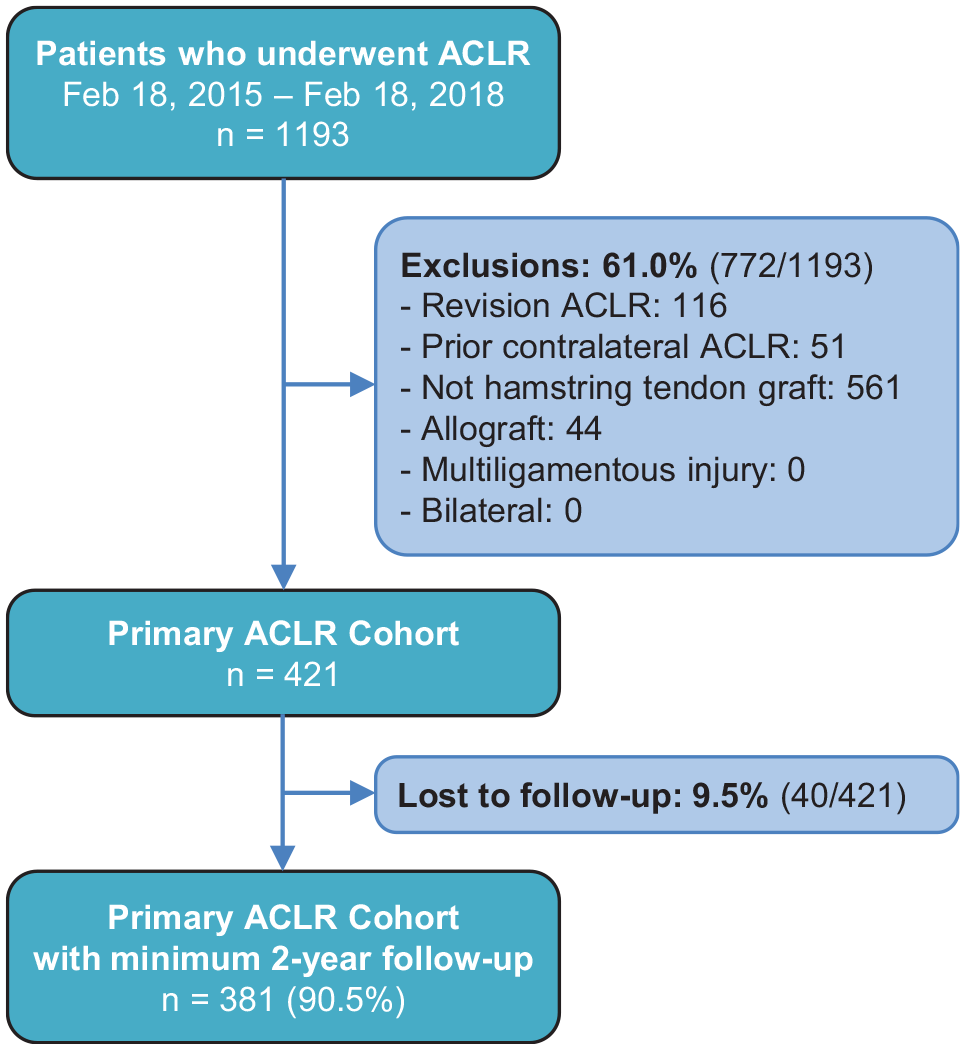
Study population inclusion/exclusion criteria and STROBE diagram. ACLR, anterior cruciate ligament reconstruction.
All included patients were operated on by 10 fellowship-trained sports medicine surgeons within a single institution. Each surgeon prepared his or her graft with the intent to maximize the diameter. The number of strands was per the surgeon’s discretion. Graft-sizing tubes were used to measure the graft diameter, and the tunnel size was selected accordingly to optimize the graft fit within the tunnel. One surgeon overdrilled the tunnel by 1 mm relative to the HT autograft (140 patients), 1 surgeon overdrilled by 0.5 mm (35 patients), 1 surgeon overdrilled by 0 to 0.5 mm based on fit (45 patients), and the remaining surgeons drilled their tunnels line to line with the measured autograft diameter (161 patients). In addition, 4 surgeons (67 patients) performed ACLR with only an HT autograft, and the remaining surgeons (314 patients) stratified their patients’ risk of graft failure and recommended an HT versus bone–patellar tendon–bone autograft accordingly.
Data Collection
Patients who elected to enroll signed the informed consent form and submitted demographic information including age, sex, body mass index (BMI), Marx activity score, 21 smoking status, and years of education before their surgery. Scores were also obtained preoperatively for the following patient-reported outcome measures: the Knee injury and Osteoarthritis Outcome Score (KOOS; pain, physical function short form, 31 and quality of life subscales), the Hospital for Special Surgery Pediatric Functional Activity Brief Scale 5 (HSS Pedi-FABS), and the Veterans RAND 12-Item Health Survey 13 (VR-12).12,33 The HSS Pedi-FABS was selected instead of the KOOS sports and recreation subscale because it demonstrates less concern for ceiling effects even when used with athletic populations.
Patients were contacted via a patient-designated method (eg, telephone, email, letter) at a minimum of 1 year postoperatively and asked to complete another set of the same patient-reported outcome measures (KOOS subscales for pain, physical function short form, and quality of life; HSS Pedi-FABS; and VR-12). Additionally, patients were asked whether they returned to their baseline work and sport (when appropriate) and whether they underwent subsequent surgery on either knee. Additional patient outreach was performed to obtain 2-year follow-up data on specific subsequent surgery events in either knee. Repeat knee injury events without subsequent surgery were not recorded. This follow-up was completed via telephone by a team of experienced research coordinators trained by surgeons to specifically discuss outcomes with patients regarding subsequent surgery, including whether surgery involved revision ACLR and/or an associated procedure (eg, meniscectomy). Operative reports were reviewed by an orthopaedic surgery resident to confirm surgical details when available. Individual outreach by the operating surgeon was employed for those who initially could not be reached via mailed patient-reported outcome measure forms and an institutional review board–approved letter that was personalized with surgical information, surgeon picture, and surgeon signature.22,39
Statistical Analysis
A test of normality was conducted for each continuous variable, and the median with interquartile range (IQR) were reported to better represent the observed skew in distribution. Categorical variables were displayed using counts and percentages. Age, sex, BMI, baseline Marx score, autograft diameter, and incidence of ipsilateral and contralateral knee surgery at 2-year follow-up were summarized. The baseline Marx score was also analyzed as a categorical variable to enable comparisons of a lower activity group (score <12) and a higher activity group (score ≥12). If patients elected to not provide the baseline Marx score, their score was recorded as “missing,” and they were included in the lower activity group (score <12). Surgeons collectively attempted to optimize graft fit within their tunnels, and the tunnel size was thereby determined to be an accurate measure of graft diameter. Consequently, HT autograft diameter was extrapolated from the recorded tunnel size. If varying tunnel sizes were drilled in the femur and tibia, the smaller diameter was utilized for analysis. HT autograft diameter and number of strands used were both analyzed as study variables within separate models.
Multivariable analyses were used to determine the incidence of ACLR failure and subsequent knee surgery for patients undergoing ACLR with an HT autograft at 2-year follow-up and establish patient and surgical variables associated with the risk. Separate multivariable analyses were conducted for the incidence of revision ACLR, all subsequent ipsilateral knee surgery, subsequent contralateral ACLR, and all subsequent contralateral knee surgery. The following variables were considered for the analysis of revision ACLR, subsequent contralateral ACLR, and all subsequent contralateral knee surgery based on the investigator’s intuition: age, sex, BMI, and autograft diameter. Given the higher number of events and additional degrees of freedom in the multivariable analysis of all subsequent ipsilateral knee surgery, baseline Marx score was added as another variable for this analysis.
Multivariable logistic regression models were built for each of these analyses and incorporated the respective covariables described above. Odds ratios (ORs) with 95% CIs and P values were reported. The relative importance of each variable in predicting the outcome of interest was ranked by the magnitude of increase in the Akaike information criterion (AIC) upon removal from the full model. 1 The AIC quantifies the amount of information explained by the variables in the model while penalizing the variables for the number of degrees of freedom that they have. A greater AIC increase indicates higher importance of the respective predictor in the model. 3 Generally speaking, an AIC increase of 2 indicates that the given variable contributes to a statistically better model. 3
For continuous variables, the ORs were rescaled to reflect the increase in the IQR (ie, an increase from the first quartile [Q1] to the third quartile [Q3] of the variables). The predictive accuracy of the model was assessed by the concordance probability (C-index) in which higher values indicate better performance. 10 Nomograms were produced to visualize model results. Data management and analysis were performed using R (Version 4.0). All tests were 2-sided, assuming an alpha level of 0.05.
Results
Characteristics of Study Population
Baseline characteristics for the 381 study patients are demonstrated in Table 1. The median age was 23.0 years (IQR, 17.0-35.0 years), with 40.4% of the patients being female. The median BMI was 25.5 kg/m2 (IQR, 22.7-28.6 kg/m2), and 31.0% had a baseline Marx score ≥12. Of the patients, 26.8% were either football or soccer athletes who were participating in the sport at the time of the injury.
Baseline Patient Characteristics (n = 381) a
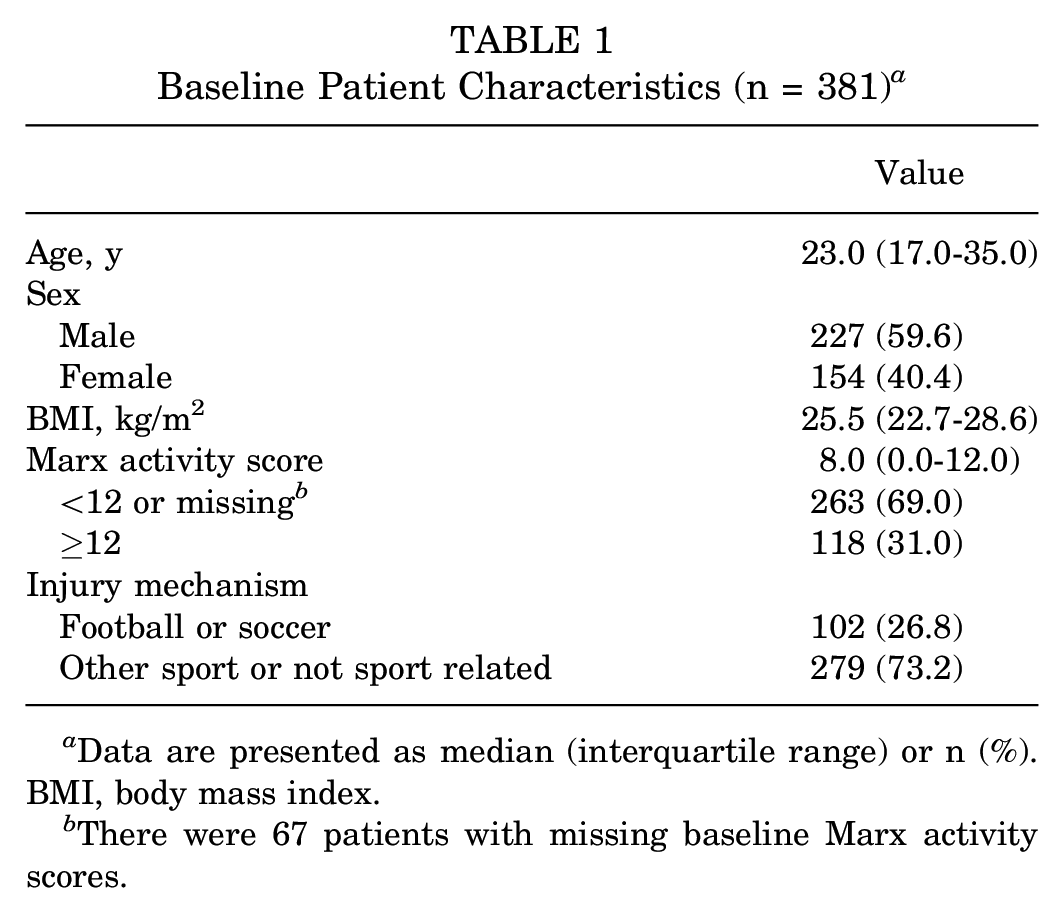
Data are presented as median (interquartile range) or n (%). BMI, body mass index.
There were 67 patients with missing baseline Marx activity scores.
The reamer diameters used for the ACLR tunnels ranged from 7.0 to 11.0 mm, shown in 0.5-mm increments in Figure 2. The median autograft diameter was 8.5 mm (IQR, 8.0-9.0 mm), and the mean diameter was 8.55 ± 0.74 mm (SD 7.81-9.29 mm) (Table 2). There were 35 patients (9.2%) who received an HT autograft with a diameter <8 mm. Surgeons predominantly utilized 4-strand (53.3%) and 5-strand (30.4%) HT autografts, with strand numbers ranging from 2 to 8. Further surgical characteristics and outcomes are demonstrated in Table 2.
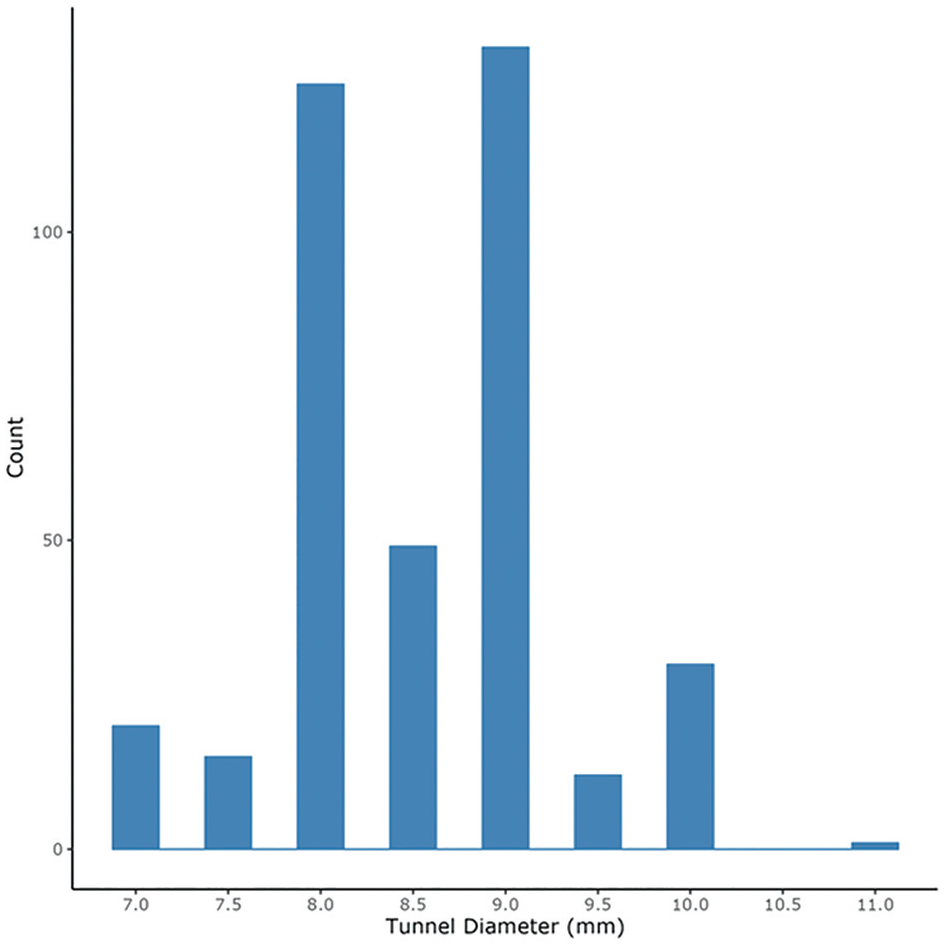
Distribution of anterior cruciate ligament reconstruction tunnel diameters.
Surgical Outcomes (n = 381) a

Data are presented as median (interquartile range) or n (%) unless otherwise indicated. ACLR, anterior cruciate ligament reconstruction.
Data were available from 59 patients.
Data were available from 29 patients.
Incidence of Subsequent Knee Surgery at 2-Year Follow-up
Overall, 59 patients (15.5%) underwent subsequent ipsilateral knee surgery within the 2-year follow-up period, including 27 patients (7.1%) who experienced graft failure and underwent revision ACLR. A total of 29 patients (7.6%) underwent subsequent surgery on the contralateral knee, including 20 patients (5.3%) who underwent contralateral ACLR within 2 years of their index ACLR.
Predictors for Any Subsequent Surgery and Revision ACLR on Ipsilateral Knee
The independent predictive value of each variable examined within the multivariable regression model and its association to the risk of any subsequent ipsilateral knee surgery and revision ACLR is illustrated in Table 3. After adjusting for age, sex, BMI, and baseline Marx score (C-statistic = 0.675), HT autograft diameter was not found to be significantly associated with the risk of any subsequent ipsilateral knee surgery (OR, 0.87 [95% CI, 0.56-1.36]; P = .536). A baseline Marx score ≥12 was significantly associated with an increased risk of any subsequent ipsilateral knee surgery after index ACLR, with the odds between 1.41 and 4.59 times that of a patient with a score <12 (OR, 2.55; P = .002), which corresponds to 155% (95% CI, 41%-369%) higher odds. Age, sex, and BMI were adjusted for the revision ACLR model (C-statistic = 0.726), and HT autograft diameter was not found to be significantly associated with the risk of revision ACLR (OR, 0.71 [95% CI, 0.38-1.33]; P = .286). Lower age was associated with a significantly increased risk of revision ACLR (OR, 0.16 [95% CI, 0.05-0.51]; P = .002), which corresponds to 84% lower odds (95% CI, 49%-95%) of undergoing revision ACLR within 2 years for patients aged 35 years (Q3) compared to patients aged 17 years (Q1). The variable effect on the AIC for any subsequent ipsilateral knee surgery and revision ACLR, ranked by importance, is detailed in Appendix Figures A1 and A2, respectively.
Multivariable Model Results for Ipsilateral Knee a

Boldface P values indicate statistical significance (P < .05). ACLR, anterior cruciate ligament reconstruction; BMI, body mass index; IQR, interquartile range; OR, odds ratio.
Baseline Marx activity score was not incorporated in the model for revision ACLR, given the number of events available and the associated degrees of freedom.
Predictors for Any Subsequent Surgery and ACLR on Contralateral Knee
The independent predictive value of each variable examined within the multivariable regression model and its correlation to any subsequent contralateral knee surgery and subsequent contralateral ACLR is illustrated in Table 4. After adjusting for age, sex, and BMI (C-statistic = 0.584), no variables were significantly associated with the risk of any subsequent contralateral knee surgery, including HT autograft diameter (OR, 0.89 [95% CI, 0.50-1.59]; P = .703). After adjusting for age, sex, and BMI (C-statistic = 0.723), HT autograft diameter was not found to be significantly associated with the risk of subsequent contralateral ACLR (OR, 0.78 [95% CI, 0.39-1.59]; P = .501). Lower age was found to be associated with an increased risk of subsequent contralateral ACLR (OR, 0.30 [95% CI, 0.10-0.93]; P = .037). This corresponded to 70% lower odds (95% CI, 7%-90%) of undergoing contralateral ACLR within 2 years for patients aged 35 years (Q3) compared to patients aged 17 years (Q1). The variable effect on the AIC for any subsequent contralateral knee surgery and subsequent contralateral ACLR, ranked by importance, is detailed in Appendix Figures A3 and A4, respectively.
Multivariable Model Results for Contralateral Knee a

Boldface P values indicate statistical significance (P < .05). ACLR, anterior cruciate ligament reconstruction; BMI, body mass index; IQR, interquartile range; OR, odds ratio.
Nomograms were constructed to illustrate the relative prognostic value of each variable in contributing to the cumulative risk of surgical outcomes (Appendix Figure A5). Theoretical outcome calculation examples using these nomograms are also included in the Appendix.
Discussion
In the current study, multivariable regression modeling revealed that HT autograft diameter was not associated with the risk of either subsequent ipsilateral or contralateral knee surgery, including revision ACLR and subsequent contralateral ACLR. A baseline Marx activity score ≥12 was associated with an increased risk of any subsequent ipsilateral knee surgery, and lower age was associated with an increased risk of revision ACLR and subsequent contralateral ACLR.
Prior studies have found a similar association between age and the risk of revision ACLR,15,18,25,44 and one study 44 found an association between male sex and the risk of revision ACLR. Previous studies15,25 evaluating patient activity levels have found mixed results in the association between baseline activity level and subsequent ACL surgery. MOON Knee Group et al 25 showed no association between baseline activity score and subsequent ACL surgery in a young athletic patient population, while Kaeding et al 15 did show an association between baseline activity level and both revision ACLR and subsequent contralateral ACLR in a more generalized patient cohort.
Multiple recent studies have shown higher rates of graft failure with the use of smaller HT autografts, as summarized in Table 5. Magnussen et al 18 performed a retrospective study on 256 patients undergoing primary ACLR with an HT graft and used multivariable logistic regression modeling to correlate patient age, sex, graft diameter, and length of follow-up with revision ACLR. Age <20 years, decreased graft diameter, and increased follow-up time were associated with an increased risk of revision. Mariscalco et al 19 performed a retrospective study on patients undergoing primary ACLR with an HT graft. The relationship between graft diameter and patient-reported outcome scores at 2-year follow-up was assessed via multivariable linear regression modeling. The relationship between graft diameter and the risk of revision was analyzed via the t test and was determined to be stronger with grafts ≤8 mm compared to larger grafts. Only 64 patients with graft diameters >8 mm were evaluated, and this group had a mean age of 27 versus 21 years for the group with graft diameters ≤8 mm. The lower mean age in the smaller diameter group is a known independent prognostic variable associated with ACLR failure.15,18,26,44 Consequently, that study did not adjust for known confounding variables when determining the association between graft diameter and the risk of revision ACLR.
Literature Review of Hamstring Tendon Autograft Diameter on Outcomes a

Dashes indicate not applicable. ACLR, anterior cruciate ligament reconstruction; BMI, body mass index; HR, hazard ratio; NR, not reported; OR, odds ratio; RR, relative risk.
Data are presented as mean, mean (range), or mean ± SD.
Snaebjörnsson et al 36 performed a retrospective study on 17,096 patients undergoing primary ACLR with an HT graft within a multinational registry using multivariable logistic regression modeling. Their results demonstrated a greater risk of revision ACLR within 2 years when comparing HT autografts <8 mm to those ≥8 mm, and they reported a revision ACLR rate 0.84 times lower for each 1-mm increase in the graft diameter. Snaebjörnsson et al 35 and Spragg et al 38 performed additional studies using a case-control study design and found a similar significant association between HT autograft diameter and surgical failure.
There are several published studies that have demonstrated no significant association between HT autograft diameter and surgical outcomes (Table 5). Rahardja et al 32 conducted a prospective study on 6145 patients undergoing ACLR with an HT autograft in New Zealand and performed multivariate regression modeling. An autograft diameter <8 mm (vs ≥8 mm) was not associated with revision ACLR. The risk of revision ACLR was associated with male sex, young age, decreased time to surgery, and tibial fixation method. The authors concluded that tibial fixation method was more important than graft diameter or number of strands in preventing surgical failure. Krishna et al 16 performed a prospective randomized controlled trial on 62 patients to compare the use of 5- and 4-strand HT autografts in patients undergoing ACLR. The mean graft diameter of the 5-strand group was 8.8 mm compared to 7.9 mm in the 4-strand group (P < .001). Univariate analysis compared graft rupture rates between the groups and found no significant difference. At 2-year follow-up, there was no significant difference in the KT-2000 arthrometer side-to-side difference in anterior laxity (P = .63), Lachman grade (P > .99), and pivot-shift grade (P = .49) when comparing the 5- and 4-strand groups. That study was limited by small patient and event sizes. Wernecke et al 44 performed a retrospective case series on 359 patients undergoing primary ACLR with an HT autograft and used multivariable logistic regression modeling to examine the correlation of graft diameter, age, sex, preinjury Tegner score, and concurrent meniscal injuries to revision ACLR. Autograft diameter was not a significant independent predictor. Male sex and younger age were associated with an increased risk of revision ACLR.
Modifiable variables found to yield an independent predictive value, such as those governed by surgical technique, are targets for optimization to improve surgical outcomes. Autograft diameter is a modifiable surgical variable. Previous studies reporting an association between a greater autograft diameter and improved patient outcomes have motivated various technique modifications to increase the HT autograft diameter during graft preparation in ACLR.4,30,43 Walczak et al 43 performed a prospective paired cohort study evaluating the change in diameter when converting from a 4- to 5-strand HT autograft intraoperatively and found the average increase in diameter to be 0.99 mm. Calvo et al 4 performed a retrospective study on 70 patients undergoing ACLR to analyze the effect of intraoperative conversion to a 5-strand HT autograft when the quadrupled graft was <8 mm. The average graft diameter in the sufficient quadrupled HT graft group was 8.5 mm (range, 8-10 mm); in the insufficient quadrupled HT graft group, the average graft diameter was 7.2 mm (range, 6.5-7.5 mm) and increased to 9.2 mm (range, 8-10 mm) after converting to a 5-strand graft (P = .00596). Comparative analyses of outcomes at 2-year follow-up found no significant difference in patient-reported outcomes or graft rupture rates (P = .55) in the 5-strand group compared to the 4-strand group, despite a significant difference in the diameter. Perkins et al 30 conducted a retrospective cohort study on 354 patients aged 10 to 19 years (mean age, 15.3 years) undergoing ACLR to assess the efficacy of augmenting small HT autografts with an allograft. The grafts augmented with an allograft had a larger average diameter (9.2 mm) than the 4- and 5-strand autografts (8.3 and 8.9 mm, respectively; P < .01). There was a 20% graft rupture rate in HT autografts augmented with an allograft compared to 14% for 4-strand autografts and 12% for 5-strand autografts (P = .51). After adjusting for age and graft diameter, grafts with allograft augmentation had a higher rate of ruptures compared with 4-strand grafts (OR, 2.60 [95% CI, 1.02-6.50]; P value not published).
The discrepancy in the reported association of HT autograft diameter with surgical outcomes in the current literature is likely multifactorial. Retrospective studies that fail to adjust for potential confounding variables are limited in their ability to assign an independent risk to single variables. The prospective study design, 90.5% follow-up rate, and multivariable regression modeling incorporated in this study help to isolate HT autograft diameter as a variable and delineate its role in surgical outcomes after ACLR. Additionally, studies within the existing literature have analyzed ACLR populations receiving smaller HT autografts relative to this study. As detailed in Table 5, studies that have reported a significant association between a smaller diameter and increased surgical failure primarily compared HT autografts with diameters ≤8 mm to those >8 mm. The mean HT autograft diameter in those studies ranged from 7.8 to 8.8 mm. Conversely, the mean diameter in this study was 8.55 mm, and only 35 patients (9.2%) received an autograft <8 mm. There were too few surgical events to enable multivariable modeling exclusive to this range of smaller autografts. Our findings demonstrated no association between HT autograft diameter and surgical outcomes in either knee for autograft diameters ≥8 mm. The present study aligns with existing studies within the literature to suggest that the minimum HT autograft diameter to help mitigate ACLR failure may be 8 mm, with no significant benefit of utilizing an HT autograft with a diameter >8 mm. This finding highlights the need to identify other modifiable surgical variables that can be optimized to improve outcomes for the individual patient.
Limitations
Among the limitations of this study, the relatively small number of revision and subsequent surgery events limited the degrees of freedom within our analysis and restricted the number of variables within the multivariable regression models. A larger sample size with more events would have empowered the analysis to look for additional independent predictive variables, such as sport at the time of the injury and graft fixation method. Revision ACLR was utilized as a surrogate for graft failure; in addition, more sensitive indicators of failure, including repeat knee injury events and knee laxity, were not routinely collected at final follow-up. There is likely to be a group of unrecognized patients in whom ACLR was unsuccessful but who did not pursue or desire revision surgery, thereby limiting the number of failure events available for analysis. As previously discussed, autograft diameters <8 mm were underrepresented in this study and may be associated with inferior outcomes. There were 10 surgeons who contributed ACLR cases, and the inherent variability in operative technique including graft harvesting, graft preparation, tunnel drilling, and graft fixation make these confounding variables for study outcomes. Tunnel diameter was used as a surrogate for graft diameter, and although each surgeon attempted to optimize graft fit within the tunnel, there was surgeon-derived variability in the technique for drilling the tunnel size relative to the measured autograft diameter. The study cohort included a relatively broad spectrum of patients, including age (median, 23.0 years; range, 13-66 years) and baseline Marx activity score, potentially limiting the application of these findings to more select patient groups such as a young athletic population, which is known to have a higher risk of ACLR-related complications.14,15,18,20,25
Conclusion
This study investigated the association between HT autograft diameter and surgical outcomes after primary ACLR. Multivariable analysis demonstrated that a minimum HT autograft diameter of 8 mm was not associated with the risk of revision ACLR or other subsequent surgery in the ipsilateral or contralateral knee. Lower age was associated with an increased risk of revision ACLR and subsequent contralateral ACLR. A baseline Marx activity score ≥12 was associated with an increased risk of all subsequent ipsilateral knee surgery. This study may guide intraoperative decision making regarding HT autograft implementation in ACLR.
Footnotes
Appendix
Acknowledgements
The authors thank Elizabeth Sosic, BS, who was fundamental in the organization and submission of this article for publication; the following surgeons who contributed cases: Thomas E. Anderson, MD, Robert J. Hampton, DO, and Alfred Serna, MD; and finally, Gregory J. Strnad, MS, for helping to create and maintain the institutional electronic data capture system.
Final revision submitted August 14, 2024; accepted September 4, 2024.
Presented at the AOSSM Annual Meeting, Washington, DC, July 13-16, 2023.
One or more of the authors has declared the following potential conflict of interest or source of funding: P.M.S. has received education payments from Rock Medical Orthopedics, consulting fees and nonconsulting fees from Arthrex, and honoraria from NovoPedics. J.T.R. has received nonconsulting fees from Smith & Nephew. M.H.J. has received consulting fees from Regeneron Pharmaceuticals and hospitality payments from DJO. A.M. has received education payments from Arthrex; has received consulting fees from Anika Therapeutics, Arthrosurface, Amniox Medical, and Trice Medical; has received nonconsulting fees from Arthrosurface; has received royalties from Anika Therapeutics, Arthrosurface, and Zimmer Biomet; has received honoraria from Arthrosurface; and has stock/stock options in Anika Therapeutics. B.M.L. has received education payments from Southern Edge Orthopaedics and consulting fees from Zimmer Biomet. K.P.S. has received education payments from Summit Surgical, consulting fees from NovoPedics and Flexion Therapeutics, and honoraria from NovoPedics. AOSSM checks author disclosures against the Open Payments Database (OPD). AOSSM has not conducted an independent investigation on the OPD and disclaims any liability or responsibility relating thereto.
Ethical approval for this study was obtained from Cleveland Clinic (reference No. 06-196).
