Abstract
Objectives:
Patients with a symptomatic meniscal tear commonly present with pain with activities, locking, catching, swelling and often they will report pain at night. Arthroscopic partial meniscectomy (APM) is commonly performed for these symptomatic meniscus tears that fail conservative management. Pain at night has been studied in patients with knee Osteoarthritis (OA) and research has demonstrated resolution of sleep disturbance after Total Knee Arthroplasty (TKA). While several studies have investigated the impact of TKA on pre-operative sleep disturbance, little research has been performed on sleep disturbance in patients with symptomatic meniscal tears and outcomes following APM.
The purpose of the present study was to assess patients with and without pre-operative pain at night who underwent APM. Second, we sought to assess post-operative resolution of night pain and associated patient reported outcome measures.
Methods:
Patients undergoing primary APM with or without chondroplasty were prospectively enrolled in a registry database. Patients undergoing other concomitant procedures, such as ligament reconstruction, were excluded. Patient demographics and validated patient reported outcome measures were obtained pre- and post-operatively including the visual analog pain scale (VAS), Knee Injury and Osteoarthritis Outcome Score (KOOS), Marx Scale, Veterans RAND 12-Item Health Survey (VR-12) physical and mental components. Knee cartilage was also assessed arthroscopically and described using the Outerbridge Classification. Pain at night was defined as reporting greater than mild pain on the KOOS question “What amount of knee pain have you experienced at night while in bed”.
Results:
Five hundred and eight-seven patients met inclusion criteria. Mean age at time of surgery was 50.7 years ± 9.5 years with a median duration of symptoms of 4.0 months (IQR 2.0mo – 9.0mo). Three hundred and twenty-three (55.9%) patients were female, and average patient BMI was 30.2 kg/m2 ± 6. kg/m2.
Two hundred and ninety-nine (50.9%) patients reported preoperative pain at night. These patients were older, more likely to be female, and more likely to be smokers compared to those not reporting pain at night. There was no significant difference in Outerbridge Grade between patients with and without pre-operative pain at night.
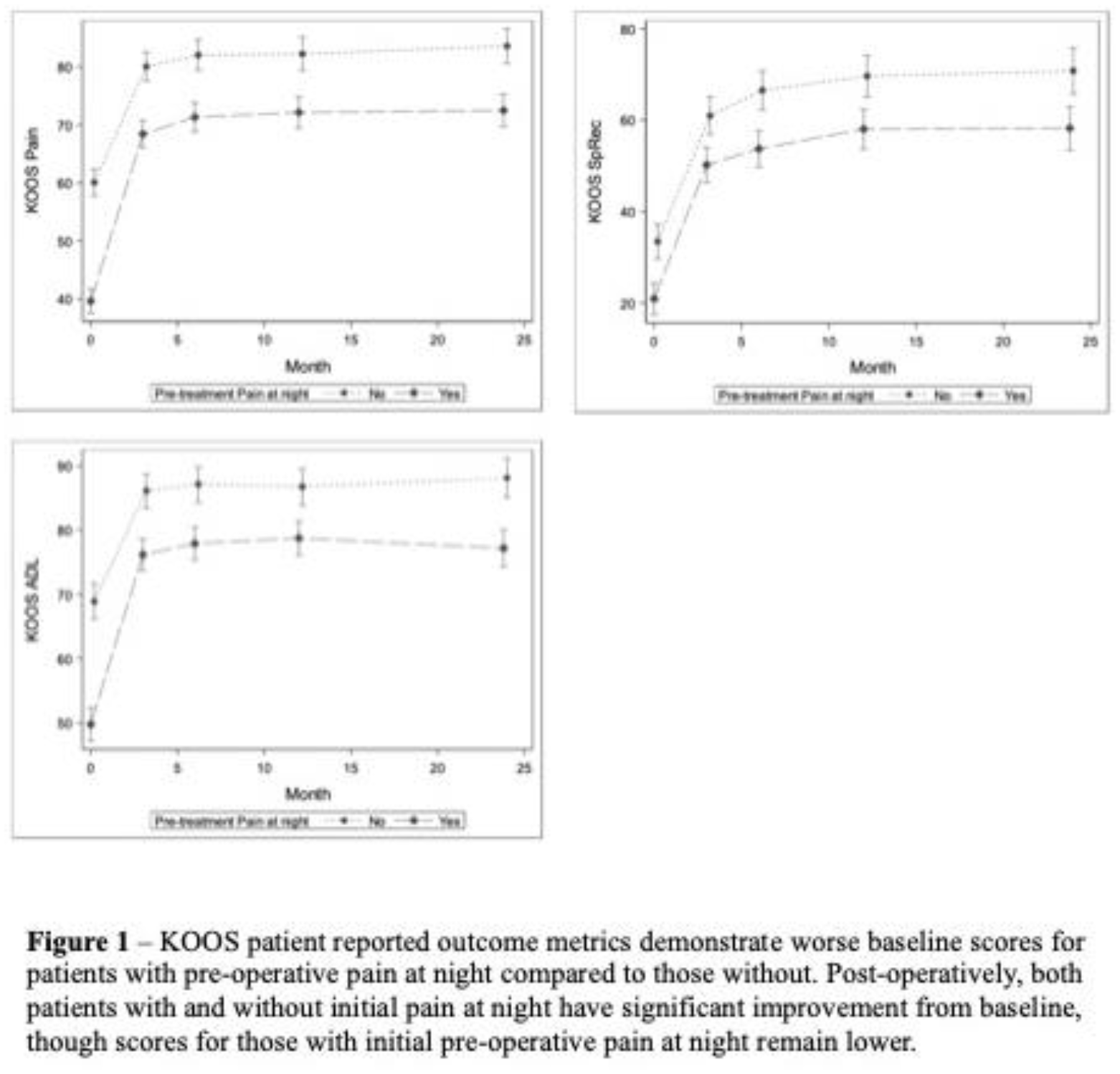
Postoperatively, pain at night resolved by 3 months in 79.9% (219) and in 91.6% (274) patients by 2 years. Patients whose pain at night persisted were more likely to have had a longer duration of symptoms pre-operatively, and also tended to have higher BMIs though this did not reach statistical significance. There was no significant difference in Outerbridge Grade between the cohort of patients whose pain at night resolved and those whose symptoms persisted. PROMs significantly improved postoperatively both for patients who had initial sleep disturbance and those who did not, with patients with initial sleep disturbance experiencing greater improvement from baseline though still with significantly worse scores at all follow-up time points compared to those with no baseline sleep symptoms preoperatively.
Conclusions:
Over half of patients undergoing arthroscopic partial meniscectomy report preoperative pain at night. These patients have significantly worse baseline functional scores compared to patients without night pain. Postoperatively, over 90% of patients with initial pain at night note resolution of symptoms, with nearly 80% improved by 3 months. Functional scores significantly improve after surgery for both patients with and without initial pain at night, though they remain lower in patients who had pain at night prior to surgery.