Abstract
Objectives:
Patellofemoral (PF) knee pain affects 20-30% of the general population. There is growing evidence that chronic PF pain is associated with the development of osteoarthritis (OA). Among the many biomechanical factors contributing to PF pain and pathology, flat-footedness and ankle eversion may be accessible targets for therapeutic interventions. These factors influence the patellofemoral joint by coupling with the tibia, where subtalar joint pronation causes internal tibial rotation, pulling the patellar tendon medially to alter alignment and tracking of the patella. Subtle degenerative changes in cartilage can be detected with MRI compositional measures such as T2 and T1ρ. In patellar lateral facets of patients with PF pain but no evidence of OA, elevated cartilage T1ρ has previously been reported. The goal of this study is to investigate the relationships between PF joint cartilage composition and biomechanical foot and ankle measures thought to impact PF health. This study tests the hypotheses that more medial foot center of pressure (COP), greater ankle eversion, and greater internal tibial rotation associate with greater patellar or trochlear cartilage T2 values.
Methods:
Participants provided written consent to participate in this IRB-approved study. The study cohort consisted of 23 participants with knee MRI, lower limb radiographs and gait assessments acquired 2 years after unilateral ACL reconstruction (ACLR), Table 1. MRI, x-ray, COP and gait data from only the uninjured limbs of the study cohort were assessed. PF cartilage in these participants was grossly intact on morphological MRI. A 10-camera optoelectronic system (Qualisys) and force plate (Bertec) were used to measure participants’ motion. Average ankle eversion over stance (°) and external tibial rotation (°) were calculated from 3 walking trials at normal self-selected speed. Foot center of pressure (COP, cm) relative to the midfoot axis was measured from the force plate. Frontal-plane mechanical axis was determined from full-length standing-alignment radiographs of the lower limbs. Knee MRIs were acquired on a 3T scanner (GE, Healthcare). T2 maps were generated from a quantitative double-echo in steady state (qDESS) MRI sequence (TR/TEs 21 ms/6, 36 ms; 0.417 x 0.417 mm resolution; 1.5 mm slice thickness). T2 values in full-thickness articular cartilage were determined in 2 “tread mark” regions on patellar and trochlear surfaces (largely consistent with known regions of cartilage contact during common daily activities), by manually segmenting 7 contiguous central qDESS slices (10.5 mm wide right to left) with custom software (MATLAB, TheMathWorks), Figure 1.
Results:
Conclusions:
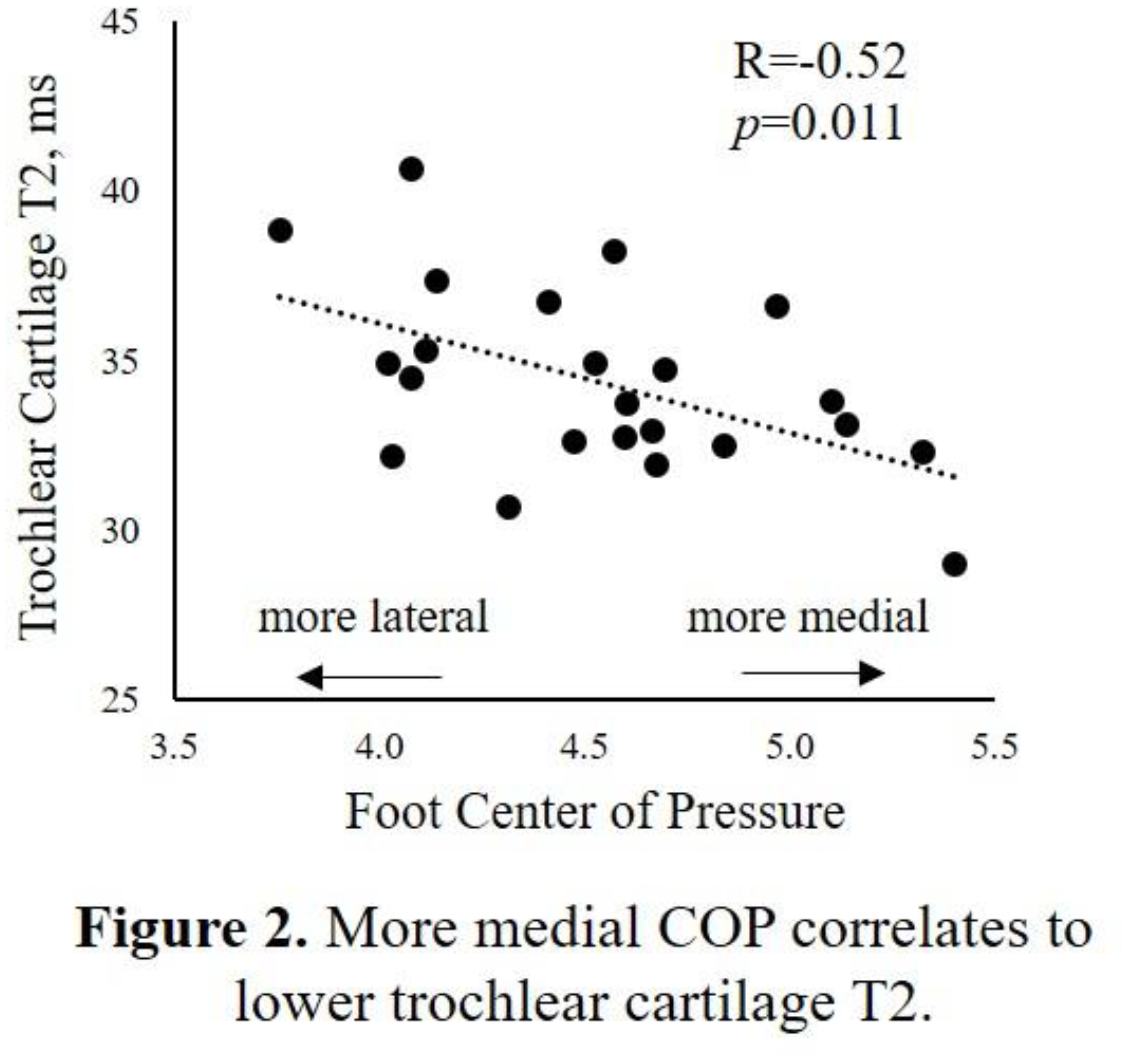
The results of this study suggest that in knees without clinical evidence of osteoarthritis, biomechanical measures of the ipsilateral foot and ankle are related to patellofemoral cartilage composition. Specifically, more medial COP and greater ankle eversion showed a correlation and trends, respectively, for lower cartilage MRI T2. While the directions of these associations are opposite to our hypothesis, they are in-line with previous studies showing T2 decreases with early subsurface compositional degeneration in morphologically surface-intact cartilage. These results are also in general agreement with studies that found excessive external tibial rotation correlated to greater patellar cartilage UTE-T2* and more laterally directed foot pressure during walking associated with anterior knee pain. In other prior work, although medial patellar cartilage damage diagnosed from morphologic MRI was detected in nearly 60% of older adults, no association was found between planus foot morphology and PF cartilage damage. By contrast, relationships between PF cartilage and foot and ankle biomechanics measured here may reflect a greater sensitivity of compositional T2 mapping compared to morphologic MR imaging to subtle and early structural changes within cartilage. In conclusion, though many biomechanical factors contribute to PF pain, foot and ankle alignment may also deserve consideration during screening and assessment for possible intervention. Correlation of foot COP to cartilage composition at the knee raises the intriguing possibility that strategies involving gait retraining or shoe interventions to alter weight distribution at the foot and ankle could be utilized to benefit to knee cartilage health to prevent or delay osteoarthritis.