Abstract
Objectives:
During a multiple knee ligament reconstruction, the graft tensioning order may influence the final tibiofemoral orientation and corresponding knee kinematics. Therefore, the objective of this study was to biomechanically evaluate the effect of different graft tensioning sequences on knee tibiofemoral orientation following multiple knee ligament reconstruction in a bicruciate ligament (anterior cruciate ligament [ACL] and posterior cruciate ligament [PCL]) with posterolateral corner [PLC] injured knee.
Methods:
Ten non-paired, fresh-frozen human cadaveric knees were utilized for this study. Following reconstruction of both cruciate and posterolateral corner ligaments and proximal graft fixation, each knee was randomly assigned to each of four graft tensioning order groups: (1) PCL → ACL → PLC, (2) PCL → PLC → ACL, (3) PLC → ACL → PCL and (4) ACL → PCL → PLC. The tibiofemoral orientation after graft tensioning was measured and compared to the intact states.
Results:
Tensioning the ACL first (tensioning order 4) resulted in posterior displacement of the tibia at 0° by 1.7 ± 1.3 mm compared to the intact state (p=0.002) (Figure 1). All tensioning orders resulted in significantly increased anterior tibial translation compared to the intact state at higher flexion angles ranging from 2.7 mm to 3.2 mm at 60° and 3.1 mm to 3.4 mm at 90° for tensioning orders 1 and 2 respectively (all p<0.001). There was no significant difference in tibiofemoral orientation in the sagittal plane between the tensioning orders at higher flexion angles. All tensioning orders resulted in increased internal tibial rotation (all p<0.001). Tensioning and fixing the PLC first (tensioning order 3) resulted in the most increases in internal rotation of the tibia; 2.4° ± 1.9°, 2.7° ± 1.8° and 2.0° ± 2.0° at 0°, 30° and 60° respectively (Table 1).
Conclusion:
None of the tensioning orders restored intact knee tibiofemoral orientation. Tensioning the posterolateral corner first should be avoided in bicruciate knee ligament reconstruction with a concurrent posterolateral corner reconstruction because it significantly increased tibial internal rotation. We recommend that the PCL be tensioned first, followed by the ACL to avoid posterior translation of the tibia in extension where the knee is primarily loaded with most activities and finally the PLC.
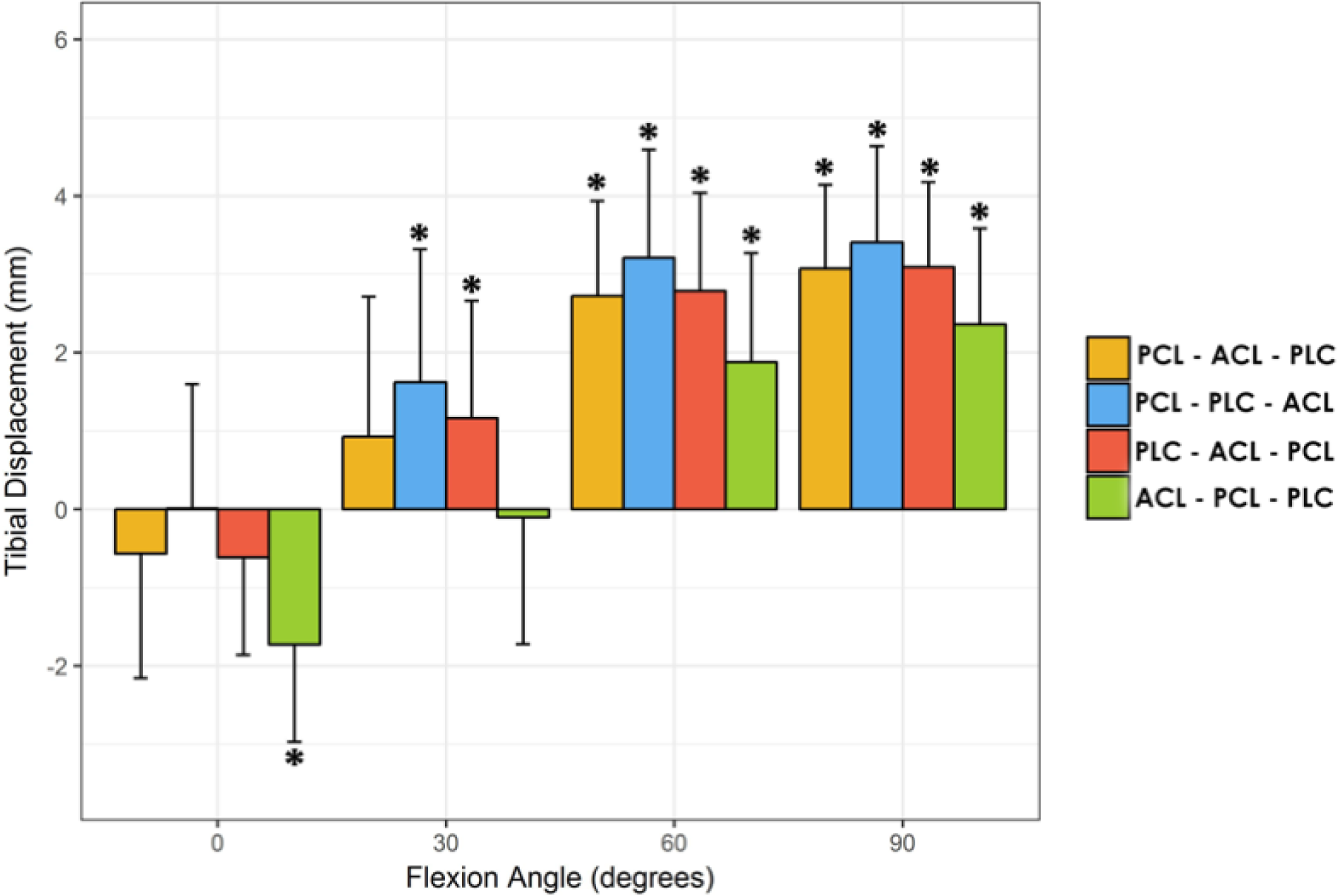
Mean changes from intact in tibial displacement in the anteroposterior (AP) direction after different tensioning sequences compared to the intact state (error bars represent ± 1 SD). The magnitude demonstrates changes after each tensioning sequence with intact subtracted. Positive values denote anterior translation, and negative values denote posterior translation of the tibia. * = significantly different from intact, native state (p < .05).0
Pairwise comparison of internal and external tibial rotation between the different tensioning orders with the intact, and between the tensioning orders at different angles (0°, 30°, 60°, 90°, respectively) for the zero force state. Angles are given in degrees, and the differences between the states are in degrees. Numbers in the top row denote tensioning order * denotes significant difference for that comparison. PP: passive path with minimal forces on the knee.

| Pairwise comparison of internal and external tibial rotation between the different tensioning orders | |||||||||
|---|---|---|---|---|---|---|---|---|---|
| 1 vs Intact | 2 vs Intact | 3 vs Intact | 4 vs Intact | 2 vs 1 | 3 vs 1 | 4 vs 1 | 3 vs 2 | 4 vs 2 | 4 vs 3 |
| 1.6* | 1.8* | 2.4* | 1.7* | 0.3 | 0.9 | 0.1 | 0.6 | -0.1 | -0.7 |
| 2.1* | 2.3* | 2.7* | 2.3* | 0.2 | 0.6 | 0.2 | 0.4 | 0 | -0.4 |
| 1.7* | 1.9* | 2.0* | 1.6* | 0.2 | 0.3 | -0.1 | 0.1 | -0.3 | -0.4 |
| 1.9 | 2.1* | 2.0* | 1.4 | 0.3 | 0.1 | -0.4 | -0.2 | -0.7* | -0.5 |
