Abstract
Background:
Some patients have a positive pivot-shift finding and rotational instability after anterior cruciate ligament (ACL) reconstruction (ACLR). Three major pathologies known to affect the pivot-shift examination include ACL tear, anterolateral ligament injury, and loss of posterior lateral meniscus root function.
Purpose:
To describe a surgical algorithm determining indications for lateral extra-articular tenodesis (LET) based on intraoperative pivot-shift examination to prevent postoperative pivot shift and rotational instability and to evaluate the 2-year clinical and functional outcomes.
Study Design:
Case series; Level of evidence, 4.
Methods:
The study included 47 consecutive patients (39 men and 8 women) who underwent operative treatment for ACL injury between 2016 and 2017. Pivot-shift examination was performed under anesthesia, and the pivot shift was graded as grade 1 (glide), grade 2 (clunk), or grade 3 (gross). According to the surgical algorithm, single-bundle ACLR was performed in patients with grade 1 pivot shift. In patients with grade 2 with loss of posterior lateral meniscus root function, concurrent lateral meniscal repair was performed, and in patients with grade 2 with an intact lateral meniscus posterior root, concurrent extra-articular iliotibial band tenodesis was performed. Patients with grade 3 underwent ACLR, lateral meniscal repair, and LET. Clinical and radiographic evaluations were performed.
Results:
The mean age was 27.2 years (range, 16-56 years). In total, 26 (55.3%) patients were evaluated as having pivot-shift grade 1; 16 (34%) patients, grade 2; and 5 (10.6%) patients, grade 3. A total of 7 (14.9%) patients underwent LET in addition to ACLR. Two of these patients had pivot-shift grade 2, and LET was performed since the lateral meniscus posterior root was intact. In 14 of 16 patients with grade 2, lateral meniscus root disruption was detected, and lateral meniscal repair was performed. One patient was excluded from the further follow-up because of graft failure. At a mean postoperative follow-up of 29 months in 46 patients, the pivot-shift examination was negative in all patients. The mean Lysholm and International Knee Documentation Committee subjective scores were 95.35 ± 4.40 and 82.87 ± 9.36, respectively. Radiographic evidence of osteoarthritis was not detected.
Conclusion:
Only 14.9% of patients needed LET. With proper ACL, lateral meniscal, and anterolateral ligament surgery, it was possible to prevent positive pivot-shift findings postoperatively.
Keywords
The anterior cruciate ligament (ACL) is the most frequently operated ligament in the knee. Although the real incidence is unknown, approximately 200,000 ACL injuries per year occur in the United States, and 100,000 ACL reconstructions (ACLRs) are performed. 22 First-line treatment is arthroscopically assisted ACLR in active patients. 28 The main aim of surgery is to bring sagittal and rotational instability under control.
Even if anterior laxity can be brought under control using modern surgical techniques, sufficient control of internal rotational instability may not always be provided. 37 A positive pivot-shift sign continuing after surgery indicates continuing rotational instability and may be associated with poor functional results, patient dissatisfaction, and the development of osteoarthritis. 3,11,14 It has been shown in cadaveric studies that while isolated ACL injuries do not increase rotational laxity, injury to the anterolateral structures together with the ACL causes significant rotational laxity. 24,27
To prevent this coronal or rotational instability, different surgical techniques, such as double-bundle ligamentous reconstruction, lateralization of femoral tunnels, and combined intra- and extra-articular reconstruction, have been developed. These hybrid techniques almost always provide the possibility of reconstruction of anterolateral structures that have been damaged in knees with rotational instability. 35 One of the surgical solutions that can be applied to prevent anterolateral laxity is extra-articular lateral tenodesis. 10 Compared with intra-articular reconstructions, the advantage is that internal rotation can be better controlled via the long force arm formed because it is farther from the center of rotation of the knee. 16 In studies by Noyes and Barber, 26 Lerat et al, 17 and Marcacci et al, 20 successful results have been reported using extra-articular reinforcement applied in addition to single-bundle ACLR.
Lateral meniscus root dysfunction is another factor leading to the positive pivot-shift examination finding and is a cause of rotational laxity. Clinical and cadaveric studies have shown that in knees with ACL injury, the posterior root of the lateral meniscus has a significant role in anterolateral laxity. 18,23,34 In patients with ACL injury, the lateral meniscus posterior root function has attracted attention because it leads to rotational instability, and repair has been reported to be important. 23,34 Although repair is almost always recommended for lateral meniscus root tears, no definitive indications for extra-articular tenodesis have been reported in the literature.
It can be considered necessary to determine the conditions leading to rotational instability and to decide on the surgical treatments required for these pathological conditions on an individual patient basis. The finding of pivot shift in physical examination is effective in showing rotational instability in patients and is the physical examination test showing the best correlation with functional results after ACLR. 15 In our clinic, we apply an algorithm that targets 3 basic pathologies (ACL, anterolateral ligament [ALL], and lateral meniscus posterior root dysfunction), which lead to the finding of pivot shift.
The aim of this study was to clearly determine the indication for lateral extra-articular tenodesis (LET) and to prospectively evaluate the surgical results of our method aimed at eliminating the pivot-shift finding without creating any unnecessary surgical comorbidity. We hypothesized that with this algorithm applied during ACLR, it would be possible to determine in which patients LET should be applied.
Methods
Approval for this prospective, single-center, consecutive case series study was granted by the local ethics committee, and all enrolled patients provided informed consent (parents provided informed consent on behalf of the minors). The study included 54 consecutive patients who were treated operatively for ACL injury at a tertiary-level university hospital between December 2016 and 2017. Patients with bilateral knee, posterior cruciate ligament, medial collateral ligament, posterolateral corner, or lateral collateral ligament (LCL) injury in addition to ACL injury and those with a history of surgery on the same knee were excluded from the study. Patients with partial ACL rupture or intact ACL determined intraoperatively were also excluded; 7 patients were excluded (Figure 1). A total of 47 patients (39 men and 8 women) with a mean age of 27.2 years (range, 16-56 years) were evaluated prospectively at 4, 8, 12, and 24 months postoperatively. All included patients were skeletally mature, and there were no open physes.
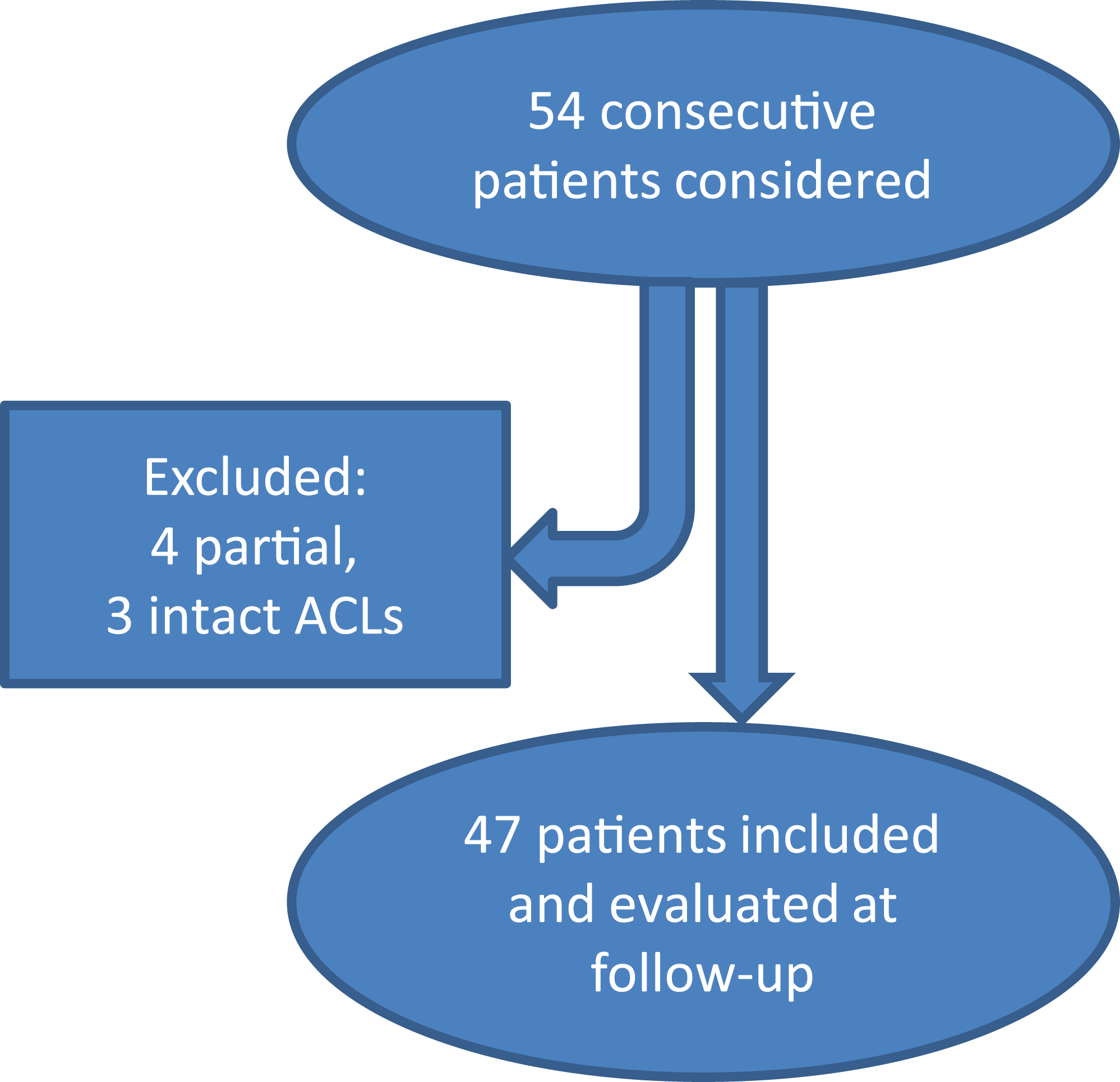
Inclusion and exclusion of patients. ACL, anterior cruciate ligament.
In 24 patients, the injury was evaluated as acute (<6 weeks); in 14 patients, chronic (>6 months); and in 9 patients, subacute (6 weeks--6 months). All of the operations were performed by the senior author (R.A.), who had experience of >10 years in sports surgery. After pivot-shift evaluation with the patient under general anesthesia, debridement was performed in diagnostic arthroscopy of any ACL remnants that could block the pivot-shift examination, and any bucket-handle tears were reduced; then the pivot-shift examination was repeated. Pivot-shift findings were classified as grade 0 (none, negative), grade 1 (glide), grade 2 (clunk), and grade 3 (gross).
Surgery was performed according to a treatment algorithm (Figure 2). For patients evaluated as having grade 1 pivot shift, single-bundle anatomic ACLR was performed. For those evaluated with grade 2 pivot shift, when there was lateral meniscus posterior root dysfunction, lateral meniscal repair and single-bundle ACLR was performed. As described by Feagin et al, 8 lateral meniscus posterior root avulsions, radial ruptures within the 9-mm region from the posterior root, large bucket-handle tears, and vertical tears extending toward the posterior root were considered to lead to lateral meniscus posterior root disruption. For patients with intact lateral meniscus posterior root, extra-articular iliotibial band (ITB) tenodesis was performed in addition to ACLR. For patients evaluated as having grade 3, ACLR, lateral meniscal repair, and extra-articular ITB tenodesis were performed because of lateral meniscus root and ALL tears together with ACL injury.

Surgical algorithm used to decide whether lateral extra-articular tenodesis (LET) is required. ACLR, anterior cruciate ligament reconstruction; LM, lateral meniscus; LMPR, lateral meniscus posterior root.
Surgical Technique
Single-bundle ACLR was performed via the IDEAL (isometric, direct fibers, eccentric/equidistant, anatomic, low tension) femoral tunnel technique using semitendinosus and gracilis autograft. 29 We used the Anatomic Anterior Cruciate Ligament Reconstruction Checklist 36 and total score was 18 points out of 19 for all patients. Endobutton (Endobutton CL Ultra; Smith & Nephew) was used for the femoral tunnel, and an interference screw (BIORCI ENDO-FIX L; Smith & Nephew) and a postfixation screw (4.5-mm titanium suture post; Smith & Nephew) were used for tibial tunnel fixation.
Meniscus posterior root tears were fixed to the anatomic root attachment site via a postfixation screw using the pullout technique from the transtibial tunnel, as described by Kim et al. 13
In patients when it was required, the LET procedure was performed after ACLR and meniscal repair. LET was performed using the modified Lemaire surgical technique. 21 Leaving the distal part of the ITB intact, the strip prepared from the ITB at 8 to 10 cm in length and 1 cm wide was passed below the proximal LCL and was fixed to anterior and proximal to the lateral head of the gastrocnemius tendon, on the lateral metaphyseal flare of the lateral femoral condyle using a staple (regular fixation staple; Smith & Nephew) at 60° of knee flexion and neutral rotation.
Meniscal tears were repaired using the all-inside, inside-out, and outside-in techniques combined according to the configuration and localization of the tear. Most of the tears were repaired using all-inside (FAST-FIX 360; Smith & Nephew) sutures, particularly posterior horn tears. The inside-out technique was used to assist all-inside sutures in large meniscal tears and in bucket-handle tears. Tears involving the anterior horn were repaired using outside-in sutures.
The patients receiving rehabilitation in the same center were mobilized on the first day postoperatively. In patients with meniscal repair, knee flexion was restricted to 90° for the first 3 weeks, then full weightbearing was permitted. In patients with meniscus root repair, full weightbearing was restricted for 6 weeks. A brace adjusted to 90° of flexion was used for 6 weeks by patients with root repair, partial weightbearing was permitted with crutches used for 2 weeks, then full weightbearing was started in the eighth week. No additional protocol was applied to patients who underwent LET. Patients were encouraged to perform static quadriceps and range of motion exercises in the first 4 weeks. In weeks 4 to 6, closed kinetic chain exercises and proprioceptive exercises were commenced. Dynamic movements and open chain isokinetic exercises were included in weeks 8 to 12 postoperatively, and running and jumping exercises were started after 3 months. Agility and hop exercises were introduced in weeks 16 to 24. Patients were allowed to return to sports in 6 months when there was no muscle atrophy of the operated leg.
Assessment
At the postoperative follow-up examinations, all the patients were evaluated by a single specialist physician (S.A.O.) who only presented during the evaluation under anesthesia with the senior surgeon (R.A.) to correlate and classify pivot-shift grades. The examiner (S.A.O.) was blinded to patient data, surgical procedures, and previous pivot-shift findings during the postoperative evaluations to minimize bias. The Lachman test, the anterior drawer test, and pivot-shift examinations were made at postoperative 4, 8, 12, and 24 months. The Lachman test was graded manually by the amount of translation as 1+ (3-5 mm), 2+ (6-10 mm), and 3+ (>10 mm) and compared with that of the contralateral knee. Outcomes were evaluated using a visual analog scale (VAS) for pain, Lysholm scoring, 5 and subjective knee evaluation via the International Knee Documentation Committee (IKDC). 6 Direct radiographs were taken preoperatively and at postoperative follow-up examinations. Arthritic changes were evaluated using the Ahlbäck classification. 2 Evaluation using magnetic resonance imaging (MRI) was made preoperatively and at 6- and 12-month follow-up.
Statistical Analysis
Data obtained in the study were evaluated statistically using SPSS Version 11.5 software (SPSS). In the comparison of the preoperative and 2-year Lysholm and IKDC scores, the Wilcoxon signed rank test was used. To determine whether or not there was any statistically significant difference among the pivot-shift groups, the Kruskal-Wallis test was applied. A value of P < .05 was accepted as statistically significant.
Results
The mean follow-up period was 29 months (range, 25-31 months). Of the total 47 patients, no patient had a grade 0 pivot shift, and 26 (55.3%) had pivot-shift grade 1 and underwent ACLR. There were no lateral meniscus root region tears in patients with grade 1 pivot shift. Sixteen (34.0%) patients had a grade 2 pivot shift; of these, 14 (87.5%) with ACL tear and lateral meniscus root disruption underwent ACLR and lateral meniscal repair. After the lateral meniscal repair, the pivot-shift finding was seen to have decreased to grade 1, and together with ACLR, it was possible to attain grade 0. In the other 2 patients (12.5% of grade 2 group; 4.3% of all patients), as the lateral meniscus was intact, we thought that insufficiency in the anterolateral structures leading to rotational instability had resulted in grade 2 pivot shift, and by performing ACLR together with LET in accordance with the study hypothesis, pivot-shift grade 0 was attained. The remaining 5 patients (10.6%) had a grade 3 pivot shift. Lateral meniscus root disruption was observed, and ACLR with LET was performed with lateral meniscal repair. LET was performed in 7 patients (14.9%) in total. There was no Segond fracture in our patients, and ALL injuries were not detectable on MRI scans preoperatively.
While MRI could detect 36 medial meniscal and 18 lateral meniscal lesions preoperatively, a total of 62 meniscal lesions (37 medial and 25 lateral) were seen during arthroscopy (Table 1). Partial medial menisectomy was performed in 17 patients, and partial lateral menisectomy was performed in 3 patients. A total of 18 medial meniscal tear repairs and 1 medial meniscus posterior root repair were made. A total of 22 lateral meniscal tear repairs were made as well as repairs for 6 lateral meniscus posterior root tears and 13 lateral meniscal tears that had led to posterior root dysfunction. There were no chondral injuries that required treatment.
Meniscal Lesion Types Found During Arthroscopy in 47 Patients

At postoperative 6 months, skin and subcutaneous infection developed in 1 patient around the Endobutton and postfixation screw. Debridement was applied in reoperation. The ACLR was intact, and the results of this patient were not removed from the study. At postoperative 8 months, rerupture occurred in 1 patient because of graft failure. The ACLR was evaluated as nonfunctional, so the data of this patient after the 8 months postoperatively were removed from the study.
The Lachman, pivot-shift, and anterior drawer test results of all 47 patients were negative at the postoperative 4-month follow-up examination. After excluding the patient with ACL rerupture at 8 months, the remaining 46 patients were all observed to have a negative pivot shift in the 2-year follow-up period. Grade 1+ Lachman and anterior drawer test positivity were determined in 2 patients. Laxity significantly improved in all the patients after surgery (P < .001). Statistically significant improvements were determined in the mean Lysholm knee scoring scale, IKDC, and VAS scores during the follow-up period (P < .001). Improvements in VAS, IKDC, and Lysholm scores were also significant in all groups when the pivot-shift groups were evaluated separately, yet there were no significant differences among the groups during the 2-year follow-up. The results according to the pivot-shift groups are shown in Table 2.
Pivot-Shift Grades and Evaluation of Functional and Subjective Scores a

a Data are presented as mean ± SD. IKDC, International Knee Documentation Committee; VAS, visual analog scale.
b One patient with grade 2 preoperatively had anterior cruciate ligament failure at 8 months postoperatively and was excluded from further follow-up.
c Significant VAS, IKDC, and Lysholm Scores compared with preoperative scores (P < .001). There was no significant difference among pivot-shift groups during the follow-up and at the end of the second year.
Throughout the 2-year follow-up period, no findings of osteoarthritis were observed. According to the Ahlbäck classification, osteoarthritis of grade 1 or higher was not seen in any patient. A total of 46 patients had MRI at follow-up, autografts were intact, and there was no pathological signal increase.
Discussion
Our study reveals satisfactory results from the surgical technique selected according to the algorithm described. When specifically required based on the patient, by performing the additional procedure of LET, sagittal and rotational stability could be provided. At the end of the 2-year follow-up period, rotational instability had been brought under control in all 46 patients. In 2 patients, there was residual grade 1+ Lachman and anterior drawer test positivity. Thus, it can be said that sagittal stability was obtained in 95% of the patients. Despite the different levels of rotational instability preoperatively, successful results were obtained in all 3 groups in the postoperative period. In accordance with the study hypothesis and the algorithm described, it was more evident which patients required the addition of LET to ACLR.
Various techniques have been described in the literature for the control of anterolateral instability and the prevention of pivot shift, one of which is extra-articular tenodesis. In studies by Lerat et al 17 and Noyes and Barber, 26 a significant improvement in knee laxity was shown with the extra-articular procedure performed in addition to ACLR. Bertoia et al, 4 Zarins and Rowe, 38 and Rackemann et al 30 reported that pivot shift could be brought under control in >90% of patients with intra-articular ACLR supported by the MacIntosh procedure. In a series of 251 cases published by Dejour et al, 7 83% excellent or good functional results were obtained using intra-articular ACLR supported by the Lemaire procedure. In studies by Marcacci et al 20 and Saragaglia et al 33 with mean follow-up periods of 11 and 6 years, respectively, when ACLR was performed using hamstring tendon grafts and lateral augmentation, it was reported to be possible to obtain grade 0 or grade 1 pivot shift in >90% of patients in both series.
Although satisfactory results of the combined procedures have been reported in literature, no definitive and objective indications have been defined for the use of these procedures, especially in primary ACLR. 9,21 Potential indications have been shown to be the degree of instability, additional injuries, young age, revision operations, meniscal failure, professional engagement in contact pivoting sports, posterior tibial slope >12°, and genu recurvatum >10°. 1,12,19,31,32 As there are high rates of failure in ACLR with these indications in isolation, they are evaluated as risk factors rather than definitive indications, and it is recommended that LET be performed in patients with these risk factors.
With a similar algorithm based on pivot shift, Musahl et al 25 planned a treatment guide that also started with pivot-shift grading; drew a general treatment plan including medial collateral ligament, LCL, and posterolateral corner injuries; and mentioned the importance of intraoperative navigation for a kinematic analysis. In our study, for ACL ruptures without concomitant ligamentous injuries, we used a specific treatment scheme that decision was made by pivot-shift evaluation under anesthesia and diagnostic arthroscopic findings. Computer-assisted navigation was not necessary. Using this algorithm, we have tried to define when LET is indicated in addition to ACLR, in a straightforward and effective way.
In the current study of patients with primary ACLR, the indication for LET was determined according to preoperative pivot-shift evaluation and intraoperative arthroscopic evaluation. Just as isolated ACL injury and grade 1 pivot-shift may be seen in professional athletes, young patients, and those with genu recurvatum, so ACL injury with pivot-shift grade 3 may be seen in patients with normal knee anatomy, aged >25 years, and who do not engage in sports. With the approach described in this study, action should be taken according to the physical examination of the patient and diagnostic arthroscopic findings, without differentiation of primary and revision cases. Thus, anterolateral rotational support is provided via LET according to the needs of each patient specifically. Considering the previously defined indications with this patient-centered approach could prevent any overtreatment. As only 14.9% of the current study patients required extra-articular tenodesis, it can be considered that by using this method only as required, potential complications associated with extra-articular tenodesis were minimized.
One of the points open for debate in the proposed algorithm is the patient group with grade 2 pivot shift. In the current study, these patients comprised 34.1% of the whole sample. The need for lateral support should be determined in these patients by examining whether or not there is continuation of the lateral meniscus root function. While the patients with grade 2 pivot shift requiring LET comprised 4.3% of all the patients, they comprised 12.5% of the grade 2 group. In this group, root repair or lateral meniscal repair is performed when there is lateral meniscus root dysfunction, and extra-articular tenodesis is performed when the root function is intact. The main point of discussion is what to do when a tear that causes lateral meniscus posterior root dysfunction cannot be repaired. In the current series, there were no such cases. Furthermore, there were no patients in the grade 2 group who underwent only ACLR. According to the algorithm, either lateral meniscal repair or LET should be performed in the grade 2 group. Although this may appear to lead to too many LET indications, in our series, LET was performed in only 2 patients in the grade 2 group to control pivot shift since there was no tear that impaired the posterior root function of the lateral meniscus. The lateral meniscus was repaired in the remaining 14 patients in the grade 2 group, and LET was not needed.
However, when repair cannot be made or in conditions progressing to partial menisectomy, should anterolateral reinforcement still be applied to prevent persistent pivot shift? This is one of the subjects that should be discussed. In these patients, when anterolateral instability originates from loss of lateral meniscus posterior root function and the anterolateral structures are known to be intact, the debatable point is whether or not the application of anterolateral reinforcement will result in overtreatment. When failure is present in the lateral meniscus, using an extra-articular procedure may increase the risk of arthrosis by leading to stiffness in the lateral compartment. In this situation, a patient-focused approach can be planned for anterolateral strengthening in patients with lateral meniscal defect and grade 2 pivot shift, such as in professional athletes with a need for extra stability.
The strong aspects of this study were the 2-year follow-up results of patients operatively treated at a single center by a single surgeon, following the same rehabilitation protocol, and evaluated by a single other surgeon blinded to the surgical procedures. Potential limitations of the study are that although the total patient group was sufficient in number, only 7 patients required extra-articular tenodesis according to the algorithm. The short-term results of the mean 2-year follow-up were successful, but there is a need for long-term outcomes.
Conclusion
The results of this study have shown that in the approach to patients with an ACL injury, the treatment according to the pivot-shift test performed under anesthesia and according to the status of lateral meniscus posterior root function has quite good outcomes. With a surgical approach appropriate to the lateral meniscus posterior horn and root, ACL, and ALL injuries, it is possible to completely prevent a positive pivot-shift finding. Further studies are required with a larger patient population in which more anterolateral reinforcement would be applied. Development of this algorithm with a longer follow-up period and a control group would be able to provide better definitive indications for LET.
Footnotes
Final revision submitted February 4, 2021; accepted February 28, 2021.
The authors declared that there are no conflicts of interest in the authorship and publication of this contribution. AOSSM checks author disclosures against the Open Payments Database (OPD). AOSSM has not conducted an independent investigation on the OPD and disclaims any liability or responsibility relating thereto.
Ethical approval for this study was obtained from Ankara University Faculty of Medicine Ethics Committee (ID No. 18-930-16).
