Abstract
Background:
Although arthroscopic screw fixation and suture fixation are mainstream interventions for displaced anterior cruciate ligament avulsion fractures of the tibia, the differences in clinical outcomes between them remain inconclusive.
Purpose:
To conduct a meta-analysis comparing the clinical and functional outcomes between arthroscopic screw fixation and suture fixation for tibial avulsion fractures.
Study Design:
Systematic review; Level of evidence, 3.
Methods:
A systematic review was conducted following the PRISMA (Preferred Reporting Items for Systematic Reviews and Meta-Analyses) guidelines and using the PubMed, Embase, and Cochrane Central Register of Controlled Trials databases. Inclusion criteria were English-language articles that compared functional outcomes after screw fixation versus suture fixation for tibial avulsion fractures and had at least 1-year follow-up. Relevant data were extracted and analyzed statistically using the Mantel-Haenszel method and variance-weighted means. Random-effects models were used to generate pooled relative risk (RR) estimates with confidence intervals (CIs).
Results:
Of 1395 articles initially identified, we included 5 studies with 184 patients (91 patients with screw fixations and 93 patients with suture fixations). The pooled results indicated similar postoperative outcomes for screw fixation and suture fixation: Lysholm score (mean difference [MD], −0.32 [95% CI, −6.08 to 5.44]; P = .91), proportion of International Knee Documentation Committee score grade A (74% vs 74%; RR, 0.63 [95% CI, 0.10-3.95]; P = .63), Tegner score (MD, 0.10 [95% CI: −1.73 to 1.92]; P = .92), and Lachman test results (stable knee joint, 82% vs 82%; RR, 0.99; 95% CI: 0.85-1.16; P = .90). Patients in the screw fixation group had a significantly higher overall subsequent surgery rate (46% vs 19%; RR, 2.33; 95% CI,1.51-3.60; P = .0001) and implant removal rate (44% vs 3%; RR, 8.52; 95% CI, 3.58-20.29; P < .00001) compared with those in the suture fixation group. Nonimplant-related subsequent surgery rates were similar for the 2 groups.
Conclusion:
The findings indicated a higher risk of subsequent surgery (RR, 2.33) and implant removal (RR, 8.52) after screw fixation when compared with suture fixation for tibial avulsion fractures. However, there were no significant differences in clinical outcome scores between the 2 techniques.
Keywords
Anterior cruciate ligament (ACL) tibial avulsion fractures, also known as tibial eminence fractures, are intra-articular fractures of the bony attachment of the ACL on the tibia. The Meyers and McKeever classification categorizes fractures of the tibial eminence into 3 types. 20 Type I fractures refer to nondisplaced or minimally displaced eminence fractures. Type II fractures indicate that the anterior one-third to one-half of the avulsed bone has been displaced proximally or hinged. Type III fractures refer to complete separation of the avulsed fragments. 20 Rotated and comminuted fractures are identified as type IV. 32 For displaced ACL avulsion fractures, nonoperative treatment commonly results in higher rates of nonunion 9 ; therefore, surgical fixation should be considered for these types of fractures.
Fixation for avulsion fracture fragments can be achieved by using a variety of implants such as Kirschner wires, 14,31 sutures, 2,10 and screws. 14,29 Among these techniques, arthroscopic fixations with screws or sutures are the current mainstream interventions. In biomechanical performance, the comparative fixation strength between sutures and screws remains inconclusive. Tsukada et al 28 found screw fixation to be superior in obtaining rigid fixation under cyclic loading. Mahar et al 17 showed no clear biomechanical differences, including in failure tensile force and deformation after cyclic loading, between fixation methods using screws and sutures. Other studies concluded that sutures provide more fixation strength than screw fixations. 3,7
In addition to the biomechanical findings, the clinical results showed contrasting findings for screw fixations and suture fixations used for tibial avulsion fractures. Better pivot-shift performance and shorter operating times were observed in screw-fixation surgical procedures, 23 whereas lower subsequent surgery rate and better functional outcome scores were observed for suture-fixation surgical procedures. 4,13 The latest clinical study conducted by Callanan et al 4 revealed that suture and screw fixations lead to comparable clinical outcomes.
The purpose of this study was to conduct a systematic review and meta-analysis comparing the clinical and functional outcomes after arthroscopic screw fixation versus suture fixation for tibial avulsion fractures.
Methods
This meta-analysis was conducted according to the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines. 22 A systemic search was conducted online in the PubMed, Embase, and Cochrane Central Register of Controlled Trials databases from their earliest entry points to January 1, 2021, using the following search keywords: “tibial eminence fracture,” “tibial eminence avulsion,” “intercondylar fracture,” “intercondylar avulsion,” and “anterior cruciate ligament avulsion.” We also used the Google search engine with these keywords and reviewed the reference lists in the relevant articles to find any additional pertinent studies.
Study Selection
After removing duplicates, all titles and abstracts of the remaining citations were screened carefully. The search for relevant studies and exclusion of papers were executed by 2 authors (C.-J.C., T.-C.H.) independently. Two authors (C.-J.C., C.-K.H.) performed data extraction and article appraisal. When discrepancies occurred, a consensus was reached through discussion. Articles designed without a control group, animal studies, biomechanical studies, studies without clear patient characteristics, and those with insufficient available data were excluded. We then appraised the studies and identified those eligible for inclusion in the analysis. The authors assessed the quality of each article by using the STROBE (strengthening the reporting of observational studies in epidemiology) statement. 30
Data Extraction
Two authors (C.-J.C., T.-C.H.) independently extracted the data from the articles, and we contacted the authors of the included articles for missing data. The following data were extracted from the included articles: (1) patient characteristics (age, sex, fracture type, follow-up time), (2) clinical outcomes (complications, Lysholm knee score, Lachman test, Tegner score, International Knee Documentation Committee [IKDC] score), (3) subsequent surgery details (implant removal, manipulation, adhesion lysis, and ACL reconstruction), (4) index surgical procedures performed arthroscopically and with limited open incision.
Statistical Analysis
The Mantel-Haenszel method and variance-weighted means were used to analyze the outcomes. We used I 2 to evaluate and quantify the effects of heterogeneity. 12 The I 2 range was from 0% to 100%. An I 2 value of greater than 50% indicated obvious heterogeneity, 11 and a random-effects analysis was used to compare studies showing heterogeneity. 5 A fixed-effects analysis was used to compare studies without obvious heterogeneity. 16 Heterogeneity, mean difference (MD), and relative risk (RR) with confidence intervals (CIs) were calculated for all outcomes in this meta-analysis. We also assessed the possibility of publication bias by using Egger funnel plots. 6 This meta-analysis was carried out with Review Manager version 5.3 software (The Nordic Cochrane Centre, The Cochrane Collaboration).
Results
Initially, a total of 1395 articles were found using the search strategy discussed in Methods. After removing duplicates, 751 articles went through title and abstract screening. After applying the inclusion and exclusion criteria, 5 retrospective cohort studies, all with level 3 evidence, were identified and included in the meta-analysis (Figure 1). No patients with Meyers and McKeever type I fractures were included among the studies. Two of the studies used arthroscopy only, 4,23 and another 2 studies used arthroscopy first, 13,26 but limited open incision could have also been used if difficulties were encountered during fracture reduction. One study included both open reduction and arthroscopic surgical procedures, 18 but information on only arthroscopic procedures was extracted from this study.

Flow diagram for study selection following the PRISMA guidelines. PRISMA, Preferred Reporting Items for Systematic Reviews and Meta-Analyses.
Characteristics of the patients in the 5 studies of interest are summarized in Table 1. A total of 91 patients receiving screw fixation and 93 patients receiving suture fixation were included in the meta-analysis. No major complications were recorded in the included studies. Hardware removal was performed in 40 patients (44%) in the screw fixation group, whereas only 3 patients (3%) received implant removal in the suture fixation group.
Summary of Studies Included in the Meta-analysis a

a ACLR, anterior cruciate ligament reconstruction; F, female; M, male; NA, not applicable; STROBE, strengthening the reporting of observational studies in epidemiology.
b All studies were retrospective cohort studies with an evidence level of 3.
c Meyers and McKeever classification.
d Out of a possible 22 points.
The average postoperative Lysholm knee score was 93.4 (76-100) in the screw fixation group and 92.2 (70-100) in the suture fixation group. The pooled data showed no significant between-group differences in these 2 treatment groups (MD, −0.32 [95% CI, −6.08 to 5.44]; P = .91) (Figure 2). IKDC grade A function level was achieved in 25 patients (25/34 = 74%) in the screw fixation group and 23 patients (23/31 = 74%) in the suture fixation group. Pooled data also revealed no significant between-group differences (RR, 0.63 [95% confidence interval [CI], 0.10-3.95]; P = .63) (Figure 3).

Forest plot comparing the mean differences in the postoperative Lysholm knee scores in the screw-fixation group and suture-fixation group. CI, confidence interval; IV, inverse variance.

Forest plot comparing IKDC scores rated as grade A function in patients with screw fixations and suture fixations. CI, confidence interval; IKDC, International Knee Documentation Committee; M-H, Mantel-Haenszel.
The average Tegner score was 7.4 in patients receiving screw fixations, whereas the average score was 6.9 in the suture fixation group. No significant differences were found in the pooled data (MD, 0.10 [95% CI, −1.73 to 1.92]; P = .92) (Figure 4). Regarding knee joint stability, 42 patients (42/51 = 82%) were assessed as “stable joint” by Lachman test in the screw fixation group, and 41 patients (41/50 = 82%) were tested to be stable joint in the suture fixation group (RR, 0.99 [95% CI, 0.85-1.16]; P = .90) (Figure 5).
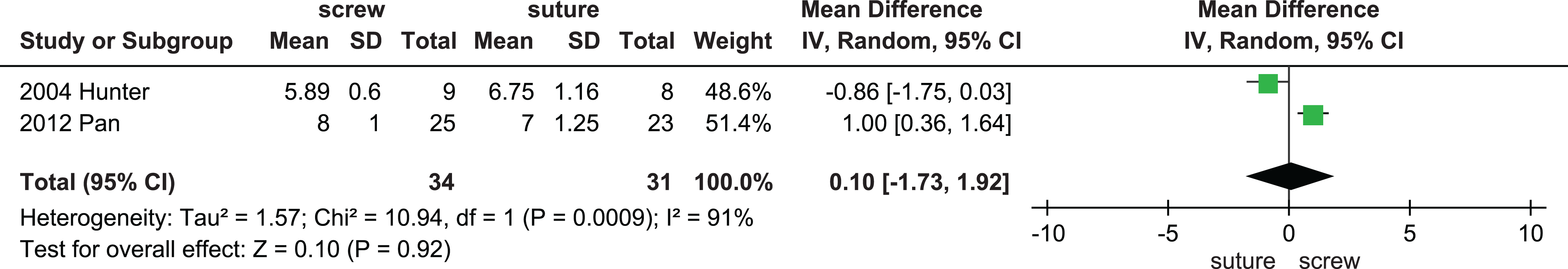
Forest plot comparing the mean differences in Tegner activity levels in patients with screw fixations with those with suture fixations. CI, confidence interval; IV, inverse variance.

Forest plot comparing the relative risk of Lachman tests assessed as “stable joint” in the screw fixation group with those in the suture fixation group. CI, confidence interval; M-H, Mantel-Haenszel.
The overall subsequent surgery rate was nearly half (42/91 = 46%) of the patients in the screw fixation group, whereas only 18 (18/93 = 19%) patients underwent reoperation in the suture fixation group (RR, 2.33; 95% CI, 1.51-3.60; P = .0001) (Figure 6). The subgroup analysis showed that risk of implant removal was significantly higher in the screw fixation group than it was in suture fixation group (44% vs 3%, respectively; RR, 8.52; 95% CI, 3.58-20.29, P < .00001) (Figure 7). However, the subgroup analysis examining the subsequent surgery rates for procedures other than hardware removal surgery revealed no between-group differences (23% vs 19% for screw fixation and suture fixation, respectively; RR, 1.15; 95% CI, 0.70-1.89; P = .58) (Figure 8).

Forest plot comparing the relative risk of overall subsequent surgery in patients with screw fixations with those undergoing suture fixations. CI, confidence interval; M-H, Mantel-Haenszel.

Forest plot comparing the relative risk of implant removal in patients with screw fixations with those with suture fixations. CI, confidence interval; M-H, Mantel-Haenszel.

Forest plot comparing the relative risk of subsequent surgical procedures other than implant removal in the screw fixation group and suture fixation group. CI, confidence interval; M-H, Mantel-Haenszel.
Discussion
The most important findings of this meta-analysis included that there were no differences in functional outcome for patients receiving screw fixations or suture fixations, including Lysholm knee scores (93.4 vs 92.2, respectively; P = .91), achievement of IKDC score grade A (74% vs 74%; P = .63), and Tegner score (7.4 vs 6.9, respectively; P = .92). No difference was noted in knee stability in terms of Lachman test results between the 2 groups (stable knee joint, 82% vs 82%; P = .90). However, the subsequent surgery rate was higher in the screw fixation group (46% vs 19% for the suture fixation group; P = .0001). Although arthroscopic interventions with screws or suture fixation are the current mainstay surgical procedures for tibial avulsion fractures, there is still no consensus on the optimal fixation methods in the past. Some surgeons adopted screw fixation because of the shorter surgical time and better pivot-shift performance, 23 whereas others preferred suture fixation owing to better functional outcome scores and lower subsequent surgery rates. 4,13
Several biomechanical studies have compared the fixation strength between screw fixation and suture fixation. Tsukada et al 28 observed less anterior translation using antegrade screw fixation compared with the Ethibond (Ethicon, Inc.) suture fixation in a type III fracture model after cyclic loading tests. On the other hand, other cadaveric studies demonstrated that Fiberwire (Arthrex, Inc.) suture fixation provided higher peak failure loading compared with screw fixation. 3,7 Residual instability after tibial avulsion fracture is a clinical concern, but the results of time-zero biomechanical testing may not imply final knee stability since the effect of bone healing is not considered. The findings of the current meta-analysis indicated that these 2 different fixations led to no differences in clinical knee stability.
The choice between suture and screw fixation is still an issue of debate. The screw fixation technique is relatively simple and allows the surgeon to maintain compression of the fracture fragments, 27 but the need for screw removal is a concern. Alternatively, suture fixation is another option since it provides equivalent, or even better, immediate fixation strength compared with screw fixation. 1,3,7,24,25 The present meta-analysis indicated that the use of suture fixation for tibial avulsion fractures leads to similar Lysholm knee scores, IKDC scores, and Tegner activity levels compared with the use of screw fixation. In addition, using suture fixation techniques leads to lower subsequent surgery rates, especially for implant removal, compared with using screw fixation methods. Based on the aforementioned findings, using suture fixation appears to be preferable.
Several newly proposed techniques for tibial avulsion fracture have been developed recently. 1,8,15,21,24 It is worth noting that these newly developed methods were all suture-related fixation techniques. Despite variations in fixation methods, both high-strength sutures and suture buttons are popular implant choices. 1,8,15,21,24 The findings of the current study also supported the use of suture fixation for tibial avulsion fractures. We believe that there will be a trend toward developing fixation techniques using suture-related fixation methods in the future.
Implant removal was common after screw fixation for tibial avulsion fractures. 13,17,19,26,28 Implant removal could be classified as either planned (plan made at time of implant insertion) or unplanned (removal because of symptoms). 4 In addition, fixed screws frequently needed to be removed to avoid violating the growth plate whenever they were used in skeletally immature patients. Callanan et al 4 reported that 66% and 45% of implants removal were planned surgical procedures in suture and screw fixation groups, respectively. They further indicated that reoperation rates between the 2 groups were not significantly different after excluding planned implants removal procedures. 4 In the present meta-analysis, both subsequent surgical procedures for hardware removal and nonhardware removal were analyzed between suture fixation and screw fixation groups. Not surprisingly, screw fixation resulted in a significantly greater rate of hardware removal. Although about half of the removal procedures were planned, 4 the higher reoperation rate was still a problem; this problem was even worse when the removal was unplanned. In addition to implant removal, subsequent surgical procedures due to postoperative stiffness and ligament laxity were occasionally required. 17,19,26,28 Conversely, no significant between-group differences were found for subsequent surgical procedures for nonhardware removal purposes in the present meta-analysis.
Limitations
There were several limitations in this meta-analysis. First, the sample size from each study was relatively small; only 1 cohort study with a larger sample size was included. All the included studies had a retrospective design, which could have potentially led to some bias. Therefore, prospective or randomized studies assessing the treatment outcomes for tibial avulsion fractures may be needed in the future. Second, management of postoperative care and the time from injury to surgery were not homogeneous among the individual studies. This is a common flaw of this type of study, and it may have contributed to bias in the current meta-analysis. Third, a wide range of age distribution existed in the included studies, and different age groups may lead to distinct clinical outcomes. Last, the size of the fracture fragments could not be controlled in our study, which could also influence the choice of fixation methods and the final fixation strength of each fragment.
Conclusion
The findings of this systematic review and meta-analysis indicated that screw fixation for ACL tibial avulsion fractures has a higher risk of subsequent surgery (RR, 2.33) and of implant removal (RR, 8.52) when compared with suture fixation. However, there was no significant difference in clinical outcome scores between techniques.
Footnotes
Final revision submitted November 17, 2021; accepted January 10, 2022.
Acknowledgment
The authors thank the Skeleton Materials and Bio-compatibility Core Lab, Research Center of Clinical Medicine, for the assistance of this project, and National Cheng Kung University Hospital (NCKUH-11101005 and NCKUH-11107005) for funding the publication fee.
Funding
The publication fee was funded by National Cheng Kung University Hospital (grant ID: NCKUH-11101005 and NCKUH-11107005).
The authors have declared that there are no conflicts of interest in the authorship and publication of this contribution. AOSSM checks author disclosures against the Open Payments Database (OPD). AOSSM has not conducted an independent investigation on the OPD and disclaims any liability or responsibility relating thereto.
