Abstract
Background:
While posterior medial meniscus root (PMMR) techniques have evolved, there remains a need to both optimize repair strength and improve resistance to cyclic loading.
Hypothesis:
Adjustable tensioning would lead to higher initial repair strength and reduce displacement with cyclic loading compared with previously described transtibial pull-out repair (TPOR) fixation techniques.
Study Design:
Controlled laboratory study.
Methods:
A total of 56 porcine medial menisci were used. Eight intact specimens served as a control for the native meniscus. For the others, PMMR tears were created and repaired with 6 different TPOR techniques (8 in each group). Fixed PMMR repairs were executed using 4 different suture techniques (two No. 2 cinch sutures, two cinch tapes, two No. 2 simple sutures, and two No. 2 sutures in a Mason-Allen configuration) all tied over a cortical button. Adjustable PMMR repairs using Mason-Allen sutures were fixed with an adjustable soft tissue anchor fixation tensioned at either 80 N or 120 N. The initial force, stiffness, and relief displacement of the repairs were measured after fixation. Repair constructs were then cyclically loaded, with cyclic displacement and stiffness measured after 1000 cycles. Finally, the specimens were pulled to failure.
Results:
The PMMR repaired with the 2 cinch sutures fixed technique afforded the lowest (P < .001) initial repair load, stiffness, and relief displacement. The adjustable PMMR repairs achieved a higher initial repair load (P < .001) and relief displacement (P < .001) than all fixed repairs. The 2 cinch sutures fixed technique showed an overall higher cyclic displacement (P < .028) and was completely loose compared with the native meniscus functional zone. Repairs with adjustable intratunnel fixation showed displacement with cyclic loading similar to the native meniscus. With cyclic loading, the Mason-Allen adjustable repair with 120 N of tension showed less displacement (P < .016) than all fixed repairs and a stiffness comparable to the fixed Mason-Allen repair. The fixed Mason-Allen technique demonstrated a higher ultimate load (P < .007) than the adjustable Mason-Allen techniques. All repairs were less stiff, with lower ultimate failure loads, than the native meniscus root attachment (P < .0001).
Conclusion:
Adjustable TPOR led to considerably higher initial repair load and relief displacement than other conventional fixed repairs and restricted cyclic displacement to match the native meniscus function. However, the ultimate failure load of the adjustable devices was lower than that of a Mason-Allen construct tied over a cortical button. All repair techniques had a significantly lower load to failure than the native meniscus root.
Clinical Relevance:
Knotless adjustable PMMR repair based on soft anchor fixation results in higher tissue compression and less displacement, but the overall clinical significance on healing rates remains unclear.
The primary role of the meniscus is to optimize the tibiofemoral load distribution over a greater contact area and congruence by reducing the contact stress on the articular surfaces.24,31 The conversion of compressive joint loads into meniscal hoop stresses explains the variable effect and frequency of meniscal tears. A tear of the posterior medial meniscus root (PMMR) has been shown to negatively affect knee joint function and biomechanics by decreasing the tibiofemoral contact area and increasing the peak contact pressure, similar to a total meniscectomy.2,13,18,28 In clinical studies, PMMR tears were associated with increased pain, meniscal extrusion, chondral lesions, osteonecrosis, and osteoarthritic progression.17,20,36 There is a wide consensus on meniscal preservation using the transtibial pull-out repair (TPOR) as the method of choice to preserve meniscal tissue and restore biomechanical function to prevent early-onset degenerative changes.2,9,12,22
The biomechanical performance of multiple PMMR repair techniques using tibial suture button and suture anchor fixation has been described.14,15,17,25,26,33 Previously, the meniscus-suture interface has been identified as the weakest interface. 10 The 2 simple sutures technique has demonstrated the lowest displacement during cyclic loading, and the modified Mason-Allen provides the highest load to failure.14,26 Direct suture anchor placement into the root footprint as another method for PMMR repair has demonstrated reduced cyclic displacement and increased stiffness when compared with TPOR. 15 However, there are hardly any data on the primary fixation of TPOR and direct suture anchor fixation at the time of surgery. The overall stability of PMMR repair is weaker than the native root attachment.15,23
Apart from the biological healing environment and patient selection, it can be assumed that a PMMR repair with greater primary fixation strength at the time of meniscal reapproximation and greater resistance to cyclic displacement during repetitive hoop-stress loading may improve the success of meniscus root healing.30,36 A recently developed TPOR device offers a knotless adjustable mechanism based on the modified Mason-Allen suture repair with intratunnel soft anchor fixation beneath the tibial plateau. There have been no studies evaluating the biomechanical performance of knotless adjustable TPORs in comparison with suture repair techniques with tibial knot tying over a suture button or suture anchor fixation.
The purpose of this study was to evaluate and compare the initial repair load and relief displacement directly after fixation of various conventional fixed techniques with knotless adjustable TPOR in a biomechanical full-construct porcine model. Additionally, the cyclic displacement and stiffness during repetitive loading as well as the ultimate load during failure testing of all repairs were compared with each other. It was hypothesized that adjustable tensioning for primary PMMR fixation would lead to a higher initial repair load and relief displacement as well as to greater resistance against displacement during cyclic loading when compared with previously described conventional techniques.
Methods
A total of 56 freshly sacrificed porcine tibias and medial menisci without any obvious macroscopic degenerative changes were obtained from a local slaughterhouse. Porcine tissue has previously been reported to have morphometric and mechanical similarities to young adult human tissue1,35 and is commonly used to evaluate meniscal repair techniques.10,14,15,19,32 All muscles and soft tissue of the porcine tibias, which were aged between 27 and 35 weeks, were removed with the bone cut axially 14 cm below the joint line.
The porcine specimens were randomly assigned to 1 of 6 groups for primary fixation and cyclic testing of various TPOR techniques of PMMR tears or a reference native meniscus group (Figure 1).

(A-D) Various fixed groups and (E) the adjustable suture repair groups (2 groups), with testing algorithm and outcome variables. A, anchor fixation; MA, Mason-Allen; TCL, 2 cinch loops; TCS, 2 cinch sutures; TS, 2 sutures.
For the native group, the medial menisci were released from the tibia by dissecting the meniscocapsular tissue and the anterior meniscotibial ligament, leaving only the posterior meniscus root intact. For the repair groups, the menisci were completely detached from the tibial plateau by cutting the posterior meniscotibial ligament at 5 mm lateral to the margin of the posterior horn as well. An oscillating saw was used to cut 1 cm medial to the PMMR insertion, perpendicular to the medial tibial plateau, to allow sufficient space for clamping of the meniscus. 15 For all repair groups, a drill guide and a 2.4-mm drill were used to create a transtibial tunnel from the anterolateral cortex to the PMMR footprint.
The tibia was embedded in a custom-made aluminum cylinder using RenCast (Huntsman Advanced Materials), a bicomponent embedding material. The tibias were positioned in line with their long axis and embedded 3 cm distal to the predetermined exit of the tibial tunnel axis to allow sufficient space for knot tying of the transtibial pull-out suture repair. All tissue was fresh frozen at −20°C after harvesting. The porcine bones were thawed at room temperature overnight, and the menisci were thawed in a saline solution 2 hours before biomechanical testing. All specimens were kept moist with physiological saline solution during specimen preparation and testing.
Repair Techniques
Four different fixed suture repair configurations (Figure 1, A-D), as described previously, 14 and 2 adjustable repair configurations using the Mason-Allen suture technique (Figure 1E) with intra-tunnel soft anchor fixation (SutureLoc; Arthrex) were prepared for biomechanical testing.
The double-loaded adjustable implant consisted of two No. 2 nonabsorbable repair sutures with corresponding shuttle sutures and a soft anchor with an anchor-deploying suture loop (Figure 2A). Because no restriction of the primary tension is considered for the adjustable technique, 2 separate test groups with 80 N (MA-80) and 120 N (MA-120) of tension applied on each loop-shortening strand were prepared. The fixed repair techniques selected in this study should cover the whole stabilization spectrum of PMMR repair, with the reported lowest cyclic displacement for the 2 simple sutures technique and the highest displacement for the cinch loop–based meniscus root refixation groups during cyclic loading.14,26 The fixed modified Mason-Allen group served as a reference group for adjustable groups, although the suture constructs with the fixation method were different. A suture passer (Knee Scorpion; Arthrex) was utilized for suture shuttling through the meniscus to replicate the arthroscopic surgical condition. The locations for suture passing through the meniscus were defined as 5 mm medial to the lateral edge of the posterior meniscus horn with 1 suture positioned next to the meniscosynovial junction. In contrast, the other suture was positioned 5 mm more anteriorly. 14 The first author (S.B.) performed all meniscus-suture configuration techniques.

(A) The adjustable implant with (B-I) stepwise surgical preparation of the adjustable Mason-Allen root repair (shown with intact medial tibial plateau).
Two Cinch Sutures
Two separately folded No. 2 nonabsorbable braided sutures (FiberWire; Arthrex) were stitched through the meniscus with the 2 free suture ends shuttled through each suture loop, creating a cinch loop at the superior surface of the meniscus by pulling the free ends (Figure 1A).
Two Cinch Loops
Two separate nonabsorbable braided suture tapes (FiberLink SutureTape, 1.3 mm; Arthrex) with a suture tape loop were stitched through the meniscus, with each free suture end passed through the loop portion, creating a cinch loop at the superior surface of the meniscus by pulling the free suture end (Figure 1B).
Two Sutures
Two separate No. 2 nonabsorbable braided sutures (FiberWire) were stitched through the meniscus (Figure 1C).
Mason-Allen Suture
A first No. 2 nonabsorbable braided suture (FiberWire) was passed twice through the meniscus in a horizontal mattress pattern, with the created loop portion on the superior surface of the meniscus. A second separate No. 2 nonabsorbable braided suture (FiberWire) was stitched through the meniscus immediately medial to and in the center of the horizontal suture loop (Figure 1D).
Adjustable Mason-Allen (MA-80/MA-120)
After tunnel preparation (Figure 2B), the adjustable implant was transtibial passed from proximal to distal with the soft anchor pulled into the tunnel (Figure 2C) and positioned directly underneath the proximal cortex (Figure 2D). The soft anchor was placed by pulling on the tibial anchor-deploying suture loop at 150 N using a digital force gauge (Mark-10 M7-50; Bronx-Systems) with slight initial manual countertension of the distal repair sutures (Figure 2E). When tension is applied, the initial elongated anchor sheath becomes shorter and thicker within the tibial tunnel beneath the tibial plateau, locking it for meniscus root fixation. A horizontal suture configuration was created with a first No. 2 nonabsorbable braided repair suture, and a second repair suture was stitched through the meniscus immediately medial to and in the center of the horizontal suture loop using the suture passer (Figure 2F). The end of the first repair suture was passed through the loop of the corresponding shuttle suture and transferred by pulling the tail of the shuttle suture through the integrated “Chinese finger” locking mechanism positioned within the anchor and tibial tunnel (Figure 2G). The second repair suture was transtibial shuttled like the first repair suture (Figure 2H), with the repair suture tension adjusted to reattach the meniscus root (Figure 2I).
Primary Fixation
The embedded tibia and a slotted aluminum metal plate (5 mm in thickness) with a central hole (2.4 mm in diameter) were rigidly secured over a bottom and a top mount to the baseplate and test machine actuator (ElectroPuls E10000; Instron), respectively (Figure 3A).

Biomechanical setup for (A) primary fixation of the transtibial pull-out meniscus root repair in line with the actuator axis and for (B) cyclic testing with load applied in alignment with the circumferential fibers of the meniscus.
The metal plate was secured by screw side-action grips (Instron) equipped with serrated grip jaw faces for a maximum loading capacity of 2 kN. The meniscus was placed onto the metal plate with the repair sutures fed through the central hole, which was aligned with the transtibial tunnel and the actuator axis. A small distance (8 mm) between the bony surface and the metal undersurface allowed for measuring the initial load on the repair and the relief displacement by impingement-free translation of the actuator to a relative repair unloading position of 2 N after fixation. 5 Before final fixation, the sutures were pretensioned with a manual 50-N pull over 5 seconds measured via the test machine's dynamic load cell (1 kN; Instron), and the repair sutures of the fixed groups were threaded through the tibial tunnel and the holes of the tibial button (TightRope Button; Arthrex). Preconditioning of the suture-meniscus interface ensured proper fixation conditions for comparative analysis of the initial tension and simultaneously reduced settling effects before cyclic testing.
The 2 cinch loops were secured by manual knot tying of a single suture couple with 4 alternating counteractive half-hitch knots over the button. All other fixed constructs (2 cinch sutures, 2 sutures, and Mason-Allen suture) required knot tying of 2 suture couples for final fixation. For the adjustable implant, 2 separate test groups with 80 N (MA-80) and 120 N (MA-120) of tension applied on each loop-shortening strand were prepared using a digital force gauge (Mark-10 M7-50; Bronx-Systems). The horizontal suture in the modified Masen-Allen configuration was tensioned first, with all adjustable sutures secured by the integrated Chinese finger locking mechanism within the anchor and finally kept knotless.
After fixation, the initial load quantified the amount of tissue compression exerted by the suture repair. The actuator movement from the initial fixation state toward repair unloading until reaching a residual load of 2 N corresponds to the relief displacement. A greater relief displacement of a device is equivalent to a higher degree of repair security at the time of fixation. The initial stiffness represents the linear inclination between the initial load position and the loading point with 5 N of tension on the repair during construct unloading. A lower load threshold of 5 N (instead of 2 N) reduced the viscoelastic influence within the initial construct behavior for the stiffness calculation. All tests were performed at room temperature, and soft tissue was kept moist with physiological saline solution during preparation and testing.
Cyclic and Failure Testing
The same knotless adjustable repair implant and meniscus of the primary fixation were used for cyclic testing. The knotted sutures of the fixed repair groups were cut after primary fixation testing and replaced by new sutures threaded through the same meniscal punctures with a needle. The suture exchange of the fixed repair samples was required for PMMR fixation in the dynamic test setup by knot tying of the new meniscal repair suture over the tibial-sided button. The use of the same meniscus throughout testing for adjustable and fixed repair constructs ensured more similar and reproducible testing conditions. For cyclic testing, the meniscus root was reapproximated toward the tibial bone and fixed by suture knot tying over the button or adjustable suture tensioning using the digital force gauge. The tibia was aligned in a way to clamp the peripheral section of the medial meniscus 1 cm lateral to the repair sutures (repair groups) or tibial insertion of the root ligament (native group), respectively, to allow tensile loading in line with the circumferential fibers of the PMMR (Figure 3B). The meniscus root repair was secured during clamping with the screw side-action grips from higher tensile loads by the specimen-protect function of the test machine, which autonomously moved the actuator to keep a constant tensile load of 2 N on the repair.
After specimen precycling between 2 and 10 N for 10 cycles at 0.5 Hz, cyclic loading was applied at a test frequency of 0.5 Hz over 1000 cycles between 5 and 30 N. The test parameters used align with numerous other studies evaluating the biomechanical performance of meniscal repair systems using tensile forces experienced during early postoperative rehabilitation.6-8,11,29,34 Final load-to-failure testing was performed at a rate of 0.5 mm/s. Native specimens were immediately pulled to failure after precycling to provide information about the failure strength and the time-zero native meniscus behavior for quantifying and qualifying the stabilization potential of various PMMR repairs. The load-displacement progressions of all native specimens were merged to represent the native meniscus behavior. The native stiffness was determined within the linear portion of the load-elongation curve within the load range of 200 to 450 N.
Load-displacement data during cyclic loading and pull to failure were recorded continuously using WaveMatrix software (Instron) with a sampling rate of 750 Hz. Metrics for comparison data included cyclic displacement and stiffness after 1000 cycles and ultimate failure load, with the mode of failure noted. Cyclic displacement represents plastic deformation (laxity) during force-controlled loading and is a relative valley measurement in relation to the test machine actuator position after precycling. Cyclic stiffness represents the linear inclination of the hysteresis valley and peak data.
Statistical Analysis
In this study, the different suture repair techniques and devices were the independent variables. All metrics for comparison were the dependent variables. Initial repair tension with relief displacement, cyclic displacement, and stiffness after 1000 load cycles as well as ultimate failure load were defined as the primary outcome variables. A sample size of 8 was selected based on previous studies comparing the biomechanical performance of various PMMR repair techniques.15,26
Statistical analysis was performed using Sigma Plot Statistics for Windows Version 13.0 (Systat Software). The statistical analysis included a 1-way analysis of variance (ANOVA) with a Holm-Sidak post hoc test performed for a significant pairwise analysis of primary outcome variables. Significance was defined as P≤ .05, and the desired power level was set at 0.8. The Shapiro-Wilk test was used to confirm that each data set followed a normal distribution. A nonparametric test (Kruskal-Wallis) was used for data sets that failed this test. For Kruskal-Wallis tests that found significance, a post hoc test according to the Dunn method was conducted to further analyze the differences. The observed post hoc mean power values of all 1-way ANOVA tests were much higher than the desired power level of 0.8, leading us to conclude that our sample size was sufficient. Data analysis was performed with MATLAB Version R2019a (MathWorks).
Results
The mean and standard deviation results across all primary fixation and dynamic testing variables with statistical analysis of construct stiffness are shown in Table 1 for repair groups.
Primary Outcome Parameter With Statistical Analysis for Construct Stiffness a

Data are shown as mean ± SD. Significant differences with P values of other parameters are shown in Figures 4 and 5. A, anchor fixation; HS, horizontal suture; MA, Mason-Allen; MA-80, 80 N was applied during fixation; MA-120, 120 N was applied during fixation; TCL, 2 cinch loops; TCS, 2 cinch sutures; TS, 2 sutures.
Significant difference compared with TCS, MA, TS, MA-80, and MA-120 (P≤ .001).
Significant difference compared with MA (P≤ .041).
Significant difference compared with MA, TS, and TCS (P≤ .004).
Significant difference compared with TCL, TCS, TS, and MA-80 (P≤ .013).
Significant difference compared with TCL, MA, MA-80, and MA-120 (P≤ .004).
Primary Fixation
Overall, the PMMR repair with only 2 sutures for knot tying (2 cinch loops technique) demonstrated the lowest (P < .001) initial repair load, relief displacement (Figure 4), and initial stiffness (Table 1). The adjustable PMMR repair showed higher initial repair load (P < .001) and relief displacement (P < .027) compared with all other fixed repairs, with greater significance for the higher-tension group (120 N). The adjustable fixation groups showed higher stiffness compared with the Mason-Allen suture group.
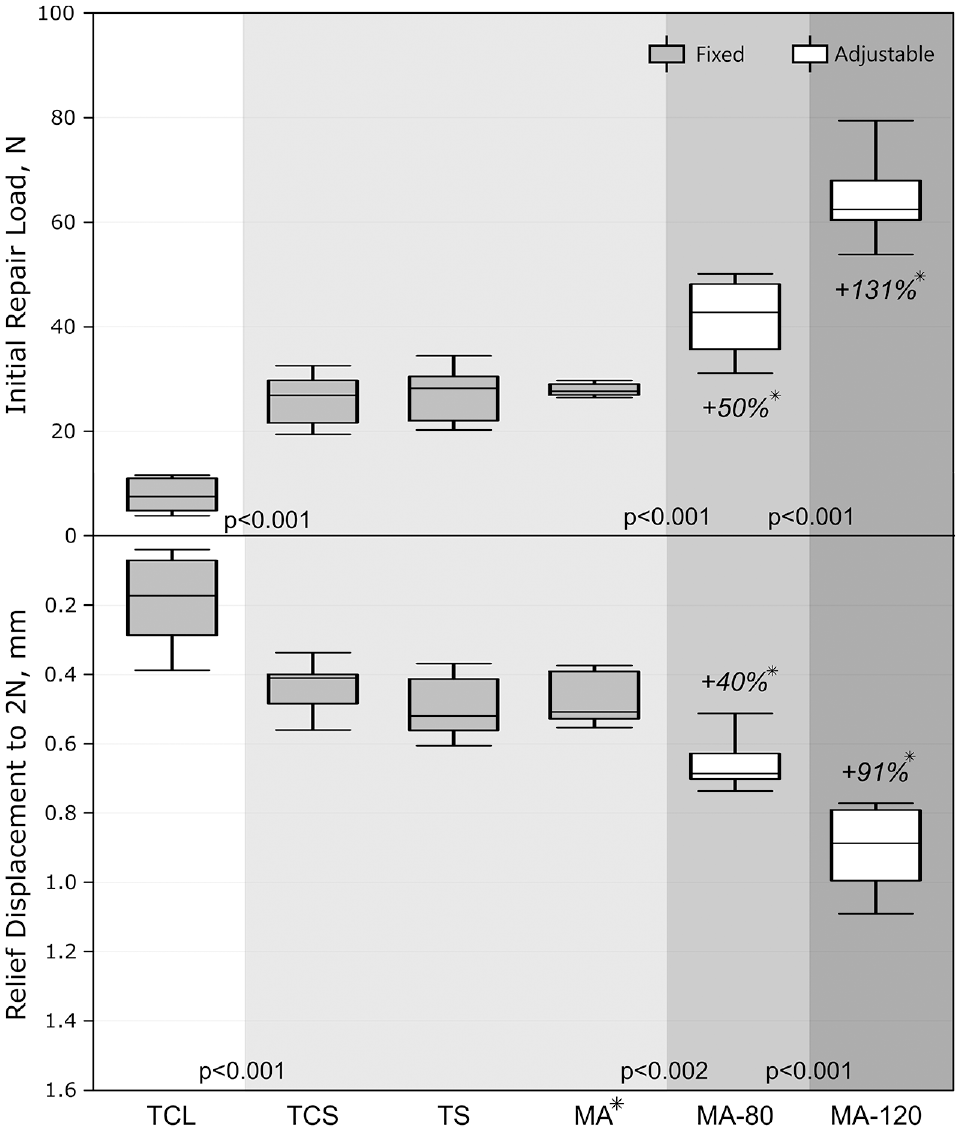
Initial repair load and corresponding relief displacement to reach the time-zero valley position (2-N load on the repair) with statistical analysis (different shaded backgrounds indicate statistical significance levels) and percentage deviation between adjustable and fixed Mason-Allen repair (asterisks with italic values). MA, Mason-Allen; TCL, 2 cinch loops; TCS, 2 cinch sutures; TS, 2 sutures.
Cyclic Testing
The displacement after 1000 load cycles is shown in Figure 5. The cinch-based suture repair groups (2 cinch loops and 2 cinch sutures) resulted in significantly higher displacement (P < .028); conversely, the high-tension adjustable repair achieved significantly smaller displacement (P < .016) compared with all other fixed groups. Besides the high-tension adjustable group, a significantly higher stiffness (P < .013) was found for the fixed Mason-Allen repair (Table 1). The stiffness of the 2 cinch sutures was similar to that of the 2 sutures but significantly lower (P < .004) compared with all other groups.

Displacement after 1000 load cycles with statistical analysis (different shaded backgrounds indicate statistical significance levels) and percentage deviation of adjustable to the fixed Mason-Allen group (asterisks with italic values). MA, Mason-Allen; TCL, 2 cinch loops; TCS, 2 cinch sutures; TS, 2 sutures.
The native meniscus provided significantly higher stiffness (104.9 ± 21.1 N/mm; P < .001) compared with all repairs. A native PMMR reference model was established to quantify and qualify the stabilization potential of actually tested repair techniques. All biomechanical time-zero tensile behaviors tested under simulated hoop-stress loading in line with the circumferential fibers were merged to establish a functional zone of the native meniscus (Figure 6). Representative hysteresis curves of each repair group at the end of testing were used to reference the native meniscus behavior. While hysteresis curves of the adjustable groups matched the function of the native meniscus, a completely loose state was assessed for cinch-based PMMR fixation groups.
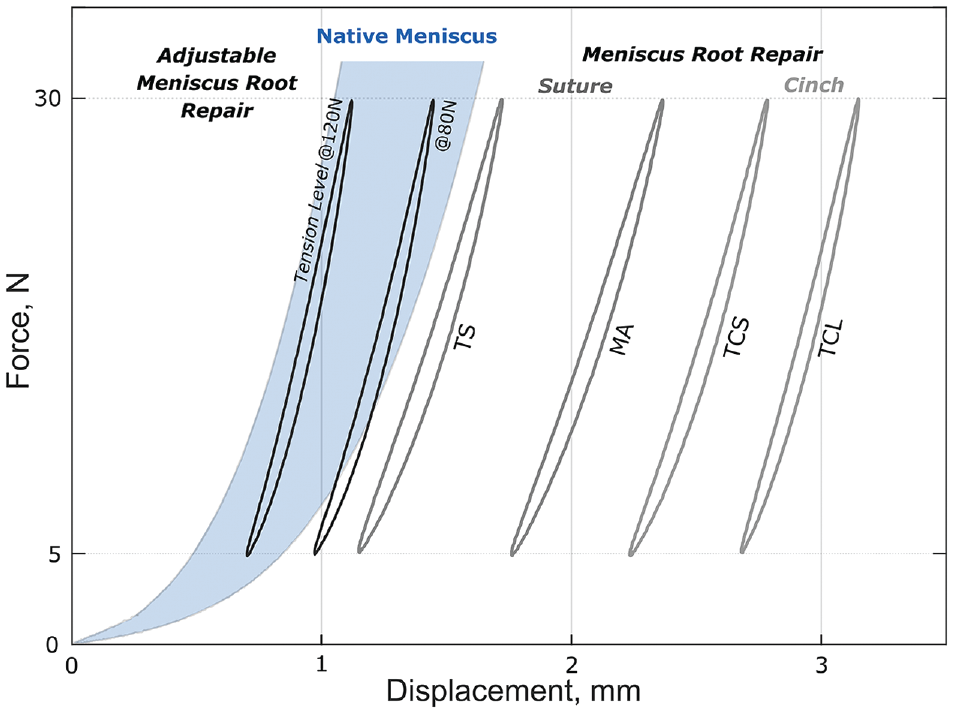
Representative hysteresis curves of various suture- and cinch-based repair groups at the end of testing (cycle 1000) illustrating the final loading situation of the adjustable and fixed repairs in reference to the native meniscus. MA, Mason-Allen; TCL, 2 cinch loops; TCS, 2 cinch sutures; TS, 2 sutures.
Pull to Failure
All constructs reached the regular test end and were pulled to failure. The 2 cinch sutures technique had the significantly lowest ultimate failure load (P < .023), whereas the Mason-Allen suture demonstrated the significantly highest ultimate failure load compared with all other PMMR repair groups (Figure 7). However, all repair techniques had significantly lower ultimate failure loads compared with the native meniscus root (711 ± 73.7 N; P < .001). Suture cut-through of the meniscus was the common mode of failure for all repair groups.
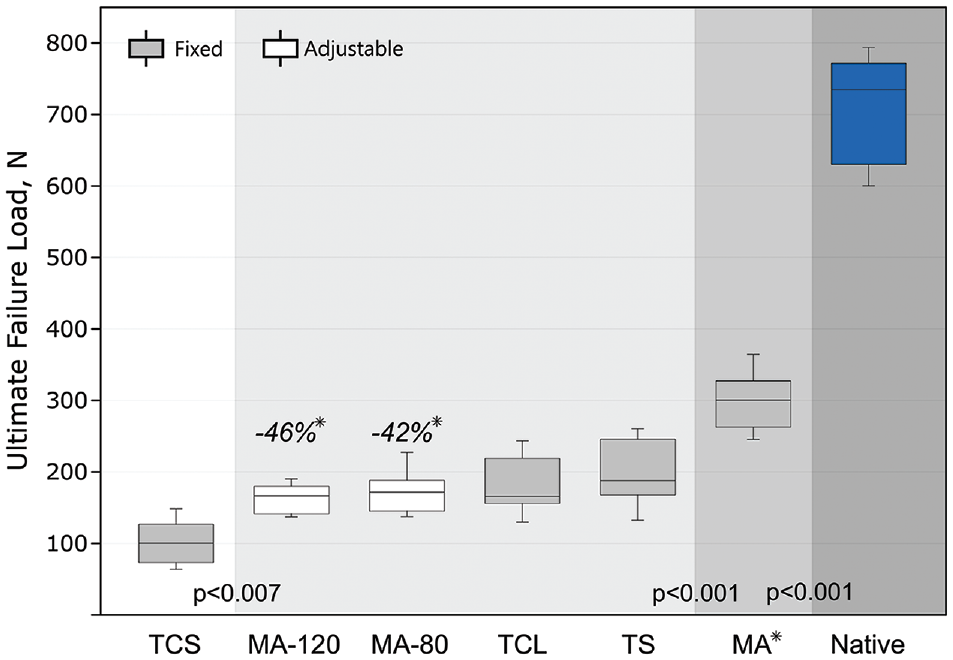
Mean and standard deviation values of the ultimate load during pull to failure with percentage deviation of adjustable to the fixed Mason-Allen group (asterisks with italic values). Different shaded backgrounds indicate statistical significance differences. MA, Mason-Allen; TCL, 2 cinch loops; TCS, 2 cinch sutures; TS, 2 sutures.
Discussion
The most important finding of this study was that a new adjustable tensioning implant for TPOR of PMMR tears increased initial repair load and relief displacement after fixation, as well as reduced cyclic displacement, compared with clinically reported suture repair techniques in a porcine model. However, the adjustable tensioning technique had a lower ultimate failure than the Mason-Allen technique using a cortical button. The PMMR repair with 2 sutures for tibial-sided knot tying (2 cinch loops) showed the lowest initial repair load, initial stiffness, and relief displacement after fixation. The cinch loop fixation constructs showed the most cyclic displacement, with some of the 2 cinch loops constructs demonstrating a displacement of >3 mm, indicating a nonfunctional repair.14,26,37 Adjustable TPOR, when tensioned to 120 N, showed significantly lower cyclic displacement compared with fixed suture constructs, while both adjustable tensioning groups (80 N and 120 N) provided sufficient stabilization to achieve similar displacement with cyclic loading to that seen in the intact meniscus.
Both the primary fixation and the resistance to cyclic displacement may influence the success of a meniscus root repair. An improved apposition of the meniscus to the prepared healing bed across a wider surface area and a more homogeneous pressure distribution onto the meniscal tissue are likely to improve the repair.27,32 A novel biomechanical test setup was established in this study for reproducible direct measurement of the tissue compression after primary fixation via the test machine. Previous biomechanical studies used displacement after the first load cycle as an indirect indicator for the initial suture repair fixation strength, without significance between groups.25,26,39 Significantly higher tissue compression and relief displacement suggest that the use of a modified Mason-Allen suture configuration with adjustable fixation, which deploys close to the joint line with higher tension on the repair suture, provides improved initial repair characteristics compared with various other conventional suture repairs with knot tying. The low initial repair load with manual knot tying of 2 sutures aligns with the reported upper tension limit (10 N) for primary repair fixation. 4 Subsequent knot tying of 4 sutures (2 suture couples) led to higher initial tissue compression, with an upper tension limit of about 30 N. Suture knot tying over a button was used as a method of choice, as it has been reported to offer higher fixation strength compared with tibial-sided suture anchor fixation. 33 It is unclear from the literature whether there is a critical tension level for optimized primary fixation or a critical displacement threshold leading to meniscus root healing compromise.
Previously reported biomechanical cyclic data align with the current results.14-16,25,26 Overlapping suture-lengthening effects of cinch loop–based meniscus root refixation with suture cut-through of the meniscus and continuous cinch loop tightening during repetitive loading may explain the overall greater cyclic displacement.14,26 In accordance with previous studies evaluating different suture materials for TPOR, no superior material behavior for either cinch-based meniscus root repair during cyclic loading was found, 16 but use of a suture tape for meniscal fixation provided a higher maximum failure load than use of a No. 2 suture.14,16,32 Our results are in agreement with previous studies that show that the 2 simple sutures fixation technique is the fixed repair technique with the least cyclic displacement, and the modified Mason-Allen repair achieves the highest ultimate failure strength.14,26 Traditionally, PEEK or titanium anchors have been used for suture repair fixation just below the tibial plateau using a posterior transseptal portal. 21 The direct suture repair with a titanium anchor has biomechanically been shown to significantly reduce displacement and increase stiffness compared with the conventional 2 simple sutures TPOR technique. 15 It was proposed that fixation adjacent to the joint line may be potentially advantageous in reducing meniscal micromotion at the repair site by enhancing the environment for meniscal healing. 15
The all-suture anchor implant for direct meniscus root fixation used in this study was locked by pulling on the deploying suture with 150 N without the need for a posterior medial portal. The actual force required to fully seat the anchor is unknown and may vary depending on the bone quality. Improper anchor deployment or placement in weaker bone (osteoporotic) could lead to anchor pull-out or excessive displacement seen with cyclic loading. Higher tissue compression coupled with adjustable tensioning of the repair sutures may have reduced the meniscus-suture complex's deformation, leading to smaller displacement during cyclic loading conditions. The rip-stop function of the modified Mason-Allen technique provided for higher resistance against suture cut-through of the meniscus to withstand repair failure. Higher resistance to cyclic displacement due to anchor migration, loop (or knot) slippage, suture elongation (“bungee effect”), or suture-induced cutting effects (“cheese wiring”) on the meniscus represents favorable fixation conditions reducing progressive, unrecoverable loosening of a repair, 39 for a greater likelihood of healing.30,36 Although the surgical application of the modified Mason-Allen technique is more challenging and requires a little extra surgical time, 3 minimizing suture-lengthening effects at the meniscus-suture interface seems to be the best way to optimize the TPOR technique. 10 The adjustable fixation used in this study had similar construct stiffness to the fixed TPORs and was lower than that found for titanium suture anchor TPOR placed at the level of the joint line. 15
While previous studies tested and analyzed the native PMMR attachment at the same cyclic test level, 15 time-zero mechanical properties of the native meniscus were used in this study as a critical reference for the repair groups. Time-zero testing is mostly considered to adequately mimic the way that loading is imposed on ligaments in real life given the complete ligament recovery after loading-unloading situations (maximum 30 N) within the linear-elastic load range. 40 In agreement with other studies, the ultimate load of repairs was inferior to that of the native PMMR attachment.15,23 The adjustable repair resulted in lower ultimate strength than the conventional Mason-Allen repair. With the suture-meniscus interface as a weak point, the critical stress threshold for suture cut-through depending on the tissue quality is crucial for the success of the repair. Favorable healing conditions with minimum elongation during cyclic loading and greater tissue compression with adjustable repair are mostly at the expense of a higher stress level in the vicinity of the suture-meniscus interface by reducing the residual stress threshold to induce damage or failure. Nevertheless, the ultimate failure loads of the adjustable and fixed repair techniques are likely to be higher than the forces acting on repaired medial meniscus root lesions in the early postoperative period with limited weightbearing. 38
Limitations
This study has several limitations. The in vitro biomechanical test model only focused on the time-zero stability of various meniscus root repairs and therefore may not be representative of a clinical setting. Releasing all the meniscocapsular junction does not replicate the in vivo situation. Simulated meniscal hoop-stress loading was applied in line with the circumferential fiber repair to achieve near-physiologic testing conditions with the meniscus fixed in customized clamps, which differs from variable in vivo loading of the knee joint including rotational and shear forces. Thus, the current test methodology is only a rough simulation of the in vivo loading environment in a porcine model, the obtained functional performance could differ from clinical device behavior for meniscus root repairs. Young porcine specimens may not replicate the quality of meniscal tissue and bone that is seen in middle-aged patients, who often sustain root tears. Variable knot tying and tensioning of the repair, depending on the surgeon's experience and the patient's bone quality, may further influence the outcome in clinical practice. Slight differences in the stitching pattern in variable menisci (size and quality) or in tunnel length may influence the mechanical behavior given the relative length of the repair construct. This biomechanical work focused on the performance of different meniscus root repair techniques, without clarifying the effects on biology and the patient's clinical outcome.
Conclusion
Adjustable TPOR led to considerably higher initial repair load and relief displacement than other conventional fixed repairs and restricted cyclic displacement to match the native meniscus function. However, the ultimate failure load of the adjustable devices was lower than that of a Mason-Allen construct tied over a cortical button. All repair techniques had significantly lower load to failure than the native meniscus root.
Footnotes
Final revision submitted September 18, 2023; accepted October 1, 2023.
One or more of the authors has declared the following potential conflicts of interest: S.B. is an employee of Arthrex. C.A.W. is an employee of Arthrex. A.J.K. is a consultant for Arthrex and has received nonconsulting fees from Arthrex; consulting fees from Arthrex, Joint Restoration Foundation, and Responsive Arthroscopy LLC; royalties or license from Arthrex; grant from DJO LLC; and honoraria from Joint Restoration Foundation and Musculoskeletal Transplant Foundation. P.A.S. is a consultant for Arthrex and has received royalties or license from Arthrex; nonconsulting fees from Kairos Surgical; education payments from United Orthopedics LLC and Elite Orthopedics LLC; hospitality payments from Medical Device Business Services; and compensation for serving as faculty or as a speaker for an accredited or certified continuing education program from Medical Device Business Services. M.J.F. is a consultant for Arthrex. R.F.L. has received royalties or license from Arthrex and Smith+Nephew; education payments from Foundation Medical LLC; nonconsulting fees from Smith+Nephew; compensation for serving as faculty or as a speaker for a nonaccredited and noncertified continuing education program from Linvatec; and consulting fees from Smith+Nephew and Arthrex. AOSSM checks author disclosures against the Open Payments Database (OPD). AOSSM has not conducted an independent investigation on the OPD and disclaims any liability or responsibility relating thereto.
Ethical approval was not sought for the present study.
