Abstract
Background:
Deep infrapatellar bursitis (DIB) has been detected in cases of Osgood-Schlatter disease (OSD). However, the clinical implications of DIB in the apophyseal stage, during the period when OSD has not yet developed, remain unclear.
Purpose:
To investigate the factors related to DIB in the apophyseal stage in preadolescent baseball players.
Study Design:
Cross-sectional study, Level of evidence, 3.
Methods:
The study participants were junior baseball players who participated in a medical checkup in 2020. We included knees in the apophyseal stage evaluated using ultrasonography, and classified them into the bursitis and no-bursitis groups using color-enhanced Doppler ultrasonography. We also investigated bone lesions of the tibial tuberosity, determined by fragmentation of the bone and irregularity of the ossification center. Demographic data, practice duration, pressure pain on tuberosity, pain while playing baseball (visual analog scale), heel-buttock distance (HBD), straight-leg raise angle, and range of hip internal and external rotation were evaluated. Group comparisons were performed using the Mann-Whitney U test and Fisher exact test, and a logistic regression analysis was performed.
Results:
A total of 261 knees (139 male players; age 10.5 ± 1.1 years) were included, 30 in the bursitis group and 231 in the no-bursitis group. Bone lesions were present in 4 knees in the bursitis group and in 32 knees in the no-bursitis group; there was no significant relationship between the presence of bone lesions and bursitis. Compared with the no-bursitis group, the bursitis group had a significantly longer practice duration (12.9 ± 3.3 vs 15.2 ± 3.8 hours/week, respectively; P = .003) and larger HBD (0.5 ± 1.3 vs 1.4 ± 2.4 cm, respectively; P = .003). The logistic regression analysis showed that practice duration (P = .001) and HBD (P = .004) were significantly related to the presence of bursitis.
Conclusion:
DIB in the apophyseal stage was related to practice duration and thigh muscle tightness. These findings may help predict overload and thigh muscle tightness at a very early stage.
Osgood-Schlatter disease (OSD) has been reported as a traction apophysitis of the tibial tuberosity developing from the apophyseal stage to the epiphyseal stage. 9,11,17,37,52 OSD is thought to be caused by repetitive strain on the quadriceps femoris muscle due to overuse and lower limb muscle tightness. 9,10,17,31,32,36,45,46 OSD generally resolves with nonoperative treatment, 5,12,17 but, in some cases, it leads to a poor sports performance and days lost from training and competition, 39 and surgery may be required for adults with free ossicles. 7,47,49
Recently, ultrasonography has been used for the noninvasive early diagnosis of OSD and the evaluation of soft tissue. 4,9,17,21,24,31,40,48 Deep infrapatellar bursitis (DIB) is reportedly an ultrasonographic feature of OSD. 4,9,40 However, we have encountered cases of DIB in the apophyseal stage without OSD, and its clinical implications remain unclear.
The purpose of this study was to investigate the association between DIB and the presence of bone lesions and factors specific to DIB in the apophyseal stage. We hypothesized that DIB in the apophyseal stage would be related to a specific background or physical features, and the early detection of DIB might lead to the very early detection of OSD.
Methods
Participants
Baseball teams registered with the Junior Baseball Federation of a Prefecture in Japan participated in a medical checkup in 2020. All participants in this cross-sectional study participated in the medical checkup. Inclusion criteria were (1) players who participated in preseason workouts as active players, (2) players who had no restrictions on baseball activities, and (3) players with knees in the apophyseal stage. Exclusion criteria were (1) players with a history of knee-related injury that restricting their baseball activities, (2) players who had not undergone the study-related examinations, and (3) players with knees in the cartilage, epiphyseal, or bony stages. This study was reviewed and approved by our university’s ethics committee, and written consent from the participants’ parents or guardians was obtained before the examination.
Demographic Data
We recorded the participants’ age, height (cm), body weight (kg), body mass index (BMI, kg/m2), and weekly practice duration (hours/week) for the team to which the athlete belonged.
Pressure Pain
We investigated the presence of pressure pain of the tuberosity and the subjective pain of tuberosity during playing baseball. Pressure pain was assessed if participants felt pain caused by pressure on palpation. The subjective pain of both sides was assessed by a 100-mm visual analog scale, with a higher score indicating more pain.
Ultrasonography Examination
Two experienced orthopaedic surgeons (SH and AO) performed the ultrasound examination using the LOGIQ e ultrasound (GH Healthcare Japan) with high-resolution linear-array probes at 12 MHz. The evaluations were performed with both knees in 90° of flexion in the supine position. Each surgeon evaluated a different set of knees in the examinations, and their findings were reviewed 1 week later to evaluate the intra- and interobserver reliability. The reliability was assessed using the κ value because they were categorical variables.
Tibial Tuberosity Development
We examined the skeletal maturation of the tibial attachment of the patellar tendon. The tibial tuberosity was examined using longitudinal ultrasonography at the site at which the tuberosity was most clearly visualized. Tibial tuberosity development as seen on ultrasonography was divided into the 4 stages described by Ehrenborg: cartilaginous, apophyseal, epiphyseal, and bony stage. 11,36,52 The cartilaginous stage is characterized by the presence of a large amount of apophyseal cartilage. The apophyseal stage is characterized by the patellar tendon attaching to apophyseal cartilage, with the secondary ossification center in the apophysis. The epiphyseal stage is characterized by the connection of the secondary ossification and tibial epiphysis. The bony stage is completely ossified, with the patellar tendon attached to a rough tibial tuberosity. Knees that were classified into the apophyseal stage were investigated in this study (Figure 1).

Representative images of tibial tuberosity development. (A) Cartilaginous stage, characterized by the presence of a large amount of apophyseal cartilage. (B) Apophyseal stage, characterized by the patellar tendon attaching to apophyseal cartilage, with the secondary ossification center in the apophysis. (C) Epiphyseal stage, characterized by the connection of the secondary ossification and tibial epiphysis. (D) Bony stage, characterized by complete ossification, with the patellar tendon attached to a rough tibial tuberosity. E, epiphysis; M, metaphysis; PT, patella tendon; arrow, secondary ossification center.
Detection of DIB
We conducted color-enhanced Doppler examination using ultrasonography with minimal sound pressure to avoid compression of any neovessels representing bursitis. 40 Doppler activity and ultrasound signs of neovessels of deep infrapatellar bursa located between the deep border of the distal third of the patellar tendon, the anterior aspect of the tibia, and the inferior border of the infrapatellar fat pad of Hoffa were recorded as positive or negative (Figure 2). 1,20 All knees determined as being in the apophyseal stage were divided into 2 groups: the bursitis group (positive Doppler activity) and the no-bursitis group (negative Doppler activity).

Representative image of Doppler-positive (red color) deep infrapatellar bursa (asterisk). E, epiphysis; H, infrapatellar fat pad of Hoffa; M, metaphysis; PT, patella tendon.
Bone Lesions
We investigated the presence of bone lesions of the tibial tuberosity. Bone lesions were defined as findings of fragmentation of the bone and irregularity of the ossification center on ultrasonography, in accordance with previous studies (Figure 3). 36,52

Bone lesion in the apophyseal stage. E, epiphysis; M, metaphysis; PT, patella tendon; arrow, fragmentation of the bone and irregularity of the ossification center.
Physical Examination
The physical examination consisted of measuring the straight-leg raise angle (SLRA), heel-buttock distance (HBD), and hip internal rotation (IR) and external rotation (ER). All examinations were performed by 2 experienced orthopaedic surgeons (HK and ST) who did not know the results of participants’ ultrasonography evaluations, with 1 assistant helping each. In the present study, no special warm-up was performed, and each examination was performed once.
A pilot test was conducted before this study to evaluate the intra- and interobserver reliability of the measurements: 10 healthy men were evaluated and were reevaluated 5 days later by the same examiners. Reliability was assessed using interclass correlation coefficients (ICCs) because these were continuous quantitative variables.
Straight-Leg Raise Angle
The SLRA was measured to evaluate the flexibility of hamstrings. 13,36 It was evaluated in the supine position and knee extension position. One examiner drew up 1 leg with full extension of the knee and flexed the hip joint until an end feel was detected. The contralateral limb was maintained in full extension, and the pelvis was stabilized. The SLRA, defined as the angle between the floor and the thigh, was measured with a digital goniometer (Digital Protractor with stainless blades; iGaging) used to measure the range of motion of joints in previous studies. 18,42
Heel-Buttock Distance
The HBD was measured to evaluate the flexibility of the quadriceps muscles. 13,36 It was measured in the prone position. One knee was placed passively in flexion with flexion at 0° of hip. The range of motion was stabilized such that when the first examiner felt resistance, the second examiner measured the horizontal distance between the lowest point of the heel and the highest point of the buttocks along with the perpendicular HBD using a ruler.
Hip IR and ER
The IR and ER of the hip were measured in the prone position according to previous studies, 18,38 using the same goniometer used in SLRA measurement. One examiner stabilized the pelvis, while the other bent the knee on the measurement side at 90° and rotated the hip joint internally and externally until an end feel was detected with flexion at 0°. The contralateral limb was maintained in full extension. The angles between the perpendicular and lower leg were defined as the IR and ER, respectively.
Statistical Analyses
In this study, the Mann-Whitney U test and Fisher exact test were used for comparisons between the bursitis group and no-bursitis group, and a logistic regression analysis was conducted. There were no missing data. All statistical procedures were conducted with a statistical analysis program (IBM SPSS Statistics 26 software package; IBM Japan). P < .05 was considered statistically significant.
Intra- and interobserver reliability was assessed as poor, moderate, good, and excellent for κ values of <0.4, 0.4-0.6, 0.6-0.8, and >0.8, respectively, and ICC values of <0.5, 0.5-0.75, 0.75-0.9, and >0.90, respectively.
With our sample size (N = 261 knees), this study had a power of over 80% and a 5% overall type I error level using the data of each evaluation item.
Results
The participants included 330 baseball players (217 males, 13 females; mean age ± standard deviation, 10.7 ± 1.3 years; range, 7-14 years). Of these participants, 306 (612 knees) were evaluated by ultrasonography and physical examinations, and ultimately included were 261 knees in the apophyseal stage from 139 male players (age, 10.5 ± 1.1 years). There were 30 knees in the bursitis group (positive Doppler activity) and 231 knees in the no-bursitis group (Figure 4).

Flowchart of study enrollment.
The bursitis group had a significantly longer practice duration (15.2 ± 3.8 hours/week) than the no-bursitis group (12.9 ± 3.3 hours/week) (P = .003). With regard to the demographic data, there were no significant differences in the age, body weight, or BMI between the 2 groups. There were also no significant between-group differences in pressure pain on tibial tuberosity or subjective pain while playing baseball (Table 1).
Age, Height, Body Weight, BMI, Practice Duration, and Pain a

a Values are presented as mean ± standard deviation (SD) unless otherwise indicated. Bold value indicates statistically significant between-group differences (P < .05). BMI, body mass index; VAS, visual analog scale.
b Mann-Whitney U test.
c Fisher exact test.
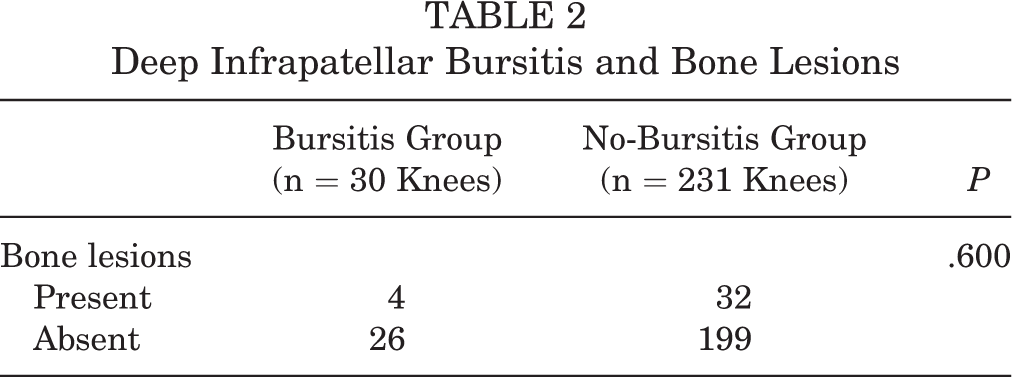
Bone lesions were present and absent in 4 and 26 knees, respectively, in the bursitis group and in 32 and 199 knees, respectively, in the no-bursitis group. There was no significant difference between groups in the presence of bone lesions (Table 2).
Deep Infrapatellar Bursitis and Bone Lesions
Regarding the physical examinations, the HBD of the bursitis group (1.4 ± 2.4 cm) was significantly larger than that of the no-bursitis group (0.5 ± 1.3 cm) (P = .003). There were no significant differences in the SLRA, hip IR, or ER between the 2 groups (Table 3).
Lower Limb Tightness a

a Values are presented as mean ± SD. Bold value indicates statistically significant between-group difference (P < .05). ER, external rotation; HBD, heel-buttock distance; IR, internal rotation; SLRA, straight-leg raise angle.
The logistic regression analysis showed that the practice duration (odds ratio, 1.231; 95% CI, 1.091-1.389; P = .001) and HBD (odds ratio, 1.427; 95% CI, 1.117-1.824; P = .004) were independently related to the presence of bursitis (Table 4).
Results of Logistic Regression Analysis for Bursitis a

a Bold values indicate statistical significance (P < .05). BMI, body mass index; CI, confidence interval; HBD, heel-buttock distance; OR, odds ratio.
The intra- and interobserver reliabilities were excellent regarding skeletal maturation of the tibial tuberosity (κ = 0.94 and 0.84, respectively), DIB assessment (κ = 0.90 and 0.81, respectively), and bone lesions (κ = 0.86 and 0.85, respectively). Regarding the pilot test for the physical measurements, the intra- and interobserver reliabilities were excellent for the SLRA (ICC = 0.98 and 0.98, respectively) and HBD (ICC = 0.99 and 0.99, respectively); for hip rotation measurements, the intraobserver reliability was excellent for IR (ICC = 0.98) and good for ER (ICC = 0.86), and the interobserver reliability was good for both (ICC = 0.90 for IR and 0.87 for ER).
Discussion
The most important finding of this study was that players with DIB in the apophyseal stage had a significantly longer practice duration (15.2 ± 3.8 hours/week) compared with players without bursitis (12.9 ± 3.3 hours/week) (P = .003), and greater thigh muscle tightness (1.4 ± 2.4 cm) compared with players without bursitis (0.5 ± 1.3 cm) (P = .003).
Bursae are normally synovial-lined structures with a dense capillary network that help reduce friction between moving structures. 1,6,44 Vasodilation and angiogenesis develop in cases of bursitis, 29,30 and are detected as positive Doppler activity. Deep infrapatellar bursae are located between the posterior aspect of the patellar tendon and anterior aspect of the tibia. 25,26 DIB has been reported to be associated with frequently repeated extension of the knee. 1,20 However, given the anatomical location of the deep infrapatellar bursae, it may reduce compressive stress between the patellar tendon and tibia during knee flexion, similar to the role of retrocalcaneal bursae between the calcaneus and the Achilles tendon. 19,28
Thigh muscle tightness increases with the development of the tibial tuberosity. 31 Muscle-tendon complexes catch up to the increase in bone length as muscle fibers increase their number of sarcomeres, but if the increase in sarcomeres does not keep pace with bone growth, muscle tightness is caused due to muscle shortening to the bone length. 22,43 Under conditions of thigh muscle tightness, compressive stress against deep infrapatellar bursae may strengthen during flexion of the knee. A longer practice duration may also increase the repetitive compressive stress at the deep infrapatellar bursa. DIB is suggested to be chronic inflammation caused by these factors.
Overload and thigh muscle tightness are factors well known to be related to OSD. 9,17,31,32,36,45,46 Some studies used the following clinical criteria to confirm the diagnosis of OSD: fragmentation of the bone and irregularity of the ossification center and pain with direct pressure on the tibial apophysis 4 ; pain before, during, and after physical activities; enlargement or prominence of the tibial apophysis; pain with resisted knee extension; and pain caused by jumping. 10 However, it is often difficult to diagnose OSD in pre-adolescent patients following these criteria because patients are required to explain their pain in detail, and enlargement or prominence of the tibial apophysis is not yet developed.
Regarding the process of tibial tuberosity maturation, hyperplasia of the chondrocyte occurs first, vascular invasion is then caused by vascular endothelial growth factor (VEGF), and finally osteogenesis occurs. 14,15 Hypertrophic chondrocytes modulate the production of VEGF under mechanical stress. 2,8,16,50 The deep infrapatellar bursa is adjacent to the apophysis, so DIB may be influenced by the overproduction of VEGF by the apophysis based on overload and muscle tightness. 40 The bone lesions seen in OSD are considered an avulsion of a portion of the developing ossification center and develop during the hypertrophic chondrocyte stage before enlarging and ossifying in later stages. 33 –35 Given that the presence of DIB was not significantly related to the presence of bone lesions in the present study, DIB in the apophyseal stage may also reflect stress on the immature apophysis before ossification.
In the present study, we simplified the assessment of pain as pressure pain on the tibial tuberosity and pain while playing baseball, and there were no significant differences noted between the bursitis and no-bursitis groups. The cause of pain in OSD has been attributed to bony fragmentation in the secondary ossification center. 10,23 However, it has been reported that knees with bursitis showed more severe pain than knees without bursitis. 40 Angiogenesis is associated with the proliferation of nerve fibers that can generate pain. 3,27 DIB in the apophyseal stage may only generate slight pain because of the short duration since its induction by DIB. Conversely, chronic DIB in the later stage may cause severe pain unless muscle tightness or overload is improved.
Identification of DIB may be useful as a technique for determining if the training load and muscle tightness are developmentally appropriate. In the present study among pre-adolescent baseball players, the differences in practice duration and HBD between the bursitis and no-bursitis groups were relatively small. However, the HBD increases with age, as does the practice duration among athletes. 31,41 A study among baseball players in the apophyseal and epiphyseal stages reported that the HBD in the symptomatic OSD group (10.5 ± 4.8 cm) was 75% longer than in the non-OSD group (6.0 ± 4.9 cm). In addition, the practice duration in the symptomatic OSD group (23.0 ± 9.0 hours/week) was 39% longer than in the non-OSD group (16.5 ± 5.7 hours/week). 36 As tightness increases and practice duration lengthens in the first few years of adolescence, it is important to make note of and improve such muscle tightness and lengthy practice durations at an early stage. It is known that the tightness of exercised muscle increases 51 ; therefore, more practice and play can cause greater muscle tightness. However, the logistic regression analysis showed that the practice duration and HBD were related independently to the presence of DIB in the present study. It is important to pay attention to relationship between DIB and either of the 2 factors. There have been no specific indicators of overload or thigh muscle tightness among pre-adolescent players without symptoms. While a further study will be needed to conclude the presence of a relationship between DIB and progress of OSD, DIB may help assess the presence of thigh muscle tightness and overload among pre-adolescent individuals at a very early stage.
When DIB is detected, doctors can give players and their family or sports staff tailored encouragement to reconsider the duration and contents of practice or advise them on stretching and appropriate self-conditioning. 22 Doctors evaluating players at sports sites are expected to play an important role in player health through such feedback and intervention.
Several limitations associated with the present study warrant a mention. First, this study was conducted in baseball players who engage in relatively little jumping and cutting actions. Second, we did not assess practice content or players’ positions. These sports specialization factors should be examined in future studies. Third, we did not evaluate the conditions around the patella, such as the thigh-foot angle, patella glides, lateral patella tilt, and bipartite patella, all factors that might affect DIB. Fourth, we did not evaluate strength, such as hip abduction, knee extension or flexion. Fifth, because this study was based on pre-adolescent baseball players, radiographic imaging was not performed. However, there have been many studies investigating OSD using ultrasonography, which is a noninvasive modality and useful for evaluating bursitis that was not evaluated using radiographic imaging. Finally, because this was a cross-sectional study, we were only able to conclude that there was an association between DIB and practice duration and thigh muscle tightness; we were unable to determine causation. Prospective studies should focus on whether or not players with DIB develop OSD and the outcomes of manipulation regarding training load and stretching using this technique.
Conclusion
In the current study, DIB in the apophyseal stage was related to practice duration and the HBD, factors already known to be related to OSD. These findings may help predict overload and thigh muscle tightness in adolescent players in the apophyseal stage.
Footnotes
Acknowledgment
The authors thank all of the study participants and their parents or guardians, as well as the staff members who cooperated and helped with this study.
Final revision submitted October 9, 2021; accepted December 8, 2021.
The authors have declared that there are no conflicts of interest in the authorship and publication of this contribution. AOSSM checks author disclosures against the Open Payments Database (OPD). AOSSM has not conducted an independent investigation on the OPD and disclaims any liability or responsibility relating thereto.
Ethical approval for this study was obtained from Gunma University Hospital (2015-1003).
