Abstract
Background:
The posterior oblique ligament (POL) is the largest structure of the posteromedial knee that is at risk of injury in conjunction with the medial collateral ligament (MCL). Its quantitative anatomy, biomechanical strength, and radiographic location have not been assessed in a single investigation.
Purpose:
To evaluate the 3-dimensional and radiographic anatomy of the posteromedial knee and the biomechanical strength of the POL.
Study Design:
Descriptive laboratory study.
Methods:
Ten nonpaired fresh-frozen cadaveric knees were dissected and medial structures were elevated off bone, leaving the POL. The anatomic locations of the related structures were recorded with a 3-dimensional coordinate measuring machine. Anteroposterior and lateral radiographs were taken with radiopaque pins inserted into the pertinent landmarks, and the distances between the collected structures were calculated. Each knee was then mounted to a dynamic tensile testing machine, and pull-to-failure testing was performed to record the ultimate tensile strength, stiffness, and failure mechanism.
Results:
The POL femoral attachment was a mean of 15.4 mm (95% CI, 13.9-16.8 mm) posterior and 6.6 mm (95% CI, 4.4-8.8 mm) proximal to the medial epicondyle. The tibial POL attachment center was a mean of 21.4 mm (95% CI, 18.1-24.6 mm) posterior and 2.2 mm (95% CI, 0.8-3.6 mm) distal to the center of the deep MCL tibial attachment and a mean of 28.6 mm (95% CI, 24.4-32.8 mm) posterior and 41.9 mm (95% CI, 36.8-47.0 mm) proximal to the center of the superficial MCL tibial attachment. On lateral radiographs, the femoral POL was a mean of 17.56 mm (95% CI, 14.83-21.95 mm) distal to the adductor tubercle and 17.32 mm (95% CI, 14.6-21.7 mm) posterosuperior to the medial epicondyle. On the tibial side, the center of the POL attachment was a mean of 4.97 mm (95% CI, 3.85-6.79 mm) distal to the joint line on anteroposterior radiographs and 6.34 mm (95% CI, 5.01-8.48 mm) distal to the tibial joint line on lateral radiographs, at the far posterior tibial aspect. The biomechanical pull-to-failure demonstrated a mean ultimate tensile strength of 225.2 ± 71.0 N and a mean stiffness of 32.2 ± 13.1 N.
Conclusion:
The anatomic and radiographic locations of the POL and its biomechanical properties were successfully recorded.
Clinical Relevance:
This information is useful to better understand POL anatomy and biomechanical properties as well as to clinically address an injury with repair or reconstruction.
The structures of the posteromedial knee such as the posterior oblique ligament (POL), posteromedial joint capsule, and meniscofemoral ligament are important for coronal and rotational stability. These structures can be injured along with the medial collateral ligament (MCL) and other medial knee structures with traumatic or sporting-type activities. Some medial-sided knee injuries can be treated in a nonoperative setting, while more severe injuries can require ligamentous reconstruction. 16 When a reconstruction of the posteromedial knee is performed, the location and positioning of this reconstruction are often grouped together with the MCL, despite its specific biomechanical role and the much larger anatomic area covered by the structures of the posteromedial knee. 2,5,8 LaPrade et al 13 performed an anatomic dissection of the medial knee while describing the qualitative anatomy of the medial knee, including the POL. While this study 13 provides basic anatomy for the surgeon attempting an anatomic reconstruction of the posteromedial knee, the present literature lacks quantitative anatomy of the posteromedial knee and its relation to frequently used radiographic landmarks.
Prior sectioning studies have demonstrated the cooperative relationship between the POL and MCL in providing stabilizing forces to a rotational stress. There is a complex load-sharing interplay between the POL and MCL, such that these ligaments both contribute to resist the combination of valgus and rotational strains. 20 While the POL and its attachments have been qualitatively described, the quantitative measurements, radiographic locations, and biomechanical strengths of various portions of the posteromedial knee have not been fully described in a single study to provide operative guidance. 2,5,6,11 Specifically, the central arm of the POL is qualitatively the most stout portion of the POL, and its bony attachment is on the femur and tibia. 5 Therefore, the central arm is the most surgically relevant target for study. As the POL is an important structure and contributor to the stability of the medial knee, severe injuries could benefit from a separate procedure to address the POL directly. Obtaining the information on quantitative anatomy, biomechanics, and replicable radiographic location of the POL would be useful in order to better understand its properties, as well as to inform clinically addressing of an injury with repair or reconstruction.
The purpose of this study was to evaluate the anatomy of the posteromedial knee along with performing a quantitative anatomic and radiographic evaluation of the central arm of the POL of the posteromedial knee. This included evaluating attachment sites and relationships to the pertinent osseous and soft tissue landmarks. We hypothesized that the POL has replicable parameters with regard to its attachment sites and consistent relationships to surgically pertinent landmarks correlating with plain radiographs. We also hypothesized that the biomechanical strength of the central band of the POL supports its role as a restraint to external rotation and valgus force and would inform the strength required in a graft choice for potential reconstruction of the central arm of the POL.
Methods
Specimen Preparation
We used 10 unpaired, fresh-frozen human cadaveric knees (mean age, 60.9 years; range, 51-68 years) without evidence of previous injuries or surgery in this study. The specimens were donated to a tissue bank for medical research and then purchased by our institution. Specimens that met the following inclusion criteria were selected: aged 18 to 69 years, no previous surgery or documented knee injury, and no history of metastatic disease. The use of cadaveric specimens does not require institutional review board approval at our institution.
All dissections were performed by 2 authors (A.J.C. and A.B.) in a stepwise fashion. The specimens were dissected of skin and subcutaneous tissue, sparing the major ligaments of the knee and the structures of the medial knee. The medial knee structures of interest were then identified and carefully resected, and their attachment sites were marked with indelible ink. The central arm of the POL was spared from dissection, with its femoral and tibial attachments maintained for later pull-to-failure testing. The attachment points on both the femur and the tibia were marked with indelible ink for future measure and evaluation. The structures of interest on the femur included the adductor tubercle, gastrocnemius tubercle, medial epicondyle, center of the MCL attachment, lateral epicondyle, central arm of the POL attachment on the femur, and meniscofemoral ligament. The structures on the tibia included the center of the superficial MCL attachment, semimembranosus anterior arm, center of the deep MCL tibial attachment, and central arm of the POL attachment on the tibia.
3-Dimensional Measurements
The femur and tibia were clamped in 50° of knee flexion. The previously described anatomic landmarks were measured and recorded using a coordinate measuring machine (Romer Absolute Arm; Hexagon Metrology) with manufacturer-reported repeatability of 0.0011 mm. Attachment areas, locations, distances between the centers of attachment sites, and pertinent landmarks were calculated. A representative dissected specimen and the corresponding anatomic landmarks that were measured and analyzed are shown in Figure 1.

Medial knee structures that were evaluated. ME, medial epicondyle; POL, posterior oblique ligament; sMCL, superficial medial collateral ligament.
Radiographic Analysis
After identification of the individual structure attachments, surgically identifiable reference points were marked with radiopaque metal pins (1.03 mm–diameter T-pins; Swinton Avenue Trading). These markers were inserted into the center of their respective attachment sites, flush to the cortical bone. These reproducible radiographic reference points included the medial epicondyle, center of the femoral POL attachment, adductor tubercle, anterior arm of the semimembranosus, tibial POL attachment, and center of the deep MCL tibial attachment. A dissected specimen and corresponding radiopaque pin placement are demonstrated in Figure 2.
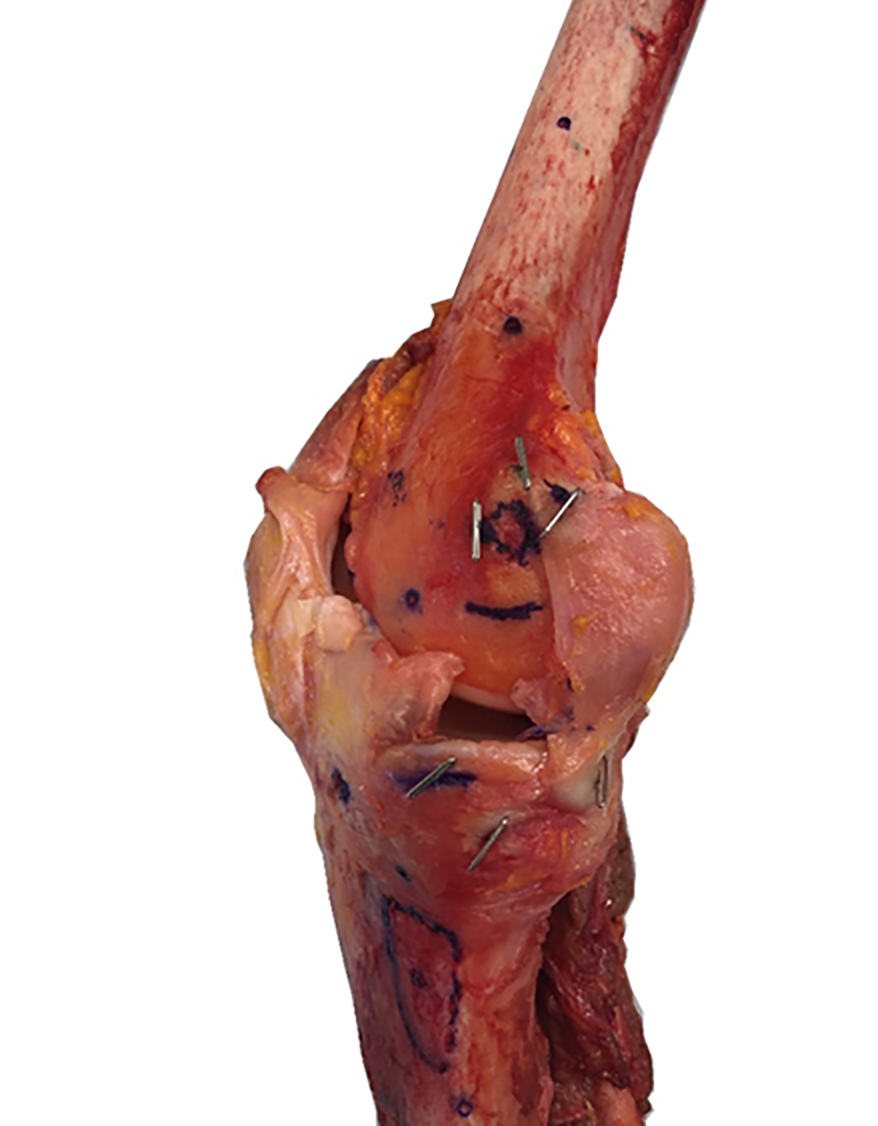
Radiographic markers for the anatomic landmarks.
True anteroposterior (AP) 12 and lateral radiographs 15 were taken in plane utilizing a fluoroscopic C-arm (GE OEC 9800; Milpitas CA). In order to correct for disparities in magnification and allow for image calibration to make digital measurements, a 25.4-mm radiopaque sphere (diameter, 25.4 ± 0.00254 mm; sphericity, 0.00061 mm; Small Parts Inc) was positioned in the field of view. These images were imported into a custom MATLAB script (MathWorks) for digital fluoroscopic measurements. The distances were measured digitally between the attachment points and pertinent bony landmarks by a single author (A.J.C.), using the marker ball for size calibration. First, the distances from the previously mentioned bony landmarks to the POL footprints were measured. Then, distances between the tibial plateau joint line and the tibial POL center were calculated on both the AP and the lateral fluoroscopic views. All measurements were made from the intersection of the horizontal and vertical limbs of the T-pins, which corresponds to the cortical bone where the anatomic feature of interest is located. The measurements that were performed on the radiographs are demonstrated in Figure 3.

POL distances on (A) anteroposterior and (B) lateral radiographs. AT, adductor tubercle; ME, medial epicondyle; MTL, meniscotibial ligament; POL, posterior oblique ligament; SM, semimembranosus.
Biomechanical Testing
The specimens had been previously skeletonized, such that the POL and other major knee ligaments were retained. These specimens were then cross-pinned in extension utilizing 2.0-mm Steinmann pins to maintain the 0° knee flexion angle and the anatomic femorotibial orientation and relationship. All other soft tissues connecting the femur and tibia were then sectioned, leaving only the POL connecting the femur to the tibia. Next, the femur and tibia were potted in polymethylmethacrylate (Fricke International Inc) and mounted to a dynamic tensile testing machine (ElectroPuls E10000; Instron). Once the specimen was mounted, the Steinmann pins were removed, and the specimen was then pulled to failure in line with the long axis of the femur and tibia. The analysis included ultimate load, stiffness, elastic limit, and failure mechanism. The results from the biomechanical analysis were reported as means with 95% CIs. The setup is shown in Figure 4.

Specimen mounted in actuator before pull-to-failure biomechanical testing.
Results
Anatomic Findings
In all specimens, the femoral insertion of the POL was identified distally and posteriorly to the apex of the adductor tubercle. The POL was located posterior to the sMCL, which originated posterior and proximal to the medial femoral epicondyle. The 3 arms of the POL were identified during dissection: the superficial, capsular, and central arms. In all specimens, the anterior portion of the distal fibers of the POL were identified merging with the semimembranosus, and the posterior fibers attached to the posteromedial tibia directly. The direct tibial insertion of the POL was proximal to the insertion of the semimembranosus. The tibial insertion of the sMCL was widely attached to the medial tibia. The anatomic locations and a majority of the measurements are shown in Figure 5.

Anatomic measurements of the posterior oblique ligament in relation to other medial anatomic reference points. AT, adductor tubercle; dMCL, deep medial collateral ligament; fPOL, femoral posterior oblique ligament; ME, medial epicondyle; SM, semimembranosus; sMCL, superficial medial collateral ligament; tPOL, tibial posterior oblique ligament.
Quantitatively, the femoral attachment area of the POL was 57.2 mm2 (95% CI, 41.0-73.4 mm2). The femoral attachment area of the sMCL was 72 mm2 (95% CI, 58.6-85.5 mm2). The tibial attachment area of the POL was 65.6 mm2 (95% CI, 56.6-74.5 mm2). The tibial attachment area of the sMCL was 438.7 mm2 (95% CI, 363.6-513.8 mm2) (Table 1).
The center of the femoral attachment of the POL was a mean of 10.8 mm (95% CI, 8.9-12.6 mm) posterior and 14.6 mm (95% CI, 12.8-16.4 mm) distal to the adductor tubercle, along with being 15.4 mm (95% CI, 13.9-16.8 mm) posterior and 6.6 mm (95% CI, 4.4-8.8 mm) proximal to the medial epicondyle. Compared with the superficial MCL center on the femur, the center of the POL femoral attachment was 11.1 mm (95% CI, 9.8-12.5 mm) posterior and 2.4 mm (95% CI, 0.0-4.9 mm) superior (Table 2).
Distance and Area Measurements for Medial Structures of the Knee a

a Data are reported as mean (95% CI). Dashes indicate areas not applicable. POL, posterior oblique ligament; sMCL, superficial medial collateral ligament..
Anatomic Locations of the Medial Knee Structures a

a Data are reported as mean (95% CI). POL, posterior oblique ligament; MCL, medial collateral ligament; sMCL, superficial medial collateral ligament.
The tibial POL attachment center was located a mean of 28.6 mm (95% CI, 24.4-32.8 mm) posterior and 41.9 mm (95% CI, 36.8-47.0 mm) proximal to the center of the superficial MCL on the tibia and 21.4 mm (95% CI, 18.1-24.6 mm) posterior and 2.2 mm (95% CI, 0.8-3.6 mm) distal to the center of the deep MCL attachment.
Radiographic Findings
The distances were all measured from the POL pin to that of the other anatomic features. On the AP radiograph, the mean distance from the femoral POL to the adductor tubercle was 14.98 mm (95% CI, 10.1-19.86 mm). The POL was a mean of 5.28 mm (95% CI, 3.32-8.43 mm) from the medial epicondyle. On the tibia, the tibial POL center was a mean of 4.97 mm (95% CI, 3.85-6.79 mm) distal to the tibial joint line, 10.16 mm (95% CI, 7.98-13.67 mm) from the center of the meniscotibial ligament, and 10.01 mm (95% CI, 8.05-13.16 mm) from the anterior extent of the semimembranosus tendon (Table 3).
On the lateral knee radiograph, the femoral POL was a mean of 17.56 mm (95% CI, 14.83-21.95 mm) distal to the adductor tubercle and 17.32 mm (95% CI, 14.6-21.7 mm) posterosuperior to the medial epicondyle. On the tibia, the tibial POL center was 6.34 mm (95% CI, 5.01-8.48 mm) distal to the joint line, 24.20 mm (95% CI, 21.46-28.63 mm) distal to the meniscotibial ligament, and 16.87 mm (95% CI, 13.63-22.11 mm) from the anterior extent of the semimembranosus tendon. The radiograph results can be found in Table 3.
Radiographic Measurement of Distances From the Medial Knee Structures to the POL a

a Data are reported as mean (95% CI). AP, anteroposterior; POL, posterior oblique ligament.
Structural Findings
The biomechanical pull-to-failure testing yielded a mean tensile strength of 225.2 ± 71.0 N, while the mean stiffness value was found to be 32.2 ± 13.1 N. The mechanism of failure varied in multiple ways, including failure at the midsubstance of the ligament (n = 7), with 2 of the 7 midsubstance tears being relatively close to the tibial attachment. The other 3 specimens had a ligament avulsion as their mechanism of failure, with 2 of the avulsions occurring at the tibial attachment and the other occurring at the femoral attachment of the ligament.
Discussion
In this cadaveric study, we evaluated the anatomic and radiographic locations of structures of the posteromedial knee, with a focus on the POL. The most important finding of this study was the localization of the central arm of the POL with respect to other surgically relevant anatomic and osseous landmarks. The anatomic localization of the POL, the reproducible radiographic localization, and biomechanical values establishing pull-to-failure tensile strength and stiffness values all provide clinical applicability and intraoperative utility.
The location of the POL was described quantitatively relative to the other medial knee structures in absolute terms, as well as by using radiography. The anatomic portion of the study revealed a completely separate femoral POL attachment site from the MCL, along with the complex interplay and close proximity with the posteromedial knee structures on the tibia. It is important to stress that the surgeon obtain “true” AP and lateral images, as the radiographic evaluation identified distinct radiographic positions of the POL attachment that can be reproducibly found and localized relative to other prominent and identifiable anatomic structures. To note, the values presented in the current study are mean values and likely vary based on patient size. Recent literature has demonstrated a relatively low consensus on treatment of posteromedial corner injuries, suggesting that there is more to be elucidated in this complex anatomic region. 3 The findings of this study contribute to a broader understanding of these medial-sided knee injuries.
The POL itself is a complex structure and has previously been described with 3 distal attachment limbs, previously termed the superficial, central, and capsular arms. 5,9,19 The central arm is the largest and thickest part of the POL, and thus it was the central focus of investigation in this study. The central arm has a robust attachment to the meniscofemoral and meniscotibial ligaments, with a distal attachment to the posteromedial portion of the medial meniscus and the posteromedial tibia. 7 The superficial and capsular arms attach to the proximal femoral footprint, with their distal attachments being either primarily fascial in nature or onto soft tissue structure. As the central arm has the bony tibial attachment, this portion of the POL was studied most in-depth as the target for reconstruction.
While much is written on medial knee injuries and the POL has long been identified as a structure, a comprehensive analysis of biomechanical properties has not been performed. 9,19 The structures of the posteromedial knee confer dynamic rotational stability in addition to valgus constraint. 8,18 The POL has been shown to work in concert with the MCL, and the loads seen by the MCL and POL vary based on knee flexion angle. 4,7,20 As such, in severe medial-sided knee injuries in which only the MCL is addressed, full restoration of stability to the knee may not be achieved.
The biomechanical investigation in this study isolated the central arm of the POL, identifying the native state and its tensile strength. Our findings revealed a mean ultimate tensile strength of 225.2 N, which is comparable with that of the native medial patellofemoral ligament from previous biomechanical studies. 1,14 Prior biomechanical work on the strength of the medial knee structures found a very similar finding of 256 N for the central arm of the POL. 11 This information may suggest an appropriate graft choice for potential reconstruction. Given that many surgeons opt for a gracilis or semitendinosus allograft for medial patellofemoral ligament reconstruction, this may be a reasonable graft choice when a POL reconstruction is planned. 18
The present study confirms the relative locations as described by LaPrade and further adds quantitative radiographic localization and tensile strength. 11,13 There were some differences in mean location of the femoral POL attachment in our study, but they were roughly the same magnitude for all measurements compared with prior work. This could be explained by varying anatomic specimens, which would change the mean distances measured, as well as differing measurement systems and techniques. Furthermore, the measurements may not be at the same knee flexion angle or reference frame.
While Athwal et al 2 similarly dissected the medial knee and evaluated it radiographically to provide anatomic locations, they primarily described it qualitatively. Furthermore, the prior work did not utilize fluoroscopy to provide measurable quantitative values that could be used to localize the POL with reference to other anatomic prominences. These additional data would be useful intraoperatively to be able to localize the POL's central arm for potential reconstruction placement during reconstruction and guide intraoperative decision making. The described technique for reconstruction of the posteromedial knee has demonstrated locations relative to other structures. 4 Our description of fluoroscopic imaging location provides further replicable information to ensure the accurate localization, which can be used intraoperatively to ensure a more anatomic placement of the graft.
We believe that combining these data of the exact location, failure mechanisms, tensile graft strengths, and radiographic landmarks to be used intraoperatively greatly facilitates potential reconstruction. This information would provide the ability to perform a more anatomic medial and posteromedial knee reconstruction. Many of the previous techniques utilize more of a sling technique and do not fully reproduce the anatomy of the medial knee. 10,14 Furthermore, isolated MCL reconstruction and repairs have demonstrated continued residual valgus gapping, and the potential that surgeons may not be fully addressing the instability. 12 Although techniques vary, the addition of a posteromedial knee reconstruction has shown very good return to sport and knee stability. 4 As such, including the data from our study to more anatomically reconstruct the POL will likely contribute to a more anatomic reconstruction with more consistent technique and improved outcomes after medial knee ligament injuries.
Limitations
We recognize that there are limitations to this study. The data that can be drawn from it are limited by the inherent limitations of cadaveric specimens. The specimens utilized came from older donors and therefore had varying amounts of degenerative change to the knees themselves. The bony architecture as well as soft tissue integrity changes with age. 15,17 There is also anatomic variability in the specimens that cannot be controlled. As such, the measurements and data may not be fully applicable to the knees of younger patients or athletes who would require a surgical intervention or reconstruction of their posteromedial knee. However, this could be said of any cadaveric biomechanical study, and the variability in specimens is likely to reflect the differing anatomy that exists in the population and represent the mean measurements across potential patients. Additionally, some of the measurements had a relatively large standard deviation. This may have been improved by increasing the number of specimens, but it also may just reflect the natural variability in the anatomy of the knee.
Second, while the biomechanical data give a mean tensile strength, this is only in tensile pull-to-failure. The POL acts as a valgus and rotational stabilizer, so the testing conditions do not mimic an injury model. Similarly, this study used a static model, and all other structures connecting the femur and tibia were sectioned before biomechanical testing; however, the knee is a dynamic structure. As a result, this does not mimic the state of the intact patient knee. However, this study establishes initial biomechanical data for POL tensile strength, which can serve as a foundation for future biomechanical studies to evaluate more complex injury mechanisms. The rationale for this testing protocol was to avoid the use of soft tissue clamps, which are commonly used for ligament load to failure. Soft tissue clamps can lead to slippage if they are too loose or to damage to the specimens if they are too tight, and it was therefore preferable to simply use the native bony attachments and load the ligament to failure from the bones themselves. Testing in a valgus and rotational mechanism would require several more degrees of freedom from the testing robot and would not truly mimic the intact knee.
Conclusion
Overall, this investigation into the anatomy, radiographic locations, and biomechanics of the posteromedial knee and POL provides additional quantitative data on the POL and radiographic locations that can be utilized intraoperatively. The study findings contribute to the knowledge of the posteromedial knee and may inform surgical decision making. Future biomechanical injury and reconstruction studies will be useful to further elucidate this complex part of the knee.
Footnotes
Final revision submitted February 3, 2023; accepted February 22, 2023.
One or more of the authors has declared the following potential conflict of interest or source of funding: A.J.C. has received grant support from Arthrex and education payments from Arthrex and Smith & Nephew. J.A.G. has received education payments from Arthrex, consulting fees from Bioventus and DePuy, and nonconsulting fees from Smith & Nephew. AOSSM checks author disclosures against the Open Payments Database (OPD). AOSSM has not conducted an independent investigation on the OPD and disclaims any liability or responsibility relating thereto.
Ethical approval was not sought for the present study.
