Abstract
Objectives:
To assess minimum 1-year magnetic resonance imaging (MRI) and clinical outcomes for 20 cases of dermal allograft augmentation of subcritical glenoid bony defects.
Methods:
Twenty patients with subcritical glenoid bone loss underwent arthroscopic dermal allograft augmentation along with labral repair. All patients were evaluated with postoperative MRI at a minimum of 12-month follow-up. Preoperative and postoperative patient-reported outcomes were collected including University of California Los Angeles Shoulder (UCLA) scores, Visual Analogue Scale (VAS) scores, and American Shoulder and Elbow Surgeons (ASES) scores. Scores were assessed for statistical significance using the analysis of variance test.
Results:
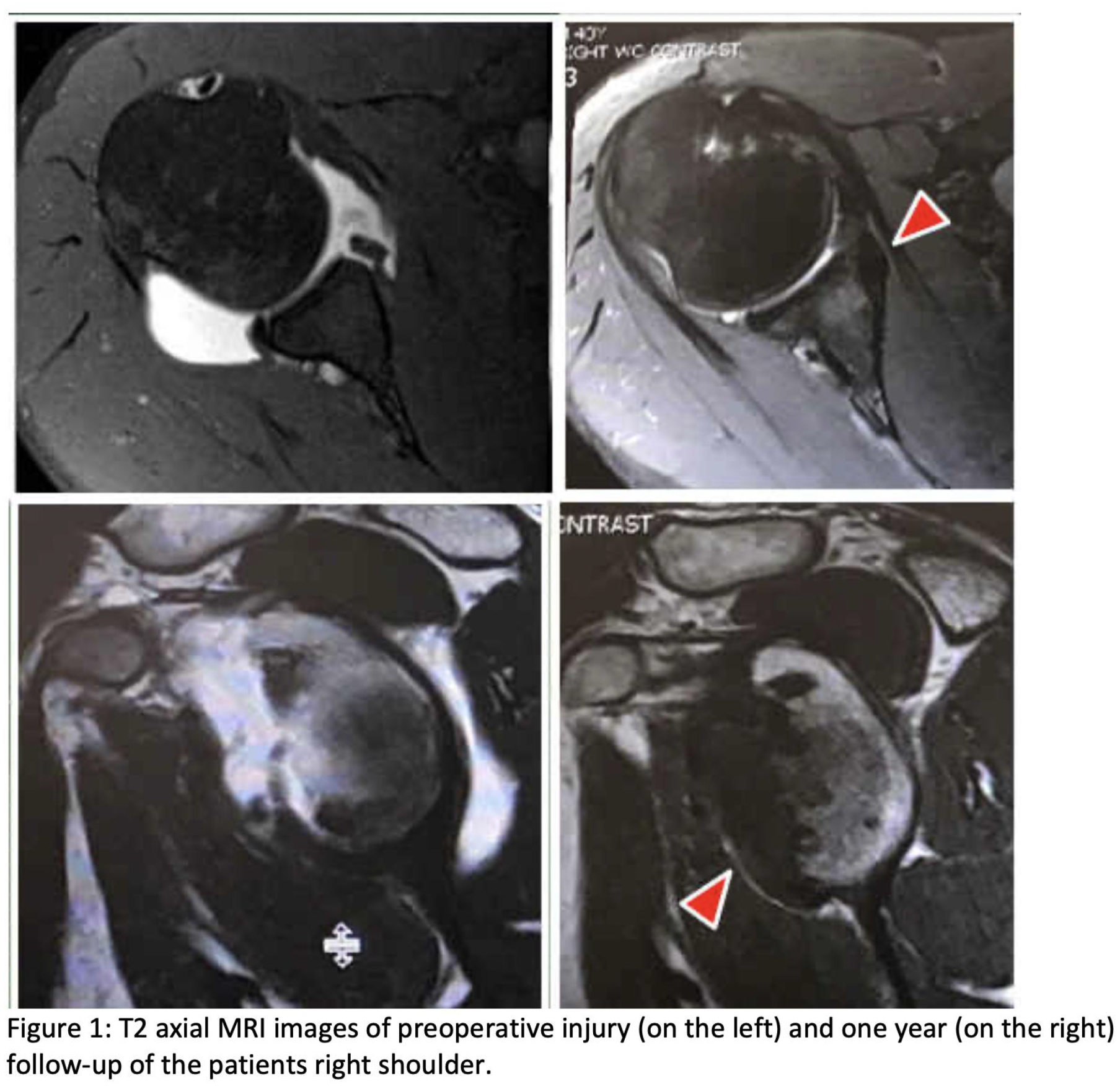
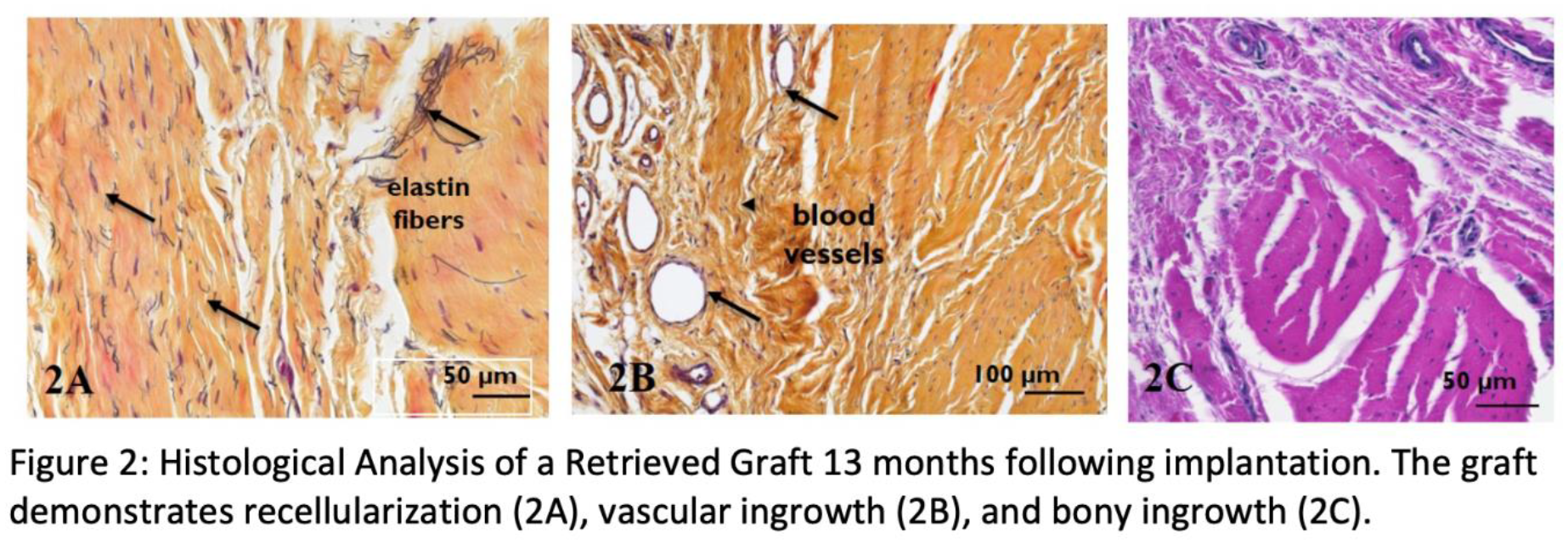
Average postoperative follow-up was 19 months (range 12-54 months). The average preoperative bony defect size was 16% (range 6.6-39%), with 19 of the patients having defects under 20%. Postoperative MRIs (Figure 1) revealed an average of 32% (range 27.7-37.4%) increase in glenoid diameter size and the average glenoid size was restored to 102.3% (range 94-114%), with excellent incorporation of the graft. There were statistically significant improvements in preoperative and postoperative scores with respect to UCLA scores (21.25 to 33.7, p < 0.05), VAS scores (5.4 to 0.2, p < 0.05) and ASES scores (58.6 to 96.4, p < 0.05). One patient had a recurrent traumatic dislocation (5%) and underwent a Latarjet procedure at 13 months from the index surgery. At the time of the Latarjet, the dermal allograft was harvested and sent for histologic analysis. Histologic analysis of the glenoid augmentation graft at the time of revision surgery revealed recellularization with fibroblast-like cells, revascularization, and incorporation of the graft into the surrounding tissue with bony ingrowth. (Figure 2)
Conclusions:
Subcritical glenoid bone loss has been associated with high failure rates when treated with standard labral repair. While a Latarjet procedure can provide stability, high complication rates and the risk of long-term arthritis makes this procedure less than ideal when bone loss is under 20%. Arthroscopic labrum repair with the addition of a dermal allograft is a viable option in patients with subcritical bone loss. In the case series with 1-year follow-up, 20 patients who underwent arthroscopic labrum repair with the addition of a dermal allograft had a significant improvement in outcome scores, and excellent incorporation of the graft as seen on MRI at 12 months from the index procedure. In the 1 failure that later underwent revision surgery, histologic analysis demonstrated recellularization and revascularization, with incorporation of the graft.